Abstract
Background
Dementia and mild cognitive impairment (MCI) are prevalent but underdiagnosed.
Objective
To compare new dementia/MCI diagnosis rates in geriatrics-focused primary care clinics and traditional primary care clinics.
Design
Secondary analysis of a prospective matched cohort study that spanned 2017–2021.
Participants
Community-dwelling Veterans over 65 receiving primary care in a geriatrics-focused medical home (GeriPACT) or traditional primary care home (PACT) at one of 57 Veterans Affairs sites. We excluded individuals with a documented diagnosis of dementia or MCI in the year prior to enrollment.
Main Measures
Diagnoses obtained from EHR. Cognitive status was assessed using modified Telephone Interview for Cognitive Status (mTICS) tool.
Key Results
The 470 participants included in this analysis were predominantly white, non-Hispanic males with an average age of 80.3 years. 9.4% of participants received a diagnosis of dementia/MCI after 24 months: 11.5% in GeriPACT and 7.2% in PACT. Adjusted OR for dementia/MCI diagnosis based on GeriPACT exposure was 1.47 (95% CI 0.65–3.29). Low mTICS score (≤ 27) (OR 4.89, 95% CI 2.36–10.13) and marital status (married/partnered) (OR 1.89, CI 0.99–3.59) were independent predictors of dementia/MCI diagnosis. When stratified by cognitive status: diagnosis rates were 20.8% in GeriPACT and 16.7% in PACT among those who scored lower on the cognitive assessment (mTICS ≤ 27); 7.4% in GeriPACT and 3.6% in PACT among those who scored higher (mTICS > 27). The OR for new dementia/MCI diagnosis in GeriPACT was 1.19 (95% CI 0.49–2.91) among those with a low mTICS score and 1.85 (95% CI 0.70–4.88) among those with a higher mTICS score.
Conclusions
Observed rates of new dementia/MCI diagnosis were higher in GeriPACT, but with considerable uncertainty around estimates. Geriatrics-focused primary care clinics may be a promising avenue for improving the detection of dementia in older adults, but further larger studies are needed to confirm this relationship.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Alzheimer’s Disease and related dementias (ADRD) afflict over three million older adults in the USA—a number that is expected to triple by 2060.1 ADRD is associated with significant negative individual and societal outcomes, including higher costs of care, greater morbidity and mortality, and increased family burden. With few efficacious treatments for dementia on the horizon, these negative consequences are best mitigated by a timely diagnosis: prompt recognition enables early discussions around goals of care, the ability to modify risk factors associated with disease progression, and timely referrals to essential resources for patients and family members.2,3,4,5 Unfortunately, despite its high prevalence, dementia remains underdiagnosed in the United States.6,7,8,9 Primary care settings play an important role in the early recognition of ADRD, as most cases are diagnosed by primary care providers.10 However, several clinic and provider factors in traditional primary care practices can impede timely diagnosis, including time constraints, lack of specialized geriatrics training, and limited interdisciplinary support.11
One potential solution to address these barriers and improve the detection of dementia is a team-based geriatrics-focused primary care clinic model. These clinics are often characterized by longer appointment times, geriatrics training for team members, emphasis on geriatric syndromes, and a multidisciplinary approach to care.12,13,14 Despite this unique potential, there is limited evidence describing the impact of geriatrics primary care clinics on the quality of care and outcomes in older adults. An ideal environment for examining this question is the Veteran’s Affairs (VA), which has rates of dementia comparable to the general population and includes the clinic models of interest: traditional primary care clinics (Patient Aligned Care Teams or PACTs) and geriatrics-focused primary care clinics (GeriPACTs).15,16 VA GeriPACTs have many characteristics that may be advantageous in the detection of dementia including smaller patient panels, specialized interdisciplinary teams, focus on geriatric syndromes, and an emphasis on functional dependencies.17,18
The overall goal of this paper was to compare rates of newly documented mild cognitive impairment (MCI) or dementia in GeriPACT and PACT settings. We hypothesized that participants who transferred care to GeriPACT would have higher rates of MCI or dementia diagnoses at 24 months, compared to similar, matched patients in PACT care. We also examined other predictors of new MCI or dementia diagnoses.
METHODS
Study Design
This is a secondary analysis of data collected for a prospective matched cohort study investigating the impact of GeriPACT on quality of care and patient experience measures (IRB #02,056). Details around study design, matching, and enrollment procedures have been published previously.19 In brief, at each VA site with ≥ 500 GeriPACT visits in 2016 (57 sites in total), we selected GeriPACT patients who newly transitioned to the GeriPACT clinic. Patients were considered to be new transfers to the GeriPACT clinic if they had only PACT visits in the 12-month pre-exposure period followed by only GeriPACT visits during the subsequent 12-month exposure period. In contrast, PACT participants were required to have at least 2 PACT visits in both the pre-exposure and exposure periods. Matching was used to guide the enrollment of GeriPACT-PACT dyads across the 57 VA medical centers. Matching variables were derived from EHR data in the pre-exposure period, and included a rich set of factors known to drive entry into GeriPACT (e.g., demographics [age, race, gender], pre-exposure care utilization [VA facility, presence of hospitalization in the past year, number of hospitalization in last year], pre-exposure health status [presence of advanced directives, JEN Frailty Index or JFI, Care Assessment Need or CAN score]) using a combination of exact and Mahalanobis distance function matching. Data sources included encounter data and diagnosis codes from VA’s electronic health record accessed through the Corporate Data Warehouse, chart reviews, and telephone-based surveys. During their initial enrollment call, participants completed a baseline survey which included questions about demographics and a validated, telephone-based cognitive assessment.20
Eligibility Criteria
Participants were potentially eligible if they were aged 65 years or older, community-dwelling, enrolled in a GeriPACT or PACT clinic and had a valid phone number in the medical record. Participants enrolled in hospice, and those with active substance use disorders or psychosis were excluded. To address our goals to examine new diagnoses of dementia, participants who were unable to complete the telephone-based cognitive assessment and those with a diagnosis of dementia/MCI in the year prior to the exposure were excluded. In order to maintain the benefits of matching, both members of the matched-pair were excluded from the analysis if either individual had a previous diagnosis of dementia/MCI or were unable to complete cognitive testing due to hearing impairment.
Variable Measurements
Cognitive Assessment
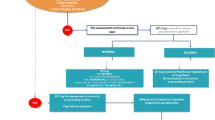
The two-part cognitive evaluation was conducted over the telephone by trained study staff. The first assessment of cognitive status was the validated Callahan six-item cognitive instrument.21,22,23 Those who scored four or less (out of six) were suspected to have cognitive impairment; therefore, the involvement of a legally authorized representative (LAR) was required before proceeding further. This LAR—rather than the patient themselves—completed the rest of the survey; therefore, the second portion of the cognitive assessment was not administered directly to these patients. For individuals who scored at least five on the Callahan instrument, the baseline phone survey also included the second instrument for evaluating cognition: the modified Telephone Interview for Cognitive Status (mTICS).24 The mTICS score was adjusted for education (see supplementary materials in the Appendix).25 Based on previously published research, an adjusted mTICS score of ≤ 27 (out of 50) was used as the cutoff for impaired cognitive function. We considered a low score on either of these two instruments to be indicative of probable cognitive impairment.
Dementia and Cognitive Impairment Diagnoses
For the purposes of this secondary analysis, we used previously published lists of diagnostic codes: we defined dementia according to the Veterans Health Administration recommendations, and cognitive impairment according to the American Academy of Neurology (AAN). 26,27 We included encounter-associated diagnosis codes in either inpatient or outpatient settings. See supplementary materials S2 in the Appendix.
Predictive Variables
For the model examining predictors of new dementia diagnosis, we prioritized candidate covariates that reflected domains of the Andersen Model of Health Care Utilization.28,29,30,31 In addition to GeriPACT exposure and mTICS score, measures included marital status, financial security, and number of activities of daily living (ADLs) for which some help was needed. Data for all three variables were obtained from the telephone-based survey administered at enrollment.
Statistical Analysis
Descriptive statistics were used to examine baseline cognitive status (mTICS score) among Veterans who transferred care to GeriPACT, compared to similar patients who remained in traditional PACTs. Individuals were analyzed according to the exposure arm. A logistic regression model was used to determine if there were any overall differences in rates of dementia/MCI diagnoses between the GeriPACT and PACT groups independent of their cognitive instrument score. Individuals were also analyzed according to their mTICS score (≤ 27 or > 27). The overall model inclusive of all patients (not stratified by cognitive assessment score) was adjusted for mTICS score (≤ 27 versus > 27), marital status (married/partnered versus other), financial security (good/ok versus other), and functional status (number of ADLs for which some help was needed). In contrast, the stratified results were adjusted for financial security and functional status. Statistical analyses were performed using SAS software. Copyright © 2022 SAS Institute Inc.
RESULTS
Patient Characteristics
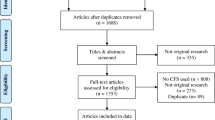
In total, 275 GeriPACT and 275 PACT participants were enrolled and included in primary study analyses (Figure S1 in the Appendix). For this secondary analysis, a further 78 individuals were excluded: 46 individuals had a pre-exposure diagnosis of dementia/MCI, 30 individuals without a diagnosis of dementia/MCI had a matched partner with a diagnosis, and 2 individuals (participant and matched partner) were excluded due to hearing difficulties and the need for a LAR respondent. One GeriPACT patient was noted to have spent the entire exposure period in a nursing home (one of the exclusion criteria for the overall study); therefore, this patient and their match were also excluded from these analyses. Ultimately, 470 participants (235 GeriPACT and 235 PACT) were included in this secondary analysis.
GeriPACT and PACT groups were comparable on matched variables and patient-reported survey variables (Table 1). Overall, the study population was older, majority white, and predominantly male. Over half of the participants self-reported a level of education at or above some trade school or college experience, and around a quarter of participants self-reported a low health literacy. Nearly a quarter of individuals self-reported financial difficulty. The majority of participants lived close to a VA hospital, and most participants received some care outside of the VA health care system, although the majority did not have private insurance and less than 10% were enrolled in Medicaid. The majority of participants were married or had a partner, and most lived with another individual. The majority also identified a caregiver (family or friend) as a potential source of support. Only a quarter of participants had advanced directives on file, and recent hospitalizations were rare. The average JFI score—which estimates the risk for long-term care needs based on documented diagnoses—was 3.7, consistent with moderate frailty (scale 0–13, with a higher score suggestive of increased frailty). The mean CAN score—which estimates the risk of hospitalization or death in the next 12 months—was 48.2, consistent with middle risk (scale 0–100, with a score indicative of patient percentile).32 Patients needed help with an average of 1.1 ADLs (out of 7) and 1.7 IADLs (out of 7).
Cognitive Status
Figure 1 shows the overall distribution of the mTICs scores (obtained at study enrollment) by exposure. The scores ranged from 16 to 46. The average overall mTICs score was 30.4 (standard deviation of 4.8). When exposure arms were considered separately, the GeriPACT and PACT mean mTICS scores were comparable: 30.2 for GeriPACT patients and 30.6 for PACT patients. 123 participants had a low score on the mTICS (≤ 27), concerning cognitive impairment. The number of low scores was similar in both exposure groups: 62 in GeriPACT and 61 in PACT. When combined with the Callahan results, 138 participants overall received a low score on cognitive testing: 72 in GeriPACT and 66 in PACT.
Dementia and Mild Cognitive Impairment Diagnoses
A total of 44 (9.4%) patients overall received a new documented diagnosis of dementia or MCI in our 24-month outcome period: 11.5% (n = 27/235) of GeriPACT patients versus 7.2% (n = 17/235) of PACT patients. The overall adjusted OR for receiving a dementia/MCI diagnosis based on GeriPACT exposure compared to PACT was 1.47 (95% confidence interval 0.65–3.29) (Fig. 2). The ORs for a new dementia or MCI diagnosis based on other individual patient-level predictive characteristics (including mTICS score, marital status, financial status, and support with ADLs) are shown in Table 2.
ORs of a new dementia/MCI diagnosis based GeriPACT exposure (overall and by cognitive assessment results). Overall model adjusted for mTICS score (≤ 27 versus > 27), marital status (married/partnered versus other), financial security (good/ok versus other), and functional status (number of ADLs). Stratified results were adjusted for financial security and functional status. n = 6 patients were excluded from this analysis due to missing data around financial security.
In order to better understand the relationship between cognitive status and dementia/MCI diagnosis, we additionally performed a logistic regression model by mTICS or Callahan results. Of the individuals with a low mTICS or Callahan score concerning cognitive impairment, 18.8% (n = 26/138) received a diagnosis during the study period: 20.8% (n = 15/72) of individuals in the GeriPACT arm, and 16.7% (n = 11/66) of individuals in the PACT arm. Of those with a higher score, 5.4% (n = 18/332) received a diagnosis during the 24-month exposure period: 7.4% (n = 12/163) in GeriPACT versus 3.6% (n = 6/169) in PACT. Table 3 summarizes the relationship between mTICS or Callahan scores and cognitive diagnoses at the end of the 24-month outcome period. When stratified by cognitive assessment performance, the OR for a diagnosis associated with GeriPACT exposure was 1.19 (95% CI 0.49–2.91) in those with a low score and 1.85 (95% CI 0.70–4.88) in those with a higher score.
DISCUSSION
Among 470 older Veterans enrolled in VA primary care clinics around the United States, we found that new dementia/MCI diagnosis rates were higher in participants who received GeriPACT care compared with PACT care; however, confidence intervals around model-based estimates were broad. Nearly one-quarter of participants (n = 123/470) scored low on the mTICS or Callahan instruments—suggestive of cognitive impairment. Our model found that participants with a low cognitive assessment score along with those who were married or lived with a partner were more likely to receive a diagnosis of dementia or MCI. When our model was stratified by cognitive status, the difference in diagnosis rate between GeriPACT and PACT individuals was largest in those who received a higher mTICS and/or Callahan score; however, these findings were similarly indeterminate due to large uncertainty around variable estimates.
These results cautiously suggest that increased referrals to geriatrics primary care clinics may be associated with higher rates of dementia diagnoses—although further studies with large study populations are needed for confirmation. Furthermore, while this study was not powered to look at the different operational characteristics of geriatrics primary care clinics, we suspect that this increased diagnosis of individuals with cognitive impairment is likely due to the unique structure and clinical processes of GeriPACT care, including decreased number of patients per provider, longer appointment times, organization of care, and clinical expertise. Future fully-powered studies could focus on (1) confirming this relationship between primary care setting and diagnosis; and (2) determining the exact reasons for this potential difference in diagnosis rates between GeriPACT and PACT settings, should it be confirmed.
These results also highlight possible patient-level predictors of dementia and MCI diagnoses. The strong OR for those participants with a low mTICS score agrees with prior studies that have demonstrated the utility of the tool for detecting signs of cognitive impairment.20,33,34 This strong relationship between assessment score and clinical diagnosis support close clinical attention to individuals who score low on cognitive testing. Despite its importance, only a small percentage of individuals with low cognitive scores received a diagnosis of dementia/MCI (21% in GeriPACT and 17% in PACT)—suggesting that while patients in GeriPACT are more likely to receive a diagnosis, both clinics still have ample room to improve on detecting early signs and identifying patients for further testing.
These results cautiously suggest that attention should also be given to a patient’s marital status. Prior studies found higher dementia/MCI rates in participants who were divorced/single/widowed due to the possible protective nature of socialization.35,36 In contrast, our research suggested higher diagnosis rates in participants who were married or partnered. Partners or caregivers may contribute to early diagnoses by spotting early signs or symptoms of cognitive impairment and facilitating a health care visit—particularly for GeriPACT, as transition to this specialty clinic is voluntary and may be prompted by family concerns. Additional understanding of the role of caregivers in VA clinics’ diagnostic processes and care coordination is required; however, our research cautiously suggests that providers should pay particular attention to patients who are divorced, widowed, or single as they may be less likely to receive dementia or MCI diagnoses.
There were several limitations to this research. The most significant limitation was the study’s sample size and the relatively small frequency of new dementia/MCI diagnoses. Limiting our focus to VA records alone may have contributed to these low diagnosis rates. Future studies to confirm these findings could benefit from a larger sample size (including across different healthcare systems) or considering a population with a higher dementia/MCI prevalence. Future research efforts could also focus on enrolling more female patients to more accurately reflect the U.S. population (currently 50.8% female).37,38 Although women were underrepresented in this patient sample, the study group’s racial representation was reflective of overall VA patient demographics.37 Importantly, selection or confounding bias was also an inherent limitation in this observational study design—particularly as GeriPACT enrollment is voluntary and referral is based on patient as well as family preferences. While it is impossible to entirely eliminate this bias, we attempted to minimize this risk by collecting information around and matching on major social, financial, and medical factors that were most likely to contribute to the transfer of care and outcomes of interest. Finally, this study was not comparing either the cognitive assessment or the presence of documented diagnoses to a gold standard for MCI/dementia; therefore, we are not assessing the accuracy of the assessment or the documented dementia diagnosis, but instead aimed to better understand the relationship between the two variables. However, a conservative cut-off value for the instrument—that allowed us to highlight individuals who should be receiving diagnoses due to the presence of more advanced cognitive impairment—was chosen to minimize overdiagnosis.20
Under detection of cognitive impairment presents a major barrier to helping the millions of adults living with dementia and mild cognitive impairment. Our results support the need for further research focused on understanding the role that geriatrics-focused primary care clinics can play in improving dementia diagnosis and other outcomes for older adults. Future studies should include a larger patient population and enroll participants with characteristics under-addressed in this study (including female patients). Additionally, further studies into GeriPACT operating processes and procedures—including the effect of appointment times, specialty training, interdisciplinary support, and the size of patient panels on diagnosis rates—could highlight potential care models to improve care for older adults struggling with other chronic conditions.
Data Availability
The datasets generated and analyzed during the study are available from the corresponding author on reasonable request.
References
Matthews KA, Xu W, Gaglioti AH, et al. Racial and ethnic estimates of Alzheimer’s disease and related dementias in the United States (2015–2060) in adults aged ≥65 years. Alzheimer’s Dement. 2019;15(1):17-24. doi:https://doi.org/10.1016/j.jalz.2018.06.3063
Owens DK, Davidson KW, Krist AH, et al. Screening for Cognitive Impairment in Older Adults: US Preventive Services Task Force Recommendation Statement. JAMA. 2020;323(8):757-763. doi:https://doi.org/10.1001/jama.2020.0435
Borson S, Frank L, Bayley PJ, et al. Improving dementia care: the role of screening and detection of cognitive impairment. Alzheimers Dement. 2013;9(2):151-159. doi:https://doi.org/10.1016/j.jalz.2012.08.008
Amjad H, Roth DL, Samus QM, Yasar S, Wolff JL. Potentially Unsafe Activities and Living Conditions of Older Adults with Dementia. J Am Geriatr Soc. 2016;64(6):1223-1232. doi:https://doi.org/10.1111/jgs.14164
Rasmussen J, Langerman H. Alzheimer’s Disease – Why We Need Early Diagnosis. Degener Neurol Neuromuscul Dis. 2019;Volume 9:123-130. doi:https://doi.org/10.2147/dnnd.s228939
Alzheimer’s Association. Alzheimer’s disease facts and figures. Alzheimer’s Dement J Alzheimer’s Assoc. 2013;12:459–509.
Lang L, Clifford A, Wei L, et al. Prevalence and determinants of undetected dementia in the community: a systematic literature review and a meta-analysis. BMJ Open. 2017;7(2):e011146. doi:https://doi.org/10.1136/bmjopen-2016-011146
Tsoi KKF, Chan JYC, Hirai HW, Wong SYS, Kwok TCY. Cognitive Tests to Detect Dementia: A Systematic Review and Meta-analysis. JAMA Intern Med. 2015;175(9):1450-1458. doi:https://doi.org/10.1001/jamainternmed.2015.2152
Smith MM, Tremont G, Ott BR. A review of telephone-administered screening tests for dementia diagnosis. Am J Alzheimers Dis Other Demen. 2009;24(1):58-69. doi:https://doi.org/10.1177/1533317508327586
Alzheimer’s Association. 2020 Facts and Figures Report. Alzheimer’s Assoc. 2020:1–91. https://www.alz.org/alzheimers-dementia/facts-figures%0Ahttps://alz.org/alzheimers-dementia/facts-figures.
Bradford A, Kunik ME, Schulz P, Williams SP, Singh H. Missed and delayed diagnosis of dementia in primary care: prevalence and contributing factors. Alzheimer Dis Assoc Disord. 2009;23(4):306-314. doi:https://doi.org/10.1097/WAD.0b013e3181a6bebc
Engel PA, Spencer J, Paul T, Boardman JB. The Geriatrics in Primary Care Demonstration: Integrating Comprehensive Geriatric Care into the Medical Home: Preliminary Data. J Am Geriatr Soc. 2016;64(4):875-879. doi:https://doi.org/10.1111/jgs.14026
Zeiss AM, Steffen AM. Interdisciplinary health care teams: The basic unit of geriatric care. In: Carstensen LL, Edelstein BA, Dornbrand L, eds. The Practical Handbook of Clinical Gerontology; 1996:423-450.
Inouye SK, Studenski S, Tinetti ME, Kuchel GA. Geriatric Syndromes: Clinical, Research and Policy Implications of a Core Geriatric Concept. J Am Geriatr Soc. 2007;55(5):780-791. doi:https://doi.org/10.1007/s10955-011-0269-9.Quantifying
Williamson V, Stevelink SAM, Greenberg K, Greenberg N. Prevalence of Mental Health Disorders in Elderly U.S. Military Veterans: A Meta-Analysis and Systematic Review. Am J Geriatr Psychiatry. 2018;26(5):534-545. doi:https://doi.org/10.1016/j.jagp.2017.11.001
Alzheimer’s Association. 2022 Alzheimer’s Disease Facts and Figures; 2022. Accessed May 25th, 2022. https://www.alz.org/media/documents/alzheimers-facts-and-figures.pdf
Sullivan JL, Eisenstein R, Price T, Solimeo S, Shay K. Implementation of the geriatric patient-aligned care team model in the veterans health administration (VA). J Am Board Fam Med. 2018;31(3):456-465. doi:10.3122/jabfm.2018.03.170272
Department of Veterans Affairs Veterans Health Administration. VHA Directive 1140.07: Geriatric Patient Aligned Care Team. Washington D.C.; 2021.
Smith VA, Van Houtven CH, Lindquist JH, Hastings SN. Evaluation of a geriatrics primary care model using prospective matching to guide enrollment. BMC Med Res Methodol. 2021;21(1):167. doi:https://doi.org/10.1186/s12874-021-01360-4
Knopman DS, Roberts RO, Geda YE, et al. Validation of the telephone interview for cognitive status-modified in subjects with normal cognition, mild cognitive impairment, or dementia. Neuroepidemiology. 2010;34(1):34-42. doi:https://doi.org/10.1159/000255464
Callahan CM, Unverzagt FW, Hui SL, Perkins AJ, Hendrie HC. Six-item screener to identify cognitive impairment among potential subjects for clinical research. Med Care. 2002;40(9):771-781. doi:https://doi.org/10.1097/00005650-200209000-00007
Shah MN, Karuza J, Rueckmann E, Swanson P, Conwell Y, Katz P. Reliability and validity of prehospital case finding for depression and cognitive impairment. J Am Geriatr Soc. 2009;57(4):697-702. doi:https://doi.org/10.1111/j.1532-5415.2009.02185.x
Carpenter CR, DesPain B, Keeling TN, Shah M, Rothenberger M. The Six-Item Screener and AD8 for the detection of cognitive impairment in geriatric emergency department patients. Ann Emerg Med. 2011;57(6):653-661. doi:https://doi.org/10.1016/j.annemergmed.2010.06.560
Salazar R, Velez CE, Royall DR. Telephone screening for mild cognitive impairment in hispanics using the Alzheimer’s questionnaire. Exp Aging Res. 2014;40(2):129-139. doi:https://doi.org/10.1080/0361073X.2014.882189
Gallo JJ, Breitner JC. Alzheimer’s disease in the NAS-NRC Registry of aging twin veterans, IV. Performance characteristics of a two-stage telephone screening procedure for Alzheimer’s dementia. Psychol Med. 1995;25(6):1211-1219. doi:https://doi.org/10.1017/s0033291700033183
American Academy of Neurology. Mild Cognitive Impairment: Quality Measurement Set. 2018:1–54. https://www.aan.com/siteassets/home-page/policy-and-guidelines/quality/quality-measures/2019.03.25-mci-measures.pdf.
VHA Geriatrics and Extended Care. FY2022 VHA Dementia ICD Codes List; 2021.
Tsoy E, Kiekhofer RE, Guterman EL, et al. Assessment of Racial/Ethnic Disparities in Timeliness and Comprehensiveness of Dementia Diagnosis in California. JAMA Neurol. 2021;78(6):657-665. doi:https://doi.org/10.1001/jamaneurol.2021.0399
Lin PJ, Daly AT, Olchanski N, et al. Dementia Diagnosis Disparities by Race and Ethnicity. Med Care. 2021;59(8):679-686. doi:https://doi.org/10.1097/MLR.0000000000001577
Amjad H, Roth DL, Sheehan OC, Lyketsos CG, Wolff JL, Samus QM. Underdiagnosis of Dementia: an Observational Study of Patterns in Diagnosis and Awareness in US Older Adults. J Gen Intern Med. 2018;33(7):1131-1138. doi:https://doi.org/10.1007/s11606-018-4377-y
Andersen RM. Revisiting the behavioral model and access to medical care: does it matter? J Health Soc Behav. 1995;36(1):1-10. doi:https://doi.org/10.2307/2137284
Wang L, Porter B, Maynard C, et al. Predicting risk of hospitalization or death among patients with heart failure in the veterans health administration. Am J Cardiol. 2012;110(9):1342-1349. doi:https://doi.org/10.1016/j.amjcard.2012.06.038
Welsh KA, Breitner JCS, Magruder-Habib KM. Detection of dementia in the elderly using telephone screening of cognitive status. Cogn Behav Neurol. 1993; 6(2): 103–110.
De Jager CA, Budge MM, Clarke R. Utility of TICS-M for the assessment of cognitive function in older adults. Int J Geriatr Psychiatry. 2003;18(4):318-324. doi:https://doi.org/10.1002/gps.830
Sundström A, Westerlund O, Kotyrlo E. Marital status and risk of dementia: a nationwide population-based prospective study from Sweden. BMJ Open. 2016;6(1):e008565. doi:https://doi.org/10.1136/bmjopen-2015-008565
Helmer C, Damon D, Letenneur L, et al. Marital status and risk of Alzheimer’s disease: a French population-based cohort study. Neurology. 1999;53(9):1953-1958. doi:https://doi.org/10.1212/wnl.53.9.1953
National Center for Veterans Analysis and Statistics. Veteran Population. https://www.va.gov/vetdata/veteran_population.asp. Published 2021. Accessed February 8, 2021.
United States Census Bureau. QuickFacts: United States. https://www.census.gov/quickfacts/fact/table/US/PST045221. Accessed September 3, 2021.
Acknowledgements:
This work was supported in part by a VA Health Services Research and Development (HSR&D) grant (IIR 15-379) and received in-kind support from the Center of Innovation to Accelerate Discovery and Practice Transformation at the Durham VA Health Care System grant (CIN 13-410) from the United States (US) Department of Veterans Affairs. It was also supported in part by a grant from the National Institute on Aging of the National Institutes of Health (1R38AG065762). The contents do not represent the views of the US Department of Veterans Affairs, the United States Government, or Duke University. The authors have no relevant financial or non-financial interests to disclose. These findings were presented at the American Geriatrics Society Annual Meeting on May 13, 2022, Duke University Resident Research Day on May 20, 2022, and the SLAM-DUNC Symposium on June 25, 2022.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note:
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information:
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Perfect, C.R., Lindquist, J., Smith, V.A. et al. Are Geriatrics-Focused Primary Care Clinics Better at Diagnosing Dementia Than Traditional Clinics? A Matched Cohort Study. J GEN INTERN MED 38, 2710–2717 (2023). https://doi.org/10.1007/s11606-023-08136-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-023-08136-0