Abstract
Due the limitations of the previous validations, the purpose of this study was to further validate the Prescription Opioid Misuse Index (POMI) in a larger sample of chronic non-cancer pain (CNCP) patients and to examine differential item functioning (DIF) across sex. Participants (n=225 CNCP patients under long-term opioid therapy) completed patient characteristics, self-reported POMI and DSM-5 prescription opioid use disorder measurements. Reliability and factor structure were assessed using both item response theory and classical test theory. ROC curve analysis was used to establish the optimum cut-off score for detecting the presence of DSM-5 prescription opioid-use disorder. Concurrent validity was also tested. The POMI showed a unidimensional factor structure and acceptable internal consistency (ωcat =0.62). DIF analysis showed that males and females respond similarly to each item of the POMI, supporting unbiased measurement of the latent trait across both groups. A cut-off point of 2 is suggested in order to maximize the accuracy of the instrument as a first-screening tool for opioid misuse (AUC=0.78; p<0.001; CI 95%: 0.72–0.85). Concurrent validity of the POMI was high with DSM-5 moderate to severe opioid-use disorder criteria (OR=7.824, p<0.001). These results indicate that the POMI is a valid and clinically feasible screening instrument for detecting CNCP patients who misuse opioid medications. The short length of the scale could meet the needs of clinical practice as it allows clinicians to precisely identify and monitor prescription opioid misuse in both male and female patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The use of prescription opioids for chronic pain treatment has increased worldwide (Helmerhorst et al., 2017; Kalkman et al., 2022). However, long-term use of these analgesics is considered a risk factor for prescription opioid abuse, increased risk of overdose, and other harms (Gallagher & Galvin, 2018; Volkow & McLellan, 2016). The importance of the risk assessment instruments in the prediction and prevention of prescription opioid use disorders has been pointed out by several authors (Ballantyne, 2017; Carballo et al., 2016; Lawrence et al., 2017). Opioid misuse prevalence is estimated between 21 and 29% in chronic pain population (Vowles et al., 2015), although data varies widely due to the heterogeneity of definitions and methodologies used to assess misuse in previous studies (Voon et al., 2017). Unfortunately, there are few adaptations of instruments for predicting opioid misuse in chronic pain population and the evidence of the accuracy of the adapted instruments is scarce (Smith et al., 2015; Voon et al., 2017).
The Prescription Opioid Misuse Index (POMI; Knisely et al., 2008) is one of the most used instruments to assess problematic prescription opioid use (Lawrence et al., 2017; Smith et al., 2017). It is a brief questionnaire made up of 6 binary items (yes/no), which identifies patients who use opioid medication inappropriately (score≥2). The initial validation of the instrument was made in a mixed sample of chronic pain patients (n=34) and opioid abusers (n=40) and the results showed good internal consistency (Cronbach’s alpha of 0.85). However, the small and homogeneous sample of chronic pain patients limited the generalization of the findings. For this reason, two recently validation studies have further tested the psychometric properties of the POMI in different samples of chronic pain patients (Delage et al., 2022; Laporte et al., 2022). The scale seems to perform better when used in pain clinics (Delage et al., 2022) rather than in general practice settings (Laporte et al., 2022). The authors also propose a shorter version of the POMI (POMI-5F; Delage et al., 2022), which also shows acceptable psychometric properties (Cronbach’s alpha of 0.71) and good external validity with the DSM-5 prescription opioid use disorder (POUD) criteria (r = 0.45; p < 0.001). Although both validations were conducted in a larger sample of chronic pain patients, there are still substantial gaps in the assessment of the diagnostic efficacy of the POMI. First, there are no studies investigating its measurement invariance. Since males are significantly more likely to report prescription opioid misuse (Silver & Hur, 2020), sex invariance should be tested for reliably interpreting differences between male and female patients. Second, both validations relied in classical test theory (CTT) approach. This implies that items of the POMI were analyzed using reliability parameters that are test- and sample-dependent. Modern methods, such as item response theory (IRT), estimate item parameters that are sample invariant and provide a richer description of the scale performance, at both item and test level (Hambleton et al., 1991). Moreover, the IRT approach is useful to estimate how precision of each item may vary across different levels of the construct (i.e., severity of the prescription opioid misuse).
To overcome these limitations, the aims of this study were (a) to further validate the POMI on a larger sample of chronic pain patients using both IRT and CTT approaches, and (b) to examine differential item functioning (DIF) across sex.
Methods
Participants
For this prospective study, participants were recruited from the Pain Care Unit (PCU) of the General University Hospital of Elche. All participants were diagnosed with chronic non-cancer pain and were currently under opioid treatment. Inclusion criteria were as follows: (1) being older than 18 years, (2) having been diagnosed with chronic non-cancer pain, and (3) being at least 3 months under opioid therapy for pain, which has been defined as long-term opioid treatment (Chou et al., 2015; Dowell et al., 2016). The exclusion criteria were (1) presenting mental severe pathologies (e.g., psychosis or dementia), (2) having a diagnosis of cancer, or (3) not being able to be correctly evaluated (e.g., due to advanced age or not accepting undergoing the complete assessment).
Although there are no general guidelines on the optimal sample size for IRT analyses, a minimum sample size of 200 was considered sufficient for estimating stable IRT model parameters (Edelen & Reeve, 2007; Morizot et al., 2007). A total of 267 chronic non-cancer pain patients were recruited for the study, of which 256 met the inclusion criteria. Thirty one questionnaires were discarded because they were not properly filled by the participants; thus, the final sample was made up with 225 patients.
Instruments
Patient and clinical characteristics were assessed (age, sex, type, and dosage in milligrams of opioids consumed and time in treatment with prescription opioids). Each opioid dose prescribed was converted to parenteral morphine equivalent dose (MED), using the American Pain Society guidelines (American Pain Society, 2016). If multiple opioids were used, the total MED per day was calculated by adding the morphine-equivalents doses of each opioid prescribed. Pain intensity and interference were assessed with the Spanish version of the Brief Pain Inventory (BPI; Badia et al., 2003), which has shown good psychometric properties (Cronbach’s alpha values between 0.87 and 0.89 in both subscales). Higher scores on the BPI reflect higher levels of pain intensity (score range: 0–40) and interference (score range: 0 to 70).
The 6 items of the POMI (Knisely et al., 2008) were used to assess prescription opioid misuse. The instrument was self-administered under the supervision of a trained psychologist. The POMI questionnaire was translated into Spanish following the International Test Commission guidelines (Muñiz et al., 2013). Two native Spanish speakers, working independently, translated the original version of the POMI into Spanish. The Spanish version was then translated back into English, without finding discrepancies between both versions of the scale (see Appendix A for the Spanish version of the POMI).
DSM-5 criteria for prescription opioid-use disorder (American Psychiatric Association, 2013) were assessed using the opioid dependence symptoms of the DSM-IV-TR checklist (excluding tolerance and withdrawal) and all the abuse symptoms of the DSM-IV-TR checklist, except legal problems. The craving criterion was assessed with the 5-item Craving Scale of Weiss (1995), which has been widely used for assessing craving of prescription opioid (M. Martel et al., 2014; M. O. Martel et al., 2016; McHugh et al., 2013; Wasan et al., 2012). A score equal to or greater than 1 was considered an indicative of the presence of craving. Finally, based on the number of criteria met, severity of the disorder was classified as mild (2–3 symptoms), moderate (4–5 symptoms), and severe (6 or more symptoms).
Procedure
Recruitment and assessment of the participants was conducted in the PCU, during regular consultation hours. Informed consent was obtained from all individuals included in the study. No participant was paid for taking part in it. Data were collected from September 2014 to January 2019 from all patients who came to the PCU. The instruments were individually applied in a single face-to-face session conducted by trained psychologists. To maintain confidentiality and anonymity of the data, identity information about patients was not included in the database. The study procedures were in accordance with the ethical standards of the Declaration of Helsinki and were approved by the Committee of Research and Ethics of the University Miguel Hernández de Elche and of the hospital.
Data Analysis
The psychometric properties and clinical utility of the POMI were assessed using CTT and IRT approaches. Data analyses were carried out with SPSS v.26 and the lavaan, mirt, ltm, eRm, difR, and pRoc packages of the R statistical software.
Item Scale Reliability
Descriptive analyses were performed for each one of the POMI items. McDonald’s categorical omega (ωcat) was calculated to determine the internal consistency of the scale. Values greater than or equal to 0.70 were considered acceptable (Nunnally & Bernstein, 1994). Item-total correlation corrected for item overlap and item-total correlation coefficients were computed. Item discrimination indices were classified as excellent (≥0.40), good (0.30–0.39), acceptable (0.20–0.29), and poor (<0.20) (Ebel & Frisbie, 1991). From the IRT approach, one- (Rasch) and two-parameter (2PL) logistic models for dichotomous item responses were also fitted to the data set. Discrimination (a) and difficulty (b) parameters were estimated for each item of the POMI. Discrimination parameters (with values ranging from 0 to 3) indicate how much each item can differentiate between patients with different levels of the latent trait (i.e., prescription opioid misuse). The a values are interpreted as very low (a<0.34), low (a=0.35–0.64), moderate (a=0.65–1.34), high (a=1.35–1.69), and very high (a≥1.70) discrimination (Kim & Baker, 2018). Difficulty or severity parameters (values approximately range from −3 to 3) indicate the severity level of the latent trait where the probability of endorsing the item (responding “yes”) is 50%. Larger positive difficulty values demonstrate that higher values of the latent trait (i.e., higher severity of prescription opioid misuse) are necessary to endorse the item.
In the Rasch model, the discrimination parameters are constrained to be equal for all items (a set to 1) and only difficulty varies between items. The 2PL is an extension of the Rasch model that allows discrimination parameters to differ per item. The likelihood-ratio test was used to compare the performance of both nested models. A significant result (p<0.05) indicates that the assumption of the parsimonious model (Rasch) does not hold, and the more complex model (2PL) fits the data better. Test information function, which sums the information (precision) of all items of the scale, was also calculated to examine the overall accuracy of the POMI along the latent trait continuum.
Differential Item Functioning (DIF)
Item invariance was tested to estimate whether males and females respond differently to each item of the POMI, after controlling for the latent trait level. Zumbo-Thomas (ZT) adjusted with Benjamini–Hochberg correction for multiple comparisons and Mantel–Haenszel (MH) χ2 tests were used to analyze DIF. Items were only considered sex biased if the ZT and MH statistics were statistically significant (p<0.05). DIF magnitude was also calculated using ZT change in R2 (ΔR2) and MH delta difference (ΔMH). Both effect sizes were classified using the ETS criteria (Dorans & Holland, 1992), which designated items as A (nonsignificant or negligible DIF), B (moderate DIF), or C (large DIF).
Confirmatory Factor Analysis
The items were subjected to confirmatory factor analysis (CFA), in order to assess if the POMI measures a unidimensional construct as intended. CFA analysis was conducted applying the diagonally weighted least squares (DWLS), as DWLS estimator is suitable for dichotomous indicators. A good model fit was considered based on the following thresholds: Comparative Fit Index (CFI) and Tucker–Lewis index (TLI) values ≥0.96, and root mean square error of approximation (RMSEA) values ≤0.05 (Yu, 2002). The χ2 statistic and degrees of freedom (df) were also reported. Unidimensionality hypothesis was tested in the IRT model using the modified parallel analysis, with a significant result (p<0.05) indicating that the scale is not measuring a single trait.
Diagnostic Efficiency and Concurrent Validity
Receiver operating characteristic (ROC) curve analysis was used to establish the optimum cut-off score for detecting the presence of prescription opioid-use disorder (DSM-5 criteria). Two ROC curves were estimated, considering participants who met ≥2 criteria (mild to severe POUD) and those who met only ≥4 criteria (moderate to severe POUD) as the reference group. Delong’s test was used to test differences between the areas under both ROC curves. The Youden’s Index (sensitivity + specificity – 1) (Youden, 1950), and positive (PPV) and negative predictive values (NPV) were computed to determine the optimal cut-off point of the POMI. Binary logistic regressions were also performed to determine the concurrent validity of the scale. All analyses were performed at a confidence level of 95%.
Results
Participant Characteristics
Participant characteristics by sex are presented in Table 1. Mean age of the total sample was 56.52±13.19 years and 67.1% (n=151) were female. Average time in treatment with opioid medication was 27.40±30.54 months and the average morphine-equivalent dose was 37.92±48.92 milligrams per day. Mean pain intensity and interference scores were 24.19±6.66 and 43.86±15.01, respectively. No significant differences were found between males and females in demographic, clinical, or treatment characteristics (p>0.05).
Of the participants, 28% (n=63) met criteria for moderate to severe DSM-5 prescription opioid-use disorder (≥4 symptoms). In addition, 36% (n=81) of the patients were classified as misusers using the original cut-off point of 2. Again, no significant differences were detected between both sexes (p>0.05).
Reliability and DIF by Sex
Categorical Mcdonald’s omega (ωcat) coefficient was 0.62 (CI 95%: 0.54–0.69), indicating a moderate but acceptable level of internal consistency. Table 2 shows the results of the reliability analyses using both CTT and IRT approaches.
CTT discrimination indices showed that all items were within the good and excellent range (ITC=0.33–0.64), except for item 3 (“Do you ever need early refills for your pain medication?”) that had the lowest corrected item-total correlation (ITC=0.25).
Rasch and 2PL logistic IRT models were also fit to the POMI scale (see models’ fit in footnote of Table 2). The 2PL model showed a significant improved fit over the Rasch model (likelihood-ratio testdf=5= 29.66, p<0.001), indicating that the POMI items exhibit varying levels of discrimination power. The 2PL discrimination parameters also identified the “early refill” item as weak (a=0.56), whereas the rest of the items showed moderate to very high discrimination power (a=0.97–3.61).
No items were flagged for DIF by sex using both Mantel–Haenszel and Zumbo–Thomas procedures (Table 3). These results indicate that female and male patients at the same level of prescription opioid misuse exhibit similar probability of endorsing each item of the scale.
According to the test information function, the optimal accuracy of the POMI was around theta values ranging 0.5 and 1.5. When the latent trait values are exceeded or below this range, the information function declines (see Fig. 1). This suggests that the POMI provides greater precision for patients whose misuse levels are around or moderately above the mean of the latent trait (theta Θ value=0), which was 1.27±1.34.
Confirmatory Factor Analyses
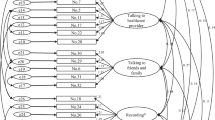
A CFA analysis was carried out on the set of the 6 items, in order to assess if the POMI measures an unidimensional construct. The results indicated that the one-factor model provided an excellent fit (χ2(df)DWLS=10.345(9), p=0.323; RMSEA=0.026, CFI=0.994, TLI=0.991), supporting the unidimensional structure of the questionnaire and the use of a single total score. Using the IRT approach, the modified parallel analysis also confirmed that the POMI measures a single trait (second eigenvalues averaged across 100 Monte Carlo samples=0.823, p=0.347).
Diagnostic Efficiency and Concurrent Validity
ROC analysis yielded an area under the curve (AUC) of 0.72 (p<0.001; CI 95%: 0.65–0.78) for the DSM-5 POUD criteria, when including mild to severe symptoms. Regarding predicting only DSM-5 moderate to severe POUD, ROC analysis generated similar results (AUC=0.78; p<0.001; CI 95%: 0.72–0.85). There was no significant improvement in the overall screening accuracy of the POMI when comparing both AUC (Delong’s test after 10,000 bootstrapping iterations: D=−1.44, p=0.149).
As shown in Table 4, the cut-off score proposed in the original validation (≥2) was the one with the highest combination of sensitivity and specificity for diagnosing opioid use disorder, notwithstanding the classification used (DSM-5 mild to severe or DMS-5 moderated to severe). Figure 2 shows the diagnostic concordance between the POMI and the reference standard DSM-5.
Finally, the results of logistic regressions showed odds ratios of 3.804 (CI 95%:2.377–6.089, p<0.001) for DSM-5 mild to severe POUD symptoms and 7.824 (CI 95%:4.079–15.004, p<0.001) for moderate to severe symptoms, supporting the concurrent validity of the POMI (score ≥2) with the DSM-5 criteria.
Discussion
Due to the methodological limitations of the previous validations of the POMI, the aims of this study were to further validate the instrument on a larger sample of chronic pain patients using both IRT and CTT approaches, and to test differential item functioning (DIF) across sex.
The results obtained show that the POMI is a valid and reliable single-factor instrument for use in the assessment of prescription opioid misuse. Considering the length of the instrument, the POMI demonstrated good internal consistency (ωcat =0.62) and high concurrent validity with DSM-5 opioid-use disorder criteria.
Around 39% of the participants responded “yes” to the item assessing the need of early refills of pain medication, which showed a poor discrimination index. This result coincides with previous findings where early refill was present in the same percentage in chronic pain patients with and without prescription drug use disorder (Meltzer et al., 2012) and it is not considered a direct measure of misuse (Lasser et al., 2016). However, because early refills could increase the risk of prescription opioid misuse (Khalid et al., 2015; Lange et al., 2015), this item was not removed from the instrument. Since risk of prescription opioid misuse is associated with sex, we also tested measurement invariance of the POMI between male and female patients. The DIF effects found indicate that none of the six items of the scale are biased for sex and, therefore, all of them represent the latent structure of prescription opioid misuse equally in males and females. In terms of research implications, these findings provide evidence that the POMI can be used to ensure valid comparisons between both sexes. Moreover, the scale could be used in clinical settings as it seems to provide a precise description of opioid misuse behaviors in both groups of chronic pain patients. In this sense, the POMI could meet the needs of daily clinical practice since it allows clinicians to monitor opioid use with a self-reported measure that can be applied indistinctly in male and female patients.
Concerning the diagnostic efficiency of the POMI, a cut-off point of 2 seems to maximize the accuracy of the instrument as a screening tool. When using this score, the POMI seems to perform well for detecting DSM-5 POUD, regardless the severity of the disorder. Nonetheless, the POMI showed greater NPV values (86.8%) when screening moderate to severe POUD. Higher NPV values are strongly recommended when assessing conditions that can benefit from an early identification and treatment (Trevethan, 2017), such as prescription opioid misuse (Ballantyne, 2017; Carballo et al., 2016; Dowell et al., 2016). Thus, the POMI seems to be more suitable for detecting higher levels of POUD severity, and less precise when including mild severity levels.
Because of its characteristics (short-length and dichotomous answers), the POMI becomes a useful and clinically feasible first-step screening tool. In this sense, when a positive result is obtained, clinicians can subject the patient to a deeper assessment, in order to correctly identify the true positives (Lalkhen & McCluskey, 2008). Moreover, the scale appears to maintain its psychometric properties when used in different populations, which means that can be used with both English and Spanish-speaking chronic pain patients.
To our knowledge, this is the first validation of the POMI done using IRT approach. The use of a bigger sample of chronic pain population is also a strength of this study. Moreover, the study was performed in a real-life scenario for chronic pain patients under opioid therapy, which also helps to demonstrate the usefulness of the scale in daily clinical practice. However, there are some limitations that should be noted. First, the predictive validity of the POMI could not be assessed. Second, the representativeness of the sample could be improved by using a random selection method. Nevertheless, the estimated prevalence of opioid-use disorder found in our study was nearer to other reviews (Boscarino et al., 2015) than the one observed in the previous validations.
The findings of this study could be important to the field of long-term opioid therapy for chronic pain, where there is yet a lack of scientific evidence on risk assessment instruments. Further studies are needed to assess the effectiveness of its use in the reduction of misuse prescription opioids during long-term therapy.
References
American Pain Society. (2016). Principles of analgesic use ((7a ed.). ed.). American Pain Society.
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders ((5a ed.). ed.). American Psychiatric Association.
Badia, X., Muriel, C., Gracia, A., Núñez-Olarte, J. M., Perulero, N., Gálvez, R., Carulla, J., & Cleeland, C. S. (2003). Validation of the Spanish version of the Brief Pain Inventory in patients with oncological pain. Medicina clinica, 120(2), 52–59.
Ballantyne, J. C. (2017). Opioids for the treatment of chronic pain: Mistakes made, lessons learned, and future directions. Anesthesia and Analgesia, 125(5), 1769–1778. https://doi.org/10.1213/ANE.0000000000002500
Boscarino, J. A., Hoffman, S. N., & Han, J. J. (2015). Opioid-use disorder among patients on long-term opioid therapy: Impact of final DSM-5 diagnostic criteria on prevalence and correlates. Substance Abuse and Rehabilitation, 6, 83–91. https://doi.org/10.2147/SAR.S85667
Carballo, J. L., Coloma-Carmona, A., Mrozowicz-Gaudyn, D., Vidal-Arenas, V., & van-der Hofstadt, C., & Rodríguez-Marín, J. (2016). Psychological assessment of opioid drug abuse. Papeles del Psicólogo, 37(1), 45–51.
Chou, R., Turner, J. A., Devine, E. B., Hansen, R. N., Sullivan, S. D., Blazina, I., Dana, T., Bougatsos, C., & Deyo, R. A. (2015). The effectiveness and risks of long-term opioid therapy for chronic pain: A systematic review for a national institutes of health pathways to prevention workshop. Annals of Internal Medicine, 162(4), 276. https://doi.org/10.7326/M14-2559
Delage, N., Cantagrel, N., Delorme, J., Pereira, B., Dualé, C., Bertin, C., Chenaf, C., Kerckhove, N., Laporte, C., Picard, P., Roussin, A., & Authier, N. (2022). Transcultural validation of a French-European version of the Prescription Opioid Misuse Index Scale (POMI-5F). Canadian Journal of Anaesthesia., 69(8), 1042–1052. https://doi.org/10.1007/s12630-022-02210-7
Dorans, N. J., & Holland, P. W. (1992). Dif detection and description: Man-Haenszel and Standardization1,2. ETS Research Report Series, 1992(1), i–40. https://doi.org/10.1002/j.2333-8504.1992.tb01440.x
Dowell, D., Haegerich, T. M., & Chou, R. (2016). CDC guideline for prescribing opioids for chronic pain—United States, 2016. MMWR. Recommendations and Reports, 65(1), 1–49. https://doi.org/10.15585/mmwr.rr6501e1
Ebel, R. L., & Frisbie, D. A. (1991). Essentials of educational measurement. Prentice-Hall.
Edelen, M. O., & Reeve, B. B. (2007). Applying item response theory (IRT) modeling to questionnaire development, evaluation, and refinement. Quality of Life Research, 16(1), 5. https://doi.org/10.1007/s11136-007-9198-0
Gallagher, H., & Galvin, D. (2018). Opioids for chronic non-cancer pain. BJA Education, 18(11), 337–341. https://doi.org/10.1016/j.bjae.2018.06.006
Hambleton, R. K., Swaminathan, H., & Rogers, H. J. (1991). Fundamentals of item response theory. SAGE.
Helmerhorst, G. T. T., Teunis, T., Janssen, S. J., & Ring, D. (2017). An epidemic of the use, misuse and overdose of opioids and deaths due to overdose, in the United States and Canada. The Bone & Joint Journal, 7, 856–864. https://doi.org/10.1302/0301-620X.99B7.BJJ-2016-1350.R1
Kalkman, G. A., van den Brink, W., Pierce, M., Atsma, F., Vissers, K. C., Schers, H. J., van Dongen, R. T., Kramers, C., & Schellekens, A. F. (2022). Monitoring opioids in Europe: The need for shared definitions and measuring drivers of opioid use and related harms. European Addiction Research, 28, 1–9. https://doi.org/10.1159/000521996
Khalid, L., Liebschutz, J. M., Xuan, Z., Dossabhoy, S., Kim, Y., Crooks, D., Shanahan, C., Lange, A., Heymann, O., & Lasser, K. E. (2015). Adherence to prescription opioid monitoring guidelines among residents and attending physicians in the primary care setting. Pain Medicine, 16(3), 480–487. https://doi.org/10.1111/pme.12602
Kim, S.-H., & Baker, F. B. (2018). birtr: A package for “The Basics of Item Response Theory Using R”. Applied Psychological Measurement, 42(5), 403–404. https://doi.org/10.1177/0146621617748327
Knisely, J. S., Wunsch, M. J., Cropsey, K. L., & Campbell, E. D. (2008). Prescription Opioid Misuse Index: A brief questionnaire to assess misuse. Journal of Substance Abuse Treatment, 35(4), 380–386. https://doi.org/10.1016/j.jsat.2008.02.001
Lalkhen, A. G., & McCluskey, A. (2008). Clinical tests: Sensitivity and specificity. Continuing Education in Anaesthesia, Critical Care & Pain, 8(6), 221–223. https://doi.org/10.1093/bjaceaccp/mkn041
Lange, A., Lasser, K. E., Xuan, Z., Khalid, L., Beers, D., Heymann, O. D., Shanahan, C. W., Crosson, J., & Liebschutz, J. M. (2015). Variability in opioid prescription monitoring and evidence of aberrant medication taking behaviors in urban safety-net clinics. Pain, 156(2), 335–340. https://doi.org/10.1097/01.j.pain.0000460314.73358.ff
Laporte, C., Fortin, F., Dupouy, J., Quirin, A., Pereira, B., Chenaf, C., Delorme, J., Maynié-François, C., Rat, C., Birebent, J., Rambaud, J., Duale, C., Kerckhove, N., Delage, N., & Authier, N. (2022). Real-life testing of the Prescription Opioid Misuse Index in French primary care. International Journal of Environmental Research and Public Health, 19(22), 14845. https://doi.org/10.3390/ijerph192214845
Lasser, K. E., Shanahan, C., Parker, V., Beers, D., Xuan, Z., Heymann, O., Lange, A., & Liebschutz, J. M. (2016). A multicomponent intervention to improve primary care provider adherence to chronic opioid therapy guidelines and reduce opioid misuse: A cluster randomized controlled trial protocol. Journal of substance abuse treatment, 60, 101–109. https://doi.org/10.1016/j.jsat.2015.06.018
Lawrence, R., Mogford, D., & Colvin, L. (2017). Systematic review to determine which validated measurement tools can be used to assess risk of problematic analgesic use in patients with chronic pain. British Journal of Anaesthesia, 119(6), 1092–1109. https://doi.org/10.1093/bja/aex316
Martel, M., Dolman, A., Edwards, R., Jamison, R., & Wasan, A. (2014). The association between negative affect and prescription opioid misuse in patients with chronic pain: The mediating role of opioid craving. The Journal of Pain, 15(1), 90–100. https://doi.org/10.1016/j.jpain.2013.09.014
Martel, M. O., Finan, P. H., McHugh, R. K., Issa, M., Edwards, R. R., Jamison, R. N., & Wasan, A. D. (2016). Day-to-day pain symptoms are only weakly associated with opioid craving among patients with chronic pain prescribed opioid therapy. Drug and Alcohol Dependence, 162, 130–136. https://doi.org/10.1016/j.drugalcdep.2016.02.047
McHugh, R. K., DeVito, E. E., Dodd, D., Carroll, K. M., Potter, J. S., Greenfield, S. F., Connery, H. S., & Weiss, R. D. (2013). Gender differences in a clinical trial for prescription opioid dependence. Journal of substance abuse treatment, 45(1), 38–43. https://doi.org/10.1016/j.jsat.2012.12.007
Meltzer, E. C., Rybin, D., Meshesha, L. Z., Saitz, R., Samet, J. H., Rubens, S. L., & Liebschutz, J. M. (2012). Aberrant drug-related behaviors: Unsystematic documentation does not identify prescription drug use disorder. Pain Medicine, 13(11), 1436–1443. https://doi.org/10.1111/j.1526-4637.2012.01497.x
Morizot, J., Ainsworth, A. T., & Reise, S. P. (2007). Toward modern psychometrics: Application of item response theory models in personality research. In En Handbook of research methods in personality psychology (pp. 407–423). The Guilford Press.
Muñiz, J., Elosua, P., & Hambleton, R. K. (2013). Directrices para la traducción y adaptación de los tests: Segunda edición. Psicothema, 25(2), 151–157. https://doi.org/10.7334/psicothema2013.24
Nunnally, J. C., & Bernstein, I. H. (1994). Psychometric theory ((3 a ed.). ed.). McGraw-Hill, Inc.
Silver, E. R., & Hur, C. (2020). Gender differences in prescription opioid use and misuse: Implications for men’s health and the opioid epidemic. Preventive Medicine, 131, 105946. https://doi.org/10.1016/j.ypmed.2019.105946
Smith, S. M., Jones, J. K., Katz, N. P., Roland, C. L., Setnik, B., Trudeau, J. J., Wright, S., Burke, L. B., Comer, S. D., Dart, R. C., Dionne, R., Haddox, J. D., Jaffe, J. H., Kopecky, E. A., Martell, B. A., Montoya, I. D., Stanton, M., Wasan, A. D., Turk, D. C., & Dworkin, R. H. (2017). Measures that identify prescription medication misuse, abuse, and related events in clinical trials: ACTTION critique and recommended considerations. The Journal of Pain, 18(11), 1287–1294. https://doi.org/10.1016/j.jpain.2017.03.015
Smith, S. M., Paillard, F., McKeown, A., Burke, L. B., Edwards, R. R., Katz, N. P., Papadopoulos, E. J., Rappaport, B. A., Slagle, A., Strain, E. C., Wasan, A. D., Turk, D. C., & Dworkin, R. H. (2015). Instruments to identify prescription medication misuse, abuse, and related events in clinical trials: An ACTTION systematic review. The Journal of Pain, 16(5), 389–411. https://doi.org/10.1016/j.jpain.2015.01.009
Trevethan, R. (2017). Sensitivity, specificity, and predictive values: Foundations, pliabilities, and pitfalls in research and practice. Frontiers in Public Health, 5, 307. https://doi.org/10.3389/fpubh.2017.00307
Volkow, N. D., & McLellan, A. T. (2016). Opioid abuse in chronic pain—Misconceptions and mitigation strategies. New England Journal of Medicine, 374(13), 1253–1263. https://doi.org/10.1056/NEJMra1507771
Voon, P., Karamouzian, M., & Kerr, T. (2017). Chronic pain and opioid misuse: A review of reviews. Substance Abuse Treatment, Prevention, and Policy, 12(1), 36. https://doi.org/10.1186/s13011-017-0120-7
Vowles, K. E., McEntee, M. L., Julnes, P. S., Frohe, T., Ney, J. P., & van der Goes, D. N. (2015). Rates of opioid misuse, abuse, and addiction in chronic pain: A systematic review and data synthesis. Pain, 156(4), 569–576. https://doi.org/10.1097/01.j.pain.0000460357.01998.f1
Wasan, A. D., Ross, E. L., Michna, E., Chibnik, L., Greenfield, S. F., Weiss, R. D., & Jamison, R. N. (2012). Craving of prescription opioids in patients with chronic pain: A longitudinal outcomes trial. The Journal of Pain, 13(2), 146–154. https://doi.org/10.1016/j.jpain.2011.10.010
Weiss, R. D., Griffin, M. L., & Hufford, C. (1995). Craving in hospitalized cocaine abusers as a predictor of outcome. The American Journal of Drug and Alcohol Abuse, 21(3), 289–301.
Youden, W. J. (1950). Index for rating diagnostic tests. Cancer, 3(1), 32–35.
Yu, C. Y. (2002). Evaluating cutoff criteria of model fit indices for latent variable models with binary and continuous outcomes. University of California.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature. This study was funded by the call for aid for conducting research to improve the care of the chronically ill complex patient and those susceptible to palliative care (2013) of the Department of Health of the Generalitat Valenciana (Spain) (ref. PCC18 /13).
Author information
Authors and Affiliations
Contributions
Both authors contributed to the design of the study. A. Coloma-Carmona participated in data collection, conducted the statistical analysis, and participated in the writing of the whole manuscript. J.L. Carballo participated in the conception and design of the study and participated in the writing of the results and discussion section of the manuscript. The two authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
The study procedures were approved by the Committee of Research and Ethics of the University Miguel Hernández de Elche and of the General University Hospital of Elche.
Informed Consent
All procedures followed were in accordance with the ethical standards of the Committee of Research and Ethics of the University Miguel Hernández de Elche and of the General University Hospital of Elche and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix A
Appendix A
POMI – Original and Spanish version
1. Do you ever use MORE of your medication, that is, take a higher dosage, than is prescribed for you? 1. ¿Alguna vez ha tomado una dosis más alta de la medicación que se le prescribió? | Yes Sí | No No |
2.Do you ever use your medication MORE OFTEN, that is, shorten the time between dosages, than is prescribed for you? 2. ¿Alguna vez ha consumido la medicación acortando el tiempo entre las dosis respecto a lo que se le había prescrito? | Yes Sí | No No |
3. Do you ever need early refills for your pain medication? 3. ¿Alguna vez ha necesitado que le recetaran más medicación para el dolor antes de lo esperado? | Yes Sí | No No |
4. Do you ever feel high or get a buzz after using your pain medication? 4. ¿Alguna vez ha sentido placer o euforia después de tomar su medicación para el dolor? | Yes Sí | No No |
5. Do you ever take your pain medication because you are upset, using the medication to relieve or cope with problems other than pain? 5. ¿Alguna vez ha tomado su medicación para el dolor porque estaba enfadado, o ha consumido su medicación para aliviar o hacer frente a problemas diferentes al dolor? | Yes Sí | No No |
6. Have you ever gone to multiple physicians including emergency room doctors, seeking more of your pain medication? 6. ¿Alguna vez ha acudido a varios médicos, incluyendo doctores de urgencias, buscando más medicación para el dolor? | Yes Sí | No No |
Scoring: Yes=1, No=0. Total score*: __________ | ||
Corrección: Sí=1, No=0 Puntuación total*: __________ *A score of ≥2 indicates presence of prescription opioid misuse *Una puntuación ≥2 indica presencia de uso problemático de opioides de prescripción | ||
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Coloma-Carmona, A., Carballo, J. . Assessing Opioid Abuse in Chronic Pain Patients: Further Validation of the Prescription Opioid Misuse Index (POMI) Using Item Response Theory. Int J Ment Health Addiction (2023). https://doi.org/10.1007/s11469-023-01029-7
Accepted:
Published:
DOI: https://doi.org/10.1007/s11469-023-01029-7