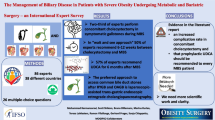
Abstract
Background
Weight loss after bariatric surgery varies among patients. Patients who do not complete long-term follow-up are considered to loose less weight than those with regular follow-up visits.
Objective
To evaluate the influence of patients’ follow-up compliance on long-term excess weight loss (%EWL) and total weight loss (%TWL) after bariatric surgery, comparing results between gastric bypass (GB) and sleeve gastrectomy (SG).
Methods
Patients with up to 5 years of follow-up data after bariatric surgery were included in this retrospective analysis. Patients were divided in 2 groups: those in group 1 who had attended every scheduled postoperative appointment and those in group 2 who had been lost to follow-up before 1 year and were later contacted by telephone. %EWL and %TWL were compared to determine the possible relationship between type of surgery and regularity of the follow-up.
Results
A total of 385 patients were included. A significant difference in EWL was observed at 5 years in the SG group (78% for group 1 versus 39% for group 2; p = 0.02) and GB group (75% for group 1 versus 62% for group 2; p = 0.01). No significant differences between surgeries were found when comparing long-term EWL in group 1 patients 77% for SG versus 75% for GB. For group 2 patients, GB achieved greater EWL than SG; p = 0.005. %TWL patients in group 2 showed significant differences in all periods of study (p < 0.05).
Conclusion
Bariatric surgery patients who attended all scheduled follow-up appointments experienced significantly greater long-term EWL and TWL than those who did not. GB has apparent increased benefits for weight loss in long-term follow-up when compared with SG for patients who did not attend long-term follow-up. Therefore, continued long-term follow-up of bariatric patients should be encouraged to increase postoperative weight loss results.


Similar content being viewed by others
References
Sjostrom L, Narbro K, Sjostrom CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357:741–52.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292:1724–37.
O’Kane M, Parretti HM, Hughes CA, et al. Guidelines for the follow-up of patients undergoing bariatric surgery. Clin Obes. 2016;6:210–24.
Busetto L, Dicker A, Azran C, et al. Obesity management task force on the European association for the study of obesity. Released practical recommendations for the post-bariatric surgery medical management. Obes Surg. 2018;28:2117–21.
Buchwald H. Consensus conference statement bariatric surgery for morbid obesity: health implications for patients, health professionals and third-party payers. Surg Obes Relat Dis. 2005;1:371–81.
Shen R, Dugay G, Rajaram K, et al. Impact of patient follow-up on weight loss after bariatric surgery. Obes Surg. 2004;14:514–9.
Sadhasivam S, Larson CJ, Lambert PJ, et al. Refusals, denials, and patient choice: reasons prospective patients do not undergo bariatric surgery. Surg Obes Relat Dis. 2007;3:531–6.
Pontiroli AE, Fossati A, Vedani P, et al. Post-surgery adherence to scheduled visits and compliance, more than personality disorders, predict outcome of bariatric restrictive surgery in morbidly obese patients. Obes Surg. 2007;17:1492–7.
Lara MD, Baker MT, Larson CJ, et al. Travel distance, age, and sex as factors in follow-up visit compliance in the post-gastric bypass population. Surg Obes Relat Dis. 2005;1:17–21.
Wheeler E, Prettyman A, Lenhard MJ, et al. Adherence to outpatient program postoperative appointments after bariatric surgery. Surg Obes Relat Dis. 2008;4:515–20.
Sockalingam S, Cassin S, Hawa R, et al. Predictors of post-bariatric surgery appointment attendance: the role of relationship style. Obes Surg. 2013;23(12):2026–32.
Gould JC, Beverstein NP, Reinhardt S, et al. Impact of routine and log-term follow-up on weight loss after laparoscopic gastric bypass. Surg Obes Relat Dis. 2007;3:627–30.
El Chaar M, McDeavitt K, Richardson S, et al. Does patient compliance with preoperative bariatric office visits affect postoperative excess weight loss? Surg Obes Relat Dis. 2011;7:743–8.
NIH conference gastrointestinal surgery for severe obesity consensus development conference panel. Ann Intern Med. 1991;115:956–61.
Harrison GG. Height-weight tables. Ann Intern Med. 1985;103:489–94.
Sjöström L, Lindroos AK, Peltonen M, et al. Swedish obese subjects study scientific group. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351(26):2683–93.
Khorgami Z, Zhang C, Messiah SE, et al. Predictors of postoperative aftercare attrition among gastric bypass patients. Bariatr Surg Pract Patient Care. 2015;10:79–83.
Harper J, Madan AK, Ternovits CA, et al. What happens to patients who do not follow-up after bariatric surgery? Am Surg. 2007;73(2):181–4.
Higa K, Ho T, Tercero F, et al. Laparoscopic Roux-en-Y gastric bypass: 10-years follow-up. Surg Obes Relat Dis. 2011;7:516–25.
Compher CW, Hanlon A, Kang Y, et al. Attendance at clinical visits predicts weight loss after gastric bypass surgery. Obes Surg. 2012;22(6):927–34.
McVay MA, Friedman KE, Applegate KL, et al. Patient predictors of follow-up care attendance in Roux-en-Y gastric bypass patients. Surg Obes Relat Dis. 2013;9:956–62.
Moroshko I, Brennan L, O'Brien P. Predictors of attrition in bariatric aftercare: a systematic review of the literature. Obes Surg. 2012;22:1640–7.
Sawhney P, Modi AC, Jenkins TM, et al. Predictors and outcomes of adolescent bariatric support group attendance. Surg Obes Relat Dis. 2013;9:773–9.
Scabim VM, Eluf Neto J, Tess BH. Adesão ao segmento nutricional ambulatorial pós-cirurgia bariátrica e fatores associados. Rev Nutr. 2012;25(4):497–506.
Jennings N, Boyle M, Mahawar K, et al. The relationship of distance from the surgical centre on attendance and weight loss after laparoscopic gastric bypass surgery in the United Kingdom. Clin Obes. 2013;3(6):180–4.
Nikolian VC, Williams AM, Jacobs BN, et al. Pilot study to evaluate the safety, feasibility and financial implications of a postoperative telemedicine program. Ann Surg. 2018;268:700–7.
Coldebella B, Armfield NR, Bambling M, et al. The use of telemedicine for delivering healthcare to bariatric surgery patients: a literature review. J Telemed Telecare. 2018;24:651–60.
Acknowledgments
The authors would like to thank Leire Alegria from the Institute of Data Science and Artificial Intelligence in the Universidad de Navarra for her assistance in the Materials and Methods section with the statistical analysis.
We acknowledge the Nurses of General Surgery of the University Clinic of Navarra for its contribution with special mention to Maria Molina.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Informed Consent
Informed consent was obtained from all individual participants included in this study.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lujan, J., Tuero, C., Landecho, M.F. et al. Impact of Routine and Long-Term Follow-Up on Weight Loss after Bariatric Surgery. OBES SURG 30, 4293–4299 (2020). https://doi.org/10.1007/s11695-020-04788-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-020-04788-7