Abstract
Introduction
Currently, there are no reports of diaphyseal femoral fracture equivalent to atypical femoral fractures (AFFs) in patients receiving long-term hemodialysis (HD).
Case report
A 56-year-old Japanese man receiving long-term HD for 34 years was admitted to our hospital due to a delay in postoperative healing. The patient began maintenance hemodialysis at 22 years of age. The patient then underwent surgical parathyroidectomy (PTX) for secondary hyperparathyroidism at 43 years of age, which resulted in decreased levels of parathyroid hormone (PTH). Thereafter, this patient’s serum 1,25(OH)2 D3 level was very low because active vitamin D3 derivative was not administered. At 54 years of age, a transverse fracture of the femoral shaft equivalent to AFF occurred. Surgery with open reduction and internal fixation using intramedullary nailing was performed; however, the delay of postoperative healing continued for 16 months. A left iliac crest bone biopsy was performed and showed osteoid-like lesion and an increase of woven bone. The patient received active vitamin D3 derivative and recombinant human PTH (1–34) derivative. Twenty-nine months after the first surgery, a reoperation was performed. Simultaneously, a right iliac crest bone biopsy was performed. Bone morphometrical improvement was confirmed. Six months after resurgery, the bone union was achieved.
Summary
Severe vitamin D3 deficiency and decreased levels of PTH may induce a higher osteoid state and an increase of woven bone, which may then attribute to the development of diaphyseal femoral fracture and impairment of postoperative bone healing. It is hypothesized that treatment with active vitamin D3 and teriparatide acetate may be a therapeutic option via the accelerated formation of lamellar bone for refractory diaphyseal femoral fracture of long-term dialysis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mineral abnormalities such as renal osteodystrophy (ROD) are common in patients with chronic kidney disease (CKD) [1]. Previously, the optimal diagnostic test for specific classification of ROD was bone biopsy with bone histomorphometry [2]. Recent studies, however, have shown that serological bone turnover markers are also a useful tool for predicting bone histopathology in patients suffering CKD [1, 3, 4]. The evaluation of such markers is now considered to be essential as it provides vital information required to determine treatment plans for these patients.
Long-term use of bisphosphonates (BPs) has been reported to be the primary cause of femoral stress fractures, also known as atypical femoral fractures (AFF) [5]. The pathogenesis of AFF, however, remains unclear and has been reported to be developed on non dialysis patients. Currently, there are no reports investigating diaphyseal femur fractures in a radiograph equivalent to AFF in patients suffering CKD receiving long-term hemodialysis (HD). In the present study, a patient on long-term HD for 34 years with a history of surgical parathyroidectomy (PTX) presented with poor postoperative healing after experiencing diaphyseal femur fractures. Furthermore, this patient experienced severe vitamin D3 deficiency during long-term HD and decreased levels of parathyroid hormone (PTH). We report that bone histomorphometrical analysis in conjunction with evaluation of serological bone turnover markers was able to clarify the pathogenesis of this patient’s bone disease.
Case presentation
A-56-year-old Japanese man on long-term HD for 34 years was admitted to our hospital for additional treatment for diaphyseal femoral fracture and delay in postoperative healing.
The patient began maintenance dialysis at the age of 22; however, the primary renal disease was unknown. Surgical PTX without autotransplantation was performed for secondary hyperparathyroidism at the age of 43. Thereafter, the patient’s level of intact parathyroid hormone (PTH) was less than 10 pg/mL. At that time, the patient was receiving hemodialysis three times a week for four hours by using dialysate Ca concentration of 3.0 mEq/L and was being prescribed sevelamer hydrochloride (5.25 g/day) and lanthanum carbonate hydrate (0.75 g/day) to treat hyperphosphatemia, precipitated calcium carbonate (2.5 g/day) to treat hypocalcemia, and menatetrenone (15 mg/day) as adjunctive therapy for osteoporosis. However, vitamin D3 derivative had not been prescribed.
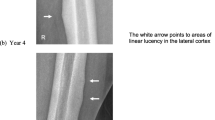
At the age of 54, the patient felt left thigh pain and experienced walking difficulty without any precipitating cause but did not fall. This pain and walking difficulty were worsening each day. One week later, radiograph showed a transverse fracture of the femoral shaft with spike formation on the postero-medial side, and left diaphyseal femoral fracture was diagnosed (Fig. 1 (1)). The patient underwent open reduction and antegrade surgery for internal fixation, using intramedullary nailing. Three weeks after surgery, partial load was added, and 6 weeks after surgery, full weight load was added. However, this patient still could not walk due to pain, and radiographs showed delayed bone union (Fig. 1 (2)). Sixteen months after this first surgery, postoperative healing was still not achieved. Therefore, the patient was admitted to our hospital for further therapeutic options.
Frontal and lateral radiograph of the left femur. (1), left femoral shaft transverse fracture; (2), bone fixation failure with pseudarthrosis; (3), open reduction and fixation performed using an angular stability plate associated with autogenous bone graft from the patient’s left iliac bone; (4), successful bone union
On admission, the patient was 163.9 cm tall and weighed 63.0 kg. Laboratory data (Table 1) was as follows: calcium, 9.0 mg/dL; phosphate, 6.0 mg/dL; alkaline phosphatase (ALP), 193 IU/L (JSCC method, normal range 117 to 350); bone ALP (BAP), 8.8 μg/L (normal range 3.8 to 22.6); tartrate-resistant acid phosphatase-5b (TRAP-5b), 267 mU/dL (normal range 250 to 760); intact PTH, 9 pg/mL (normal range 25 to 117), whole PTH, 12 pg/mL (normal range 9–39); 25-hydroxyvitamin D, 11.5 ng/mL (normal > 20); 1.25-dihydroxyvitamin D3, < 4.0 pg/mL (normal range 20–60); osteocalcin, 50.1 ng/mL (normal range 8–33); and undercarboxylated osteocalcin (ucOC), 16.0 ng/mL (normal < 4.5).
Clinical course 1
Open reduction and fixation were performed using angular stability plate associated with autogenous bone graft from the patient’s left iliac bone (Fig. 1 (3)). Postsurgical therapy was then conducted for the affected limb, using non-weight bearing methods. Simultaneously, biopsy of the left iliac crest bone was performed to determine the pathogenesis of both diaphyseal femur fractures and impaired bone healing. Bone histomorphometrical analysis was performed by Mrs. Akemi Ito of the Ito Bone Science Institute (Niigata, Japan). Tetracycline double labeling was not performed, because the patient hoped emergent surgery.
First bone histomorphometric examination
The frame of the cortical bone was thin, and the majority of the trabecular bone consisted of cancellous bone. Bone histomorphometric analysis for cancellous bone was measured (Table 2). Trabecular bone volume (BV/TV), trabecular thickness (Tb.Th), and trabecular unit wall thickness (Th.W) were increased by 32.49%, 160.4 μm, and 48.33 μm, respectively, compared with an age-matched reference range according to the report by Reccker RR et al. [6]. Woven bone (Wo.V/BV) of the cancellous bone occupied 2.47% of bone volume, while cortical bone near the cancellous bone occupied 35.3% of bone volume (Fig. 2 (1)). All osteoid markers including osteoid volume to tissue volume (OV/TV), osteoid volume to bone volume (OV/BV), osteoid surface (OS/BS), and osteoid thickness (O.Th) were increased by 4.71%, 14.5%, 66.56%, and 17.45 μm, respectively (Fig. 2 (2)). Fibrous tissue volume to total volume (Fb.V/TV) and eroded surface to bone surface (ES/BS) were increased by 1.08% and 29.98%, respectively. Osteoblasts (Obs) were increased in number by 33.48/mm2 and showed cuboidal cytoplasm indicative of an increase in activity. Multinucleated osteoclasts (N.Mu.Ocs) were located in Howship’s lacuna (resorption bay) with deep infoldings, and osteoclast surface to bone surface (Oc.s/BS) was increased by 13.22% with an increase in both number (2.47/mm2) and size.
Natural light microscopic analysis. (1), the 1st iliac cortical bone near a cancellous bone section, with woven bone in the cortical bone near cancellous bone (yellow zone). The 2nd iliac cortical bone near cancellous bone with a decrease in woven bone in the cortical bone near cancellous bone and formation of lamellar bone; (2), natural light and fluorescent microscopic analysis of the 1st iliac trabecular bone section. An increase in the amount of osteoid, along with increased thickness of osteoid seam width, and a low calcification area on the bone surface and in the bone, was observed. The 2nd iliac trabecular bone section. The trabeculae bone consisted of minimodeling with minimal to no calcification
Diagnosis
The patient was diagnosed with osteitis fibrosa due to Fb.V/TV of 1.08% (> 0.5%) and OV/BV of 14.5% (< 15%) according to Sherrard’s classification of ROD [7]. This patient’s osteoid volume (OV/BV) of 14.5% did not reach to limit of osteomalacia (15%) but was increased compared with the normal range value (4.9 ± 1.2) [8]. Osteomalacia-like lesion was definite. Increased activity of both Obs and Ocs was also noted. Fb.V/TV of 1.08% (> 0.5%) and an increase of woven bone imply osteitis fibrosa, which suggested hyperparathyroidism due to higher serum levels of intact PTH [9]; however, the patient’s serum levels of intact PTH were very low with post-PTX. Although this pathogenesis is complex, 1,25-dihydroxyvitamin D3 deficiency–related osteomalacia-like lesion and an increase of woven bone were considered to be responsible for the delay in postoperative healing.
Clinical course 2
The patient began treatment with active vitamin D3 derivative (alfacalcidol) at a dose of 0.5 μg/day, in conjunction with recombinant human PTH (1–34) derivative (teriparatide acetate) at 56.5 μg/week, and continues being used for 18 months until today. Nine months later, bone union was still not achieved. A third operation was then performed to decorticate the pseudarthrosis associated with the autogenous bone graft from the patient’s right iliac bone. Simultaneously, bone rebiopsy of the right iliac crest was performed 29 months after the first surgery.
Second bone histomorphometric analysis
Compared with the first bone biopsy, BV/TV, Tb.Th, and W.Th were decreased to 13.71%, 72.42 μm, and 29.01 μm, respectively. However, trabecular bone consisted of predominantly lamellar bone, and woven bone of cancellous bone was decreased from 2.47 to 1.3%. Furthermore, woven bone volume of cortical bone near cancellous bone was decreased from 35.3 to 9.3% (Fig. 2 (1)). This may indicate that abnormal woven bone was decreased, and consequently, total bone volume was decreased, while healthy lamellar bone was increased.
Compared with the first biopsy, OV/TV, OV/BV, OS/BS, and O.Th improved to 1.15%, 8.36%, 24.73%, and 12.18 μm, respectively. In addition, bone formation by minimodeling, characterized by the lack of precedent bone erosion by osteoclasts, was visible (Fig. 2 (2)) [10]. Both Fb.V/TV and ES/BS decreased by 0.04% and 12.26%, respectively. The Obs had flattened cytoplasm suggesting low activity, and their numbers had decreased to 2.76/mm2. Multinucleated osteoclasts (N.Mu.Oc/BS) and osteoclast surface (Oc.s/BS) were decreased (0.26/mm2 and 2.01%, respectively), and osteoclast size was decreased. An improvement in bone histomorphometric was confirmed.
Biochemically, the bone turnover markers, osteocalcin and BAP, increased in response to treatment compared with the first operation. Serum intact PTH and whole PTH remained low. Also, compared with the first surgery, 1,25-dihydroxyvitamin D3 was increased.
Six months after the third surgery, the bone fracture was in union (Fig. 1 (4)).
Discussion
Chronic kidney disease–mineral and bone disorder (CKD–MBD) is a complex disorder of both bone and mineral metabolism. Several studies have shown that the risk factors associated with AFF include glucocorticoid, rheumatoid arthritis, and femoral curvature [11, 12]. Currently, ROD is associated with bone fragility and ROD due to long-term HD is considered to be the primary cause of stress fractures [13, 14]. Therefore, it is necessary to accurately evaluate ROD and diagnose the specific type of ROD. According to histological features of bone biopsies [7], ROD is classified as follows: osteitis fibrosa, osteomalacia, and a mixed, mild, or adynamic disease. Previous studies have reported that circulating levels of intact PTH and bone turnover markers are useful tools for predicting bone histopathology [1, 3, 4]. Both BAP and intact PTH are directly correlated with bone formation parameters, and BAP levels are positively correlated with serum levels of intact PTH in patients undergoing HD [1, 4]. In addition, tartrate-resistant acid phosphatase 5b (TRAP-5b) has been reported to be a marker of bone resorption in patients receiving long-term HD [3].
The patient in the current investigation had low levels of intact PTH (< 10 pg/mL) following PTX. This low level of intact PTH continued for 14 years post-PTX. In this particular case, the presence of adynamic bone would be expected, as adynamic bone is caused by hypoparathyroidism. Hypoparathyroidism is typically characterized by hypocellular bone surfaces and markedly reduced bone remodeling. However, it was surprising to find osteitis fibrosa in the first bone histomorphology analysis of this case, indicated by an OV/BV of 14.5% (< 15.0%) and Fb.V/TV of 1.08% (> 0.5%), as osteitis fibrosa is caused primarily by hyperparathyroidism [15]. In addition, the patient had very low serum levels of 1,25-dihydroxyvitamin D3. Consequently, it was speculated that severe vitamin D3 deficiency in combination with low serum levels of intact PTH following total PTX may have contributed to the bone abnormalities and pseudarthrosis formation, as characterized by postoperative healing failure in this patient. Such speculations are supported by findings of previous, similar case studies [16, 17]. In an attempt to improve postoperative healing, the patient was administered active vitamin D3 derivative, to address vitamin D3 deficiency, and recombinant human parathyroid hormone (1–34) derivative, to address low postoperative PTH levels.
A common issue among patients undergoing long-term HD is secondary hyperparathyroidism. While considerable advances in medical therapy for secondary hyperparathyroidism have been made, PTX remains the dominant therapeutic tool to address this problem. When compared with other surgical therapies, surgical PTX is considered the superior choice to prevent recurrence of hyperparathyroidism [18]. However, PTX can induce hypocalcaemia and adynamic bone disease [19, 20], and currently, there is no appropriate pharmacotherapy for low levels of PTH following surgical PTX.
Diaphyseal femoral stress fracture or AFF is predominantly caused by long-term treatment with BPs [21]. BPs are potent inhibitors of osteoclast-mediated bone resorption. Long-term use of BPs leads to an accumulation of bone microdamage and suppression of bone turnover, both of which may attribute to AFF. It has been shown that the BP, alendronate, can inhibit normal repair of bone microdamage and cause an accumulation of microdamage [22, 23]. Finally, a previous report suggested that the presence of osteoclasts and resorption were increased in bone biopsies of patients currently being treated with BPs [24]. There was not the report of diaphyseal femoral fracture on patients receiving long-term HD thus far, although femoral neck fracture has been reported.
A previous study has reported the beneficial effects of the recombinant human PTH (1–34), teriparatide, in bone healing following surgery due to AFF [25]. Several studies have also shown the beneficial effects of teriparatide in regard to bone healing in patients undergoing long-term, chronic HD [26]. Low-frequency teriparatide administration has been reported to result in the formation of thicker trabeculae via bone remodeling and minimodeling in young adult male mice [27]. Minimodeling has been reported to have a close relation with bone reformation in hypoparathyroid patients [10]. The findings of the present investigation support these earlier reports, as the second bone biopsy of the patient showed that treatment with teriparatide led to the trabeculae consisting of lamellar bone and minimodeling.
Osteitis fibrosa has been reported to being developed on patients with very high PTH levels. Sherrard et al. reported that fibrous volume (Fb.V/TV) of 57 patients with osteitis fibrosa due to very high PTH levels was 2.2 ± 0.3(%) [7]. Compared with their report, Fb.V/TV of our patient showed lower value with 1.08% and was near normal limit of 0.5%. Originally, dialysis patients with low serum PTH levels will result in adynamic bone when vitamin D3 is supplemented. However, we believe that the continuation of severe vitamin D3 deficiency in combination with low serum levels of intact PTH induces an increase of osteoid due to mineralization loss and may induce an inappropriate activation of osteoclast and osteoblast leading to mild osteitis fibrosa.
Osteocalcin and ucOC are sensitive markers of bone formation, and these two markers’ value of this patient was always high compared with normal range and increased parallel to treatment with active vitamin D3 derivative and recombinant human PTH (1–34) derivative. This indicates that bone formation by osteoblast was progressing surely. Osteomalacia is a disease characterized by an increase of unmineralized osteoid volume, which is developed by osteoblast, but cannot be mineralized primarily due to severe vitamin D3 deficiency. Higher level of osteocalcin and ucOC of this patient at first biopsy imply that osteoid formation by osteoblast was progressing. And after treatment with active vitamin D3 derivative and recombinant human PTH (1–34) derivative, osteoid is mineralized by using active vitamin D3 derivative, and bone formation by osteoblast is accelerated by using recombinant human PTH (1–34) derivative and resulted in lamellar bone formation.
In conclusion, severe vitamin D3 deficiency for long-term HD treatment, and a decrease in serum PTH levels following surgical PTX, may induce an increase in osteoid volume and woven bone, ultimately resulting in diaphyseal femur fracture and impaired bone healing. Daily treatment with active vitamin D3 and weekly Intermittent PTH stimulation by using teriparatide acetate may be a potential therapeutic option via the accelerated formation of lamellar bone for refractory diaphyseal femur fracture in a patient receiving HD for a long period of time.
Abbreviations
- AFF:
-
Atypical femoral fracture
- BAP:
-
Bone alkaline phosphatase
- BPs:
-
Bisphosphonates
- BV/TV:
-
Trabecular bone volume to total volume
- CKD:
-
Chronic kidney disease
- CKD–MBD:
-
Chronic kidney disease–mineral and bone disorder
- ES/BS:
-
Eroded surface to bone surface
- Fb.V/TV:
-
Fibrous tissue volume to total volume
- HD:
-
Hemodialysis
- N.Mu.Oc/BS:
-
Multinucleated osteoclasts to bone surface
- Obs:
-
Osteoblasts
- Oc.s/BS:
-
Osteoclast surface to bone surface
- OS/BS:
-
Osteoid surface to bone surface
- O.Th:
-
Osteoid thickness
- OV/BV:
-
Osteoid volume to bone volume
- OV/TV:
-
Osteoid volume to tissue volume
- PTH:
-
Parathyroid hormone
- PTX:
-
Parathyroidectomy
- ROD:
-
Renal osteodystrophy
- Tb.Th:
-
Trabecular thickness
- Th.W:
-
Trabecular unit wall thickness
- TRACP-5b:
-
Tartrate-resistant acid phosphatase 5b
- ucOC:
-
Undercarboxylated osteocalcin
- Wo.Md.BV:
-
Woven and mineralized bone volume
- Wo.V/BV:
-
Woven bone volume to bone volume
References
Sprague SM, Bellorin-Font E, Jorgetti V, Carvalho AB, Malluche HH, Ferreira A, D’Haese PC, Drüeke TB, Du H, Manley T, Rojas E, Moe SM (2016) Diagnostic accuracy of bone turnover markers and bone histology in patients with CKD treated by dialysis. Am J Kidney Dis 67(4):559–566
Moe S, Drüeke T, Cunningham J, Goodman W, Martin K, Olgaard K, Ott S, Sprague S, Lameire N, Eknoyan G (2006) Definition, evaluation, and classification of renal osteodystrophy: a position statement from Kidney Disease: Improving Global Outcomes (KDIGO). Kidney Int 69(11):1945–1953
Shidara K, Inaba M, Okuno S, Yamada S, Kumeda Y, Imanishi Y, Yamakawa T, Ishimura E, Nishizawa Y (2008) Serum levels of TRAP5b, a new bone resorption marker unaffected by renal dysfunction, as a useful marker of cortical bone loss in hemodialysis patients. Calcif Tissue Int 82(4):278–287
Ureña P, Hruby M, Ferreira A, Ang KS, de Vernejoul MC (1996) Plasma total versus bone alkaline phosphatase as markers of bone turnover in hemodialysis patients. J Am Soc Nephrol 7(3):506–512
Shane E, Burr D, Abrahamsen B, Adler RA, Brown TA, Cheung AM, Cosman F, Curtis JR, Dell R, Dempster DW, Ebeling PR, Einhorn TA, Genant HK, Geusens P, Klaushofer K, Lane JM, McKiernan F, McKinney R, Ng A, Nieves J, O’Keefe R, Papapoulos S, Howe TS, van der Meulen MC, Weinstein RS, Whyte MP (2014) Atypical subtrochanteric and diaphyseal femoral fractures: second report of a task force of the American Society for Bone and Mineral Research. J Bone Miner Res 29(1):1–23
Recker RR, Kimmel DB, Parfitt MA, Davies KM, Keshawarz N, Hinders S (1988) Static and tetracycline-based bone histomorphometric data from 34 normal postmenopausal females. J Bone Miner Res 3(2):133–144
Sherrard DJ, Hercz G, Pei Y, Maloney NA, Greenwood C, Manuel A, Saiphoo C, Fenton SS, Segre GV (1993) The spectrum of bone disease in end-stage renal failure--an evolving disorder. Kidney Int 43(2):436–442
Bhan A, Qiu SJ, Rao SD (2018) Bone histomorphometry in the evaluation of osteomalacia. Bone Rep 8:124–135
Al-Shoha A, Qiu S, Palnitkar S, Rao DS (2009) Osteomalacia with bone marrow fibrosis due to severe vitamin D deficiency after a gastrointestinal bypass operation for severe obesity. Endocr Pract 15:528–533
Ubara Y, Tagami T, Nakanishi S, Sawa N, Hoshino J, Suwabe T, Katori H, Takemoto F, Hara S, Takaichi K (2005) Significance of minimodeling in dialysis patients with adynamic bone disease. Kidney Int 68(2):833–839
Lim SJ, Yeo I, Yoon PW, Yoo JJ, Rhyu KH, Han SB, Lee WS, Song JH, Min BW, Park YS (2018) Incidence, risk factors, and fracture healing of atypical femoral fractures: a multicenter case-control study. Osteoporos Int 29(11):2427–2435
Sasaki S, Miyakoshi N, Hongo M, Kasukawa Y, Shimada Y (2012) Low-energy diaphyseal femoral fractures associated with bisphosphonate use and severe curved femur: a case series. J Bone Miner Metab 30(5):561–567
Pimentel A, Ureña-Torres P, Zillikens MC, Bover J, Cohen-Solal M (2017) Fractures in patients with CKD-diagnosis, treatment, and prevention: a review by members of the European Calcified Tissue Society and the European Renal Association of Nephrology Dialysis and Transplantation. Kidney Int 92(6):1343–1355
Hiramatsu R, Ubara Y, Suwabe T, Sumida K, Hayami N, Yamanouchi M, Mise K, Hasegawa E, Hoshino J, Sawa N, Takaichi K (2012) Osteomalacia and insufficiency fracture in a hemodialysis patient with autosomal dominant polycystic kidney disease. Intern Med 51(23):3277–3280
Malluche HH, Monier-Faugere MC (1994) The role of bone biopsy in the management of patients with renal osteodystrophy. J Am Soc Nephrol 4(9):1631–1642
Kanis JA (1981) Osteomalacia and chronic renal failure. J Clin Pathol 34(11):1295–1307
Yajima A, Tsuchiya K, Burr DB, Wallace JM, Damrath JD, Inaba M, Tominaga Y, Satoh S, Nakayama T, Tanizawa T, Ogawa H, Ito A, Nitta K (2019) The importance of biologically active vitamin D for mineralization by osteocytes after parathyroidectomy for renal hyperparathyroidism. JBMR Plus 3(11):e10234
Schneider R, Slater EP, Karakas E, Bartsch DK, Schlosser K (2012) Initial parathyroid surgery in 606 patients with renal hyperparathyroidism. World J Surg 36(2):318–326
Lorenz K, Ukkat J, Sekulla C, Gimm O, Brauckhoff M, Dralle H (2006) Total parathyroidectomy without autotransplantation for renal hyperparathyroidism: experience with a qPTH-controlled protocol. World J Surg 30(5):743–751
Saunders RN, Karoo R, Metcalfe MS, Nicholson ML (2005) Four gland parathyroidectomy without reimplantation in patients with chronic renal failure. Postgrad Med J 81(954):255–258
Tamminen IS, Yli-Kyyny T, Isaksson H, Turunen MJ, Tong X, Jurvelin JS, Kröger H (2013) Incidence and bone biopsy findings of atypical femoral fractures. J Bone Miner Metab 31(5):585–594
Odvina CV, Zerwekh JE, Rao DS, Maalouf N, Gottschalk FA, Pak CY (2005) Severely suppressed bone turnover: a potential complication of alendronate therapy. J Clin Endocrinol Metab 90(3):1294–1301
Mashiba T, Hirano T, Turner CH, Forwood MR, Johnston CC, Burr DB (2000) Suppressed bone turnover by bisphosphonates increases microdamage accumulation and reduces some biomechanical properties in dog rib. J Bone Miner Res 15(4):613–620
Compston J (2011) Pathophysiology of atypical femoral fractures and osteonecrosis of the jaw. Osteoporos Int 22(12):2951–2961
Im GI, Lee SH (2015) Effect of teriparatide on healing of atypical femoral fractures: a systemic review. J Bone Metab 22(4):183–189
Sumida K, Ubara Y, Hoshino J, Mise K, Hayami N, Suwabe T, Kawada M, Imafuku A, Hiramatsu R, Hasegawa E, Yamanouchi M, Sawa N, Takaichi K (2016) Once-weekly teriparatide in hemodialysis patients with hypoparathyroidism and low bone mass: a prospective study. Osteoporos Int 27(4):1441–1450
Yamamoto T, Hasegawa T, Sasaki M, Hongo H, Tsuboi K, Shimizu T, Ota M, Haraguchi M, Takahata M, Oda K, Luiz de Freitas PH, Takakura A, Takao-Kawabata R, Isogai Y, Amizuka N (2016) Frequency of teriparatide administration affects the histological pattern of bone formation in young adult male mice. Endocrinology 157(7):2604–2620
Acknowledgments
We wish to thank Mrs. Akemi Ito (Ito Bone Science Institute, Niigata, Japan) for the bone histomorphometrical analyses.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
This investigation was conducted in accordance with the Declaration of Helsinki. The patient provided signed informed consent for the publication of this case report.
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(PPTX 2438 kb).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hatano, M., Kitajima, I., Isawa, K. et al. Diaphyseal femoral fracture due to severe vitamin D3 deficiency and low parathyroid hormone levels on long-term hemodialysis: a case report. Arch Osteoporos 15, 179 (2020). https://doi.org/10.1007/s11657-020-00849-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-020-00849-7