Abstract
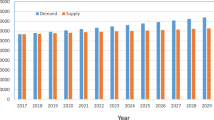
The regulation of duty hours of physicians in training remains among the most hotly debated subjects in medical education. Although recent duty hour reforms have been chiefly motivated by concerns about resident well-being and medical errors attributable to resident fatigue, the debate surrounding duty hour reform has infrequently involved discussion of one of the most important secular changes in hospital care that has affected nearly all developed countries over the last 3 decades: the declining demand for hospital care. For example, in 1980, we show that resident physicians in US teaching hospitals provided, on average, 1,302 inpatient days of care per resident physician compared to 593 inpatient days in 2011, a decline of 54 %. This decline in the demand for hospital care by residents provides an under-recognized economic rationale for reducing residency duty hours, a rationale based solely on supply and demand considerations. Work hour reductions and growing requirements for outpatient training can be seen as an appropriate response to the shrinking demand for hospital care across the health-care sector.


Similar content being viewed by others
References
Rybock JD. Residents’ duty hours and professionalism. N Engl J Med. 2009;361:930–931.
Axelrod L, Shah DJ, Jena AB. The European Working Time Directive: an uncontrolled experiment in medical care and education. JAMA. 2013;309:447–448.
Moonesinghe SR, Lowery J, Shahi N, Millen A, Beard JD. Impact of reduction in working hours for doctors in training on postgraduate medical education and patients’ outcomes: systematic review. BMJ 342:d1580 http://www.bmj.com/content/342/bmj.d1580.
Landrigan CP, Rothschild JM, Cronin JW, et al. Effect of reducing interns’ work hours on serious medical errors in intensive care units. N Engl J Med. 2004;351:1838–1848.
Buysse DJ, Barzansky B, Dinges D, et al. Sleep, fatigue, and medical training: setting an agenda for optimal learning and patient care. Sleep. 2003;26:218–225.
Barger LK, Cade BE, Ayas NT, et al. Extended work shifts and the risk of motor vehicle crashes among interns. N Engl J Med. 2005;352:125–134.
Poretz DM, Eron LJ, Goldenberg RI, et al. Intravenous antibiotic therapy in an outpatient setting. JAMA. 1982;248:336–339.
Investing in hospitals of the future. 2009. (Accessed May 9, 2014, at http://www.euro.who.int/__data/assets/pdf_file/0009/98406/E92354.pdf).
Block L, Habicht R, Wu AW, et al. In the wake of the 2003 and 2011 duty hours regulations, how do internal medicine interns spend their time? J Gen Intern Med. 2013;28:1042–1047.
Goitein L, Ludmerer KM. Resident workload—let’s treat the disease, not just the symptom: comment on “effect of the 2011 vs 2003 duty hour regulation–compliant models on sleep duration, trainee education, and continuity of patient care among internal medicine house staff”. JAMA Intern Med. 2013;173:655–656.
Funding Sources
Support was provided by the Office of the Director, National Institutes of Health (NIH Early Independence Award, 1DP5OD017897-01, Dr. Jena).
Conflict of Interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jena, A.B., DePasse, J.W. & Prasad, V. The Declining Demand for Hospital Care as a Rationale for Duty Hour Reform. J GEN INTERN MED 29, 1400–1403 (2014). https://doi.org/10.1007/s11606-014-2901-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-014-2901-2