Abstract
Background
History of abuse may impact weight loss (WL) following bariatric surgery. Some investigations have indicated slower WL rates among patients reporting abuse; however, among studies with multiple assessments, significant differences in WL are not evidenced at later measurement. Few investigations have extended follow-up beyond 18 months, limiting understanding of the impact of abuse on weight trajectory over time. Furthermore, existing research has insufficiently accounted for forms of interpersonal trauma beyond sexual abuse (i.e., emotional, physical) that may impact WL and other health outcomes.
Objectives
To determine whether post-surgical percent total WL (%TWL) and specific clinical outcomes are differentially impacted by history of interpersonal abuse.
Setting
Large, comprehensive medical center.
Methods
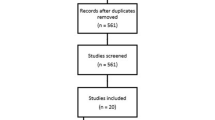
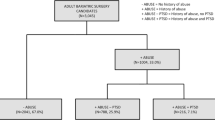
Retrospective data was collected from patients who underwent bariatric surgery at a single center (N = 433). Based on pre-surgical interview, patients were grouped according to reported history of interpersonal abuse (Y/N). Nonlinear repeated measures regression examined impact of abuse history on %TWL, and clinical selequae.
Results
Differences in %TWL at 6, 12, 18, 24, and 36 months post-surgically did not differ significantly. Further, %TWL did not differ across time, according to group. A significantly greater number of those with history of interpersonal abuse had a clinical diagnosis of depression as compared with those not reporting interpersonal abuse (38% vs. 22% respectively), p < .001.
Conclusions
Interpersonal abuse history does not negatively impact %TWL post-surgically but is associated with diagnosis of depression, indicating depressive symptoms may be a viable clinical intervention target for surgery patients with interpersonal trauma history.

Similar content being viewed by others
References
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724–37.
Sarwer DB, Wadden TA, Fabricatore AN. Psychosocial and behavioral aspects of bariatric surgery. Obes Res. 2005;13(4):639–48. https://doi.org/10.1038/oby.2005.71.
Finzi R, Har-Even D, Shnit D, et al. Psychosocial characterization of physically abused children from low socioeconomic households in comparison to neglected and nonmaltreated children. J Child Fam Stud. 2002;11:441–53. https://doi.org/10.1023/A:1020983308496.
Crosson-Tower C. Understanding child abuse and neglect. 6th ed. Toronto: Pearson Education; 2005.
Dillon G, Hussain R, Loxton D, et al. Mental and physical health and intimate partner violence against women: a review of the literature. Int J Family Med. 2013;2013:1–15. https://doi.org/10.1155/2013/313909.
Paolucci EO, Genuis ML, Violato C. A meta-analysis of the published research on the effects of child sexual abuse. J Psychol. 2001;135:17–36. https://doi.org/10.1080/00223980109603677.
Najdowski CJ, Ullman SE. Prospective effects of sexual victimization on PTSD and problem drinking. Addict Behav. 2009;34:965–8. https://doi.org/10.1037/e637872009-001.
Coker AL, Davis KE, Arias I, et al. Physical and mental health effects of intimate partner violence for men and women. Am J Prev Med. 2002;23:260–8. https://doi.org/10.1016/S0749-3797(02)00514-7.
Hetzel-Riggin MD, Roby RP. Trauma type and gender effects on PTSD, general distress, and peritraumatic dissociation. J Loss Trauma. 2013;18:41–53. https://doi.org/10.1080/15325024.2012.679119.
Walsh K, Resnick HS, Danielson CK, et al. Patterns of drug and alcohol use associated with lifetime sexual revictimization and current posttraumatic stress disorder among national samples of adolescent, college, and household-residing women. Addict Behav. 2014;39(3):684–9. https://doi.org/10.1016/j.addbeh.2013.12.006.
Shapero BG, Black SK, Liu RT, et al. Stressful life events and depression symptoms: the effect of childhood emotional abuse on stress reactivity. J Clin Psychol. 2014;70(3):209–23. https://doi.org/10.1002/jclp.22011.
Mandelli L, Petrelli C, Serretti A. The role of specific early trauma in adult depression: a meta-analysis of published literature. Childhood trauma and adult depression. Eur Psychiatry. 2015;30(6):665–80. https://doi.org/10.1016/j.eurpsy.2015.04.007.
Gibb BE, Alloy LB, Abramson LY, et al. History of childhood maltreatment, negative cognitive styles, and episodes of depression in adulthood. Cogn Ther Res. 2001;25:425–46. https://doi.org/10.1023/A:1005586519986.
Gustafson TB, Sarwer DB. Childhood sexual abuse and obesity. Obes Rev. 2004;5(3):129–35. https://doi.org/10.1111/j.1467-789X.2004.00145.x.
Steinig J, Wagner B, Shang E, et al. Sexual abuse in bariatric surgery candidates–impact on weight loss after surgery: a systematic review. Obes Rev. 2012;13(10):892–901. https://doi.org/10.1111/j.1467-789x.2012.01003.x.
Fujioka K, Yan E, Wang HJ, et al. Evaluating preoperative weight loss, binge eating disorder, and sexual abuse history on roux-en-Y gastric bypass outcome. Surg Obes Relat Dis. 2008;4(2):137–43. https://doi.org/10.1016/j.soard.2008.01.005.
Hensel JM, Kaplan KG, Anvari M, et al. The impact of history of exposure to abuse on outcomes after bariatric surgery: data from the Ontario Bariatric Registry. Surg Obes Relat Dis. 2016;12(8):1441–6. https://doi.org/10.1016/j.soard.2016.03.016.
Ray EC, Nickels MW, Sayeed S, et al. Predicting success after gastric bypass: the role of psychosocial and behavioral factors. Surgery. 2003;134(4):555–63. https://doi.org/10.1016/s0039-6060(03)00279-4.
Buser A, Dymek-Valentine M, Hilburger J, et al. Outcome following gastric bypass surgery: impact of past sexual abuse. Obes Surg. 2004;14(2):170–4. https://doi.org/10.1381/096089204322857519.
Oppong BA, Nickels MW, Sax HC. The impact of a history of sexual abuse on weight loss in gastric bypass patients. Psychosomatics. 2006;47(2):108–11. https://doi.org/10.1176/appi.psy.47.2.108.
Buser AT, Lam CS, Poplawski SC. A long-term cross-sectional study on gastric bypass surgery: impact of self-reported past sexual abuse. Obes Surg. 2009;19(4):422–6. https://doi.org/10.1007/s11695-008-9555-2.
Larsen JK, Geenen R. Childhood sexual abuse is not associated with a poor outcome after gastric banding for severe obesity. Obes Surg. 2005;15(4):534–7. https://doi.org/10.1381/0960892053723277.
Grilo CM, White MA, Masheb RM, et al. Relation of childhood sexual abuse and other forms of maltreatment to 12-month postoperative outcomes in extremely obese gastric bypass patients. Obes Surg. 2006;16(4):454–60. https://doi.org/10.1381/096089206776327288.
Ikossi DG, Maldonado JR, Hernandez-Boussard T, et al. Post-traumatic stress disorder (PTSD) is not a contraindication to gastric bypass in veterans with morbid obesity. Surg Endosc. 2010;24(8):1892–7. https://doi.org/10.1007/s00464-009-0866-8.
Clark MM, Hanna BK, Mai JL, et al. Sexual abuse survivors and psychiatric hospitalization after bariatric surgery. Obes Surg. 2007;17(4):465–9. https://doi.org/10.1007/s11695-007-9084-4.
Wedin S, Madan A, Correll J, et al. Emotional eating, marital status and history of physical abuse predict 2-year weight loss in weight loss surgery patients. Eat Behav. 2014;15(4):619–24. https://doi.org/10.1016/j.eatbeh.2014.08.019.
Wood GC, Chu X, Manney C, et al. An electronic health record-enabled obesity database. BMC Med Inform Decis Mak. 2012;12(1) https://doi.org/10.1186/1472-6947-12-45.
Felitti VJ. Childhood sexual abuse, depression, and family dysfunction in adult obese patients. South Med J. 1993;86(7):732–6. https://doi.org/10.1097/00007611-199307000-00002.
Felitti VJ. Long-term medical consequences of incest, rape, and molestation. South Med J. 1991;84(3):328–31. https://doi.org/10.1097/00007611-199103000-00008.
Funding
This research was supported by a grant from Geisinger (18-062; S. Gorrell and L. Campbell) and National Institutes of Health grant NIH P30 DK072488 (GC Wood). The funders had no role in study design, data analysis, interpretation, or dissemination of study findings.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Dr. Gorrell is now a fulltime employee of University of California, San Francisco. Dr. Mahoney is now a fulltime employee of The National Center for PTSD and Boston University.
Rights and permissions
About this article
Cite this article
Gorrell, S., Mahoney, C.T., Lent, M. et al. Interpersonal Abuse and Long-term Outcomes Following Bariatric Surgery. OBES SURG 29, 1528–1533 (2019). https://doi.org/10.1007/s11695-018-03696-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-018-03696-1