Abstract
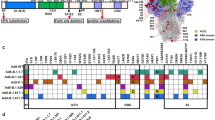
Multivalent vaccines combining crucial mutations from phylogenetically divergent variants could be an effective approach to defend against existing and future SARS-CoV-2 variants. In this study, we developed a tetravalent COVID-19 vaccine SCTV01E, based on the trimeric Spike protein of SARS-CoV-2 variants Alpha, Beta, Delta, and Omicron BA.1, with a squalene-based oil-in-water adjuvant SCT-VA02B. In the immunogenicity studies in naïve BALB/c and C57BL/6J mice, SCTV01E exhibited the most favorable immunogenic characteristics to induce balanced and broad-spectrum neutralizing potencies against pre-Omicron variants (D614G, Alpha, Beta, and Delta) and newly emerging Omicron subvariants (BA.1, BA.1.1, BA.2, BA.3, and BA.4/5). Booster studies in C57BL/6J mice previously immunized with D614G monovalent vaccine demonstrated superior neutralizing capacities of SCTV01E against Omicron subvariants, compared with the D614G booster regimen. Furthermore, SCTV01E vaccination elicited naïve and central memory T cell responses to SARS-CoV-2 ancestral strain and Omicron spike peptides. Together, our comprehensive immunogenicity evaluation results indicate that SCTV01E could become an important COVID-19 vaccine platform to combat surging infections caused by the highly immune evasive BA.4/5 variants. SCTV01E is currently being studied in a head-to-head immunogenicity comparison phase 3 clinical study with inactivated and mRNA vaccines (NCT05323461).
Article PDF
Similar content being viewed by others
References
Amanat, F., Strohmeier, S., Meade, P.S., Dambrauskas, N., Mühlemann, B., Smith, D.J., Vigdorovich, V., Sather, D.N., Coughlan, L., and Krammer, F. (2021). Vaccination with SARS-CoV-2 variants of concern protects mice from challenge with wild-type virus. PLoS Biol 19, e3001384.
Bai, Y., Du, Z., Xu, M., Wang, L., Wu, P., Lau, E.H.Y., Cowling, B.J., and Meyers, L.A. (2022). International risk of SARS-CoV-2 Omicron variant importations originating in South Africa. J Travel Med 29.
Bekliz, M., Adea, K., Vetter, P., Eberhardt, C.S., Hosszu-Fellous, K., Vu, D. L., Puhach, O., Essaidi-Laziosi, M., Waldvogel-Abramowski, S., Stephan, C., et al. (2022). Neutralization capacity of antibodies elicited through homologous or heterologous infection or vaccination against SARS-CoV-2 VOCs. Nat Commun 13, 3840.
Bi, Z., Hong, W., Que, H., He, C., Ren, W., Yang, J., Lu, T., Chen, L., Lu, S., Peng, X., et al. (2021). Inactivated SARS-CoV-2 induces acute respiratory distress syndrome in human ACE2-transgenic mice. Sig Transduct Target Ther 6, 439.
Branche, A.R., Rouphael, N.G., Diemert, D.D., Falsey, A.R., Losada, C., Baden, L.R., Frey, S.E., Whitaker, J.A., Little, S.J., Anderson, E.J., et al. (2022). SARS-CoV-2 variant vaccine boosters trial: preliminary analyses. medRxiv doi: https://doi.org/10.1101/2022.07.12.22277336.
Cameroni, E., Bowen, J.E., Rosen, L.E., Saliba, C., Zepeda, S.K., Culap, K., Pinto, D., VanBlargan, L.A., De Marco, A., di Iulio, J., et al. (2022). Broadly neutralizing antibodies overcome SARS-CoV-2 Omicron antigenic shift. Nature 602, 664–670.
Cao, Y., Yisimayi, A., Jian, F., Song, W., Xiao, T., Wang, L., Du, S., Wang, J., Li, Q., Chen, X., et al. (2022). BA.2.12.1, BA.4 and BA.5 escape antibodies elicited by Omicron infection. Nature 608, 593–602.
Carreño, J.M., Alshammary, H., Tcheou, J., Singh, G., Raskin, A.J., Kawabata, H., Sominsky, L.A., Clark, J.J., Adelsberg, D.C., Bielak, D. A., et al. (2022). Activity of convalescent and vaccine serum against SARS-CoV-2 Omicron. Nature 602, 682–688.
Chen, L.L., Chu, A.W.H., Zhang, R.R.Q., Hung, I.F.N., and To, K.K.W. (2022). Serum neutralisation of the SARS-CoV-2 omicron sublineage BA.2. Lancet Microbe 3, e404.
Dejnirattisai, W., Shaw, R.H., Supasa, P., Liu, C., Stuart, A.S., Pollard, A.J., Liu, X., Lambe, T., Crook, D., Stuart, D.I., et al. (2022). Reduced neutralisation of SARS-CoV-2 omicron B.1.1.529 variant by post-immunisation serum. Lancet 399, 234–236.
Desingu, P.A., Nagarajan, K., and Dhama, K. (2022). Emergence of Omicron third lineage BA.3 and its importance. J Med Virol 94, 1808–1810.
Du, P., Li, N., Xiong, X., Tang, S., Dai, Q., Liu, Z., Wang, T., Gu, X., and Zhou, Z. (2022). A bivalent vaccine containing D614G and BA.1 spike trimer proteins or a BA.1 spike trimer protein booster shows broad neutralizing immunity. J Med Virol 94, 4287–4293.
FDA. (2022). Pfizer/BioNTech COVID-19 Omicron-modified vaccine options. In: Food and Drug Administration (FDA) Vaccines and Related Biological Products Advisory Committee Meeting. Available from URL: https://www.fda.gov/media/159496/download.
Fisher, E., Padula, L., Podack, K., O’Neill, K., Seavey, M.M., Jayaraman, P., Jasuja, R., and Strbo, N. (2021). Induction of SARS-CoV-2 protein S-specific CD8+ T cells in the lungs of gp96-Ig-S vaccinated mice. Front Immunol 11, 602254.
Grifoni, A., Weiskopf, D., Ramirez, S.I., Mateus, J., Dan, J.M., Moderbacher, C.R., Rawlings, S.A., Sutherland, A., Premkumar, L., Jadi, R.S., et al. (2020). Targets of T cell responses to SARS-CoV-2 coronavirus in humans with COVID-19 disease and unexposed individuals. Cell 181, 1489–1501.e15.
Hachmann, N.P., Miller, J., Collier, A.Y., Ventura, J.D., Yu, J., Rowe, M., Bondzie, E.A., Powers, O., Surve, N., Hall, K., et al. (2022). Neutralization escape by SARS-CoV-2 Omicron subvariants BA.2.12.1, BA.4, and BA.5. N Engl J Med 387, 86–88.
Haddad, D., John, S.E., Mohammad, A., Hammad, M.M., Hebbar, P., Channanath, A., Nizam, R., Al-Qabandi, S., Al Madhoun, A., Alshukry, A., et al. (2021). SARS-CoV-2: possible recombination and emergence of potentially more virulent strains. PLoS ONE 16, e0251368.
He, Y., Ma, W., Dang, S., Chen, L., Zhang, R., Mei, S., Wei, X., Lv, Q., Peng, B., Chen, J., et al. (2022). Possible recombination between two variants of concern in a COVID-19 patient. Emerg Microbes Infect 11, 552–555.
Ikemura, N., Hoshino, A., Higuchi, Y., Taminishi, S., Inaba, T., and Matoba, S. (2021). SARS-CoV-2 Omicron variant escapes neutralization by vaccinated and convalescent sera and therapeutic monoclonal antibodies. medRxiv doi: https://doi.org/10.1101/2021.12.13.21267761.
Jackson, B., Boni, M.F., Bull, M.J., Colleran, A., Colquhoun, R.M., Darby, A.C., Haldenby, S., Hill, V., Lucaci, A., McCrone, J.T., et al. (2021). Generation and transmission of interlineage recombinants in the SARS-CoV-2 pandemic. Cell 184, 5179–5188.e8.
Khan, K., Karim, F., Ganga, Y., Bernstein, M., Jule, Z., Reedoy, K., Cele, S., Lustig, G., Amoako, D., Wolter, N., et al. (2022). Omicron BA.4/BA.5 escape neutralizing immunity elicited by BA.1 infection. Nat Commun 13, 4686.
Lechmere, T., Snell, L.B., Graham, C., Seow, J., Shalim, Z.A., Charalampous, T., Alcolea-Medina, A., Batra, R., Nebbia, G., Edgeworth, J. D., et al. (2022). Broad neutralization of SARS-CoV-2 variants, including Omicron, following BREAKTHROUGH INFECTION WITh Delta in COVID-19-Vaccinated Individuals. mBio 13, e0379821.
Lee, I.J., Sun, C.P., Wu, P.Y., Lan, Y.H., Wang, I.H., Liu, W.C., Yuan, J.P. Y., Chang, Y.W., Tseng, S.C., Tsung, S.I., et al. (2022). A booster dose of Delta×Omicron hybrid mRNA vaccine produced broadly neutralizing antibody against Omicron and other SARS-CoV-2 variants. J Biomed Sci 29, 49.
Li, C., Guo, Y., Fang, Z., Zhang, H., Zhang, Y., and Chen, K. (2022). Analysis of the protective efficacy of approved COVID-19 vaccines against various mutants. Front Immunol 13, 804945.
Liu, Y., Zeng, Q., Deng, C., Li, M., Li, L., Liu, D., Liu, M., Ruan, X., Mei, J., Mo, R., et al. (2022). Robust induction of B cell and T cell responses by a third dose of inactivated SARS-CoV-2 vaccine. Cell Discov 8, 10.
Lu, L., Mok, B.W.Y., Chen, L.L., Chan, J.M.C., Tsang, O.T.Y., Lam, B.H. S., Chuang, V.W.M., Chu, A.W.H., Chan, W.M., Ip, J.D., et al. (2022). Neutralization of severe acute respiratory syndrome coronavirus 2 Omicron variant by sera from BNT162b2 or CoronaVac vaccine recipients. Clin Infect Dis 75, e822–e826.
Luan, N., Wang, Y., Cao, H., Lin, K., and Liu, C. (2022). Comparison of immune responses induced by two or three doses of an alum-adjuvanted inactivated SARS-CoV-2 vaccine in mice. J Med Virol 94, 2250–2258.
Meier, S., Güthe, S., Kiefhaber, T., and Grzesiek, S. (2004). Foldon, the natural trimerization domain of T4 fibritin, dissociates into a monomeric A-state form containing a stable β-hairpin: atomic details of trimer dissociation and local β-hairpin stability from residual dipolar couplings. J Mol Biol 344, 1051–1069.
Nohynek, H., and Wilder-Smith, A. (2022). Does the world still need new COVID-19 vaccines? N Engl J Med 386, 2140–2142.
Ou, J., Lan, W., Wu, X., Zhao, T., Duan, B., Yang, P., Ren, Y., Quan, L., Zhao, W., Seto, D., et al. (2022). Tracking SARS-CoV-2 Omicron diverse spike gene mutations identifies multiple inter-variant recombination events. Sig Transduct Target Ther 7, 138.
Park, G., and Hwang, B.H. (2021). SARS-CoV-2 variants: mutations and effective changes. Biotechnol Bioproc E 26, 859–870.
Qu, P., Faraone, J., Evans, J.P., Zou, X., Zheng, Y.M., Carlin, C., Bednash, J.S., Lozanski, G., Mallampalli, R.K., Saif, L.J., et al. (2022). Neutralization of the SARS-CoV-2 Omicron BA.4/5 and BA.2.12.1 subvariants. N Engl J Med 386, 2526–2528.
Rössler, A., Knabl, L., von Laer, D., and Kimpel, J. (2022a). Neutralization profile after recovery from SARS-CoV-2 omicron infection. N Engl J Med 386, 1764–1766.
Rössler, A., Riepler, L., Bante, D., von Laer, D., and Kimpel, J. (2022b). SARS-CoV-2 Omicron variant neutralization in serum from vaccinated and convalescent persons. N Engl J Med 386, 698–700.
Reed, L.J., and Muench, H. (1938). A simple method of estimating fifty percent endpoints. Am J Epidemiol 27, 493–497.
Reynolds, C.J., Pade, C., Gibbons, J.M., Otter, A.D., Lin, K.M., Muñoz Sandoval, D., Pieper, F.P., Butler, D.K., Liu, S., Joy, G., et al. (2022). Immune boosting by B.1.1.529 (Omicron) depends on previous SARS-CoV-2 exposure. Science 377, eabq1841.
Richardson, S.I., Madzorera, V.S., Spencer, H., Manamela, N.P., van der Mescht, M.A., Lambson, B.E., Oosthuysen, B., Ayres, F., Makhado, Z., Moyo-Gwete, T., et al. (2022). SARS-CoV-2 Omicron triggers cross-reactive neutralization and Fc effector functions in previously vaccinated, but not unvaccinated, individuals. Cell Host Microbe 30, 880–886.e4.
Saxena, S.K., Kumar, S., Ansari, S., Paweska, J.T., Maurya, V.K., Tripathi, A.K., and Abdel-Moneim, A.S. (2022). Transmission dynamics and mutational prevalence of the novel severe acute respiratory syndrome coronavirus-2 Omicron variant of concern. J Med Virol 94, 2160–2166.
Schubert, M., Bertoglio, F., Steinke, S., Heine, P.A., Ynga-Durand, M.A., Maass, H., Sammartino, J.C., Cassaniti, I., Zuo, F., Du, L., et al. (2022). Human serum from SARS-CoV-2-vaccinated and COVID-19 patients shows reduced binding to the RBD of SARS-CoV-2 Omicron variant. BMC Med 20, 102.
Su, D., Li, X., Huang, X., He, C., Zeng, C., Wang, Q., Mu, Z., Qin, W., Ambrosino, D., and Siber, G. (2022). Protection from Omicron and other VOCs by Bivalent S-Trimer COVID-19 vaccine. bioRxiv, doi: https://doi.org/10.37421/2736-657X.06.2022.004.
Suryawanshi, R.K., Chen, I.P., Ma, T., Syed, A.M., Brazer, N., Saldhi, P., Simoneau, C.R., Ciling, A., Khalid, M.M., Sreekumar, B., et al. (2022). Limited cross-variant immunity from SARS-CoV-2 Omicron without vaccination. Nature 607, 351–355.
Tarke, A., Sidney, J., Methot, N., Yu, E.D., Zhang, Y., Dan, J.M., Goodwin, B., Rubiro, P., Sutherland, A., Wang, E., et al. (2021). Impact of SARS-CoV-2 variants on the total CD4+ and CD8+ T cell reactivity in infected or vaccinated individuals. Cell Rep Med 2, 100355.
Tuekprakhon, A., Huo, J., Nutalai, R., Dijokaite-Guraliuc, A., Zhou, D., Ginn, H.M., Sekvaraj, M., Liu, C., Mentzer, A.J., Supasa, P., et al. (2022a). Further antibody escape by Omicron BA.4 and BA.5 from vaccine and BA.1 serum. bioRxiv, doi: https://doi.org/10.1101/2022.05.21.492554.
Tuekprakhon, A., Nutalai, R., Dijokaite-Guraliuc, A., Zhou, D., Ginn, H. M., Selvaraj, M., Liu, C., Mentzer, A.J., Supasa, P., Duyvesteyn, H.M. E., et al. (2022b). Antibody escape of SARS-CoV-2 Omicron BA.4 and BA.5 from vaccine and BA.1 serum. Cell 185, 2422–2433.e13.
Vatteroni, M.L., Capria, A.L., Spezia, P.G., Frateschi, S., and Pistello, M. (2022). Co-infection with SARS-CoV-2 Omicron BA.1 and BA.2 subvariants in a non-vaccinated woman. Lancet Microbe 3, e478.
Wang, L.F., Tan, C.W., Chia, W.N., Zhu, F., Young, B., Chantasrisawad, N., Hwa, S.H., Yeoh, A.Y.Y., Lim, B.L., Yap, W.C., et al (2022a). Differential escape of neutralizing antibodies by SARS-CoV-2 Omicron and pre-emergent sarbecoviruses. Res Sq, doi: https://doi.org/10.21203/rs.3.rs-1362541/v1.
Wang, R., Sun, C., Ma, J., Yu, C., Kong, D., Chen, M., Liu, X., Zhao, D., Gao, S., Kou, S., et al. (2022b). A bivalent COVID-19 vaccine based on Alpha and Beta variants elicits potent and broad immune responses in mice against SARS-CoV-2 variants. Vaccines 10, 702.
WHO. (2022). COVID-19 Vaccines with WHO Emergency Use Listing. Available from URL: https://extranet.who.int/pqweb/vaccines/vacci-nescovid-19-vaccine-eul-issued.
Willett, B.J., Kurshan, A., Thakur, N., Newman, J., Manali, M., Tyson, G., Logan, N., Murcia, P.R., Snell, L.B., Edgeworth, J.D., et al. (2022). Distinct antigenic properties of the SARS-CoV-2 Omicron lineages BA.4 and BA.5. bioRxiv, doi: https://doi.org/10.1101/2022.05.25.493397.
Yamasoba, D., Kosugi, Y., Kimura, I., Fujita, S., Uriu, K., Ito, J., and Sato, K. (2022). Neutralisation sensitivity of SARS-CoV-2 omicron subvariants to therapeutic monoclonal antibodies. Lancet Infect Dis 22, 942–943.
Zeng, C., Evans, J.P., Chakravarthy, K., Qu, P., Reisinger, S., Song, N.J., Rubinstein, M.P., Shields, P.G., Li, Z., and Liu, S.L. (2022). COVID-19 mRNA booster vaccines elicit strong protection against SARS-CoV-2 Omicron variant in patients with cancer. Cancer Cell 40, 117–119.
Zhang, X., Wu, S., Wu, B., Yang, Q., Chen, A., Li, Y., Zhang, Y., Pan, T., Zhang, H., and He, X. (2021). SARS-CoV-2 Omicron strain exhibits potent capabilities for immune evasion and viral entrance. Sig Transduct Target Ther 6, 430.
Zhang, Y., Tan, W., Lou, Z., Huang, B., Zhou, W., Zhao, Y., Zhang, J., Liang, H., Li, N., Zhu, X., et al. (2022). Immunogenicity evaluating of the multivalent COVID-19 inactivated vaccine against the SARS-CoV-2 variants. Vaccines 10, 956.
Zhao, X., Li, D., Ruan, W., Chen, Z., Zhang, R., Zheng, A., Qiao, S., Zheng, X., Zhao, Y., Dai, L., et al. (2022). Effects of a prolonged booster interval on neutralization of Omicron variant. N Engl J Med 386, 894–896.
Zou, J., Kurhade, C., Xia, H., Liu, M., Xie, X., Ren, P., and Shi, P.Y. (2022). Cross-neutralization of Omicron BA.1 against BA.2 and BA.3 SARS-CoV-2. Nat Commun 13, 2956.
Acknowledgements
This work was supported by Sinocelltech with grant support from Beijing Municipal Science and Technology Program (Z211100002521026, Z221100007922012).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Compliance and ethics The author(s) are employees of Sinocelltech Ltd. and have an ownership or the potential stock option of the company.
Supporting Information
Rights and permissions
About this article
Cite this article
Wang, R., Huang, H., Yu, C. et al. A spike-trimer protein-based tetravalent COVID-19 vaccine elicits enhanced breadth of neutralization against SARS-CoV-2 Omicron subvariants and other variants. Sci. China Life Sci. 66, 1818–1830 (2023). https://doi.org/10.1007/s11427-022-2207-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11427-022-2207-7