Abstract
Background
Pouchitis is a common late complication in patients with ulcerative colitis (UC) who undergo ileal pouch–anal anastomosis (IPAA). The heterogeneous nature of the clinical and endoscopic presentations could affect the evaluation of therapeutic interventions for pouchitis. Thus, identifying the risk factors and clinical outcomes of pouch inflammation at different sites and severity is becoming increasingly important for colorectal surgeons.
Methods
Data on patients who underwent IPAA January from 2008 to June 2022 in our three pouch centers affiliated with the China UC Pouch Center Union were retrospectively collected. Pouchitis was categorized as a different phenotype according to the Chicago Classification. J pouches were classified into short (14 ± 2 cm) and long pouches (22 ± 2 cm) according to the distribution of ileal pouch length in our institute.
Results
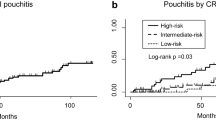
Altogether, 143 patients with a median follow-up time of 5.0 years (interquartile range: 2.0–8.0) were enrolled. Among them, 41 patients (28.7%) developed pouchitis and 32 patients (78%) had diffuse inflammation of the pouch. Patients with diffuse pouchitis had a higher pouchitis disease activity index and more seriously impaired improvement of long-term quality of life than those with pouch phenotypes. A short J pouch, recurrent UC, and preoperative high white blood cell count were independent risk factors for diffuse pouchitis. Furthermore, a short J pouch could effectively predict the occurrence of diffuse pouchitis with an area under the receiver-operating characteristic curve of 0.614, a sensitivity of 62.5%, and a specificity of 60.4% (p = 0.049) and significantly decreased the overall diffuse pouchitis-free survival compared to a long J pouch (p = 0.0002).
Conclusion
Diffuse pouchitis is a common phenotype of pouchitis that seriously impairs long-term prognosis. For colorectal surgeons, decision-making regarding pouch construction with an appropriate length should be considered to prevent the development of diffuse pouchitis.
Graphical Abstract





Similar content being viewed by others
Data Availability
The data supporting the conclusions of this article will be made available by the authors.
References
R. Marchioni Beery, S. Kane, Current approaches to the management of new-onset ulcerative colitis, Clinical and experimental gastroenterology, 7 (2014) 111-132.
A.G. Parks, R.J. Nicholls, Proctocolectomy without ileostomy for ulcerative colitis, British medical journal, 2 (1978) 85-88.
V.W. Fazio, M.G. O'Riordain, I.C. Lavery, J.M. Church, P. Lau, S.A. Strong, T. Hull, Long-term functional outcome and quality of life after stapled restorative proctocolectomy, Annals of surgery, 230 (1999) 575-584; discussion 584-576.
V.W. Fazio, Y. Ziv, J.M. Church, J.R. Oakley, I.C. Lavery, J.W. Milsom, T.K. Schroeder, Ileal pouch-anal anastomoses complications and function in 1005 patients, Annals of surgery, 222 (1995) 120-127.
F. Michelassi, J. Lee, M. Rubin, A. Fichera, K. Kasza, T. Karrison, R.D. Hurst, Long-term functional results after ileal pouch anal restorative proctocolectomy for ulcerative colitis: a prospective observational study, Annals of surgery, 238 (2003) 433-441; discussion 442-435.
W. Xu, H. Ye, Y. Zhu, W. Ding, J. Fu, L. Cui, P. Du, Long-term quality of life associated with early surgical complications in patients with ulcerative colitis after ileal pouch-anal anastomosis: A single-center retrospective study, International journal of surgery (London, England), 48 (2017) 174-179.
U. Mahadevan, W.J. Sandborn, Diagnosis and management of pouchitis, Gastroenterology, 124 (2003) 1636-1650.
J. Landy, H.O. Al-Hassi, S.D. McLaughlin, S.C. Knight, P.J. Ciclitira, R.J. Nicholls, S.K. Clark, A.L. Hart, Etiology of pouchitis, Inflammatory bowel diseases, 18 (2012) 1146-1155.
V.W. Fazio, R.P. Kiran, F.H. Remzi, J.C. Coffey, H.M. Heneghan, H.T. Kirat, E. Manilich, B. Shen, S.T. Martin, Ileal pouch anal anastomosis: analysis of outcome and quality of life in 3707 patients, Annals of surgery, 257 (2013) 679-685.
E. Manilich, F.H. Remzi, V.W. Fazio, J.M. Church, R.P. Kiran, Prognostic modeling of preoperative risk factors of pouch failure, Diseases of the colon and rectum, 55 (2012) 393-399.
P.P. Tekkis, R.E. Lovegrove, H.S. Tilney, J.J. Smith, P.M. Sagar, A.J. Shorthouse, N.J. Mortensen, R.J. Nicholls, Long-term failure and function after restorative proctocolectomy - a multi-centre study of patients from the UK National Ileal Pouch Registry, Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland, 12 (2010) 433-441.
W.J. Sandborn, W.J. Tremaine, K.P. Batts, J.H. Pemberton, S.F. Phillips, Pouchitis after ileal pouch-anal anastomosis: a Pouchitis Disease Activity Index, Mayo Clinic proceedings, 69 (1994) 409-415.
B. Shen, J.P. Achkar, B.A. Lashner, A.H. Ormsby, F.H. Remzi, C.L. Bevins, A. Brzezinski, R.E. Petras, V.W. Fazio, Endoscopic and histologic evaluation together with symptom assessment are required to diagnose pouchitis, Gastroenterology, 121 (2001) 261-267.
W. Xu, W. Tang, W. Ding, H. Hu, W. Chen, Q. Qian, L. Cui, Z. Ding, P. Du, Preoperative Endoscopic Activity Predicts the Occurrence of Pouchitis After Ileal Pouch-Anal Anastomosis in Ulcerative Colitis: A Multicenter Retrospective Study in China, Frontiers in surgery, 8 (2021) 740349.
S. Akiyama, J.E. Ollech, V. Rai, L.R. Glick, Y. Yi, C. Traboulsi, J. Runde, R.D. Cohen, K.B. Skowron, R.D. Hurst, K. Umanskiy, B.D. Shogan, N.H. Hyman, M.A. Rubin, S.R. Dalal, A. Sakuraba, J. Pekow, E.B. Chang, D.T. Rubin, Endoscopic Phenotype of the J Pouch in Patients With Inflammatory Bowel Disease: A New Classification for Pouch Outcomes, Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association, 20 (2022) 293-302.e299.
J.C. Coffey, D.C. Winter, P. Neary, A. Murphy, H.P. Redmond, W.O. Kirwan, Quality of life after ileal pouch-anal anastomosis: an evaluation of diet and other factors using the Cleveland Global Quality of Life instrument, Diseases of the colon and rectum, 45 (2002) 30-38.
M.S. Silverberg, J. Satsangi, T. Ahmad, I.D. Arnott, C.N. Bernstein, S.R. Brant, R. Caprilli, J.F. Colombel, C. Gasche, K. Geboes, D.P. Jewell, A. Karban, E.V. Loftus, Jr., A.S. Peña, R.H. Riddell, D.B. Sachar, S. Schreiber, A.H. Steinhart, S.R. Targan, S. Vermeire, B.F. Warren, Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a Working Party of the 2005 Montreal World Congress of Gastroenterology, Canadian journal of gastroenterology = Journal canadien de gastroenterologie, 19 Suppl A (2005) 5a-36a.
A. Cheifetz, S. Itzkowitz, The diagnosis and treatment of pouchitis in inflammatory bowel disease, Journal of clinical gastroenterology, 38 (2004) S44-50.
D.S. Pardi, W.J. Sandborn, Systematic review: the management of pouchitis, Alimentary pharmacology & therapeutics, 23 (2006) 1087-1096.
M. Turina, C.J. Pennington, J. Kimberling, A.J. Stromberg, R.E. Petras, S. Galandiuk, Chronic pouchitis after ileal pouch-anal anastomosis for ulcerative colitis: effect on quality of life, Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract, 10 (2006) 600-606.
M. Kayal, M. Plietz, M. Radcliffe, A. Rizvi, C. Yzet, E. Tixier, R.P. Hirten, B. Cohen, P. Sylla, S. Khaitov, A. Greenstein, J.F. Colombel, M.C. Dubinsky, R.C. Ungaro, Endoscopic activity in asymptomatic patients with an ileal pouch is associated with an increased risk of pouchitis, Alimentary pharmacology & therapeutics, 50 (2019) 1189-1194.
B. Shen, F.H. Remzi, I.C. Lavery, B.A. Lashner, V.W. Fazio, A proposed classification of ileal pouch disorders and associated complications after restorative proctocolectomy, Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association, 6 (2008) 145-158; quiz 124.
S.A. Miratashi Yazdi, M.S. Fazeli, H. Ahmadi Amoli, E. Rahimpour, B. Behboudi, Functional and quality of life outcomes after ileal pouch-anal anastomosis in short versus long ileal J-pouch configuration in ulcerative colitis patients: a cohort study, Updates in surgery, 72 (2020) 827-833.
Y. Li, S. Xia, X. Jiang, C. Feng, S. Gong, J. Ma, Z. Fang, J. Yin, Y. Yin, Gut Microbiota and Diarrhea: An Updated Review, Frontiers in cellular and infection microbiology, 11 (2021) 625210.
J.F. LeBlanc, J.P. Segal, L.M. de Campos Braz, A.L. Hart, The Microbiome as a Therapy in Pouchitis and Ulcerative Colitis. Nutrients, 13 (2021).
A.N. Anbazhagan, S. Priyamvada, W.A. Alrefai, P.K. Dudeja, Pathophysiology of IBD associated diarrhea, Tissue barriers, 6 (2018) e1463897.
Funding
This work was supported by the National Natural Science Foundation of China (No. 82000481, 82270549, and 81873547), the Shanghai Sailing Program (No. 20YF1429400) and the Qingfeng Scientific Research Fund of the China Crohn’s & Colitis Foundation (CCCF) (No. CCCF-QF-2022C14-21).
Author information
Authors and Affiliations
Contributions
Peng Du and Zhao Ding conceived the study. Weimin Xu analyzed the data and wrote the manuscript. Yaosheng Wang and Zhebin Hua assisted some analysis. Hang Hu, Wenhao Chen, and Zerong Cai collaborated to collect the information of patients. Long Cui, Xiaojian Wu, and Lei Lian reviewed and revised the manuscript. All authors approved the final version.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xu, W., Wang, Y., Hua, Z. et al. Risk Factors and Quality of Life in Patients with Diffuse Pouchitis After Ileal Pouch Anal Anastomosis According to the Chicago Classification for J Pouch: a Retrospective Multicenter Cohort Study in China. J Gastrointest Surg 27, 766–776 (2023). https://doi.org/10.1007/s11605-022-05563-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-022-05563-y