Abstract
Background
Exocrine pancreatic insufficiency (EPI) occurs when pancreatic enzyme activity in the intestinal lumen is insufficient for normal digestion to occur. The true incidence and diagnosis of EPI after pancreatectomy has not been fully understood and optimized. The aim of this study was to present incidence and diagnostic criteria for EPI after pancreatectomy for cancer and provide a guide for management and optimal therapy in pancreatectomy patients with cancer.
Methods
A comprehensive review of the literature with publication dates from 2014 to 2019 was performed. A comprehensive diagnostic and treatment algorithm was then created based on literature review and current treatment options.
Results
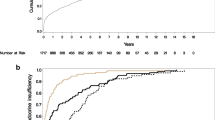
In total, 30 studies were included, 19 combined both pancreaticoduodenectomy (PD) and distal pancreatectomy (DP), 9 for central pancreatectomy, and 2 others. EPI was defined subjectively without definitive testing using any of the established diagnostic studies in the majority of studies 23 (76%). Preoperative EPI was calculated to be 11.52%. Most studies assessed exocrine function at least 6 months postoperatively with four studies extending the follow-up period beyond 12 months. EPI diagnosed postoperatively at 1 month (40.27%), 3 months (30.94%), 6 months (36.06%), and 12 months (34.69%). After PD, the median prevalence of postoperative EPI was 43.14%, CP, the median prevalence was 4.85%, DP, median prevalence of postoperative EPI of 11.94%.
Conclusion
EPI is a frequent outcome that is often misdiagnosed or under-reported by the patient post-pancreatectomy. Given the increasing overall survival in pancreatectomy patients for cancer, surgeon awareness and assessment is critical to improving patients’ overall quality of life.


Similar content being viewed by others
References
Conroy T, Hammel P, Hebbar M, et al. FOLFIRINOX or Gemcitabine as Adjuvant Therapy for Pancreatic Cancer. N Engl J Med. 2018;379(25):2395-2406.
Halloran CM, Cox TF, Chauhan S, et al. Partial pancreatic resection for pancreatic malignancy is associated with sustained pancreatic exocrine failure and reduced quality of life: a prospective study. Pancreatology. 2011;11(6):535-545.
Partelli S, Frulloni L, Minniti C, et al. Faecal elastase-1 is an independent predictor of survival in advanced pancreatic cancer. Dig Liver Dis. 2012;44(11):945-951.
Dominguez-Munoz JE. Pancreatic enzyme therapy for pancreatic exocrine insufficiency. Curr Gastroenterol Rep. 2007;9(2):116-122.
Kahl S, Malfertheiner P. Exocrine and endocrine pancreatic insufficiency after pancreatic surgery. Best Pract Res Clin Gastroenterol. 2004;18(5):947-955.
Friess H, Michalski CW. Diagnosing exocrine pancreatic insufficiency after surgery: when and which patients to treat. HPB (Oxford). 2009;11 Suppl 3:7-10.
Sikkens EC, Cahen DL, de Wit J, Looman CW, van Eijck C, Bruno MJ. Prospective assessment of the influence of pancreatic cancer resection on exocrine pancreatic function. Br J Surg. 2014;101(2):109-113.
Scholten L, Stoop TF, Del Chiaro M, et al. Systematic review of functional outcome and quality of life after total pancreatectomy. Br J Surg. 2019;106(13):1735-1746.
Stoop TF, Ateeb Z, Ghorbani P, et al. Impact of Endocrine and Exocrine Insufficiency on Quality of Life After Total Pancreatectomy. Ann Surg Oncol. 2019.
Capurso G, Traini M, Piciucchi M, Signoretti M, Arcidiacono PG. Exocrine pancreatic insufficiency: prevalence, diagnosis, and management. Clin Exp Gastroenterol. 2019;12:129-139.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009;62(10):e1-34.
Tseng DS, Molenaar IQ, Besselink MG, van Eijck CH, Borel Rinkes IH, van Santvoort HC. Pancreatic Exocrine Insufficiency in Patients With Pancreatic or Periampullary Cancer: A Systematic Review. Pancreas. 2016;45(3):325-330.
Agency for Healthcare Research and Quality. National Guideline C. Practicing Chiropractors’ Committee on Radiology Protocols (PCCRP) for biomechanical assessment of spinal subluxation in chiropractic clinical practice. https://www.ahrq.gov/gam/index.html. Published 2014. Accessed 8/11/2014.
Keller J, Meier V, Wolfram KU, Rosien U, Layer P. Sensitivity and specificity of an abbreviated (13)C-mixed triglyceride breath test for measurement of pancreatic exocrine function. United European Gastroenterol J. 2014;2(4):288-294.
Steinberg WM, Anderson KK. Serum trypsinogen in diagnosis of chronic pancreatitis. Dig Dis Sci. 1984;29(11):988-993.
Tjaden C, Hassenpflug M, Hinz U, et al. Outcome and prognosis after pancreatectomy in patients with solid pseudopapillary neoplasms. Pancreatology. 2019;19(5):699-709.
Shi Y, Wang Y, Wang J, et al. Learning curve of robot-assisted middle pancreatectomy (RMP): experience of the first 100 cases from a high-volume pancreatic center in China. Surg Endosc. 2019.
Xiao W, Zhu J, Peng L, Hong L, Sun G, Li Y. The role of central pancreatectomy in pancreatic surgery: a systematic review and meta-analysis. HPB (Oxford). 2018;20(10):896-904.
Senthilnathan P, Gul SI, Gurumurthy SS, et al. Laparoscopic central pancreatectomy: Our technique and long-term results in 14 patients. J Minim Access Surg. 2015;11(3):167-171.
Goudard Y, Gaujoux S, Dokmak S, et al. Reappraisal of central pancreatectomy a 12-year single-center experience. JAMA Surg. 2014;149(4):356-363.
Zhang T, Wang X, Huo Z, et al. Robot-Assisted Middle Pancreatectomy for Elderly Patients: Our Initial Experience. Med Sci Monit. 2015;21:2851-2860.
Kang P, Wang Z, Leng K, et al. Binding pancreaticogastrostomy anastomosis in central pancreatectomy: A single center experience. Medicine (Baltimore). 2017;96(45):e8354.
Hong D, Liu Y, Peng S, et al. Binding pancreaticogastrostomy in laparoscopic central pancreatectomy: a novel technique in laparoscopic pancreatic surgery. Surg Endosc. 2016;30(2):715-720.
Jiang CY, Wang W. Initial experience in total laparoscopic central pancreatectomy with pancreatogastrostomy. Cell Biochem Biophys. 2015;71(2):1023-1028.
Jilesen AP, van Eijck CH, Busch OR, van Gulik TM, Gouma DJ, van Dijkum EJ. Postoperative Outcomes of Enucleation and Standard Resections in Patients with a Pancreatic Neuroendocrine Tumor. World J Surg. 2016;40(3):715-728.
Lim PW, Dinh KH, Sullivan M, et al. Thirty-day outcomes underestimate endocrine and exocrine insufficiency after pancreatic resection. HPB (Oxford). 2016;18(4):360-366.
Neophytou H, Wangermez M, Gand E, Carretier M, Danion J, Richer JP. Predictive factors of endocrine and exocrine insufficiency after resection of a benign tumour of the pancreas. Ann Endocrinol (Paris). 2018;79(2):53-61.
Wang X, Chen YH, Tan CL, et al. Enucleation of pancreatic solid pseudopapillary neoplasm: Short-term and long-term outcomes from a 7-year large single-center experience. Eur J Surg Oncol. 2018;44(5):644-650.
Maignan A, Ouaissi M, Turrini O, et al. Risk factors of exocrine and endocrine pancreatic insufficiency after pancreatic resection: A multi-center prospective study. J Visc Surg. 2018;155(3):173-181.
Hirono S, Murakami Y, Tani M, et al. Identification of risk factors for pancreatic exocrine insufficiency after pancreaticoduodenectomy using a 13C-labeled mixed triglyceride breath test. World J Surg. 2015;39(2):516-525.
Okano K, Murakami Y, Nakagawa N, et al. Remnant pancreatic parenchymal volume predicts postoperative pancreatic exocrine insufficiency after pancreatectomy. Surgery. 2016;159(3):885-892.
Li Y, Li Y. Central versus Distal Pancreatectomy for Benign or Low-Grade Malignant Lesions in the Pancreatic Neck and Proximal Body. Am Surg. 2019;85(11):1239-1245.
Hallac A, Aleassa EM, Rogers M, Falk GA, Morris-Stiff G. Exocrine pancreatic insufficiency in distal pancreatectomy: incidence and risk factors. HPB (Oxford). 2020;22(2):275-281.
Roberts KJ, Bannister CA, Schrem H. Enzyme replacement improves survival among patients with pancreatic cancer: Results of a population based study. Pancreatology. 2019;19(1):114-121.
Kusakabe J, Anderson B, Liu J, et al. Long-Term Endocrine and Exocrine Insufficiency After Pancreatectomy. J Gastrointest Surg. 2019;23(8):1604-1613.
Othman MO, Harb D, Barkin JA. Introduction and practical approach to exocrine pancreatic insufficiency for the practicing clinician. Int J Clin Pract. 2018;72(2).
Borowitz DS, Grand RJ, Durie PR. Use of pancreatic enzyme supplements for patients with cystic fibrosis in the context of fibrosing colonopathy. Consensus Committee. J Pediatr. 1995;127(5):681-684.
Southern WN, Rahmani R, Aroniadis O, et al. Postoperative Clostridium difficile-associated diarrhea. Surgery. 2010;148(1):24-30.
Permissions
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Moore, J.V., Tom, S., Scoggins, C.R. et al. Exocrine Pancreatic Insufficiency After Pancreatectomy for Malignancy: Systematic Review and Optimal Management Recommendations. J Gastrointest Surg 25, 2317–2327 (2021). https://doi.org/10.1007/s11605-020-04883-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-020-04883-1