Abstract
Purpose
Intestinal protozoan parasites are responsible for diarrheal diseases causing significant morbidity and mortality. Entamoeba histolytica is the principle protozoan parasite associated with diarrheal infections. The infection is often associated with inaccessibility to clean drinking water and poor sanitary conditions in low- and middle-income countries including India. A comprehensive systematic review was performed to evaluate a reliable nationwide estimate for prevalence and geographic distribution of amoebiasis in India and the complications associated with it.
Methods
We used the PRISMA guidelines to perform a systematic review and meta-analysis of articles published between the year 2001–2020. Two English language databases PubMed and Web of Science were searched to achieve relevant studies.
Results
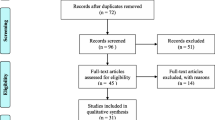
Initial searches resulted in 467 studies out of which 64 eligible articles involving data from 289,659 human subjects from 12 states and 4 union territories were included in the final analysis. Prevalence of amoebiasis ranged from 3-23% in asymptomatic population, 0.64–11% in symptomatic patients and 1–17.5% in HIV-infected patients. Highest prevalence was seen in Tamil Nadu, Andaman Nicobar Island and North East India. Extra intestinal invasion of Entamoeba histolytica leading to complications such as amoebic liver abscess, amoebic colitis, colonic perforation and ameboma were also reported. Such complications have the potential to increase healthcare burden and may prove to be fatal.
Conclusion
Amoebiasis remains a significant public health issue in India responsible for diarrheal diseases causing significant morbidity and mortality. Entamoeba histolytica is the principle protozoan parasite associated with amoebiasis. Public health efforts should be directed towards its control and better diagnostic methods should be employed for distinguishing between pathogenic and non-pathogenic species of Entamoeba.


Similar content being viewed by others
References
https://www.who.int/news-room/fact-sheets/detail/diarrhoeal-disease. Accessed 6 May 2021
Troeger C, Blacker BF, Khalil IA, Rao PC, Cao S, Zimsen SR, Reiner RC Jr (2018) Estimates of the global, regional, and national morbidity, mortality, and aetiologies of diarrhoea in 195 countries: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Infect Dis 18(11):1211–1228
Shirley DAT, Farr L, Watanabe K, Moonah S (2018) A review of the global burden, new diagnostics, and current therapeutics for amebiasis. Open Forum Infect Dis 5(7):ofy161 (US: Oxford University Press)
Carrero JC, Reyes-Lopez M, Serrano-Luna J, Shibayama M, Unzueta J, Leon-Sicairos N, de la Garza M (2020) Intestinal amoebiasis: 160 years of its first detection and still remains as a health problem in developing countries. Int J Med Microbiol 310(1):151358
Pritt BS, Clark CG (2008) Amebiasis. Mayo Clinic Proc 83(10):1154–1160
Stanley SL Jr (2003) Amoebiasis. The lancet 361(9362):1025–1034
https://www.unicef.org/india/what-we-do/clean-drinking-water. Accessed 6 May 2021
Anvikar AR, Dolla C, Dutta S, Rao VG, Gadge VS, Shukla GP, Karforma C (2007) Role of Escherichia coli in acute diarrhoea in tribal preschool children of central India. Paediatr Perinat Epidemiol. https://doi.org/10.1111/j.1365-3016.2007.00892.x
Bisht D, Verma AK, Bharadwaj HH (2011) Intestinal parasitic infestation among children in a semi-urban Indian population. Trop Parasitol 1(2):104–107. https://doi.org/10.4103/2229-5070.86946
Choubisa SL (2009) Amoebiasis among tribals of Rajasthan (India). J Commun Dis 41(1):53–55
Choubisa SL, Jaroli VJ, Choubisa P, Mogra N (2012) Intestinal parasitic infection in Bhil tribe of Rajasthan, India. J Parasitic Dis 36(2):143–148. https://doi.org/10.1007/s12639-012-0151-y
Mirdha BR (2002) Hymenolepis nana: a common cause of paediatric diarrhoea in urban slum dwellers in India. J Trop Pediatr 48(6):331–334. https://doi.org/10.1093/tropej/48.6.331
Verma AK, Verma R, Ahuja V, Paul J (2012) Real-time analysis of gut flora in Entamoeba histolytica infected patients of Northern India. BMC Microbiol 12(1):183. https://doi.org/10.1186/1471-2180-12-183
Mahapatra A, Mohanty N, Behera BK, Dhal S, Praharaj AK (2020) Soil transmitted helminth infections among school going age children of slums from Bhubaneswar, Odisha. Tropical Parasitol 10(1):34–38. https://doi.org/10.4103/tp.TP_30_19
Nath J, Ghosh SK, Singha B, Paul J (2015) Molecular epidemiology of amoebiasis: a cross-sectional study among North East Indian Population. PLoS Negl Trop Dis 9(12):e0004225. https://doi.org/10.1371/journal.pntd.0004225
Nath J, Hussain G, Singha B, Paul J, Ghosh S (2015) Burden of major diarrheagenic protozoan parasitic co-infection among amoebic dysentery cases from North East India: a case report. Parasitology 142(10):1318–1325. https://doi.org/10.1017/S0031182015000669
Subba SH, Singh TS (2020) Study on the prevalence of intestinal parasitic infections and the assessment of the efficacy of albendazole in soil-transmitted helminths in school-going children in East Sikkim. Trop Parasitol 10(1):18–23. https://doi.org/10.4103/tp.TP_62_18
Langbang D, Dhodapkar R, Parija S, Premarajan K, Rajkumari N (2019) Prevalence of intestinal parasites among rural and urban population in Puducherry, South India - a community-based study. J Family Med Primary Care 8(5):1607. https://doi.org/10.4103/jfmpc.jfmpc_196_19
Rayan P, Verghese S, Mcdonnell P (2010) Geographical location and age affect the incidence of parasitic infestations in school children. Indian J Pathol Microbiol 53(3):504. https://doi.org/10.4103/0377-4929.68292
Dhanabal J, Selvadoss PP, Muthuswamy K (2014) Comparative study of the prevalence of intestinal parasites in low socioeconomic areas from South Chennai, India. J Parasitol Res 2014:1–7. https://doi.org/10.1155/2014/630968
Gopalakrishnan S, Eashwar V, Muthulakshmi M, Geetha A (2018) Intestinal parasitic infestations and anaemia among urban female school children in Kancheepuram district, Tamil Nadu. J Family Med Primary Care 7(6):1395–1400. https://doi.org/10.4103/jfmpc.jfmpc_89_18
Biswal M, Khurana S, Taneja N, Kaur T, Samanta P, Malla N, Sharma M (2012) Is routine medical examination of food handlers enough to ensure food safety in hospitals? J Commun Dis 44(3):139–144
Shubha D, Fatima F (2011) A coprological survey for assessing intensity of parasitic infection in school children: Cross-sectional study. Trop Parasitol 1(2):88–93. https://doi.org/10.4103/2229-5070.86940
Kumar CS, Anand Kumar H, Sunita V, Kapur I (2003) Prevalence of anaemia and worm infestation in school going girls at Gulbarga, Karnataka. Indian Paediatrics 40(1):70–72
Takalkar A, Madhekar N, Kumavat A, Bhayya S (2010) Prevalence of intestinal parasitic infections amongst food handlers in hotels and restaurants in Solapur city. Indian J Public Health 54(1):47. https://doi.org/10.4103/0019-557x.70557
Thamizhmani R, Sugunan AP, Raghvan PR, Vijayachari P (2016) Intestinal parasitic infestation among paediatric diarrhoea patients attending hospitals in Port Blair, Andaman and Nicobar Islands. J Parasit Dis 41(2):584–589. https://doi.org/10.1007/s12639-016-0814-1
Uppal B, Perween N, Aggarwal P, Kumar SK (2015) A comparative study of bacterial and parasitic intestinal infections in India. J Clin Diagn Res 9(3):DC01–DC04
Praharaj I, Kang G, Sarkar R, Ajjampur SR, Roy S (2017) Temporal trends of intestinal parasites in patients attending a tertiary care hospital in south India: a seven-year retrospective analysis. Indian J Med Res 146(1):111. https://doi.org/10.4103/ijmr.ijmr_1236_14
Kaur R, Rawat D, Kakkar M, Uppal B, Sharma VK (2002) Intestinal parasites in children with diarrhea in Delhi, India. The Southeast Asian J Trop Med Public Health 33(4):725–729
Mukherjee A, Chowdhury P, Bhattacharya M, Ghosh M, Rajendran K, Ganguly S (2009) Hospital-based surveillance of enteric parasites in Kolkata. BMC Res Notes 2(1):110. https://doi.org/10.1186/1756-0500-2-110
Roy M, Singha B, Dhar D, Roychoudhury S (2019) Prevalence of Giardia intestinalis with other co-infecting parasites in Barak Valley, Assam, India: a molecular approach. J Parasit Dis 43(3):426–442. https://doi.org/10.1007/s12639-019-01107-5
Parija SC, Khairnar K (2005) Entamoeba moshkovskii and Entamoeba dispar-associated infections in pondicherry, India. J Health Popul Nutr 23(3):292–295
Saurabh K (2017) Spectrum of Parasitic infections in patients with diarrhea attending a tertiary care hospital in Western Rajasthan, India. J Clin Diagn Res https://doi.org/10.7860/jcdr/2017/29001.10346
Yogyata M, Binita S (2011) Prevalence of intestinal parasites at Ujjain, Madhya Pradesh, India: five-year study. Afr J Microbiol Res 5(18):2711–2714. https://doi.org/10.5897/ajmr11.459
Khairnar K, Parija SC, Palaniappan R (2007) Diagnosis of intestinal amoebiasis by using nested polymerase chain reaction-restriction fragment length polymorphism assay. J Gastroenterol 42(8):631–640. https://doi.org/10.1007/s00535-007-2080-6
Janagond AB, Sasikala G, Agatha D, Ravinder T, Thenmozhivalli PR (2013) Enteric parasitic infections in relation to diarrhoea in HIV infected individuals with CD4 T cell counts <1000 Cells/μl in Chennai, India. J Clin Diagn Res 7(10):2160–2162. https://doi.org/10.7860/JCDR/2013/5837.3458
Jayalakshmi J, Appalaraju B, Mahadevan K (2008) Evaluation of an enzyme-linked immunoassay for the detection of Cryptosporidium antigen in fecal specimens of HIV/AIDS patients. Indian J Pathol Microbiol 51(1):137–138. https://doi.org/10.4103/0377-4929.40427
Mohandas S, R., Sud, A., & Malla, N. (2002) Prevalence of intestinal parasitic pathogens in HIV-seropositive individuals in Northern India. Jpn J Infect Dis 55(3):83–84
Mohanty I, Panda P, Sahu S, Dash M, Narasimham MV, Padhi S, Parida B (2013) Prevalence of isosporiasis in relation to CD4 cell counts among HIV-infected patients with diarrhea in Odisha, India. Adv Biomed Res 2:61. https://doi.org/10.4103/2277-9175.115810
Prasad N, Nag VL, Dhole TN, Ayyagari A (2000) Identification of enteric pathogens in HIV-positive patients with diarrhoea in Northern India. J Health Popul Nutr 18(1):23–26
Ramakrishnan K, Shenbagarathai R, Uma A, Kavitha K, Rajendran R, Thirumalaikolundusubramanian P (2007) Prevalence of intestinal parasitic infestation in HIV/AIDS patients with diarrhea in Madurai City, South India. Jpn J Infect Dis 60(4):209–210
Reddy SG, Ali SY, Khalidi A (2016) Study of infections among human immunodeficiency virus/acquired immunodeficiency syndrome patients in Shadan Hospital, Telangana, India. Indian J Sex Transm Dis AIDS 37(2):147–150. https://doi.org/10.4103/0253-7184.192122
Shah S, Kongre V, Kumar V, Bharadwaj R (2016) A Study of parasitic and bacterial pathogens associated with Diarrhea in HIV-Positive patients. Cureus. https://doi.org/10.7759/cureus.807
Kulkarni SV, Kairon R, Sane SS, Padmawar PS, Kale VA, Thakar MR, Mehendale SM, Risbud AR (2009) Opportunistic parasitic infections in HIV/AIDS patients presenting with diarrhoea by the level of immunesuppression. Indian J Med Res 130(1):63–66
Deepika K, Rajkumari N, Liji A, Parija SC, Hamide A (2017) Multiple parasitic and viral infections in a patient living with HIV/AIDS on antiretroviral therapy. Indian J Med Microbiol 35(3):432–435. https://doi.org/10.4103/ijmm.ijmm_16_304
Vignesh R, Balakrishnan P, Shankar EM, Murugavel KG, Hanas S, Cecelia AJ, Thyagarajan SP, Solomon S, Kumarasamy N (2007) High proportion of isosporiasis among HIV-infected patients with diarrhea in southern India. Am J Trop Med Hyg 77(5):823–824
Nath J, Banyal N, Gautam D, Ghosh S, Singha B, Paul J (2015) Systematic detection and association of Entamoeba species in stool samples from selected sites in India. Epidemiol Infect 143(1):108–119. https://doi.org/10.1017/S0950268814000715
Kulkarni S, Patsute S, Sane S, Chandane M, Vidhate P, Risbud A (2013) Enteric pathogens in HIV infected and HIV uninfected individuals with diarrhea in Pune. Trans R Soc Trop Med Hyg 107(10):648–652. https://doi.org/10.1093/trstmh/trt067
Shenoy VP, Vishwanath S, Indira B, Rodrigues G (2010) Hepato-pulmonary amebiasis: a case report. Braz J Infect Dis 14(4):372–373. https://doi.org/10.1016/s1413-8670(10)70077-5
Chaudhary S, Noor MT, Jain S, Kumar R, Thakur BS (2016) Amoebic liver abscess: a report from central India. Trop Doct 46(1):12–15. https://doi.org/10.1177/0049475515592283
Khairnar K, Parija SC (2008) Detection of Entamoeba histolytica DNA in the saliva of amoebic liver abscess patients who received prior treatment with metronidazole. J Health Popul Nutr 26(4):418–425. https://doi.org/10.3329/jhpn.v26i4.1883
Kumar Jha A, Jha P, Chaudhary M, Kumar S, Prakash V, Mohan Dayal V (2019) The relation of toddy (palm wine) intake to amoebic liver abscess in a predominantly toddy-drinking population: a cross-sectional study. Trop Doct 49(3):197–200. https://doi.org/10.1177/0049475519840242
Makkar RP, Sachdev GK, Malhotra V (2003) Alcohol consumption, hepatic iron load and the risk of amoebic liver abscess: a case-control study. Intern Med 42(8):644–649. https://doi.org/10.2169/internalmedicine.42.644
Singh A, Banerjee T, Kumar R, Shukla SK (2019) Prevalence of cases of amebic liver abscess in a tertiary care centre in India: a study on risk factors, associated microflora and strain variation of Entamoeba histolytica. PLoS ONE. https://doi.org/10.1371/journal.pone.0214880
Singh R, Adhikari DR, Patil BP, Talathi NR, Hanamshetti SR, Joshi RM (2011) Amoebic liver abscess: an appraisal. Int Surg 96(4):305–309. https://doi.org/10.9738/cc9.1
Jain M, Jain J, Gupta S (2016) Amebic liver abscess in children—experience from Central India. Indian J Gastroenterol 35(3):248–249. https://doi.org/10.1007/s12664-016-0669-5
Naveed S, Gupta V, Kapoor M, Quari H, Altaf A, Para M (2014) Liver abscess in the tropics: an experience from Jammu. Psychol Sci 59(3):516–522. https://doi.org/10.1111/j.1467-9280.2009.02325.x
Rani R, Murthy RS, Bhattacharya S, Ahuja V, Rizvi MA, Paul J (2006) Changes in bacterial profile during amebiasis: demonstration of anaerobic bacteria in ALA pus samples. Am J Trop Med Hyg 75(5):880–885
Singh V, Bhalla A, Sharma N, Mahi SK, Lal A, Singh P (2008) Pathophysiology of jaundice in amoebic liver abscess. Am J Trop Med Hyg 78(4):556–559
Sodhi KS, Ojili V, Sakhuja V, Khandelwal N (2008) Hepatic and inferior vena caval thrombosis: vascular complication of amebic liver abscess. J Emerg Med 34(2):155–157. https://doi.org/10.1016/j.jemermed.2007.05.045
Muzaffar J, Madan K, Sharma MP, Kar P (2006) Randomized, single-blind, placebo-controlled multicenter trial to compare the efficacy and safety of metronidazole and satranidazole in patients with amebic liver abscess. Dig Dis Sci 51(12):2270–2273. https://doi.org/10.1007/s10620-006-9111-7
Zaman M, Chowdhary K, Kaur G, Shah A (2018) Amoebic colonic perforation presenting as peritonitis in emergency, incidence and outcome: our experience. Maedica 13(1):51–54
Jain BK, Garg PK, Kumar A, Mishra K, Mohanty D, Agrawal V (2013) Colonic perforation with peritonitis in amoebiasis: a tropical disease with high mortality. Trop Gastroenterol 34(2):83–86. https://doi.org/10.7869/tg.2012.102
Singla K, Mahajan G, Agarwal S (2012) Role of histopathological examination in nontraumatic perforation of colon. Trop Gastroenterol 33(4):265–269. https://doi.org/10.7869/tg.2012.68
Chaturvedi R, Gupte PA, Joshi AS (2015) Fulminant amoebic colitis: a clinicopathological study of 30 cases. Postgrad Med J 91(1074):200–205. https://doi.org/10.1136/postgradmedj-2014-132597
Singh R, Balekuduru A, Simon EG, Alexander M, Pulimood A (2015) The differentiation of amebic colitis from inflammatory bowel disease on endoscopic mucosal biopsies. Indian J Pathol Microbiol 58(4):427–432. https://doi.org/10.4103/0377-4929.168880
Beg MY, Bains L, Mahajan R, Lal P, Choudhury S, Kumar NP, Pal V (2020) Fulminant necrotising amoebic colitis of whole of large bowel: a rare complication of a common infectious disease. Case Rep Infect Dis 2020:1–6. https://doi.org/10.1155/2020/8845263
Boopathy V, Alexander T, Balasubramanian P, Phansalkar M (2014) Amoeboma: resurfacing of a vanishing illness. Case Rep. https://doi.org/10.1136/bcr-2013-202616
Fernandez MC, Verghese S, Bhuvaneswari R, Elizabeth SJ, Mathew T, Anitha A, Chitra AK (2002) A comparative study of the intestinal parasites prevalent among children living in rural and urban settings in and around Chennai. J Commun Dis 34(1):35–39
Kataria H, Seth A, Attri AK, Singh Punia RP (2018) Ameboma of colon simulating colonic adenocarcinoma. Int J Appl Basic Med Res 8(1):42–44. https://doi.org/10.4103/ijabmr.IJABMR_285_17
Jaiswal V, Ghoshal U, Mittal B, Dhole TN, Ghoshal UC (2014) Association between allelic variation due to short tandem repeats in tRNA gene of Entamoeba histolytica and clinical phenotypes of amoebiasis. Acta Trop 133:1–7. https://doi.org/10.1016/j.actatropica.2014.01.009
Salam N, Mustafa S, Hafiz A, Chaudhary AA, Deeba F, Parveen S (2018) Global prevalence and distribution of cases of coinfection of malaria, dengue and chikungunya: a systematic review. BMC Public Health 18(1):710
Uman LS (2011) Systematic reviews and meta-analyses. J Canad Acad Child Adolesc Psychiatr 20(1):57
Salam N, Azam S (2017) Prevalence and distribution of soil-transmitted helminth infections in India. BMC Public Health 17(1):1–12
Nath J, Singha B, Paul J, Ghosh SK (2018) Diagnosis and epidemiology of amoebiasis in India. Curr Sci 114(10):2045–2052
Singh A, Banerjee TD, Khan U, Shukla SK (2021) Epidemiology of clinically relevant Entamoeba spp. (E histolytica/dispar/moshkovskii/ bangladeshi): a cross sectional study from North India. PLoS Negl Trop Dis 15(9):e0009762
Karp CL, Auwaerter PG (2007) Coinfection with HIV and tropical infectious diseases. I. Protozoal pathogens. Clin Infect Dis 45(9):1208–1213
Funding
No funding was received for this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gupta, P., Singh, K.K., Balodhi, A. et al. Prevalence of Amoebiasis and Associated Complications in India: A Systematic Review. Acta Parasit. 67, 947–961 (2022). https://doi.org/10.1007/s11686-022-00547-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11686-022-00547-z