Abstract
Background
Our goal was to evaluate the relationship between perioperative fluid administration and the development of clinically relevant postoperative pancreatic fistula (CR-POPF) after pancreaticoduodenectomy (PD).
Methods
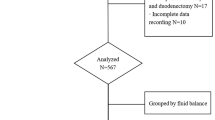
Retrospectively, we analyzed fluid balance over the first 72 h in 104 consecutive patients who underwent PD between 2013 and 2017. Patients were categorized into tertiles (low, medium, and high) by net fluid balance.
Results
POPF was identified in 17.3% of patients (n = 18). No significant demographic differences were identified among tertiles. Similarly, there were no differences in ASA, smoking status, hemoglobin A1C, pathologic findings, operative time, blood loss, intraoperative fluid administration, use of pancreatic stents, use of epidurals, or postoperative lactate. Patients with high 72-h net fluid balance had significantly increased rates of POPF compared with those in the medium and low tertiles (31.4% vs. 11.4% vs. 8.8%, p = 0.02). On multivariate analysis, increasing net fluid balance remained associated with CR-POPF (OR 1.26, CI 1.03–1.55, p = 0.03).
Conclusion
High net 72-h fluid balance is an independent predictor of POPF after PD. Given ongoing efforts to minimize PD morbidity, net fluid balance may represent a clinical predictor and, possibly, a modifiable target for prevention of POPF.

Similar content being viewed by others
References
Bassi C, Marchegiani G, Dervenis C, Sarr M, Abu Hilal M, Adham M et al. The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years After. Surgery. 2017;161(3):584–91. https://doi.org/10.1016/j.surg.2016.11.014.
Machado NO. Pancreatic fistula after pancreatectomy: definitions, risk factors, preventive measures, and management-review. Int J Surg Oncol. 2012;2012:602478. https://doi.org/10.1155/2012/602478.
Smits FJ, van Santvoort HC, Besselink MG, Batenburg MCT, Slooff RAE, Boerma D et al. Management of severe pancreatic fistula after pancreatoduodenectomy. JAMA Surg. 2017;152(6):540–8. https://doi.org/10.1001/jamasurg.2016.5708.
Ahmad SA, Edwards MJ, Sutton JM, Grewal SS, Hanseman DJ, Maithel SK et al. Factors influencing readmission after pancreaticoduodenectomy: a multi-institutional study of 1302 patients. Ann Surg. 2012;256(3):529–37. https://doi.org/10.1097/SLA.0b013e318265ef0b.
Fong ZV, Ferrone CR, Thayer SP, Wargo JA, Sahora K, Seefeld KJ et al. Understanding hospital readmissions after pancreaticoduodenectomy: can we prevent them?: a 10-year contemporary experience with 1,173 patients at the Massachusetts General Hospital.J Gastrointest Surg. 2014;18(1):137–44; discussion 44–5. https://doi.org/10.1007/s11605-013-2336-9.
Enestvedt CK, Diggs BS, Cassera MA, Hammill C, Hansen PD, Wolf RF. Complications nearly double the cost of care after pancreaticoduodenectomy. Am J Surg. 2012;204(3):332–8. https://doi.org/10.1016/j.amjsurg.2011.10.019.
Callery MP, Pratt WB, Kent TS, Chaikof EL, Vollmer CM, Jr. A prospectively validated clinical risk score accurately predicts pancreatic fistula after pancreatoduodenectomy. J Am Coll Surg. 2013;216(1):1–14. https://doi.org/10.1016/j.jamcollsurg.2012.09.002.
Kantor O, Talamonti MS, Pitt HA, Vollmer CM, Riall TS, Hall BL et al. Using the NSQIP pancreatic demonstration project to derive a modified fistula risk score for preoperative risk stratification in patients undergoing pancreaticoduodenectomy. J Am Coll Surg. 2017;224(5):816–25. https://doi.org/10.1016/j.jamcollsurg.2017.01.054.
Yeo CJ, Cameron JL, Maher MM, Sauter PK, Zahurak ML, Talamini MA et al. A prospective randomized trial of pancreaticogastrostomy versus pancreaticojejunostomy after pancreaticoduodenectomy. Ann Surg. 1995;222(4):580–8; discussion 8–92.
Bassi C, Falconi M, Molinari E, Mantovani W, Butturini G, Gumbs AA et al. Duct-to-mucosa versus end-to-side pancreaticojejunostomy reconstruction after pancreaticoduodenectomy: results of a prospective randomized trial. Surgery. 2003;134(5):766–71. https://doi.org/10.1016/S0039.
Bassi C, Falconi M, Molinari E, Salvia R, Butturini G, Sartori N et al. Reconstruction by pancreaticojejunostomy versus pancreaticogastrostomy following pancreatectomy: results of a comparative study. Ann Surg. 2005;242(6):767–71, discussion 71–3.
Keck T, Wellner UF, Bahra M, Klein F, Sick O, Niedergethmann M et al. Pancreatogastrostomy versus pancreatojejunostomy for RECOnstruction After PANCreatoduodenectomy (RECOPANC, DRKS 00000767): perioperative and long-term results of a multicenter randomized controlled trial. Ann Surg. 2016;263(3):440–9. https://doi.org/10.1097/SLA.0000000000001240.
Figueras J, Sabater L, Planellas P, Munoz-Forner E, Lopez-Ben S, Falgueras L et al. Randomized clinical trial of pancreaticogastrostomy versus pancreaticojejunostomy on the rate and severity of pancreatic fistula after pancreaticoduodenectomy. Br J Surg. 2013;100(12):1597–605. https://doi.org/10.1002/bjs.9252.
Berger AC, Howard TJ, Kennedy EP, Sauter PK, Bower-Cherry M, Dutkevitch S et al. Does type of pancreaticojejunostomy after pancreaticoduodenectomy decrease rate of pancreatic fistula? A randomized, prospective, dual-institution trial. J Am Coll Surg. 2009;208(5):738–47; discussion 47–9. https://doi.org/10.1016/j.jamcollsurg.2008.12.031.
Shrikhande SV, Sivasanker M, Vollmer CM, Friess H, Besselink MG, Fingerhut A et al. Pancreatic anastomosis after pancreatoduodenectomy: a position statement by the International Study Group of Pancreatic Surgery (ISGPS). Surgery. 2017;161(5):1221–34. https://doi.org/10.1016/j.surg.2016.11.021.
McMillan MT, Malleo G, Bassi C, Allegrini V, Casetti L, Drebin JA et al. Multicenter, prospective trial of selective drain management for pancreatoduodenectomy using risk stratification. Ann Surg. 2017;265(6):1209–18. https://doi.org/10.1097/SLA.0000000000001832.
Witzigmann H, Diener MK, Kienkotter S, Rossion I, Bruckner T, Barbel W et al. No need for routine drainage after pancreatic head resection: the dual-center, randomized, controlled PANDRA trial (ISRCTN04937707). Ann Surg. 2016;264(3):528–37. https://doi.org/10.1097/SLA.0000000000001859.
Andrianello S, Pea A, Pulvirenti A, Allegrini V, Marchegiani G, Malleo G et al. Pancreaticojejunostomy after pancreaticoduodenectomy: suture material and incidence of post-operative pancreatic fistula. Pancreatology. 2016;16(1):138–41. https://doi.org/10.1016/j.pan.2015.11.004.
Winter JM, Cameron JL, Campbell KA, Chang DC, Riall TS, Schulick RD et al. Does pancreatic duct stenting decrease the rate of pancreatic fistula following pancreaticoduodenectomy? Results of a prospective randomized trial. J Gastrointest Surg. 2006;10(9):1280–90; discussion 90. https://doi.org/10.1016/j.gassur.2006.07.020.
Jang JY, Chang YR, Kim SW, Choi SH, Park SJ, Lee SE et al. Randomized multicentre trial comparing external and internal pancreatic stenting during pancreaticoduodenectomy. Br J Surg. 2016;103(6):668–75. https://doi.org/10.1002/bjs.10160.
Dong Z, Xu J, Wang Z, Petrov MS. Stents for the prevention of pancreatic fistula following pancreaticoduodenectomy. Cochrane Database Syst Rev. 2016(5):CD008914. https://doi.org/10.1002/14651858.CD008914.pub3.
Montorsi M, Zago M, Mosca F, Capussotti L, Zotti E, Ribotta G et al. Efficacy of octreotide in the prevention of pancreatic fistula after elective pancreatic resections: a prospective, controlled, randomized clinical trial. Surgery. 1995;117(1):26–31.
Yeo CJ, Cameron JL, Lillemoe KD, Sauter PK, Coleman J, Sohn TA et al. Does prophylactic octreotide decrease the rates of pancreatic fistula and other complications after pancreaticoduodenectomy? Results of a prospective randomized placebo-controlled trial. Ann Surg. 2000;232(3):419–29.
Allen PJ, Gonen M, Brennan MF, Bucknor AA, Robinson LM, Pappas MM et al. Pasireotide for postoperative pancreatic fistula. N Engl J Med. 2014;370(21):2014–22. https://doi.org/10.1056/NEJMoa1313688.
Shrikhande SV, Barreto SG, Shetty G, Suradkar K, Bodhankar YD, Shah SB et al. Post-operative abdominal drainage following major upper gastrointestinal surgery: single drain versus two drains. J Cancer Res Ther. 2013;9(2):267–71. https://doi.org/10.4103/0973-1482.113380.
Van Buren G, 2nd, Bloomston M, Hughes SJ, Winter J, Behrman SW, Zyromski NJ et al. A randomized prospective multicenter trial of pancreaticoduodenectomy with and without routine intraperitoneal drainage. Ann Surg. 2014;259(4):605–12. https://doi.org/10.1097/SLA.0000000000000460.
Lillemoe KD, Cameron JL, Kim MP, Campbell KA, Sauter PK, Coleman JA et al. Does fibrin glue sealant decrease the rate of pancreatic fistula after pancreaticoduodenectomy? Results of a prospective randomized trial. J Gastrointest Surg. 2004;8(7):766–72; discussion 72–4. https://doi.org/10.1016/j.gassur.2004.06.011.
Eng OS, Melstrom LG, Carpizo DR. The relationship of perioperative fluid administration to outcomes in colorectal and pancreatic surgery: a review of the literature. J Surg Oncol. 2015;111(4):472–7. https://doi.org/10.1002/jso.23857.
Brandstrup B, Tonnesen H, Beier-Holgersen R, Hjortso E, Ording H, Lindorff-Larsen K et al. Effects of intravenous fluid restriction on postoperative complications: comparison of two perioperative fluid regimens: a randomized assessor-blinded multicenter trial. Ann Surg. 2003;238(5):641–8. https://doi.org/10.1097/01.sla.0000094387.50865.23.
Berri RN, Sahai SK, Durand JB, Lin HY, Folloder J, Rozner MA et al. Serum brain naturietic peptide measurements reflect fluid balance after pancreatectomy. J Am Coll Surg. 2012;214(5):778–87. https://doi.org/10.1016/j.jamcollsurg.2012.01.046.
Eng OS, Goswami J, Moore D, Chen C, Gannon CJ, August DA et al. Intraoperative fluid administration is associated with perioperative outcomes in pancreaticoduodenectomy: a single center retrospective analysis. J Surg Oncol. 2013;108(4):242–7. https://doi.org/10.1002/jso.23393.
Boesen AK, Maeda Y, Rorbaek Madsen M. Perioperative fluid infusion and its influence on anastomotic leakage after rectal cancer surgery: implications for prevention strategies. Colorectal Dis. 2013;15(9):e522–7. https://doi.org/10.1111/codi.12321.
Marjanovic G, Villain C, Juettner E, zur Hausen A, Hoeppner J, Hopt UT et al. Impact of different crystalloid volume regimes on intestinal anastomotic stability. Ann Surg. 2009;249(2):181–5. https://doi.org/10.1097/SLA.0b013e31818b73dc.
Kulemann B, Timme S, Seifert G, Holzner PA, Glatz T, Sick O et al. Intraoperative crystalloid overload leads to substantial inflammatory infiltration of intestinal anastomoses—a histomorphological analysis. Surgery. 2013;154(3):596–603. https://doi.org/10.1016/j.surg.2013.04.010.
Melis M, Marcon F, Masi A, Sarpel U, Miller G, Moore H et al. Effect of intra-operative fluid volume on peri-operative outcomes after pancreaticoduodenectomy for pancreatic adenocarcinoma. J Surg Oncol. 2012;105(1):81–4. https://doi.org/10.1002/jso.22048.
Grant FM, Protic M, Gonen M, Allen P, Brennan MF. Intraoperative fluid management and complications following pancreatectomy. J Surg Oncol. 2013;107(5):529–35. https://doi.org/10.1002/jso.23287.
Wang S, Wang X, Dai H, Han J, Li N, Li J. The effect of intraoperative fluid volume administration on pancreatic fistulas after pancreaticoduodenectomy. J Invest Surg. 2014;27(2):88–94. https://doi.org/10.3109/08941939.2013.839766.
Han IW, Kim H, Heo J, Oh MG, Choi YS, Lee SE et al. Excess intraoperative fluid volume administration is associated with pancreatic fistula after pancreaticoduodenectomy: a retrospective multicenter study. Medicine (Baltimore). 2017;96(22):e6893. https://doi.org/10.1097/MD.0000000000006893.
Bruns H, Kortendieck V, Raab HR, Antolovic D. Intraoperative fluid excess is a risk factor for pancreatic fistula after partial pancreaticoduodenectomy. HPB Surg. 2016;2016:1601340. https://doi.org/10.1155/2016/1601340.
Wright GP, Koehler TJ, Davis AT, Chung MH. The drowning whipple: perioperative fluid balance and outcomes following pancreaticoduodenectomy. J Surg Oncol. 2014;110(4):407–11. https://doi.org/10.1002/jso.23662.
Behman R, Hanna S, Coburn N, Law C, Cyr DP, Truong J et al. Impact of fluid resuscitation on major adverse events following pancreaticoduodenectomy. Am J Surg. 2015;210(5):896–903. https://doi.org/10.1016/j.amjsurg.2015.04.020.
Lavu H, Sell NM, Carter TI, Winter JM, Maguire DP, Gratch DM et al. The HYSLAR trial: a prospective randomized controlled trial of the use of a restrictive fluid regimen with 3% hypertonic saline versus lactated Ringers in patients undergoing pancreaticoduodenectomy. Ann Surg. 2014;260(3):445–53; discussion 53–5. https://doi.org/10.1097/SLA.0000000000000872.
Grant F, Brennan MF, Allen PJ, DeMatteo RP, Kingham TP, D'Angelica M et al. Prospective randomized controlled trial of liberal vs restricted perioperative fluid management in patients undergoing pancreatectomy. Ann Surg. 2016;264(4):591–8. https://doi.org/10.1097/SLA.0000000000001846.
Israel JS, Rettammel RJ, Leverson GE, Hanks LR, Cho CS, Winslow ER et al. Does postoperative drain amylase predict pancreatic fistula after pancreatectomy? J Am Coll Surg. 2014;218(5):978–87. https://doi.org/10.1016/j.jamcollsurg.2014.01.048.
Molinari E, Bassi C, Salvia R, Butturini G, Crippa S, Talamini G et al. Amylase value in drains after pancreatic resection as predictive factor of postoperative pancreatic fistula: results of a prospective study in 137 patients. Ann Surg. 2007;246(2):281–7. https://doi.org/10.1097/SLA.0b013e3180caa42f.
Shimizu A, Kawai M, Hirono S, Okada KI, Miyazawa M, Kitahata Y et al. Postoperative visceral tissue edema assessed by computed tomography is a predictor for severe complications after pancreaticoduodenectomy. J Gastrointest Surg. 2018;22(1):77–87. https://doi.org/10.1007/s11605-017-3608-6.
Author information
Authors and Affiliations
Contributions
All persons who meet authorship criteria are listed as authors, and all authors certify that they have participated sufficiently in the work to take public responsibility for the content, including participation in the concept, design, analysis, writing, or revision of the manuscript. Furthermore, each author certifies that this material or similar material has not been and will not be submitted to or published in any other publication before its appearance in the Journal of Gastrointestinal Surgery.
CATEGORY 1
Conception and design of study:
Leah K Winer, Vikrom K Dhar, Syed A Ahmad, Sameer H Patel
Acquisition of data:
Leah K Winer, Tiffany C Lee, Mackenzie C Morris
Analysis and/or interpretation of data:
Leah K Winer, Vikrom K Dhar, Koffi Wima, Shimul A Shah, Syed A Ahmad, Sameer H Patel
CATEGORY 2
Drafting the manuscript:
Leah K Winer, Vikrom K Dhar, Sameer H Patel
Revising the manuscript critically for important intellectual content:
Leah K Winer, Vikrom K Dhar, Koffi Wima, Tiffany C Lee, Mackenzie C Morris, Shimul A Shah, Syed A Ahmad, Sameer H Patel
CATEGORY 3
Final approval of the version of the manuscript to be published:
Leah K Winer, Vikrom K Dhar, Koffi Wima, Tiffany C Lee, Mackenzie C Morris, Shimul A Shah, Syed A Ahmad, Sameer H Patel
CATEGORY 4
Agreement to be accountable for all aspects of the work:
Leah K Winer, Vikrom K Dhar, Koffi Wima, Tiffany C Lee, Mackenzie C Morris, Shimul A Shah, Syed A Ahmad, Sameer H Patel
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that there are no conflicts of interest.
Rights and permissions
About this article
Cite this article
Winer, L.K., Dhar, V.K., Wima, K. et al. Perioperative Net Fluid Balance Predicts Pancreatic Fistula After Pancreaticoduodenectomy. J Gastrointest Surg 22, 1743–1751 (2018). https://doi.org/10.1007/s11605-018-3813-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-3813-y