Abstract
Background
Accurate prognostic estimation is crucial; however, the prognostic value of tumor deposits in gastric cancer remains controversial. This study aimed to investigate their prognostic significance.
Methods
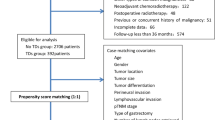
Clinicopathological and prognostic data of 1012 gastric cancer patients who underwent R0 or R1 surgery from 2010 to 2017 at the Osaka International Cancer Institute were retrospectively reviewed.
Results
Overall, 6.3% patients had tumor deposits, which were associated with Borrmann type, surgical procedure, type of gastrectomy, extent of lymphadenectomy, tumor size, histology, pT, pN, pM, pStage, lymphatic invasion, vascular invasion, preoperative chemotherapy, and postoperative chemotherapy. Tumor deposit-positive patients had worse 5-year disease-free survival (32.60% vs. 92.45%) and overall survival (41.22% vs. 89.37%) than tumor deposit-negative patients. Subgroup analysis regarding pStage II–III also showed significant differences between patients with and without tumor deposits for 5-year disease-free survival (34.15% vs. 80.98%) and overall survival (43.17% vs. 75.78%). Multivariable analysis showed that older age, undifferentiated histology, deeper tumor invasion, lymph node metastasis, distant metastasis, and presence of tumor deposits were significantly correlated with early tumor recurrence and shorter survival time; these factors were identified as independent prognostic factors. The 5-year disease-free survival of tumor deposit-positive patients was significantly worse than that of patients in the pStage III group and comparable to that of patients in the pT4, pN3, and pM1 groups. The 5-year overall survival of tumor deposit-positive patients was comparable to that of the pT4, pN3, pM1, and pStage III groups.
Conclusions
Tumor deposits are strong and independent predictors of tumor recurrence and poor survival.




Similar content being viewed by others
Data Availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Smyth EC, Nilsson M, Grabsch HI, van Grieken NC, Lordick F. Gastric cancer. Lancet 2020; 396(10251):635-648.
Amin MB, Edge, S., Greene, F., Byrd, D.R., Brookland, R.K., Washington, M.K., Gershenwald, J.E., Compton, C.C., Hess, K.R., Sullivan, D.C., Jessup, J.M., Brierley, J.D., Gaspar, L.E., Schilsky, R.L., Balch, C.M., Winchester, D.P., Asare, E.A., Madera, M., Gress, D.M., Meyer, L.R. (Eds.). Gastric Cancer AJCC 8th Ed.
J.D.Brierley, M.K.Gospodarowicz & C.Wittekind. TNM Classification of Malignant Tumours, 8th ed.State of New Jersey: JOHN WILEY & SONS, LTD., 2017.
Japanese Gastric Cancer Treatment Guidelines 2021 (6th edition). Gastric Cancer 2023; 26(1):1–25.
Gabriel WB. A Small High-grade Carcinoma of the Rectum with Extensive Lymphatic Spread. Proc R Soc Med 1947; 40(13):833-834.
Mignano JE, Zahurak ML, Chakravarthy A, Piantadosi S, Dooley WC, Gage I. Significance of axillary lymph node extranodal soft tissue extension and indications for postmastectomy irradiation. Cancer 1999; 86(7):1258-1262.
Lee YC, Wu CT, Kuo SW, Tseng YT, Chang YL. Significance of extranodal extension of regional lymph nodes in surgically resected non-small cell lung cancer. Chest 2007; 131(4):993-999.
Sarioglu S, Akbulut N, Iplikci S, Aydin B, Dogan E, Unlu M, Ellidokuz H, Ada E, Akman F, Ikiz AO. Tumor deposits in head and neck carcinomas. Head Neck 2016; 38 Suppl 1:E256-260.
Puppa G, Ueno H, Kayahara M, Capelli P, Canzonieri V, Colombari R, Maisonneuve P, Pelosi G. Tumor deposits are encountered in advanced colorectal cancer and other adenocarcinomas: an expanded classification with implications for colorectal cancer staging system including a unifying concept of in-transit metastases. Mod Pathol 2009; 22(3):410-415.
Liang Y, Wu L, Liu L, Ding X, Wang X, Liu H, Meng J, Xu R, He D, Liang H. Impact of extranodal tumor deposits on prognosis and N stage in gastric cancer. Surgery 2019; 166(3):305-313.
Anup S, Lu J, Zheng CH, Li P, Xie JW, Wang JB, Lin JX, Chen QY, Cao LL, Lin M, Yu Q, Yang YH, Huang CM. Prognostic significance of perigastric tumor deposits in patients with primary gastric cancer. BMC Surg 2017; 17(1):84.
Wenquan L, Yuhua L, Jianxin C, Hongqing X, Kecheng Z, Jiyang L, Yunhe G, Yi L, Wang Z, Shaoqing L, Yixun L, Shen Q, Wanguo X, Zhi Q, Lin C. Tumor deposit serves as a prognostic marker in gastric cancer: A propensity score-matched analysis comparing survival outcomes. Cancer Med 2020; 9(10):3268-3277.
Nagtegaal ID, Tot T, Jayne DG, McShane P, Nihlberg A, Marshall HC, Pahlman L, Brown JM, Guillou PJ, Quirke P. Lymph nodes, tumor deposits, and TNM: are we getting better? J Clin Oncol 2011; 29(18):2487-2492.
. Japanese classification of gastric carcinoma: 3rd English edition. Gastric Cancer 2011; 14(2):101–112.
Japanese gastric cancer treatment guidelines 2018 (5th edition). Gastric Cancer 2021; 24(1):1–21.
Lauren P. THE TWO HISTOLOGICAL MAIN TYPES OF GASTRIC CARCINOMA: DIFFUSE AND SO-CALLED INTESTINAL-TYPE CARCINOMA. AN ATTEMPT AT A HISTO-CLINICAL CLASSIFICATION. Acta Pathol Microbiol Scand 1965; 64:31–49.
Lee HS, Lee HE, Yang HK, Kim WH. Perigastric tumor deposits in primary gastric cancer: implications for patient prognosis and staging. Ann Surg Oncol 2013; 20(5):1604-1613.
Sun Z, Wang ZN, Xu YY, Zhu GL, Huang BJ, Xu Y, Liu FN, Zhu Z, Xu HM. Prognostic significance of tumor deposits in gastric cancer patients who underwent radical surgery. Surgery 2012; 151(6):871-881.
Tan J, Yang B, Xu Z, Zhou S, Chen Z, Huang J, Gao H, Zheng S, Wen L, Han F. Tumor deposit indicates worse prognosis than metastatic lymph node in gastric cancer: a propensity score matching study. Ann Transl Med 2019; 7(22):671.
Wang W, Li Y, Zhang Y, Yuan X, Xu D, Guan Y, Feng X, Chen Y, Sun X, Li W, Zhan Y, Zhou Z. (2011) Incorporation of extranodal metastasis of gastric carcinoma into the 7th edition UICC TNM staging system. PoS One. 6(6):e19557
Yildiz B, Etiz D, Dal P, Junushova B, Pasaoglu O, Yilmaz E, Erkasap S, Dincer M. Tumor deposits: Prognostic significance in gastric cancer patients. J buon 2016; 21(6):1476-1481.
Al-Batran SE, Homann N, Pauligk C, Goetze TO, Meiler J, Kasper S, Kopp HG, Mayer F, Haag GM, Luley K, Lindig U, Schmiegel W, Pohl M, Stoehlmacher J, Folprecht G, Probst S, Prasnikar N, Fischbach W, Mahlberg R, Trojan J, Koenigsmann M, Martens UM, Thuss-Patience P, Egger M, Block A, Heinemann V, Illerhaus G, Moehler M, Schenk M, Kullmann F, Behringer DM, Heike M, Pink D, Teschendorf C, Löhr C, Bernhard H, Schuch G, Rethwisch V, von Weikersthal LF, Hartmann JT, Kneba M, Daum S, Schulmann K, Weniger J, Belle S, Gaiser T, Oduncu FS, Güntner M, Hozaeel W, Reichart A, Jäger E, Kraus T, Mönig S, Bechstein WO, Schuler M, Schmalenberg H, Hofheinz RD. Perioperative chemotherapy with fluorouracil plus leucovorin, oxaliplatin, and docetaxel versus fluorouracil or capecitabine plus cisplatin and epirubicin for locally advanced, resectable gastric or gastro-oesophageal junction adenocarcinoma (FLOT4): a randomised, phase 2/3 trial. Lancet 2019; 393(10184):1948-1957.
Kang YK, Yook JH, Park YK, Lee JS, Kim YW, Kim JY, Ryu MH, Rha SY, Chung IJ, Kim IH, Oh SC, Park YS, Son T, Jung MR, Heo MH, Kim HK, Park C, Yoo CH, Choi JH, Zang DY, Jang YJ, Sul JY, Kim JG, Kim BS, Beom SH, Cho SH, Ryu SW, Kook MC, Ryoo BY, Kim HK, Yoo MW, Lee NS, Lee SH, Kim G, Lee Y, Lee JH, Noh SH. PRODIGY: A Phase III Study of Neoadjuvant Docetaxel, Oxaliplatin, and S-1 Plus Surgery and Adjuvant S-1 Versus Surgery and Adjuvant S-1 for Resectable Advanced Gastric Cancer. J Clin Oncol 2021; 39(26):2903-2913.
Thumaty DB, Chacko RT, John AO, Joel A, Georgy JT, Jacob M, Samarasam I, Masih D, Isaiah R, Jeyaseelan V, Singh A. Docetaxel, Oxaliplatin and Capecitabine (TEX) triplet regimen as adjuvant chemotherapy in resected gastric adenocarcinoma. Ecancermedicalscience 2021; 15:1292.
Wu L, Feng Y, Wu Z, Xu H, Zhang C, Ning J, Wang R, Chen J, Xie M, Zhang Y, Bu L, Hao J, Ma T. Survival outcomes of adjuvant taxanes, platinum plus fluoropyrimidines versus platinum and fluoropyrimidines for gastric cancer patients after D2 gastrectomy: a retrospective propensity score-matched analysis. World J Surg Oncol 2021; 19(1):272.
Zhang M, Hu W, Hu K, Lin Y, Feng Z, Yun JP, Gao N, Zhang L. Association of KRAS mutation with tumor deposit status and overall survival of colorectal cancer. Cancer Causes Control 2020; 31(7):683-689.
Author information
Authors and Affiliations
Contributions
All the authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Kaoru Fujikawa and Takeshi Omori. The first draft of the manuscript was written by Kaoru Fujikawa, and all the authors commented on previous versions of the manuscript. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fujikawa, K., Omori, T., Shinno, N. et al. Tumor Deposit Is an Independent Factor Predicting Early Recurrence and Poor Prognosis in Gastric Cancer. J Gastrointest Surg 27, 1336–1344 (2023). https://doi.org/10.1007/s11605-023-05668-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-023-05668-y