Abstract
Background
Sleeve gastrectomy is being performed increasingly, mainly due to its low morbidity and mortality, but complications do occur. The aim of this study was to evaluate bleeding and leakage rates of primary and revisional sleeve gastrectomy in a personal series of 664 consecutive patients.
Methods
Medical charts of all patients undergoing a primary or revisional sleeve gastrectomy between August 2008 and December 2014 were reviewed retrospectively. Subgroup analysis compared bleeding in patients after reduced port versus multiport technique and primary versus revisional sleeve gastrectomy.
Results
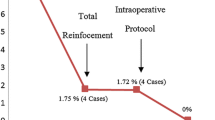
A total of 664 sleeve gastrectomies (489 women and 175 men) were performed. Mean age and body mass index were 36.03 ± 11.4 years and 42.9 ± 8.3 kg/m2, respectively. Mean operative time was 58.5 ± 20.0 min, with a 0.15 % conversion rate. Mean hospital stay was 2.1 ± 0.3 days. The overall 30-day complication rate was 7.5 %. Thirteen patients sustained postoperative bleeding (2 %), three of whom required reoperation (0.5 %). Staple line leakage and mortality were both nil in this series. No difference in postoperative complications was found between the subgroups.
Conclusions
In this single-surgeon, single-center experience, sleeve gastrectomy was a safe and effective bariatric procedure with a low complication rate. Staple line reinforcement by oversewing was associated with low bleeding complications and no leakage. The majority of patients with postoperative bleeding could be managed conservatively. In our experience, reduced port technique and revisional sleeve gastrectomy had similar complication rates compared to multiport and primary sleeve gastrectomy.


Similar content being viewed by others
References
Ren CJ, Patterson E, Gagner M. Early results of laparoscopic biliopancreatic diversion with duodenal switch: a case series of 40 consecutive patients. Obes Surg. 2000;10:514–23. Discussion 524.
Mittermair R, Sucher R, Perathoner A. Results and complications after laparoscopic sleeve gastrectomy. Surg Today. 2014;44:1307–12.
Himpens J, Dapri G, Cadière GB. A prospective randomized study between laparoscopic gastric banding and laparoscopic isolated sleeve gastrectomy: results after 1 and 3 years. Obes Surg. 2006;16:1450–6.
Consten EC, Gagner M, Pomp A, et al. Decreased bleeding after laparoscopic sleeve gastrectomy with or without duodenal switch for morbid obesity using a stapled buttressed absorbable polymer membrane. Obes Surg. 2004;14:1360–6.
Parikh M, Issa R, McCrillis A, et al. Surgical strategies that may decrease leak after laparoscopic sleeve gastrectomy: a systematic review and meta-analysis of 9991 cases. Ann Surg. 2013;257:231–7. doi:10.1097/SLA.0b013e31826cc714.
Knapps J, Ghanem M, Clements J, et al. A systematic review of staple-line reinforcement in laparoscopic sleeve gastrectomy. JSLS. 2013;17:390–9. doi:10.4293/108680813X13654754534639.
Aggarwal S, Sharma AP, Ramaswamy N. Outcome of laparoscopic sleeve gastrectomy with and without staple line oversewing in morbidly obese patients: a randomized study. J Laparoendosc Adv Surg Tech A. 2013;23:895–9. doi:10.1089/lap.2013.0137.
Albanopoulos K, Alevizos L, Flessas J, et al. Reinforcing the staple line during laparoscopic sleeve gastrectomy: prospective randomized clinical study comparing two different techniques. Preliminary results. Obes Surg. 2012;22:42–6. doi:10.1007/s11695-011-0421-2.
Dapri G, Cadière GB, Himpens J. Reinforcing the staple line during laparoscopic sleeve gastrectomy: prospective randomized clinical study comparing three different techniques. Obes Surg. 2010;20:462–7. doi:10.1007/s11695-009-0047-9.
Gentileschi P, Camperchioli I, D’Ugo S, et al. Staple-line reinforcement during laparoscopic sleeve gastrectomy using three different techniques: a randomized trial. Surg Endosc. 2012;26:2623–9. doi:10.1007/s00464-012-2243-2.
Chen B, Kiriakopolous A, Tsakayannis D, et al. Reinforcement does not necessarily reduce the rate of staple line leaks after sleeve gastrectomy. A review of the literature and clinical experiences. Obes Surg. 2009;19:166–72. doi:10.1007/s11695-008-9668-7.
Giannopoulos GA, Tzanakis NE, Rallis GE, et al. Staple line reinforcement in laparoscopic bariatric surgery: does it actually make a difference? A systematic review and meta-analysis. Surg Endosc. 2010;24:2782–8. doi:10.1007/s00464-010-1047-5.
Choi YY, Bae J, Hur KY, et al. Reinforcing the staple line during laparoscopic sleeve gastrectomy: does it have advantages? A meta-analysis. Obes Surg. 2012;22:1206–13. doi:10.1007/s11695-012-0674-4.
Daskalakis M, Berdan Y, Theodoridou S, et al. Impact of surgeon experience and buttress material on postoperative complications after laparoscopic sleeve gastrectomy. Surg Endosc. 2011;25:88–97. doi:10.1007/s00464-010-1136-5.
Durmush E, Ermerak G, Durmush D. Short-term outcomes of sleeve gastrectomy for morbid obesity: does staple line reinforcement matter? Obes Surg. 2014;24:1109–16. doi:10.1007/s11695-014-1251-9.
Al Hajj G, Haddad J. Preventing staple-line leak in sleeve gastrectomy: reinforcement with bovine pericardium vs oversewing. Obes Surg. 2013;23:1915–21. doi:10.1007/s11695-013-1062-4.
Deitel M, Gagner M, Erickson AL, et al. Third International Summit: current status of sleeve gastrectomy. Surg Obes Relat Dis. 2011;7:749–59. doi:10.1016/j.soard.2011.07.017.
Inabnet 3rd WB, Belle SH, Bessler M, et al. Comparison of 30-day outcomes after non-LapBand primary and revisional bariatric surgical procedures from the longitudinal assessment of bariatric surgery study. Surg Obes Relat Dis. 2010;6:22–30. doi:10.1016/j.soard.2009.10.007.
Berende CA, de Zoete JP, Smulders JF, et al. Laparoscopic sleeve gastrectomy feasible for bariatric revision surgery. Obes Surg. 2012;22:330–4. doi:10.1007/s11695-011-0501-3.
Goitein D, Feigin A, Segal-Lieberman G, et al. Laparoscopic sleeve gastrectomy as a revisional option after gastric band failure. Surg Endosc. 2011;25:2626–30. doi:10.1007/s00464-011-1615-3.
Obeid NR, Schwack BF, Kurian MS, et al. Single-stage versus 2-stage sleeve gastrectomy as a conversion after failed adjustable gastric banding: 30-day outcomes. Surg Endosc. 2014;28:3186–92. doi:10.1007/s00464-014-3585-8.
Kim SM, Ha MH, Seo JE, et al. Comparison of reduced port Totally Laparoscopic Distal Gastrectomy (Duet TLDG) and conventional laparoscopic-assisted distal gastrectomy. Ann Surg Oncol. 2015;22:2567–72. doi:10.1245/s10434-014-4333-y.
Saber AA, Elgamal MH, Itawi EA, et al. Single incision laparoscopic sleeve gastrectomy (SILS): a novel technique. Obes Surg. 2008;18:1338–42. doi:10.1007/s11695-008-9646-0.
Gomberawalla A, Salamat A, Lutfi R. Outcome analysis of single incision vs traditional multiport sleeve gastrectomy: a matched cohort study. Obes Surg. 2014;24:1870–4. doi:10.1007/s11695-014-1312-0.
Lakdawala MA, Muda NH, Goel S, et al. Single-incision sleeve gastrectomy versus conventional laparoscopic sleeve gastrectomy–a randomised pilot study. Obes Surg. 2011;21:1664–70. doi:10.1007/s11695-011-0478-y.
Sucher R, Resch T, Mohr E, et al. Single-incision laparoscopic sleeve gastrectomy versus multiport laparoscopic sleeve gastrectomy: analysis of 80 cases in a single center. J Laparoendosc Adv Surg Tech A. 2014;24:83–8. doi:10.1089/lap.2013.0250.
Updated position statement on sleeve gastrectomy as a bariatric procedure. ASMBS Clinical Issues Committee. Surg Obes Relat Dis. 2012;8(3):e21-6. doi:10.1016/j.soard.2012.02.001.
Lalor PF, Tucker ON, Szomstein S, et al. Complications after laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2008;4:33–8.
Frezza EE, Reddy S, Gee LL, et al. Complications after sleeve gastrectomy for morbid obesity. Obes Surg. 2009;19:684–7. doi:10.1007/s11695-008-9677-6.
Aurora AR, Khaitan L, Saber AA. Sleeve gastrectomy and the risk of leak: a systematic analysis of 4888 patients. Surg Endosc. 2012;26:1509–15. doi:10.1007/s00464-011-2085-3.
Ojo P, Asiyanbola B, Valin E, et al. Post discharge prophylactic anticoagulation in gastric bypass patient-how safe? Obes Surg. 2008;18:791–6. doi:10.1007/s11695-007-9382-x.
Khoursheed M, Al-Bader I, Al-Asfar F, et al. Therapeutic effect of low-molecular weight heparin and incidence of lower limb deep venous thrombosis and pulmonary embolism after laparoscopic bariatric surgery. Surg Laparosc Endosc Percutan Tech. 2013;23:491–3. doi:10.1097/SLE.0b013e31828e3c92.
Dallal RM, Bailey L, Nahmias N. Back to basics—clinical diagnosis in bariatric surgery: routine drains and upper GI series are unnecessary. Surg Endosc. 2007;21:2268–71.
Alvarez Uslar R, Molina H, Torres O, et al. Total gastrectomy with or without abdominal drains. A prospective randomized trial. Rev Esp Enferm Dig. 2005;97:562–9. Article in English, Spanish.
Kim J, Lee J, Hyung WJ, et al. Gastric cancer surgery without drains: a prospective randomized trial. J Gastrointest Surg. 2004;8:727–32.
Albanopoulos K, Alevizos L, Linardoutsos D, et al. Routine abdominal drains after laparoscopic sleeve gastrectomy: a retrospective review of 353 patients. Obes Surg. 2011;21:687–91. doi:10.1007/s11695-010-0343-4.
Lacy A, Obarzaba A, Pando E, et al. Revisional surgery after sleeve gastrectomy. Surg Laparosc Endosc Percutan Tech. 2010;20:351–6. doi:10.1097/SLE.0b013e3181f62895.
Gagner M, Buchwald JN. Comparison of laparoscopic sleeve gastrectomy leak rates in four staple-line reinforcement options: a systematic review. Surg Obes Relat Dis. 2014;10:713–24. doi:10.1016/j.soard.2014.01.016.
Rosenthal RJ, International Sleeve Gastrectomy Expert Panel, Diaz AA, et al. International sleeve gastrectomy expert panel consensus statement: best practice guidelines based on experience of >12,000 cases. Surg Obes Relat Dis. 2012;8:8–19. doi:10.1016/j.soard.2011.10.019.
Stamou KM, Menenakos E, Dardamanis D, et al. Prospective comparative study of the efficacy of staple-line reinforcement in laparoscopic sleeve gastrectomy. Surg Endosc. 2011;25:3526–30. doi:10.1007/s00464-011-1752-8.
Alley J, Fenton S, Harnisch M, et al. Integrated bioabsorbable tissue reinforcement in laparoscopic sleeve gastrectomy. Obes Surg. 2011;21:1311–5. doi:10.1007/s11695-010-0313-x.
Casella G, Soricelli E, Rizello M, et al. Nonsurgical treatment of staple line leaks after laparoscopic sleeve gastrectomy. Obes Surg. 2009;19:821–6. doi:10.1007/s11695-009-9840-8.
Burgos AM, Braghetto I, Csendes A, et al. Gastric leak after laparoscopic sleeve gastrectomy for obesity. Obes Surg. 2009;19:1672–7. doi:10.1007/s11695-009-9884-9.
Cooper JD. Technique to reduce air leaks after resection of emphysematous lung. Ann Thorac Surg. 1994;57:1038–9.
Pinheiro JS, Correa JL, Cohen RV, et al. Staple line reinforcement with new biomaterial increased burst strength pressure: an animal study. Surg Obes Relat Dis. 2006;2:397–9. discussion 400.
Kasalicky M, Michalsky D, Housova J, et al. Laparoscopic sleeve gastrectomy without an over-sewing of the staple line. Obes Surg. 2008;18:1257–62. doi:10.1007/s11695-008-9635-3.
Iannelli A, Schneck AS, Ragot E, et al. Laparoscopic sleeve gastrectomy as revisional procedure for failed gastric banding and vertical banded gastroplasty. Obes Surg. 2009;19:1216–20. doi:10.1007/s11695-009-9903-x.
Foletto M, Prevedello L, Bernante P, et al. Sleeve gastrectomy as revisional procedure for failed gastric banding or gastroplasty. Surg Obes Relat Dis. 2010;6:146–51. doi:10.1016/j.soard.2009.09.003.
Yazbek T, Safa N, Denis R, et al. Laparoscopic Sleeve Gastrectomy (LSG)—a good bariatric option for failed Laparoscopic Adjustable Gastric Banding (LAGB): a review of 90 patients. Obes Surg. 2013;23:300–5. doi:10.1007/s11695-012-0825-7.
Delgado S, Ibarzabal A, Adelsdorfer C, et al. Transumbilical single port sleeve gastrectomy: initial experience and comparative study. Surg Endosc. 2012;26:1247–53. doi:10.1007/s00464-011-2002-9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Khoursheed, M., Al-Bader, I., Mouzannar, A. et al. Postoperative Bleeding and Leakage After Sleeve Gastrectomy: a Single-Center Experience. OBES SURG 26, 2944–2951 (2016). https://doi.org/10.1007/s11695-016-2215-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2215-z