Abstract
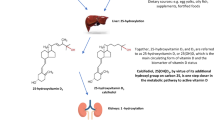
Osteoporosis is a major cause of morbidity and mortality worldwide and its prevention in order to avert fractures was considered of great importance in maintaining well-being and independence among the elderly. Strategies for osteoporosis prevention are well delineated, but research shows that the treatment options offered today could still be improved. The role of plain vitamin D (cholecalciferol) in bone health and the prevention of osteoporosis are well documented; however, as a treatment for osteoporosis, either with or without calcium, it has been shown to be ineffective. This is due in part to the strong negative feedback mechanisms in place in vitamin D-replete patients. However, other factors linked directly to ageing such as oestrogen depletion, reduced kidney or liver function may also be involved in reducing the body’s capability to activate plain vitamin efficiently. This is why active vitamin D analogues such as alfacalcidol, 1-α-(OH)D3, are of clinical interest. Alfacalcidol requires only one hydroxylation reaction to become active 1,25-(OH)2-vitamin D3, and the 25-hydroxylase catalyzing this reaction is found in the liver and also interestingly in osteoblasts suggesting a local effect. Registered for use in postmenopausal osteoporosis, in most countries worldwide, alfacalcidol has also shown efficacy in glucocorticoid-induced and male osteoporosis. The present review provides compelling evidence for the efficacy of this compound in the treatment of osteoporosis and prevention of fractures both in monotherapy and when combined with other osteoporotic drugs where additive effects are clear. The safety profile of alfacalcidol is shown to be highly acceptable and it is considered less likely to induce hypercalcaemia than another more widely used analogue, calcitriol. Therefore, it remains unclear as to why alfacalcidol is not more widely used in clinical practice.


Similar content being viewed by others
References
NIH Consensus Development Panel on Osteoporosis Prevention D, Therapy (2001) Osteoporosis prevention, diagnosis, and therapy. JAMA 285(6):785–795. https://doi.org/10.1001/jama.285.6.785
WHO Study Group (1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis : report of a WHO study group [meeting held in Rome from 22 to 25 June 1992]. WHO technical report series, vol 843. WHO, Geneva
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A (2007) Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res 22(3):465–475. https://doi.org/10.1359/jbmr.061113
Svedbom A, Hernlund E, Ivergard M, Compston J, Cooper C, Stenmark J, McCloskey EV, Jonsson B, Kanis JA, IOF EURPo (2013) Osteoporosis in the European Union: a compendium of country-specific reports. Arch Osteoporos 8:137. https://doi.org/10.1007/s11657-013-0137-0
Kim J, Lee E, Kim S, Lee TJ (2016) Economic burden of osteoporotic fracture of the elderly in South Korea: a national survey. Value Health Reg Issues 9:36–41. https://doi.org/10.1016/j.vhri.2015.09.007
National Instituts of Health (2000) Osteoporosis prevention, diagnosis, and therapy. NIH Consensus Statement, vol 17. NIH, Kensington MD
Wilkin TJ, Devendra D (2001) Bone densitometry is not a good predictor of hip fracture. BMJ 323(7316):795–797. https://doi.org/10.1136/bmj.323.7316.795
Leali PT, Muresu F, Melis A, Ruggiu A, Zachos A, Doria C (2011) Skeletal fragility definition. Clin Cases Miner Bone Metab 8(2):11–13
Guideline Development Group (GDG) (2012) Osteoporosis: assessing the risk of fragility fracture. NICE short clinical guideline, London
Cosman F, de Beur SJ, LeBoff MS, Lewiecki EM, Tanner B, Randall S, Lindsay R, National Osteoporosis F (2014) Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos Int 25(10):2359–2381. https://doi.org/10.1007/s00198-014-2794-2
Khazai N, Judd SE, Tangpricha V (2008) Calcium and vitamin D: skeletal and extraskeletal health. Curr Rheumatol Rep 10(2):110–117
DeLuca HF (2016) Vitamin D: historical overview. Vitam Horm 100:1–20
Bikle DD (1994) Role of vitamin D, its metabolites, and analogs in the management of osteoporosis. Rheum Dis Clin N Am 20(3):759–775
Compston JE, McClung MR, Leslie WD (2019) Osteoporosis. Lancet 393(10169):364–376. https://doi.org/10.1016/S0140-6736(18)32112-3
Qaseem A, Forciea MA, McLean RM, Denberg TD, Clinical Guidelines Committee of the American College of Physicians (2017) Treatment of low bone density or osteoporosis to prevent fractures in men and women: a clinical practice guideline update from the American College of Physicians. Ann Intern Med 166(11):818–839. https://doi.org/10.7326/M15-1361
Albright F, Smith PH, Richardson AM (1941) Postmenopausal osteoporosis. J Am Med Assoc 116:2465–2474
Gallagher JC, Sai AJ (2010) Vitamin D insufficiency, deficiency, and bone health. J Clin Endocrinol Metab 95(6):2630–2633. https://doi.org/10.1210/jc.2010-0918
Gallagher JC, Riggs BL, DeLuca HF (1980) Effect of estrogen on calcium absorption and serum vitamin D metabolites in postmenopausal osteoporosis. J Clin Endocrinol Metab 51(6):1359–1364. https://doi.org/10.1210/jcem-51-6-1359
Clarke BL, Khosla S (2010) Physiology of bone loss. Radiol Clin N Am 48(3):483–495. https://doi.org/10.1016/j.rcl.2010.02.014
van Driel M, van Leeuwen JP (2014) Vitamin D endocrine system and osteoblasts. Bonekey Rep 3:493. https://doi.org/10.1038/bonekey.2013.227
Lund B, Sorensen OH, Lund B, Agner E (1982) Serum 1,25-dihydroxyvitamin D in normal subjects and in patients with postmenopausal osteopenia. Influence of age, renal function and oestrogen therapy. Horm Metab Res 14(5):271–274. https://doi.org/10.1055/s-2007-1018990
Gallagher JC, Riggs BL, Eisman J, Hamstra A, Arnaud SB, DeLuca HF (1979) Intestinal calcium absorption and serum vitamin D metabolites in normal subjects and osteoporotic patients: effect of age and dietary calcium. J Clin Invest 64(3):729–736. https://doi.org/10.1172/JCI109516
Abrahamsen B, van Staa T, Ariely R, Olson M, Cooper C (2009) Excess mortality following hip fracture: a systematic epidemiological review. Osteoporos Int 20(10):1633–1650. https://doi.org/10.1007/s00198-009-0920-3
Riggs BL, Khosla S, Melton LJ 3rd (1998) A unitary model for involutional osteoporosis: estrogen deficiency causes both type I and type II osteoporosis in postmenopausal women and contributes to bone loss in aging men. J Bone Miner Res 13(5):763–773. https://doi.org/10.1359/jbmr.1998.13.5.763
Smith LM, Gallagher JC, Kaufmann M, Jones G (2018) Effect of increasing doses of vitamin D on bone mineral density and serum N-terminal telopeptide in elderly women: a randomized controlled trial. J Intern Med 284(6):685–693. https://doi.org/10.1111/joim.12825
Bolland MJ, Grey A, Avenell A (2018) Effects of vitamin D supplementation on musculoskeletal health: a systematic review, meta-analysis, and trial sequential analysis. Lancet Diabetes Endocrinol 6(11):847–858. https://doi.org/10.1016/S2213-8587(18)30265-1
Grant AM, Avenell A, Campbell MK, McDonald AM, MacLennan GS, McPherson GC, Anderson FH, Cooper C, Francis RM, Donaldson C, Gillespie WJ, Robinson CM, Torgerson DJ, Wallace WA, Group RT (2005) Oral vitamin D3 and calcium for secondary prevention of low-trauma fractures in elderly people (Randomised Evaluation of Calcium Or vitamin D, RECORD): a randomised placebo-controlled trial. Lancet 365(9471):1621–1628. https://doi.org/10.1016/S0140-6736(05)63013-9
Khaw KT, Stewart AW, Waayer D, Lawes CMM, Toop L, Camargo CA Jr, Scragg R (2017) Effect of monthly high-dose vitamin D supplementation on falls and non-vertebral fractures: secondary and post-hoc outcomes from the randomised, double-blind, placebo-controlled ViDA trial. Lancet Diabetes Endocrinol 5(6):438–447. https://doi.org/10.1016/S2213-8587(17)30103-1
Anderson PH, May BK, Morris HA (2003) Vitamin D metabolism: new concepts and clinical implications. Clin Biochem Rev 24(1):13–26
Breslau NA (1988) Normal and abnormal regulation of 1,25-(OH)2D synthesis. Am J Med Sci 296(6):417–425. https://doi.org/10.1097/00000441-198812000-00009
Mawer EB, Backhouse J, Holman CA, Lumb GA, Stanbury SW (1972) The distribution and storage of vitamin D and its metabolites in human tissues. Clin Sci 43(3):413–431. https://doi.org/10.1042/cs0430413
Abbas MA (2017) Physiological functions of vitamin D in adipose tissue. J Steroid Biochem Mol Biol 165(Pt B):369–381. https://doi.org/10.1016/j.jsbmb.2016.08.004
DeLuca HF (2004) Overview of general physiologic features and functions of vitamin D. Am J Clin Nutr 80(6 Suppl):1689S–1696S. https://doi.org/10.1093/ajcn/80.6.1689S
Martinaityte I, Kamycheva E, Didriksen A, Jakobsen J, Jorde R (2017) Vitamin D stored in fat tissue during a 5-year intervention affects serum 25-hydroxyvitamin D levels the following year. J Clin Endocrinol Metab 102(10):3731–3738. https://doi.org/10.1210/jc.2017-01187
Bordelon P, Ghetu MV, Langan RC (2009) Recognition and management of vitamin D deficiency. Am Fam Physician 80(8):841–846
Gallagher JC, Riggs BL, Jerpbak CM, Arnaud CD (1980) The effect of age on serum immunoreactive parathyroid hormone in normal and osteoporotic women. J Lab Clin Med 95(3):373–385
Zaheer S, de Boer I, Allison M, Brown JM, Psaty BM, Robinson-Cohen C, Ix JH, Kestenbaum B, Siscovick D, Vaidya A (2016) Parathyroid hormone and the use of diuretics and calcium-channel blockers: the multi-ethnic study of atherosclerosis. J Bone Miner Res 31(6):1137–1145. https://doi.org/10.1002/jbmr.2779
Sanders KM, Stuart AL, Williamson EJ, Simpson JA, Kotowicz MA, Young D, Nicholson GC (2010) Annual high-dose oral vitamin D and falls and fractures in older women: a randomized controlled trial. JAMA 303(18):1815–1822. https://doi.org/10.1001/jama.2010.594
Nuti R, Bianchi G, Brandi ML, Caudarella R, D’Erasmo E, Fiore C, Isaia GC, Luisetto G, Muratore M, Oriente P, Ortolani S (2006) Superiority of alfacalcidol compared to vitamin D plus calcium in lumbar bone mineral density in postmenopausal osteoporosis. Rheumatol Int 26(5):445–453. https://doi.org/10.1007/s00296-005-0073-4
PRODUCT(2017) SUMMARY for Etalpha, capsules, soft. Leo PHARMA
Tilyard MW, Spears GF, Thomson J, Dovey S (1992) Treatment of postmenopausal osteoporosis with calcitriol or calcium. N Engl J Med 326(6):357–362. https://doi.org/10.1056/NEJM199202063260601
Brandi L (2017) Alfacalcidol in CKD-MBD - a fresh look. J Clin Nephrol Res 4(2):1061
Ringe JD, Farahmand P, Schacht E (2013) Alfacalcidol in men with osteoporosis: a prospective, observational, 2-year trial on 214 patients. Rheumatol Int 33(3):637–643. https://doi.org/10.1007/s00296-012-2429-x
Ringe JD, Schacht E (2007) Improving the outcome of established therapies for osteoporosis by adding the active D-hormone analog alfacalcidol. Rheumatol Int 28(2):103–111. https://doi.org/10.1007/s00296-007-0422-6
Cianferotti L, Cricelli C, Kanis JA, Nuti R, Reginster JY, Ringe JD, Rizzoli R, Brandi ML (2015) The clinical use of vitamin D metabolites and their potential developments: a position statement from the European Society for Clinical and Economic Aspects of Osteoporosis and Osteoarthritis (ESCEO) and the International Osteoporosis Foundation (IOF). Endocrine 50(1):12–26. https://doi.org/10.1007/s12020-015-0606-x
Cavalli L, Cavalli T, Marcucci G, Falchetti A, Masi L, Brandi ML (2009) Biological effects of various regimes of 25-hydroxyvitamin D3 (calcidiol) administration on bone mineral metabolism in postmenopausal women. Clin Cases Miner Bone Metab 6(2):169–173
Kanis JA, Cooper C, Rizzoli R, Reginster JY, Scientific Advisory Board of the European Society for C, Economic Aspects of O, the Committees of Scientific A, National Societies of the International Osteoporosis F (2019) European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporos Int 30(1):3–44. https://doi.org/10.1007/s00198-018-4704-5
Jones G (2010) Why dialysis patients need combination therapy with both cholecalciferol and a calcitriol analogs. Semin Dial 23(3):239–243. https://doi.org/10.1111/j.1525-139X.2010.00722.x
Shiraki M, Kushida K, Yamazaki K, Nagai T, Inoue T, Orimo H (1996) Effects of 2 years’ treatment of osteoporosis 1 ci-hydroxy vitamin D3 on bone mineral density and incidence of fracture: a placebo-controlled, double-blind prospective study. Endocr J 43:211–220
Francis RMB, Boyle IT, Moniz C, Sutcliffe AM, Davis BS, Beastall GH, Cowan RA, Downes N (1996) A comparison of the effects of alfacalcidol treatment and vitamin D2 supplementation on calcium absorption in elderly women with vertebral fractures. Osteoporos Int 6:284–290
Francis R, Robinson C, Davison C, Rodgers A (1988) The short term effects of alfacaicidol in elderly osteoporotic women. In: Norman AW, Schaefer K, Grigoleit H-G, Herrath D (eds) Vitamin D: molecular, cellular and clinical Endocrinology, vol 846. Waiter de Gruyter, Berlin, p 7
Cohen HN, Farrah D, Fogelman I, Goll CC, Beastall GH, McIntosh WB, Fletcher M, Boyle IT (1980) A low dose regime of 1 alpha hydroxyvitamin D3 in the management of senile osteoporosis: a pilot study. Clin Endocrinol 12(6):537–542. https://doi.org/10.1111/j.1365-2265.1980.tb01373.x
Ringe JD, Coster A, Meng T, Schacht E, Umbach R (1999) Treatment of glucocorticoid-induced osteoporosis with alfacalcidol/calcium versus vitamin D/calcium. Calcif Tissue Int 65(4):337–340. https://doi.org/10.1007/s002239900708
Fleisch H (1998) Bisphosphonates: mechanisms of action. Endocr Rev 19(1):80–100. https://doi.org/10.1210/edrv.19.1.0325
Ebina K, Kashii M, Hirao M, Hashimoto J, Noguchi T, Koizumi K, Kitaguchi K, Matsuoka H, Iwahashi T, Tsukamoto Y, Yoshikawa H (2017) Comparison of the effects of denosumab between a native vitamin D combination and an active vitamin D combination in patients with postmenopausal osteoporosis. J Bone Miner Metab 35(5):571–580. https://doi.org/10.1007/s00774-016-0792-5
Compston J, Cooper A, Cooper C, Gittoes N, Gregson C, Harvey N, Hope S, Kanis JA, McCloskey EV, Poole KES, Reid DM, Selby P, Thompson F, Thurston A, Vine N, National Osteoporosis Guideline G (2017) UK clinical guideline for the prevention and treatment of osteoporosis. Arch Osteoporos 12(1):43. https://doi.org/10.1007/s11657-017-0324-5
Shao HB, Yao YM, Wang ZY, Zhang QF, Wei W (2015) Effects of combined alendronate and alfacalcidol on prevention of fractures in osteoporosis patients: a network meta-analysis. Int J Clin Exp Med 8(8):12935–12941
Cummings SR, San Martin J, McClung MR, Siris ES, Eastell R, Reid IR, Delmas P, Zoog HB, Austin M, Wang A, Kutilek S, Adami S, Zanchetta J, Libanati C, Siddhanti S, Christiansen C, Trial F (2009) Denosumab for prevention of fractures in postmenopausal women with osteoporosis. N Engl J Med 361(8):756–765. https://doi.org/10.1056/NEJMoa0809493
Black DM, Delmas PD, Eastell R, Reid IR, Boonen S, Cauley JA, Cosman F, Lakatos P, Leung PC, Man Z, Mautalen C, Mesenbrink P, Hu H, Caminis J, Tong K, Rosario-Jansen T, Krasnow J, Hue TF, Sellmeyer D, Eriksen EF, Cummings SR, Trial HPF (2007) Once-yearly zoledronic acid for treatment of postmenopausal osteoporosis. N Engl J Med 356(18):1809–1822. https://doi.org/10.1056/NEJMoa067312
Neer RM, Arnaud CD, Zanchetta JR, Prince R, Gaich GA, Reginster JY, Hodsman AB, Eriksen EF, Ish-Shalom S, Genant HK, Wang O, Mitlak BH (2001) Effect of parathyroid hormone (1-34) on fractures and bone mineral density in postmenopausal women with osteoporosis. N Engl J Med 344(19):1434–1441. https://doi.org/10.1056/NEJM200105103441904
Black DM, Cummings SR, Karpf DB, Cauley JA, Thompson DE, Nevitt MC, Bauer DC, Genant HK, Haskell WL, Marcus R, Ott SM, Torner JC, Quandt SA, Reiss TF, Ensrud KE (1996) Randomised trial of effect of alendronate on risk of fracture in women with existing vertebral fractures. Fracture Intervention Trial Research Group. Lancet 348(9041):1535–1541. https://doi.org/10.1016/s0140-6736(96)07088-2
Black DM, Thompson DE, Bauer DC, Ensrud K, Musliner T, Hochberg MC, Nevitt MC, Suryawanshi S, Cummings SR, Fracture Intervention T (2000) Fracture risk reduction with alendronate in women with osteoporosis: the Fracture Intervention Trial. FIT Research Group. J Clin Endocrinol Metab 85(11):4118–4124. https://doi.org/10.1210/jcem.85.11.6953
Cummings SR, Black DM, Thompson DE, Applegate WB, Barrett-Connor E, Musliner TA, Palermo L, Prineas R, Rubin SM, Scott JC, Vogt T, Wallace R, Yates AJ, LaCroix AZ (1998) Effect of alendronate on risk of fracture in women with low bone density but without vertebral fractures: results from the Fracture Intervention Trial. JAMA 280(24):2077–2082. https://doi.org/10.1001/jama.280.24.2077
Ones K, Schacht E (2006) Superiority of a combined treatment of alfacalcidol and alendronate compared to the monotherapies in postmenopausal osteoporosis. Osteoporos Int 17(1):S20(P112)
Ringe JD, Farahmand P, Schacht E, Rozehnal A (2007) Superiority of a combined treatment of alendronate and alfacalcidol compared to the combination of alendronate and plain vitamin D or alfacalcidol alone in established postmenopausal or male osteoporosis (AAC-Trial). Rheumatol Int 27(5):425–434. https://doi.org/10.1007/s00296-006-0288-z
Schacht E, Dukas L, Richy F (2007) Combined therapies in osteoporosis: bisphosphonates and vitamin D-hormone analogs. J Musculoskelet Neuronal Interact 7(2):174–184
Felsenberg D, Bock O, Borst H, Armbrecht G, Beller G, Degner C, Stephan-Oelkers M, Schacht E, Mazor Z, Hashimoto J, Roth HJ, Martus P, Runge M (2011) Additive impact of alfacalcidol on bone mineral density and bone strength in alendronate treated postmenopausal women with reduced bone mass. J Musculoskelet Neuronal Interact 11(1):34–45
Orimo H, Nakamura T, Fukunaga M, Ohta H, Hosoi T, Uemura Y, Kuroda T, Miyakawa N, Ohashi Y, Shiraki M, group ATr (2011) Effects of alendronate plus alfacalcidol in osteoporosis patients with a high risk of fracture: the Japanese Osteoporosis Intervention Trial (JOINT) - 02. Curr Med Res Opin 27(6):1273–1284. https://doi.org/10.1185/03007995.2011.580341
Ettinger B, Black DM, Mitlak BH, Knickerbocker RK, Nickelsen T, Genant HK, Christiansen C, Delmas PD, Zanchetta JR, Stakkestad J, Gluer CC, Krueger K, Cohen FJ, Eckert S, Ensrud KE, Avioli LV, Lips P, Cummings SR (1999) Reduction of vertebral fracture risk in postmenopausal women with osteoporosis treated with raloxifene: results from a 3-year randomized clinical trial. Multiple Outcomes of Raloxifene Evaluation (MORE) Investigators. JAMA 282(7):637–645. https://doi.org/10.1001/jama.282.7.637
Gorai I, Hattori S, Tanaka Y, Iwaoki Y (2012) Alfacalcidol-supplemented raloxifene therapy has greater bone-sparing effect than raloxifene-alone therapy in postmenopausal Japanese women with osteoporosis or osteopenia. J Bone Miner Metab 30(3):349–358. https://doi.org/10.1007/s00774-011-0325-1
Lobo RA (2017) Hormone-replacement therapy: current thinking. Nat Rev Endocrinol 13(4):220–231. https://doi.org/10.1038/nrendo.2016.164
Mizunuma H, Shiraki M, Shintani M, Gorai I, Makita K, Itoga S, Mochizuki Y, Mogi H, Iwaoki Y, Kosha S, Yasui T, Ishihara O, Kurabayashi T, Kasuga Y, Hayashi K (2006) Randomized trial comparing low-dose hormone replacement therapy and HRT plus 1alpha-OH-vitamin D3 (alfacalcidol) for treatment of postmenopausal bone loss. J Bone Miner Metab 24(1):11–15. https://doi.org/10.1007/s00774-005-0639-y
Lips P (2001) Vitamin D deficiency and secondary hyperparathyroidism in the elderly: consequences for bone loss and fractures and therapeutic implications. Endocr Rev 22(4):477–501. https://doi.org/10.1210/edrv.22.4.0437
Drake MT, Clarke BL, Khosla S (2008) Bisphosphonates: mechanism of action and role in clinical practice. Mayo Clin Proc 83(9):1032–1045. https://doi.org/10.4065/83.9.1032
Ringe JD, Dorst A, Faber H, Schacht E, Rahlfs VW (2004) Superiority of alfacalcidol over plain vitamin D in the treatment of glucocorticoid-induced osteoporosis. Rheumatol Int 24(2):63–70. https://doi.org/10.1007/s00296-003-0361-9
McCloskey EV, Johansson H, Oden A, Austin M, Siris E, Wang A, Lewiecki EM, Lorenc R, Libanati C, Kanis JA (2012) Denosumab reduces the risk of osteoporotic fractures in postmenopausal women, particularly in those with moderate to high fracture risk as assessed with FRAX. J Bone Miner Res 27(7):1480–1486. https://doi.org/10.1002/jbmr.1606
Fujita T (1990) Studies of osteoporosis in Japan. Metabolism 39(4 Suppl 1):39–42
Orimo H, Shiraki M, Hayashi Y, Hoshino T, Onaya T, Miyazaki S, Kurosawa H, Nakamura T, Ogawa N (1994) Effects of 1 alpha-hydroxyvitamin D3 on lumbar bone mineral density and vertebral fractures in patients with postmenopausal osteoporosis. Calcif Tissue Int 54(5):370–376. https://doi.org/10.1007/bf00305521
Nakano M, Tsujimoto M, Sowa H (2013) The effect of the concomitant administration of active vitamin D on the safety of once-a-day subcutaneous injection of teriparatide 20μg/day. Jpn J Clin Pharmacol Ther 44(54):395–403
Ringe JD (2004) Questions on the superiority of alfacalcidol over plain vitamin D in the treatment of glucocorticoid-induced osteoporosis. Rheumatol Int 24(6):370. https://doi.org/10.1007/s00296-004-0523-4
Brandi ML (2010) Indications on the use of vitamin D and vitamin D metabolites in clinical phenotypes. Clin Cases Miner Bone Metab 7(3):243–250
Chen JT, Shiraki M, Hasumi K, Tanaka N, Katase K, Kato T, Hirai Y, Nakamura T, Ogata E (1997) 1-alpha-Hydroxyvitamin D3 treatment decreases bone turnover and modulates calcium-regulating hormones in early postmenopausal women. Bone 20(6):557–562. https://doi.org/10.1016/s8756-3282(97)00054-9
Funding
Editorial assistance was supported by LEO Pharma.
Author information
Authors and Affiliations
Contributions
Sole author.
Corresponding author
Ethics declarations
Conflicts of interest
None.
Ethics approval
Not relevant review of previously published studies.
Consent to participate
Given.
Consent for publication
Given.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ringe, J.D. Plain vitamin D or active vitamin D in the treatment of osteoporosis: where do we stand today?. Arch Osteoporos 15, 182 (2020). https://doi.org/10.1007/s11657-020-00842-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-020-00842-0