Abstract
Objective
To explore the effect of Tangshen Formula (糖肾方, TSF), a Chinese herbal medicine, on interstitial cells of Cajal (ICC) in the colon of diabetic rats.
Methods
Fifty-four male Wistar rats were randomly divided into normal control (NC, n=14) and high-fat diet (HFD) groups (n=40). After 6 weeks, the rats in the HFD group were injected intraperitoneally streptozotocin once (30 mg/kg). Thirty rats with fasting blood glucose higher than 11.7 mmol/L were randomly divided into diabetes (DM) and TSF groups, 15 rats in each group. Rats in the NC and DM groups were intragastrically administered with saline, and those in the TSF group were given with TSF (2.4 g/kg) once daily for 20 weeks. Expression levels of Bax, Bcl-2, and caspase-3 in colonic smooth muscle layer were measured by Western blotting and immunohistochemical staining. The number of ICC was determined by immunohistochemical staining. Immunofluorescence was used for analyzing the ratio of classically activated macrophages (M1) and alternatively activated macrophages (M2) to total macrophages. Electron microscopy was used to observe the epithelial ultrastructure and junctions.
Results
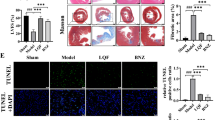
TSF appeared to partially prevented loss of ICC in DM rats (P<0.05). Compared with the NC group, expression levels of Bcl-2, Bax, caspase-3, and TNF-α as well as the ratio of M1 to total macrophages increased in DM rats (all P<0.05), and the ratio of M2 to total macrophages decreased (P<0.05 or P<0.01). Compared with the DM group, TSF decreased the expression levels of abovementioned proteins and restore M2 to total macrophages ratio (P<0.05 or P<0.01). TSF appeared to attenuate the ultrastructural changes of epithelia and improve the tight and desmosome junctions between epithelia reduced in the DM rats.
Conclusion
Reduced number of ICC in DM rats may be associated with damage of the intestinal barrier. The protective effects of TSF on ICC may be through repair of the epithelial junctions, which attenuates inflammation and inflammation-initiated apoptosis in colon of DM rats.
Similar content being viewed by others
References
Yarandi SS, Srinivasan S. Diabetic gastrointestinal motility disorders and the role of enteric nervous system: current status and future directions. Neurogastroent Motil 2014;26:611–624.
Zawada AE, Moszak M, Skrzypczak D, Grzymislawski M. Gastrointestinal complications in patients with diabetes mellitus. Adv Clin Exp Med 2018;27:567–572.
Careyva B, Stello B. Diabetes mellitus: management of gastrointestinal complications. Am Fam Physic 2016;94:980–986.
Jung HK, Kim DY, Moon IH, Hong YS. Colonic transit time in diabetic patients—comparison with healthy subjects and the effect of autonomic neuropathy. Yonsei Med J 2003;44:265–272.
Forrest A, Parsons M. The enhanced spontaneous activity of the diabetic colon is not the consequence of impaired inhibitory control mechanisms. Auton Autacoid Pharmacol 2003;23:149–158.
Nam Y, Lee JM, Wang Y, Ha HS, Sohn UD. The effect of Flos Lonicerae Japonicae extract on gastro-intestinal motility function. J Ethnopharmacol 2016;179:280–290.
Xiong X, Peng W, Chen L, Liu H, Huang W, Yang B, et al. Traditional Chinese medicine Zhiqiao-Houpu herb-pair induce bidirectional effects on gastric motility in rats. J Ethnopharmacol 2015;175:444–450.
Takaki M. Gut pacemaker cells: the interstitial cells of Cajal (ICC). J Smooth Muscle Res 2003;39:137–161.
Wu T, Rayner CK, Young RL, Horowitz M. Gut motility and enteroendocrine secretion. Curr Opin Pharmacol 2013;13:928–934.
Siegman MJ, Eto M, Butler TM. Remodeling of the rat distal colon in diabetes: function and ultrastructure. Am J Physiol Cell Physiol 2016;310:C151–C160.
Chen P, Zhao J, Gregersen H. Up-regulated expression of advanced glycation end-products and their receptor in the small intestine and colon of diabetic rats. Digest Dis Sci 2012;57:48–57.
Eisenman ST, Gibbons SJ, Verhulst PJ, Cipriani G, Saur D, Farrugia G. Tumor necrosis factor alpha derived from classically activated “M1” macrophages reduces interstitial cell of Cajal numbers. Neurogastroenterol Motil 2017; doi:https://doi.org/10.1111/nmo.12984.
Li P, Chen Y, Liu J, Hong J, Deng Y, Yang F, et al. Efficacy and safety of Tangshen Formula on patients with type 2 diabetic kidney disease: a multicenter double-blinded randomized placebo-controlled trial. PLoS One 2015;10:e0126027.
Liu P, Peng L, Zhang H, Tang PM, Zhao T, Yan M, et al. Tangshen Formula attenuates diabetic nephropathy by promoting ABCA1-mediated renal cholesterol efflux in db/db mice. Front Physiol 2018; doi: https://doi.org/10.3389/fphys.2018.00343.
Zhao T, Sun S, Zhang H, Huang X, Yan M, Dong X, et al. Therapeutic effects of Tangshen Formula on diabetic nephropathy in rats. PLoS One 2016; doi: https://doi.org/10.1371/journal.pone.0147693.
Chen P, Zhao J, Zhang H, Yang X, Zhao T, Zhang H, et al. Tangshen Formula attenuates colonic structure remodeling in type 2 diabetic rats. Evid Based Complementa Altern Med 2017; doi:https://doi.org/10.1155/2017/4064156.
Kong Q, Zhang H, Zhao T, Zhang W, Yan M, Dong X, et al. Tangshen Formula attenuates hepatic steatosis by inhibiting hepatic lipogenesis and augmenting fatty acid oxidation in db/db mice. Int J Mol Med 2016;38:1715–1726.
Shapouri-Moghaddam A, Mohammadian S, Vazini H, Taghadosi M, Esmaeili SA, Mardani F, et al. Macrophage plasticity, polarization, and function in health and disease. J Cell Physiol 2018;233:6425–6440.
Martinez FO, Sica A, Mantovani A, Locati M. Macrophage activation and polarization. Front Biosci 2008;13:453–461.
Mosser D, Edwards J. Exploring the full spectrum of macrophage activation. Nature Rev Immunol 2008;8:958–969.
Neshatian L, Gibbons SJ, Farrugia G. Macrophages in diabetic gastroparesis-the missing link? Neurogastroenterol Motil 2015;27:7–18.
Arimatsu K, Yamada H, Miyazawa H, Minagawa T, Nakajima M, Ryder MI, et al. Oral pathobiont induces systemic inflammation and metabolic changes associated with alteration of gut microbiota. Sci Rep 2014; doi: https://doi.org/10.1038/srep04828.
Davis-Richardson AG, Triplett EW. A model for the role of gut bacteria in the development of autoimmunity for type 1 diabetes. Diabetologia 2015;58:1386–1393.
Hooper LV, Littman DR, Macpherson AJ. Interactions between the microbiota and the immune system. Science 2012;336:1268–1273.
Ringel Y, Maharshak N. Intestinal microbiota and immune function in the pathogenesis of irritable bowel syndrome. Am J Physiol Gastrointest Liver Physiol 2013;305:G529–G541.
Zhang H, Li P, Burczynski FJ, Gong Y, Choy P, Sha H, et al. Attenuation of diabetic nephropathy in Otsuka Long-Evans Tokushima Fatty (OLETF) rats with a combination of Chinese herbs (Tangshen Formula). Evid-Based Complement Altern Med 2011; doi: https://doi.org/10.1155/2011/613737.
Acknowledgments
The authors thank Nissi S. Wang, MSc, for editing this manuscript.
Author information
Authors and Affiliations
Contributions
Chen PM designed, performed the experiment, and prepared the manuscript. Zhao JB supervised the study, provided suggestions and revised the manuscript. Yang X and Zhang HJ performed the animal experiments. Zhang HC was responsible for the sample collection and data analysis. Li J and Zhang YT performed electron microscopy. Li P supervised the study and revised the manuscript. All authors read and approved the final manuscript for publication.
Corresponding author
Additional information
Conflict of Interest
The authors declare that they have no conflict of interests
Supported by National Natural Science Foundation of China (No. 81873135)
Rights and permissions
About this article
Cite this article
Chen, Pm., Zhao, Jb., Yang, X. et al. Protective Effect of Tangshen Formula (糖肾方) on Interstitial Cells of Cajal in Colon of Diabetic Rats. Chin. J. Integr. Med. 28, 43–51 (2022). https://doi.org/10.1007/s11655-021-3297-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-021-3297-6