Abstract
Background
Post-hepatectomy liver regeneration is of great interest to liver surgeons, and understanding the process of regeneration could contribute to increasing the safety of hepatectomies and improving prognoses.
Methods
Five hundred thirty-eight patients who underwent hepatectomy were retrospectively analyzed. Postoperative outcomes were evaluated, with a focus on the effects of portal vein resection and resected liver volume on remnant liver regeneration in patients with liver tumors. Remnant liver volumes (RLVs) and laboratory data were measured postoperatively using multidetector computed tomography on day 7 and months 1, 2, 5, 12, and 24 after the operation.
Results
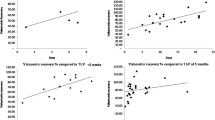
Liver regeneration speed peaked at 1 week postoperatively and gradually decreased. Regeneration with large resections was longer than that with small resections, with the remnant liver regeneration rate being significantly lower in the former at all time points. Remnant liver regeneration plateaued around 5 months postoperatively, when regeneration is almost complete. Up to 1 month postoperatively, laboratory data were significantly worse when more portal veins was resected. After 2 months postoperatively, these data recovered to near normal levels.
Conclusion
The speed and rate of remnant liver regeneration primarily showed a strong correlation with the number of resected portal veins and the amount of removed liver parenchyma. The larger the resection ratio, the longer it took the liver to regenerate. We confirmed that recovery of the liver’s functional aspects accompanies recovery of the RLV.

Similar content being viewed by others
Abbreviations
- RLV:
-
remnant liver volume
- MDCT:
-
multidetector computed tomography
- 3D:
-
three-dimensional
- CT:
-
computed tomography
- BMI:
-
body mass index
- PT:
-
prothrombin time
- ICG-R15:
-
indocyanine green retention rate at 15 min
- TLV:
-
total liver volume
- PHLF:
-
post-hepatectomy liver failure
- OR:
-
odds ratio
- CI:
-
confidence interval
References
Higgins GM, Anderson RM. Experimental pathology of the liver. Restoration of the liver of the white rat following partial surgical removal. Arch Pathol 1931;12:186–202.
Tuczek HV, Rabes H. Verlust der Proliferationsfahigkeit der Hepatozyten nach subtotaler Hepatectomie. Experientia 1971;27:526.
Bégin A, Martel G, Lapointe R, Belblidia A, Lepanto L, Sler L, et al. Accuracy of preoperative automatic measurement of the liver volume by CT-scan combined to a 3D virtual surgical planning software (3DVSP). Surg Endosc 2014;28:3408–3412.
Yamanaka J, Saito S, Fujimoto J. Impact of preoperative planning using virtual segmental volumetry on liver resection for hepatocellular carcinoma. World J Surg 2007;31:1249–1255.
Pugh RN, Murray-Lyon IM, Dawson JL, Pietroni MC, Williams R. Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 1973;60:646–649.
Couinaud C. [Surgical anatomy of the liver. Several new aspects] [Article in French]. Chirurgie 1986;112:337–342.
Makuuchi M, Kosuge T, Takayama T, Yamazaki S, Kakazu T, Miyagawa S, Kawasaki S. Surgery for small liver cancers. Semin Surg Oncol 1993:9:298–304.
Yamada T, Tanaka K, Uryuhara K, Ito K, Takada Y, Uemoto S. Selective hemi-portocaval shunt based on portal vein pressure for small-for-size graft in adult living donor liver transplantation. Am J Transplant 2008;8:847–53.
Inoue Y, Hayashi M, Komeda K, Masubuchi S, Yamamoto M, Yamana H, et al. Resection margin with anatomic or nonanatomic hepatectomy for liver metastasis from colorectal cancer. J Gastrointest Surg 2012;16:1171–1180.
Inoue Y, Imai Y, Fujii K, Hirokawa F, Hayashi M, Uchiyama K. The utility of 5-aminolevulinic acid-mediated photodynamic diagnosis in the detection of intraoperative bile leakage. Am J Surg 2017;213:1077–1082.
Inoue Y, Tanaka R, Komeda K, Hirokawa F, Hayashi M, Uchiyama K. Fluorescence detection of malignant liver tumors using 5-aminolevulinic acid-mediated photodynamic diagnosis: principles, technique, and clinical experience. World J Surg 2014;38:1786–1794.
Strasberg SM. Nomenclature of hepatic anatomy and resection: a review of the Brisbane 2000 system. J Hepatobiliary Pancreat Surg 2005;12:351–355.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 2004;240:205–213.
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, et al. The Clavien–Dindo classification of surgical complications: five-year experience. Ann Surg 2009;250:187–196.
Koch M, Garden J, Padbury R, Rahbari NN, Adam R, Capussotti L, et al. Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the International Study Group of Liver Surgery. Surgery 2011;149:680–688.
Rahbari NN, Garden OJ, Padbury R, Brooke-Smith M, Crawford M, Adam R, et al. Posthepatectomy liver failure: a definition and grading by the International Study Group of Liver Surgery (ISGLS). Surgery 2011;149:713–724.
Arroyo V, Gines P, Gerbes AL, Dudley FJ, Gentilini P, Laffi G, et al. Definition and diagnostic criteria of refractory ascites and hepatorenal syndrome in cirrhosis. International Ascites Club. Hepatology 1996;23:164–176.
Bedossa P, Poynard T. An algorithm for the grading of activity in chronic hepatitis C. The METAVIR Cooperative Study Group Hepatology 1996;24:289–293.
Inoue Y, Suzuki Y, Fujii K, Kawaguchi N, Ishii M, Masubuchi S, et al. Laparoscopic liver resection using the lateral approach from intercostal ports in segments VI, VII, and VIII. J Gastrointest Surg 2017;21:2135–2143.
Inoue Y, Suzuki Y, Ota M, Fujii K, Kawaguchi N, Hirokawa F, et al.Short- and long-term results of laparoscopic parenchyma-sparing hepatectomy for small-sized hepatocellular carcinoma: a comparative study using propensity score matching analysis. Am Surg 2018;84:230–237.
Yamamoto KN, Ishii M, Inoue Y, Hirokawa F, MacArthur BD, Nakamura A, et al. Prediction of postoperative liver regeneration from clinical information using a data-led mathematical model. Sci Rep 2016;6:34214.
Yamanaka N, Okamoto E, Oriyama T, Fujimoto J, Furukawa K, Kawamura E, et al. A prediction scoring system to select the surgical treatment of liver cancer. Further refinement based on 10 years of use. Ann Surg 1994;219:342–346.
Yamamoto M, Takasaki K, Ohtsubo T, Katsuragawa H, Fukuda C, Katagiri S. Effectiveness of systematized hepatectomy with Glisson’s pedicle transection at the hepatic hilus for small nodular hepatocellular carcinoma: retrospective analysis. Surgery 2001;130:443–448.
Hasegawa K, Kokudo N, Imamura H, Matsuyama Y, Aoki T, Minagawa M, et al. Prognostic impact of anatomic resection for hepatocellular carcinoma. Ann Surg 2005;242:252–259.
Morioka D, Tanaka K, Sekido H, Matsuo K, Sugita M, Ueda M, et al. Disruption of the middle hepatic vein is not crucial for liver regeneration of the remnant liver after right hemihepatectomy for hepatic tumors. Ann Surg Oncol 2006;13(12):1560–1568.
Funding
This work was supported by the Mitsui Life Social Welfare Foundation.
Author information
Authors and Affiliations
Contributions
YI conceived the study and design, was involved in patient care, and drafted the manuscript. KF, MI, SK, AT, HH, WO, YT, SM, MY, AA, KK, TS, MA, SF, FH, YN, KH, and KU were involved in the creation of the study concept and design, patient care, and drafting of the manuscript. All authors have read and approved the final version of the manuscript.
Corresponding author
Rights and permissions
About this article
Cite this article
Inoue, Y., Fujii, K., Ishii, M. et al. Volumetric and Functional Regeneration of Remnant Liver after Hepatectomy. J Gastrointest Surg 23, 914–921 (2019). https://doi.org/10.1007/s11605-018-3985-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-3985-5