Abstract
Objective
To describe the rate and characteristics of air bubble retention (ABR) within cerebral aneurysms treated by flow diversion.
Methods
Procedural flat detector CT (FDCT) studies were scrutinized for the presence of air bubbles (density < − 200 HU) in patients treated by flow diversion. Patients with intrasaccular treatment or previous clipping were excluded. Clinical outcomes, procedural angiograms, aneurysm characteristics and imaging features of air within the aneurysm were evaluated.
Results
Bubbles were noted in 17.1% of 105 aneurysms in 85 FDCTs. Aneurysms with ABR were significantly larger (mean diameter: 18.9 versus 7.5 mm, P < 0.0001). There was a trend for the use of multiple devices during the treatment of these aneurysms (72.2% vs 49.4%, P = 0.071). All of the bubbles were located rostrally in the aneurysm sac and were smaller than 6 mm (mean diameter: 2.1 ± 1.3 mm). None of the patients had post-procedural neurological deterioration. The air had spontaneously disappeared on follow-up CT images (available in 12 patients) obtained at a mean follow-up duration of 48 h.
Conclusions
ABR is not infrequent in cerebral flow diversion procedures. It is a clinically silent and self-limited technical complication. We propose air entrapment or filtration through the flow diverter as causative factors.


Similar content being viewed by others
References
Chow M, McDougall C, O'Kelly C, Ashforth R, Johnson E, Fiorella D. Delayed spontaneous rupture of a posterior inferior cerebellar artery aneurysm following treatment with flow diversion: a clinicopathologic study. Am J Neuroradiol. 2012;33(4):E46–51.
De Vries J, Boogaarts J, Van Norden A, Wakhloo AK. New generation of flow diverter (surpass) for unruptured intracranial aneurysms: a prospective single-center study in 37 patients. Stroke. 2013;44(6):1567–77.
Gurkas E, Kaya T, Daglioglu E, Akmangit I, Belen D, Peker A, et al. Silk device for the treatment of intracranial aneurysms. Part 1: peri-procedural results, technical aspects and learning curve. Turk Neurosurg. 2016;26(4):525–32.
Luecking H, Engelhorn T, Lang S, Goelitz P, Kloska S, Roessler K, et al. FRED flow diverter: a study on safety and efficacy in a consecutive group of 50 patients. Am J Neuroradiol. 2017;38(3):596–602.
Zhang Y, Zhou Y, Yang P, Liu J, Xu Y, Hong B, et al. Comparison of the flow diverter and stent-assisted coiling in large and giant aneurysms: safety and efficacy based on a propensity score-matched analysis. Eur Radiol. 2016;26(7):2369–77.
Belton PJ, Nanda A, Alqadri SL, Khakh GS, Chandrasekaran PN, Newey C, et al. Paradoxical cerebral air embolism causing large vessel occlusion treated with endovascular aspiration. J neurointerv Surg. 2017;9(4):e10.
Lee DH, Hwang SM, Lim OK, Kim JK. In vitro observation of air bubbles during delivery of various detachable aneurysm embolization coils. Korean J Radiol. 2012;13(4):412–6.
Fowler MJ Jr, Thomas CE, Koenigsberg RA, Schwartzman RJ, Kantharia BK. Diffuse cerebral air embolism treated with hyperbaric oxygen: a case report. J Neuroimaging. 2005;15(1):92–6.
Ialongo P, Ciarpaglini L, Tinti MD, Suadoni MN, Cardillo G. Systemic air embolism as a complication of percutaneous computed tomography guided transthoracic lung biopsy. Ann R Coll Surg Engl. 2017;99(6):e174–e176176.
Trabanco S, Pardo S, Williams M, Diaz J, Ruiz C. Cerebral air embolism after ERCP. J Clin Anesth. 2017;36:133–5.
Bendszus M, Koltzenburg M, Bartsch AJ, Goldbrunner R, Gunthner-Lengsfeld T, Weilbach FX, et al. Heparin and air filters reduce embolic events caused by intra-arterial cerebral angiography: a prospective, randomized trial. Circulation. 2004;110(15):2210–5.
Hossmann KA. Experimental models for the investigation of brain ischemia. Cardiovasc Res. 1998;39(1):106–20.
Muth CM, Shank ES. Gas embolism. N Engl J Med. 2000;342(7):476–82.
Yang TK. Spontaneous absorption of cerebral air embolus developed accidentally during an intra-arterial procedure. J Cerebrovasc Endovasc Neurosurg. 2016;18(4):391–5.
Mamourian AC, Weglarz M, Dunn J, Cromwell LD, Saykin AJ. Injection of air bubbles during flushing of angiocatheters: an in vitro trial of conventional hardware and techniques. Am J Neuroradiol. 2001;22(4):709–12.
Kulcsar Z, Augsburger L, Reymond P, Pereira VM, Hirsch S, Mallik AS, et al. Flow diversion treatment: intra-aneurismal blood flow velocity and WSS reduction are parameters to predict aneurysm thrombosis. Acta Neurochir. 2012;154(10):1827–34.
Struffert T, Saake M, Ott S, Engelhorn T, Golitz P, Kloska S, et al. Intravenous flat detector CT angiography for non-invasive visualisation of intracranial flow diverter: technical feasibility. Eur Radiol. 2011;21(8):1797–801.
Struffert T, Richter G, Engelhorn T, Doelken M, Goelitz P, Kalender WA, et al. Visualisation of intracerebral haemorrhage with flat-detector CT compared to multislice CT: results in 44 cases. Eur Radiol. 2009;19(3):619–25.
Zwarzany L, Poncyljusz W, Burke TH. Flat detector CT and its applications in the endovascular treatment of wide-necked intracranial aneurysms—a literature review. Eur J Radiol. 2017;88:26–31.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This retrospective study was approved by the ethics committee of our university hospital.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Figure 1
(a-p) FDCT images of all of the cases with intraaneurysmal air in this series in a variety of oblique planes showing both the air and the adjacent flow diverter. (PDF 624 kb)
Figure 2
Basic flow model constructed to simulate air displacement during flow diverter deployment. Arrows indicate the straight arm of the Y-connector which serves as the parent artery, the side arm simulates a small aneurysm (arrow head). Pulsatility of the flow was maintained by turning the roller clamp of the fluid line “on and off” in constant cycles. The fluid line was connected with a drip chamber to a saline bag pressurized at 300 mmHg and air was introduced during cycles by puncturing the yellow rubber connectors with a 26 G hypodermic needle. The fluid in the efferent limb of the line was let to flow freely in an empty fluid bag (PDF 281 kb)
Video 1
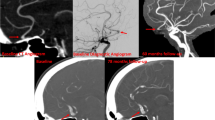
Left ICA arteriogram in working projection just before flow diverter deployment shows the air bubble generated during catheterization (the same patient as in Fig. 2) (MOV 512 kb)
Video 2
a Biplane left ICA arteriogram in working projection obtained during the deployment of the flow diverter is suggestive of filtration of air and its coalescence to form a bubble that migrates to rostral portion of the aneurysm (the same patient as in Fig. 1) (MOV 640 kb)
b
Biplane left ICA arteriogram in working projection obtained during the deployment of the flow diverter is suggestive of filtration of air and its coalescence to form a bubble that migrates to rostral portion of the aneurysm (the same patient as in Fig. 1) (MOV 624 kb)
Video 3
Despite rigorous flushing of the flow diverter before insertion into guiding catheter, air bubbles are entrapped between struts of the device (MP4 10234 kb)
Video 4
During the on/off cycles, air was introduced within the 3 mm Surpass flow diverter with a long needle from the efferent limb to observe how it behaved, then 0.01 mL of air was injected from the afferent limb. Please note that the air within the lumen of the device tends to stay inside the flow diverter throughout the cycles whereas the air bubble at the edge of the “funnel” of flow diverter formed as the device exits the delivery catheter, remains entrapped at the interstices of the diverter without entering the lumen of the flow diverter. With the injection of 0.1 mL of air via the afferent limb, this air bubble and the incoming air bubble both fragment and filter into the side-arm of the connector where some of the smaller bubbles are seen to coalesce (MP4 12169 kb)
About this article
Cite this article
Ocal, O., Arat, A. Intra-aneurysmal air after flow diversion treatment in intracranial aneurysms: incidence, characteristics and clinical significance. Jpn J Radiol 37, 549–554 (2019). https://doi.org/10.1007/s11604-019-00842-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11604-019-00842-2