Abstract
Aim and Background
The aim of this study was to compare the efficacy and safety between endoscopic full-thickness resection (EFR) and laparoscopic or surgical resection methods for gastric gastrointestinal stromal tumor (GIST) in size of 5.0 cm or less. Gastric GISTs are common, and resection is the most effective treatment.
Method
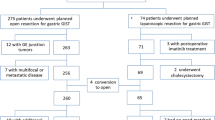
We retrospectively reviewed 216 resections of gastric GISTs in size of up to 5.0 cm at our center from 2009 to 2017.Eligible resection cases were divided into EFR (n = 85), laparoscopic(n = 64), and surgical (n = 67) groups. The clinical records, patient demographic, symptoms, perioperative data, pathological findings, and long-term follow-up outcomes were collected and compared statistically.
Results
No tumor rupture or recurrence occurred in the three groups. The prevalence of complications was significantly lower in EFR (5.9%) than both laparoscopic (7.8%) and surgical group (16.4%) (P < 0.01). In EFR group, the R0 resection rate (95.3%) was significantly lower than in the laparoscopic group and surgical group (100%) (P < 0.001). The hospital cost (OR = 62.79, CI: 12.954–304.363, P < 0.0001) were significantly lower in the EFR than in the laparoscopic group. The hospital cost (OR = 39.032, CI: 8.045–189.371, P < 0.0001) and post-operative diet time (OR = 2.779, CI: 1.225–6.304, P < 0.05) were also significantly lower in the EFR than in the surgical group.
Conclusion
EFR was a feasible treatment for gastric GISTs of size of ≤ 5.0 cm with an acceptable complete resection rate. In addition, EFR had significantly fewer postoperative complications, shorter length of hospital stay, and lower cost.

Similar content being viewed by others
References
Demetri GD, von Mehren M, Antonescu CR, DeMatteo RP, Ganjoo KN, Maki RG, Pisters PW, Raut CP, Riedel RF, Schuetze S, et al: NCCN Task Force report: update on the management of patients with gastrointestinal stromal tumors. J Natl Compr Canc Netw 2010, 8 Suppl 2:S1–41; quiz S42–44.
American Gastroenterological Association I: American Gastroenterological Association Institute medical position statement on the management of gastric subepithelial masses. Gastroenterology 2006, 130:2215–2216.
Miettinen M, Sobin LH, Lasota J: Gastrointestinal stromal tumors of the stomach: a clinicopathologic, immunohistochemical, and molecular genetic study of 1765 cases with long-term follow-up. Am J Surg Pathol 2005, 29:52–68.
Judson I, Bulusu R, Seddon B, Dangoor A, Wong N, Mudan S: UK clinical practice guidelines for the management of gastrointestinal stromal tumours (GIST). Clin Sarcoma Res 2017, 7:6.
Jeong IH, Kim JH, Lee SR, Kim JH, Hwang JC, Shin SJ, Lee KM, Hur H, Han SU: Minimally invasive treatment of gastric gastrointestinal stromal tumors: laparoscopic and endoscopic approach. Surg Laparosc Endosc Percutan Tech 2012, 22:244–250.
von Mehren M: Management of Gastrointestinal Stromal Tumors. Surg Clin North Am 2016, 96:1059–1075.
Wakamatsu K, Lo Menzo E, Szomstein S, Seto Y, Chalikonda S, Rosenthal RJ: Feasibility of Laparoscopic Resection of Gastrointestinal Stromal Tumor of the Stomach. J Laparoendosc Adv Surg Tech A 2018, 28:569–573.
Tan Y, Tan L, Lu J, Huo J, Liu D: Endoscopic resection of gastric gastrointestinal stromal tumors. Transl Gastroenterol Hepatol 2017, 2:115.
Yu C, Liao G, Fan C, Yu J, Nie X, Yang S, Bai J: Long-term outcomes of endoscopic resection of gastric GISTs. Surg Endosc 2017, 31:4799–4804.
Pidhorecky I, Cheney RT, Kraybill WG, Gibbs JF: Gastrointestinal stromal tumors: current diagnosis, biologic behavior, and management. Ann Surg Oncol 2000, 7:705–712.
Goh BK, Chow PK, Kesavan SM, Yap WM, Chung YF, Wong WK: Outcome after curative resection of large (>or=10 cm) gastric gastrointestinal stromal tumors: how frequent is adjacent organ involvement and is concomitant distal pancreatectomy necessary? J Gastrointest Surg 2010, 14:607–613.
Andalib I, Yeoun D, Reddy R, Xie S, Iqbal S: Endoscopic resection of gastric gastrointestinal stromal tumors originating from the muscularis propria layer in North America: methods and feasibility data. Surg Endosc 2018, 32:1787–1792.
Tan Y, Tang X, Guo T, Peng D, Tang Y, Duan T, Wang X, Lv L, Huo J, Liu D: Comparison between submucosal tunneling endoscopic resection and endoscopic full-thickness resection for gastric stromal tumors originating from the muscularis propria layer. Surg Endosc 2017, 31:3376–3382.
Yang F, Wang S, Sun S, Liu X, Ge N, Wang G, Guo J, Liu W, Feng L, Ma W: Factors associated with endoscopic full-thickness resection of gastric submucosal tumors. Surg Endosc 2015, 29:3588–3593.
Meng FS, Zhang ZH, Hong YY, Li DJ, Lin JQ, Chen X, Ji F: Comparison of endoscopic submucosal dissection and surgery for the treatment of gastric submucosal tumors originating from the muscularis propria layer: a single-center study (with video). Surg Endosc 2016, 30:5099–5107.
Joo MK, Park JJ, Kim H, Koh JS, Lee BJ, Chun HJ, Lee SW, Jang YJ, Mok YJ, Bak YT: Endoscopic versus surgical resection of GI stromal tumors in the upper GI tract. Gastrointest Endosc 2016, 83:318–326.
Dai WJ, Liu G, Wang M, Liu WJ, Song W, Yang XZ, Wang QL, Zhang XY, Fan ZN: Endoscopic versus laparoscopic resection of gastric gastrointestinal stromal tumors: a multicenter study. Oncotarget 2017, 8:11259–11267.
Joensuu H: Risk stratification of patients diagnosed with gastrointestinal stromal tumor. Hum Pathol 2008, 39:1411–1419.
Chok AY, Koh YX, Ow MY, Allen JC, Jr., Goh BK: A systematic review and meta-analysis comparing pancreaticoduodenectomy versus limited resection for duodenal gastrointestinal stromal tumors. Ann Surg Oncol 2014, 21:3429–3438.
Cai M, Zhou P, Lourenco LC, Zhang D: Endoscopic Full-thickness Resection (EFTR) for Gastrointestinal Subepithelial Tumors. Gastrointest Endosc Clin N Am 2016, 26:283–295.
Li QL, Yao LQ, Zhou PH, Xu MD, Chen SY, Zhong YS, Zhang YQ, Chen WF, Ma LL, Qin WZ: Submucosal tumors of the esophagogastric junction originating from the muscularis propria layer: a large study of endoscopic submucosal dissection (with video). Gastrointest Endosc 2012, 75:1153–1158.
Zhang Q, Gao LQ, Han ZL, Li XF, Wang LH, Liu SD: Effectiveness and safety of endoscopic resection for gastric GISTs: a systematic review. Minim Invasive Ther Allied Technol 2018, 27:127–137.
Ye LP, Yu Z, Mao XL, Zhu LH, Zhou XB: Endoscopic full-thickness resection with defect closure using clips and an endoloop for gastric subepithelial tumors arising from the muscularis propria. Surg Endosc 2014, 28:1978–1983.
Chan SM, Chiu PW, Teoh AY, Lau JY: Use of the Over-The-Scope Clip for treatment of refractory upper gastrointestinal bleeding: a case series. Endoscopy 2014, 46:428–431.
Feng Y, Yu L, Yang S, Li X, Ding J, Chen L, Xu Y, Shi R: Endolumenal endoscopic full-thickness resection of muscularis propria-originating gastric submucosal tumors. J Laparoendosc Adv Surg Tech A 2014, 24:171–176.
Mori H, Kobara H, Nishiyama N, Fujihara S, Masaki T: Review of Pure Endoscopic Full-Thickness Resection of the Upper Gastrointestinal Tract. Gut Liver 2015, 9:590–600.
Cai JQ, Chen K, Mou YP, Pan Y, Xu XW, Zhou YC, Huang CJ: Laparoscopic versus open wedge resection for gastrointestinal stromal tumors of the stomach: a single-center 8-year retrospective cohort study of 156 patients with long-term follow-up. BMC Surg 2015, 15:58.
Karakousis GC, Singer S, Zheng J, Gonen M, Coit D, DeMatteo RP, Strong VE: Laparoscopic versus open gastric resections for primary gastrointestinal stromal tumors (GISTs): a size-matched comparison. Ann Surg Oncol 2011, 18:1599–1605.
Navarrete A, Momblan D, Fernandez-Esparrach G, Delgado S, Jimenez M, Hessheimer A, Lacy AM: Endoscopic full-thickness resection of esophagogastric junction gastrointestinal stromal tumor assisted by laparoscopy after neoadjuvant therapy. Endoscopy 2016, 48 Suppl 1:E112–114.
Kwon OK, Yu W: Endoscopic and Laparoscopic Full-Thickness Resection of Endophytic Gastric Submucosal Tumors Very Close to the Esophagogastric Junction. J Gastric Cancer 2015, 15:278–285.
Gluzman MI, Kashchenko VA, Karachun AM, Orlova RV, Nakatis IA, Pelipas IV, Vasiukova EL, Rykov IV, Petrova VV, Nepomniashchaia SL, Klimov AS: Technical success and short-term results of surgical treatment of gastrointestinal stromal tumors: an experience of three centers. Transl Gastroenterol Hepatol 2017, 2:56.
Acknowledgments
Thanks to all the authors for their contributions to this article.
Funding
This work was supported by grants from the National Natural Science Foundation of China (Grant Nos. 81572338 and 81201909) and the Nanjing Medical Science and Technology Development Program No. YKK16078. This work was also part of a C-class sponsored research project of the Jiangsu Provincial Six Talent Peaks (WSN-078).
Author information
Authors and Affiliations
Contributions
X. Z. approved the final version. G. X. contributed to the conception of the study. Q. H. revised the study critically for important intellectual content. Y. Z. performed the data analyses and wrote the manuscript. T. P. and B. Z. contributed significantly to analysis and manuscript preparation. L. W., Y. L., T. L., and X. Z. contributed significantly to acquired data.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhao, Y., Pang, T., Zhang, B. et al. Retrospective Comparison of Endoscopic Full-Thickness Versus Laparoscopic or Surgical Resection of Small (≤ 5 cm) Gastric Gastrointestinal Stromal Tumors. J Gastrointest Surg 24, 2714–2721 (2020). https://doi.org/10.1007/s11605-019-04493-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-019-04493-6