Abstract
Objective
Nonalcoholic fatty liver disease (NAFLD) is a common cause of clinical liver dysfunction and an important prepathological change of liver cirrhosis. Central obesity, type 2 diabetes mellitus, dyslipidemia, and metabolic syndrome are the major risk factors for NAFLD. Sitagliptin (Sig) is a novel hypoglycemic agent that improves blood glucose levels by increasing the level of active incretin. Sig has been shown to prevent the development of fatty livers in mice on a fructose-rich diet. The purpose of this study was to observe the efficacy of Sig on NAFLD in type 2 diabetic mice.
Methods
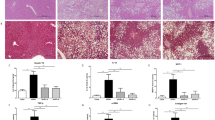
The diet-induced obesity mouse model was established, and the diabetic mice were screened by an intraperitoneal glucose tolerance trial. The mice were randomly divided into four groups for 8 weeks of intervention: high-fat diet (HFD) group, Sig group, metformin (Met) group, and Sig+Met group. After the intervention, the liver function indexes as well as the blood glucose and blood lipid levels of the mice were measured. In addition, the wet weight of the liver was measured; the pathological sections of the liver tissues were stained to observe the hepatocyte fatty degeneration, inflammation, necrosis, and fibrosis; and the hepatic histological injury was recorded as the NAFLD activity score (NAS).
Results
Compared with the normal control group, the body weight, liver weight, blood glucose level, insulin resistance (IR), blood lipid level, and transaminase level of the mice in the HFD group were significantly increased, showing typical metabolic syndrome. After treatment with Sig and/or Met, the mice gained less weight, had lower levels of blood glucose, triglyceride (TG), low-density lipoprotein cholesterol (LDL-C), and transaminase, and had improved IR compared with the HFD group. The liver pathological NASs in the Sig group (P=0.01), Met group (P=0.028), and Sig+Met group (P<0.001) were lower than those in the HFD group (P<0.05), suggesting that the use of the two drugs alone or in combination can improve the state of liver inflammation. In terms of fibrosis, there was no fibrosis in the control group but there was significant fibrosis in the HFD group (P<0.001). There was no significant difference between the drug intervention groups and the HFD group, indicating that the drug therapy (Sig and/or Met) did not significantly improve the pre-existing fibrosis.
Conclusion
Our experiment proved that Sig can improve NAFLD, including improvement of the serum transaminase level, hepatic pathological inflammation level, and hepatocyte adiposis, suggesting that Sig may play a role by improving glucose and lipid metabolism, reducing the body weight and liver weight, improving insulin sensitivity, and inhibiting fatty liver inflammation. Sig may be a new direction for the treatment of patients with a nonalcoholic fatty liver and diabetes, delaying the progression of NAFLD.
Similar content being viewed by others
References
Stein LL, Dong MH, Loomba R. Insulin sensitizers in nonalcoholic fatty liver disease and steatohepatitis: Current status. Adv Ther, 2009,26(10):893–907
Dietrich P, Hellerbrand C. Non-alcoholic fatty liver disease, obesity and the metabolic syndrome. Best Pract Res Clin Gastroenterol, 2014,28(4):637–653
Smits MM, Ioannou GN, Boyko EJ, et al. Non-alcoholic fatty liver disease as an independent manifestation of the metabolic syndrome: results of a US national survey in three ethnic groups. J Gastroenterol Hepatol, 2013,28(4):664–670
Santoro N, Caprio S. Nonalcoholic fatty liver disease/nonalcoholic steatohepatitis in obese adolescents: a looming marker of cardiac dysfunction. Hepatology, 2014,59(2):372–374
Staels B, Rubenstrunk A, Noel B, et al. Hepatoprotective effects of the dual peroxisome proliferator-activated receptor alpha/delta agonist, GFT505, in rodent models of nonalcoholic fatty liver disease/nonalcoholic steatohepatitis. Hepatology, 2013,58(6):1941–1952
Ahrén B, Landin-Olsson M, Jansson P-A, et al. Inhibition of dipeptidyl peptidase-4 reduces glycemia, sustains insulin levels, and reduces glucagon levels in type 2 diabetes. J Clin Endocrinol Metab, 2004,89(5):2078–2084
Balaban YH, Korkusuz P, Simsek H, et al. Dipeptidyl peptidase IV (DDP IV) in NASH patients. Ann Hepatol, 2007,6(4):242–250
Maiztegui B, Borelli MI, Madrid VG, et al. Sitagliptin prevents the development of metabolic and hormonal disturbances, increased β-cell apoptosis and liver steatosis induced by a fructose-rich diet in normal rats. Clin Sci (Lond), 2011,120(2):73–80
Ohara M, Maesawa C, Takebe N, et al. Different susceptibility to insulin resistance and fatty liver depending on the combination of TNF-α C-857T and adiponectin G+276T gene polymorphisms in Japanese subjects with type 2 diabetes. Tohoku J Exp Med, 2012,226(2):161–169
Kleiner DE, Brunt EM, Van Natta M, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology, 2005,41(6): 1313–1321
Senateş, E, Colak Y, Yeşil A, et al. Circulating resistin is elevated in patients with non-alcoholic fatty liver disease and is associated with steatosis, portal inflammation, insulin resistance and nonalcoholic steatohepatitis scores. Minerva Med, 2012,103(5):369–376
Gruben N, Shiri-Sverdlov R, Koonen DPY, et al. Nonalcoholic fatty liver disease: A main driver of insulin resistance or a dangerous liaison? Biochim Biophys Acta, 2014,1842(11):2329–2343
Olson AL. Insulin resistance: cross-talk between adipose tissue and skeletal muscle, through free fatty acids, liver X receptor, and peroxisome proliferator-activated receptor-α signaling. Horm Mol Biol Clin Investig, 2013,15(3):115–121
Manne V, Handa P, Kowdley KV. Pathophysiology of Nonalcoholic Fatty Liver Disease/Nonalcoholic Steatohepatitis. Clin Liver Dis, 2018,22(1):23–37
Rabasseda X. Sitagliptin in the treatment of type 2 diabetes: new data presented during the American Diabetes Association annual meeting (San Diego, California, June 2011). Drugs of today (Barcelona, Spain: 1998), 2011,47 Suppl D:1–8
Mu J, Woods J, Zhou YP, et al. Chronic inhibition of dipeptidyl peptidase-4 with a sitagliptin analog preserves pancreatic beta-cell mass and function in a rodent model of type 2 diabetes. Diabetes, 2006,55(6):1695–1704
Yan J, Yao B, Kuang H, et al. Liraglutide, Sitagliptin, and Insulin Glargine Added to Metformin: The Effect on Body Weight and Intrahepatic Lipid in Patients With Type 2 Diabetes Mellitus and Nonalcoholic Fatty Liver Disease. Hepatology, 2019,69(6):2414–2426
Shirakawa J, Fujii H, Ohnuma K, et al. Diet-induced adipose tissue inflammation and liver steatosis are prevented by DPP-4 inhibition in diabetic mice. Diabetes, 2011,60(4):1246–1257
Itou M, Kawaguchi T, Taniguchi E, et al. Dipeptidyl Peptidase IV Inhibitor Improves Insulin Resistance and Steatosis in a Refractory Nonalcoholic Fatty Liver Disease Patient: A Case Report. Case Rep Gastroenterol, 2012,6(2):538–544
Iwasaki T, Yoneda M, Inamori M, et al. Sitagliptin as a novel treatment agent for non-alcoholic Fatty liver disease patients with type 2 diabetes mellitus. Hepato-Gastroenterology, 2011,58(112):2103–2105
Rizzo MR, Barbieri M, Marfella R, et al. Reduction of oxidative stress and inflammation by blunting daily acute glucose fluctuations in patients with type 2 diabetes: role of dipeptidyl peptidase-IV inhibition. Diabetes Care, 2012,35(10):2076–2082
Allam MM, Ibrahim RM, El Gazzar WB, et al. Dipeptedyl peptidase-4 (DPP-4) inhibitor downregulates HMGB1/TLR4/NF-κB signaling pathway in a diabetic rat model of non-alcoholic fatty liver disease. Arch Physiol Biochem, 2021:1–9
Rhee EJ, Lee WY, Min KW, et al. Efficacy and safety of the dipeptidyl peptidase-4 inhibitor gemigliptin compared with sitagliptin added to ongoing metformin therapy in patients with type 2 diabetes inadequately controlled with metformin alone. Diabetes Obes Metab, 2013,15(6):523–530
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflict of Interest Statement
The authors declare that they have no conflicts of interest.
This project was supported by Research Foundation of Beijing Friendship Hospital (No. yyqdkt2018-8).
Rights and permissions
About this article
Cite this article
Zhou, St., Cui, W., Kong, L. et al. Efficacy of Sitagliptin on Nonalcoholic Fatty Liver Disease in High-fat-diet-fed Diabetic Mice. CURR MED SCI 42, 513–519 (2022). https://doi.org/10.1007/s11596-022-2573-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2573-9