Abstract
Background
Bariatric surgery is performed mostly on obese women of reproductive age. Many studies have analyzed pregnancy outcomes after bariatric surgery, but only a small number have studied the impact of pregnancy on the postoperative outcomes.
Purpose
To study the effect of pregnancy on outcomes after bariatric surgery in women of childbearing age.
Methods
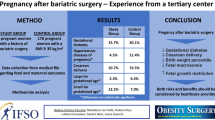
From January 2010 to October 2017, a retrospective study of a prospectively maintained database was conducted at the University Hospital of Geneva (HUG), where 287 women between the ages of 18 and 45 years had undergone Roux-en-Y gastric bypass (RYGB). A comparison of the results during a 5-year follow-up was performed between women who became pregnant after their bariatric surgery (pregnancy group, n = 40) and postoperative non-pregnant women (non-pregnancy group, n = 247). The two groups were compared for weight loss, complications, and nutritional deficiencies.
Results
The pregnancy group was significantly younger (29.2 ± 5.5 vs. 36.4± 6.3 years, p < 0.001) and heavier (124.0 ± 18.0 kg vs. 114.7 ± 17.1, p < 0.001) compared with the non-pregnancy group at the time of surgery. The percentage of excess BMI loss (%EBMI loss) was similar in both groups during the 5-year follow-up. Complications after RYGB and nutritional deficiencies were nearly identical in the two groups. The interval of time between bariatric surgery and first pregnancy was a median of 20.8 months. Out of 40 first pregnancies, 28 women completed pregnancy successfully with live birth.
Conclusion
Pregnancy after bariatric surgery is safe and does not adversely affect outcomes after RYGB.
Similar content being viewed by others
References
WHO. Obesity and overweight www.who.int/en/news-room/fact-sheets/detail/obesity-and-overweight: WHO World Health Organisation; 2018.
Ehrmann DA. Polycystic ovary syndrome. N Engl J Med. 2005;352(12):1223–36. https://doi.org/10.1056/NEJMra041536.
Maggard MA, Yermilov I, Li Z, et al. Pregnancy and fertility following bariatric surgery: a systematic review. JAMA. 2008;300(19):2286–96. https://doi.org/10.1001/jama.2008.641.
Sjöström L, Narbro K, Sjöström CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52. https://doi.org/10.1056/NEJMoa066254.
Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2011. Obes Surg. 2013;23(4):427–36. https://doi.org/10.1007/s11695-012-0864-0.
Gynecologists ACoOa. ACOG Committee opinion no. 549: obesity in pregnancy. Obstet Gynecol. 2013;121(1):213–7. https://doi.org/10.1097/01.AOG.0000425667.10377.60.
Roos N, Neovius M, Cnattingius S, et al. Perinatal outcomes after bariatric surgery: nationwide population based matched cohort study. BMJ. 2013;347:f6460. PubMed PMID: 24222480; PubMed Central PMCID: PMCPMC3898199
Aricha-Tamir B, Weintraub AY, Levi I, et al. Downsizing pregnancy complications: a study of paired pregnancy outcomes before and after bariatric surgery. Surg Obes Relat Dis. 2012;8(4):434–9. https://doi.org/10.1016/j.soard.2011.12.009.
Weintraub AY, Levy A, Levi I, et al. Effect of bariatric surgery on pregnancy outcome. Int J Gynaecol Obstet. 2008;103(3):246–51. https://doi.org/10.1016/j.ijgo.2008.07.008.
Bennett WL, Gilson MM, Jamshidi R, et al. Impact of bariatric surgery on hypertensive disorders in pregnancy: retrospective analysis of insurance claims data. BMJ. 2010;340:c1662. PubMed PMID: 20388692; PubMed Central PMCID: PMCPMC2854330
Lesko J, Peaceman A. Pregnancy outcomes in women after bariatric surgery compared with obese and morbidly obese controls. Obstet Gynecol. 2012;119(3):547–54. https://doi.org/10.1097/AOG.0b013e318239060e.
Kjaer MM, Nilas L. Pregnancy after bariatric surgery--a review of benefits and risks. Acta Obstet Gynecol Scand. 2013;92(3):264–71. https://doi.org/10.1111/aogs.12035.
Ducarme G, Parisio L, Santulli P, et al. Neonatal outcomes in pregnancies after bariatric surgery: a retrospective multi-centric cohort study in three French referral centers. J Matern Fetal Neonatal Med. 2013;26(3):275–8. https://doi.org/10.3109/14767058.2012.735723.
Belogolovkin V, Salihu HM, Weldeselasse H, et al. Impact of prior bariatric surgery on maternal and fetal outcomes among obese and non-obese mothers. Arch Gynecol Obstet. 2012;285(5):1211–8. https://doi.org/10.1007/s00404-011-2134-0.
Amsalem D, Aricha-Tamir B, Levi I, et al. Obstetric outcomes after restrictive bariatric surgery: what happens after 2 consecutive pregnancies? Surg Obes Relat Dis. 2014;10(3):445–9. https://doi.org/10.1016/j.soard.2013.08.016.
Bloomberg RD, Fleishman A, Nalle JE, et al. Nutritional deficiencies following bariatric surgery: what have we learned? Obes Surg. 2005;15(2):145–54. https://doi.org/10.1381/0960892053268264.
Guelinckx I, Devlieger R, Vansant G. Reproductive outcome after bariatric surgery: a critical review. Hum Reprod Update. 2009;15(2):189–201. https://doi.org/10.1093/humupd/dmn057.
Chevrot A, Lesage N, Msika S, et al. Digestive surgical complications during pregnancy following bariatric surgery: experience of a center for perinatology and obesity. J Gynecol Obstet Biol Reprod (Paris). 2016;45(4):372–9. https://doi.org/10.1016/j.jgyn.2015.04.007.
Wax JR. Risks and management of obesity in pregnancy: current controversies. Curr Opin Obstet Gynecol. 2009;21(2):117–23. https://doi.org/10.1097/GCO.0b013e328328d3c7.
Alatishe A, Ammori BJ, New JP, et al. Bariatric surgery in women of childbearing age. QJM. 2013;106(8):717–20. https://doi.org/10.1093/qjmed/hct081.
Quyên Pham T, Pigeyre M, Caiazzo R, et al. Does pregnancy influence long-term results of bariatric surgery? Surg Obes Relat Dis. 2015;11(5):1134–9. https://doi.org/10.1016/j.soard.2015.03.015.
Wax JR, Pinette MG, Cartin A. Roux-en-Y gastric bypass-associated bowel obstruction complicating pregnancy-an obstetrician's map to the clinical minefield. Am J Obstet Gynecol. 2013;208(4):265–71. https://doi.org/10.1016/j.ajog.2012.08.014.
Andreasen LA, Nilas L, Kjær MM. Operative complications during pregnancy after gastric bypass--a register-based cohort study. Obes Surg. 2014;24(10):1634–8. https://doi.org/10.1007/s11695-014-1232-z.
Altieri MS, Telem DA, Kim P, et al. Case review and consideration for imaging and work evaluation of the pregnant bariatric patient. Surg Obes Relat Dis. 2015;11(3):667–71. https://doi.org/10.1016/j.soard.2014.09.025.
Esmailzadeh H, Powell W, Lourie D. Use of computed tomography in diagnosis of major postoperative gastrointestinal complications of laparoscopic Roux-en-Y gastric bypass surgery. Am Surg. 2004;70(11):964–6.
Leal-González R, De la Garza-Ramos R, Guajardo-Pérez H, et al. Internal hernias in pregnant women with history of gastric bypass surgery: case series and review of literature. Int J Surg Case Rep. 2013;4(1):44–7. https://doi.org/10.1016/j.ijscr.2012.10.006. PubMed PMID: 23108170; PubMed Central PMCID: PMCPMC3537949
Gudbrand C, Andreasen LA, Boilesen AE. Internal hernia in pregnant women after gastric bypass: a retrospective register-based cohort study. Obes Surg. 2015;25(12):2257–62. https://doi.org/10.1007/s11695-015-1693-8.
Pathi A, Esen U, Hildreth A. A comparison of complications of pregnancy and delivery in morbidly obese and non-obese women. J Obstet Gynaecol. 2006;26(6):527–30. https://doi.org/10.1080/01443610600810914.
Gynecologists ACoOa. ACOG practice bulletin no. 105: bariatric surgery and pregnancy. Obstet Gynecol. 2009;113(6):1405–13. https://doi.org/10.1097/AOG.0b013e3181ac0544.
Eid-Arimoku L. How does bariatric surgery affect female fertility? BMJ. 2012;345:e6397.
Scholtz S, Le Roux C, Balen AH. The role of bariatric surgery in the management of female fertility. Hum Fertil (Camb). 2010;13(2):67–71. https://doi.org/10.3109/14647273.2010.492700.
Magdaleno R, Pereira BG, Chaim EA, et al. Pregnancy after bariatric surgery: a current view of maternal, obstetrical and perinatal challenges. Arch Gynecol Obstet. 2012;285(3):559–66. https://doi.org/10.1007/s00404-011-2187-0.
Koch TR, Finelli FC. Postoperative metabolic and nutritional complications of bariatric surgery. Gastroenterol Clin N Am. 2010;39(1):109–24. https://doi.org/10.1016/j.gtc.2009.12.003.
Poitou Bernert C, Ciangura C, Coupaye M, et al. Nutritional deficiency after gastric bypass: diagnosis, prevention and treatment. Diabetes Metab. 2007;33(1):13–24. https://doi.org/10.1016/j.diabet.2006.11.004.
Wittgrove AC, Jester L, Wittgrove P, et al. Pregnancy following gastric bypass for morbid obesity. Obes Surg. 1998;8(4):461–4; discussion 5-6. https://doi.org/10.1381/096089298765554368.
Woodard CB. Pregnancy following bariatric surgery. J Perinat Neonatal Nurs. 2004;18(4):329–40.
Magee SR, Shih G, Hume A. Malabsorption of oral antibiotics in pregnancy after gastric bypass surgery. J Am Board Fam Med. 2007;20(3):310–3. https://doi.org/10.3122/jabfm.2007.03.060177.
Kjær MM, Lauenborg J, Breum BM, et al. The risk of adverse pregnancy outcome after bariatric surgery: a nationwide register-based matched cohort study. Am J Obstet Gynecol. 2013;208(6):464.e1–5. https://doi.org/10.1016/j.ajog.2013.02.046.
Johansson K, Stephansson O, Neovius M. Outcomes of pregnancy after bariatric surgery. N Engl J Med. 2015;372(23):2267–8. https://doi.org/10.1056/NEJMc1503863.
Groupe de travail de la Clinique pédiatrique universitaire de Zurich (Paediatrica 2011 V, No 1). Courbes de croissance - Wachstumskurven www.kispi.uzh.ch/de/zuweiser/broschueren/Seiten/default.aspx: Kinderspital Zürich; 2018.
WHO. Preterm birth. http://www.who.int/news-room/fact-sheets/detail/preterm-birth: WHO World Health Organisation; 2018.
Apgar V. A proposal for a new method of evaluation of the newborn infant. Originally published in July 1953, volume 32, pages 250-259. Anesth Analg. 2015;120(5):1056–9. https://doi.org/10.1213/ANE.0b013e31829bdc5c.
Victory R, Penava D, Da Silva O, et al. Umbilical cord pH and base excess values in relation to adverse outcome events for infants delivering at term. Am J Obstet Gynecol. 2004;191(6):2021–8. https://doi.org/10.1016/j.ajog.2004.04.026.
Tierney JP, Welsh J, Owen P, et al. Management of early pregnancy loss—a complete audit cycle. J Obstet Gynaecol. 2006;26(3):229–32.
González I, Rubio MA, Cordido F, et al. Maternal and perinatal outcomes after bariatric surgery: a Spanish multicenter study. Obes Surg. 2015;25(3):436–42. https://doi.org/10.1007/s11695-014-1387-7.
Author information
Authors and Affiliations
Contributions
Conception and design: Brönnimann and Buchs. Acquisition of data: Brönnimann and Niclauss. Analysis and interpretation of data: Brönnimann, Jung, Niclauss, Hagen, Toso, and Buchs. Drafting the article: Brönnimann and Buchs. Revising it critically for important intellectual content: Jung, Hagen, Toso, Buchs, and Niclauss. Final approval of the version to be published: Brönnimann, Jung, Niclauss, Hagen, Toso, and Buchs.
Corresponding author
Ethics declarations
Conflict of Interest
A. Brönnimann, M. K. Jung, N. Niclauss, M. E. Hagen, C. Toso, N. C. Buchs have no conflict of interest. Monika E. Hagen received personal fees and non-financial support from Intuitive Surgical Inc., Quantgene Inc., Ethicon Inc., and Verb Surgical, outside this project.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent Statement
For this type of study (retrospective), formal consent is not required. However, all patients signed an informed consent form before undergoing bariatric surgery.
Open Access
This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Brönnimann, A., Jung, M.K., Niclauss, N. et al. The Impact of Pregnancy on Outcomes After Bariatric Surgery. OBES SURG 30, 3001–3009 (2020). https://doi.org/10.1007/s11695-020-04643-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-020-04643-9