Abstract
Background
Simple ileocecectomy and right hemicolectomy are two potential operative approaches to treat patients with neuroendocrine neoplasm in the terminal ileum and/or cecum (IC-NENs). We sought to define the long-term outcome of patients undergoing ileocecectomy versus right hemicolectomy for IC-NENs, as well as characterize number of nodes evaluated and lymph node metastasis (LNM) associated with each procedure.
Methods
Patients who underwent curative-intent resections for IC-NENs between 2000 and 2016 were identified from a multi-institutional database. The clinicopathologic characteristics, surgical procedures, and the overall (OS) and recurrence-free survival (RFS) were compared among patients who underwent formal right hemicolectomy versus ileocecectomy only.
Results
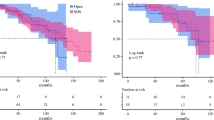
Among 127 patients with IC-NENs, median size of the largest tumor size was 2.0 (IQR 1.2–2.9) cm; 35 (27.6%) patients had multiple lesions. At the time of surgery, 93 (73.2%) patients underwent a right hemicolectomy, whereas 34 (26.8%) had ileocecectomy only. Every patient had a lymph node dissection (LND) with a median number of 16 (IQR 12–22) nodes evaluated. A majority (n = 110, 86.6%) of patients had LNM with a median number of 3 (IQR 2–5) LNM. Patients who underwent hemicolectomy had more lymph nodes evaluated versus patients who had an ileocecectomy only (median, 18 vs. 14, p = 0.004). Patients who underwent formal right hemicolectomy versus ileocecectomy had a similar OS (median OS, 101.9 vs. 144.5 months, p = 0.44) and RFS (median RFS, 70.3 vs. not attained, p = 0.80), respectively.
Conclusions
Ileocecectomy had similar long-term outcomes versus right hemicolectomy in treatment of IC-NENs despite a difference in the lymph node harvest.



Similar content being viewed by others
References
Dasari A, Shen C, Halperin D, et al. Trends in the Incidence, Prevalence, and Survival Outcomes in Patients With Neuroendocrine Tumors in the United States. JAMA Oncol. 2017;3:1335-1342.
Kacmaz E, Klumpen HJ, Bemelman WA, Nieveen van Dijkum EJM, Engelsman AF, Tanis PJ. Evaluating Nationwide Application of Minimally Invasive Surgery for Treatment of Small Bowel Neuroendocrine Neoplasms. World J Surg. 2021;45:2463-2470.
Benson AB, Venook AP, Al-Hawary MM, et al. Small Bowel Adenocarcinoma, Version 1.2020, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Netw. 2019;17:1109-1133.
Shah MH, Goldner WS, Benson AB, et al. Neuroendocrine and Adrenal Tumors, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Netw. 2021;19:839-868.
Boudreaux JP, Klimstra DS, Hassan MM, et al. The NANETS consensus guideline for the diagnosis and management of neuroendocrine tumors: well-differentiated neuroendocrine tumors of the Jejunum, Ileum, Appendix, and Cecum. Pancreas. 2010;39:753-766.
Salazar R, Wiedenmann B, Rindi G, Ruszniewski P. ENETS 2011 Consensus Guidelines for the Management of Patients with Digestive Neuroendocrine Tumors: an update. Neuroendocrinology. 2012;95:71-73.
Pedrazzani C, Conti C, Valdegamberi A, et al. Is Laparoscopic CME Right Hemicolectomy an Optimal Indication for NET of the Right Colon and Terminal Ileum? J Gastrointest Surg. 2021;25:333-336.
Broder MS, Cai B, Chang E, Neary MP. Epidemiology of Gastrointestinal Neuroendocrine Tumors in a U.S. Commercially Insured Population. Endocr Pract. 2017;23:1210-1216.
Kulke MH, Shah MH, Benson AB, 3rd, et al. Neuroendocrine tumors, version 1.2015. J Natl Compr Canc Netw. 2015;13:78-108.
Pape UF, Perren A, Niederle B, et al. ENETS Consensus Guidelines for the management of patients with neuroendocrine neoplasms from the jejuno-ileum and the appendix including goblet cell carcinomas. Neuroendocrinology. 2012;95:135-156.
Crown A, Simianu VV, Kennecke H, et al. Appendiceal Neuroendocrine Tumors: Does Colon Resection Improve Outcomes? J Gastrointest Surg. 2020;24:2121-2126.
Mehrvarz Sarshekeh A, Advani S, Halperin DM, et al. Regional lymph node involvement and outcomes in appendiceal neuroendocrine tumors: a SEER database analysis. Oncotarget. 2017;8:99541-99551.
Zhang XF, Xue F, Wu Z, et al. (2020) Development and Validation of a Modified Eighth AJCC Staging System for Primary Pancreatic Neuroendocrine Tumors. Ann Surg
Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250:187-196.
Ricci C, Ingaldi C, Alberici L, et al. Histopathological diagnosis of appendiceal neuroendocrine neoplasms: when to perform a right hemicolectomy? A systematic review and meta-analysis. Endocrine. 2019;66:460-466.
Alabraba E, Pritchard DM, Griffin R, et al. The impact of lymph node metastases and right hemicolectomy on outcomes in appendiceal neuroendocrine tumours (aNETs). Eur J Surg Oncol. 2021;47:1332-1338.
Holmager P, Willemoe GL, Nielsen K, et al. Neuroendocrine neoplasms of the appendix: Characterization of 335 patients referred to the Copenhagen NET Center of Excellence. Eur J Surg Oncol. 2021;47:1357-1363.
Rault-Petit B, Do Cao C, Guyetant S, et al. Current Management and Predictive Factors of Lymph Node Metastasis of Appendix Neuroendocrine Tumors: A National Study from the French Group of Endocrine Tumors (GTE). Ann Surg. 2019;270:165-171.
Pape UF, Niederle B, Costa F, et al. ENETS Consensus Guidelines for Neuroendocrine Neoplasms of the Appendix (Excluding Goblet Cell Carcinomas). Neuroendocrinology. 2016;103:144-152.
Nasseri YY, Zhu R, Sutanto C, et al. Role of right hemicolectomy in patients with low-grade appendiceal mucinous adenocarcinoma. Am J Surg. 2019;218:1239-1243.
Xu L, Su X, He Z, et al. Short-term outcomes of complete mesocolic excision versus D2 dissection in patients undergoing laparoscopic colectomy for right colon cancer (RELARC): a randomised, controlled, phase 3, superiority trial. Lancet Oncol. 2021;22:391-401.
Kim MK, Warner RR, Ward SC, et al. Prognostic significance of lymph node metastases in small intestinal neuroendocrine tumors. Neuroendocrinology. 2015;101:58-65.
Zaidi MY, Lopez-Aguiar AG, Dillhoff M, et al. Prognostic Role of Lymph Node Positivity and Number of Lymph Nodes Needed for Accurately Staging Small-Bowel Neuroendocrine Tumors. JAMA Surg. 2019;154:134-140.
Chi W, Warner RRP, Chan DL, et al. Long-term Outcomes of Gastroenteropancreatic Neuroendocrine Tumors. Pancreas. 2018;47:321-325.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, MX., Lopez-Aguiar, A.G., Poultsides, G. et al. Surgical Treatment of Neuroendocrine Tumors of the Terminal Ileum or Cecum: Ileocecectomy Versus Right Hemicolectomy. J Gastrointest Surg 26, 1266–1274 (2022). https://doi.org/10.1007/s11605-022-05269-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-022-05269-1