Abstract
Background
The aim of this study was to study the process of intestinal adaptation in the three limbs of the small intestine after malabsorptive bariatric surgery: the biliopancreatic limb, the alimentary limb, and the common channel. These limbs are exposed to different stimuli, namely, gastrointestinal transit and nutrients in the alimentary limb, biliopancreatic secretions in the biliopancreatic limb, and a mix of both in the common channel. We also wished to investigate the effect of glutamine supplementation on the adaptation process.
Methods
Three types of surgery were performed using a porcine model: biliopancreatic bypass (BPBP), massive (75%) short bowel resection as the positive control, and a sham operation (transection) as the negative control. We measured the height and width of intestinal villi, histidine decarboxylase (HDC) activity, and amount of HDC messenger RNA (mRNA) (standard diet or a diet supplemented with glutamine).
Results
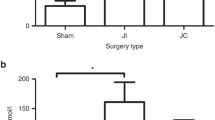
An increase in HDC activity and mRNA expression was observed in the BPBP group. This increase coincided with an increase in the height and width of the intestinal villi. The increase in villus height was observed immediately after surgery and peaked at 2 weeks. Levels remained higher than those observed in sham-operated pigs for a further 4 weeks.
Conclusions
The intestinal adaptation process in animals that underwent BPBP was less intense than in those that underwent massive short bowel resection and more intense than in those that underwent transection only. Supplementation with glutamine did not improve any of the parameters studied, although it did appear to accelerate the adaptive process.





Similar content being viewed by others
References
Carswell KA, Vincent RP, Belgaumkar AP, et al. The effect of bariatric surgery on intestinal absorption and transit time. Obes Surg. 2014;24(5):796–805.
Albert V, Young GP, Morton CL, et al. Systemic factors are trophic in bypassed rat small intestine in the absence of luminal contents. Gut. 1990;31(3):311–6.
Randy JS, Adam PC, Darleen AS. The role of gut adaptation in the potent effects of multiple bariatric surgeries on obesity and diabetes. Cell Metabolism Cell Metab. 2015;21(3):369–78.
Neelis EG, Olieman JF, Hulst JM, et al. Promoting intestinal adaptation by nutrition and medication. Best Pract Res Clin Gastroenterol. 2016;30(2):249–61.
Mitchell JL, Qasba P, Stofko RE, et al. Ornithine decarboxylase modification and polyamine-stimulated enzyme inactivation in HTC cells. Biochem J. 1985;228(2):297–308.
Chomczynski P, Sacchi N. Single-step method of RNA isolation by acid guanidinium thiocyanate-phenol-chloroform extraction. Anal Biochem. 1987;162(1):156–9.
Reyes-Engel A, García-Villanova J, Dieguez-Lucena JL, et al. New approach to mRNA. Quantification: additive RT-PCR. BioTechniques. 1996;21:202–4.
Seeley RJ, Chambers AP, Sandoval DA. The role of gut adaptation in the potent effects of multiple bariatric surgeries on obesity and diabetes. Cell Metab. 2015;21(3):369–78.
Taqi E, Wallace LE, de Heuvel E, et al. The influence of nutrients, biliary-pancreatic secretions, and systemic trophic hormones on intestinal adaptation in a Roux-en-Y bypass model. J Pediatr Surg. 2010;45(5):987–95.
le Roux CW, Borg C, Wallis K, et al. Gut hypertrophy after gastric bypass is associated with increased glucagon-like peptide 2 and intestinal crypt cell proliferation. Ann Surg. 2010;252(1):50–6.
Li B, Lu Y, Srikant CB, et al. Intestinal adaptation and Reg gene expression induced by antidiabetic duodenal-jejunal bypass surgery in Zucker fatty rats. Am J Physiol Gastrointest Liver Physiol. 2013;304(7):G635–45.
Tappenden KA. Intestinal adaptation following resection. JPEN J Parenter Enteral Nutr. 2014;38(1 Suppl):23S–31S.
Chen J, Qin Z, Shan H, et al. Early adaptation of small intestine after massive small bowel resection in rats. Iran J Pediatr. 2015;25(4):e530.
García-Caballero M, Fernández JL, Ruiz J, et al. Middle term intestinal adaptation after massive distal small bowel resection in oral feeding dogs. Nutr Hosp. 1996;11(5):265–73.
Kennedy L, Hodges K, Meng F, et al. Histamine and histamine receptor regulation of gastrointestinal cancers. Transl Gastrointest Cancer. 2012;1(3):215–27.
Graf A, Meng F, Hargrove L, et al. Knockout of histidine decarboxylase decreases bile duct ligation-induced biliary hyperplasia via downregulation of the histidine decarboxylase/VEGF axis through PKA-ERK1/2 signaling. Am J Physiol Gastrointest Liver Physiol. 2014;307(8):G813–23.
Fujimoto K, Imamura I, Granger DN, et al. Histamine and histidine decarboxylase are correlated with mucosal repair in rat small intestine after ischemia-reperfusion. J Clin Invest. 1992;89(1):126–33.
Dartsch C, Chen D, Håkanson R, et al. Multiple forms of histidine decarboxylase may reflect posttranslational activation. Biochem Soc Trans. 1998;26(4):S377.
Windmueller HG, Spaeth AE. Identification of ketone bodies and glutamine as the major respiratory fuels in vivo for postabsorptive rat small intestine. J Biol Chem. 1978;253:69–76.
Yang H, Larsson J, Permert J, et al. No effect of bolus glutamine supplementation on the postresectional adaptation of small bowel mucosa in rats receiving chow ad libitum. Dig Surg. 2000;17(3):256–60.
Demaria EJ, Winegar DA, Pate VW, et al. Early postoperative outcomes of metabolic surgery to treat diabetes from sites participating in the ASMBS bariatric surgery center of excellence program as reported in the Bariatric Outcomes Longitudinal Database. Anna Surg. 2010;252:559–67.
Welbourn R, Pournaras D. Bariatric surgery: a cost-effective intervention for morbid obesity; functional and nutritional outcomes. Proc Nutr Soc. 2010;69:528–35.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval Statement
Housing and care of the animals complied with current regulations Directive 2010/63/EU of the European parliament and of the council of 22 September 2010 on the protection of animals used for scientific purposes (Official Journal of the European Union. 20/10/2010. 276:33–79).
Additional information
This work was performed in the Department of Surgical Specialities, Biochemistry and Immunology, Faculty of Medicine, University of Málaga, (Spain).
In memory of Prof. Manuel Garcia-Caballero
Rights and permissions
About this article
Cite this article
Martínez Moreno, J.M., Reyes-Ortiz, A., Lage Sánchez, J.M. et al. Timeline of Intestinal Adaptation After Malabsortive Surgery: Effect of Luminal Nutrients, Biliopancreatic Secretion, and Glutamine Supplementation. OBES SURG 27, 3133–3141 (2017). https://doi.org/10.1007/s11695-017-2754-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2754-y