Abstract
Air pollution remains a major threat to cardiovascular health and most acute myocardial infarction (AMI) deaths occur at home. However, currently established knowledge on the deleterious effect of air pollution on AMI has been limited to routinely monitored air pollutants and overlooked the place of death. In this study, we examined the association between short-term residential exposure to China’s routinely monitored and unmonitored air pollutants and the risk of AMI deaths at home. A time-stratified case-crossover analysis was undertaken to associate short-term residential exposure to air pollution with 0.1 million AMI deaths at home in Jiangsu Province (China) during 2016–2019. Individual-level residential exposure to five unmonitored and monitored air pollutants including PM1 (particulate matter with an aerodynamic diameter ≤ 1 μm) and PM2.5 (particulate matter with an aerodynamic diameter ≤ 2.5 μm), SO2 (sulfur dioxide), NO2 (nitrogen dioxide), and O3 (ozone) was estimated from satellite remote sensing and machine learning technique. We found that exposure to five air pollutants, even below the recently released stricter air quality standards of the World Health Organization (WHO), was all associated with increased odds of AMI deaths at home. The odds of AMI deaths increased by 20% (95% confidence interval: 8 to 33%), 22% (12 to 33%), 14% (2 to 27%), 13% (3 to 25%), and 7% (3 to 12%) for an interquartile range increase in PM1, PM2.5, SO2, NO2, and O3, respectively. A greater magnitude of association between NO2 or O3 and AMI deaths was observed in females and in the warm season. The greatest association between PM1 and AMI deaths was found in individuals aged ≤ 64 years. This study for the first time suggests that residential exposure to routinely monitored and unmonitored air pollutants, even below the newest WHO air quality standards, is still associated with higher odds of AMI deaths at home. Future studies are warranted to understand the biological mechanisms behind the triggering of AMI deaths by air pollution exposure, to develop intervention strategies to reduce AMI deaths triggered by air pollution exposure, and to evaluate the cost-effectiveness, accessibility, and sustainability of these intervention strategies.
Graphical abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Air pollution is a widely recognized and inhalable threat to cardiovascular health (GBD 2019 Risk Factors Collaborators 2020; Rajagopalan et al. 2018). As one of the major contributors to cardiovascular morbidity and mortality, acute myocardial infarction (AMI) attacks remain a major public health problem in China, leading to massive burden of hospitalizations and deaths in the past decades (Chang et al. 2017; Liu et al. 2017; Li et al. 2022). There has been an increasing number of studies reporting an increased risk of AMI attacks within few days after exposure to particulate or gaseous air pollutants such as PM2.5 (particulate matter with an aerodynamic diameter ≤ 2.5 μm), PM10 (particulate matter with an aerodynamic diameter ≤ 10 μm), SO2 (sulfur dioxide), NO2 (nitrogen dioxide), and O3 (ozone) (Rajagopalan et al. 2018; Claeys et al. 2016; Liu et al. 2021). Aside from these routinely monitored and widely studied air pollutants in many regions of the world, many routinely unmonitored air pollutants such as PM1 (particulate matter with an aerodynamic diameter ≤ 1 μm) have been increasingly reported to have adverse and greater health impacts (Chen et al., 2017a, b; Hu et al. 2018; Yen and Chen 2022). However, the effect of PM1 on AMI deaths remains largely unknown so far (Mei et al. 2022; Xu et al. 2022; Song et al. 2022).
AMI attacks have marked circadian rhythm, with incidents occurring more during midnight or early morning (Jia et al. 2012; Mohammad et al. 2018; Sert Kuniyoshi et al. 2008). AMI attacks and deaths often happen when patients are at home (Cross and Warraich 2019; Wu et al. 2021). However, the existing studies investigating the association between short-term exposure to air pollution and risk of AMI deaths mainly used city-level air pollution data, which was subject to exposure measurement bias (Bhaskaran et al. 2011; Liang et al. 2018). One recent study in China utilized air pollution data from ground monitoring stations and applied geographic prediction model to derive spatially resolved air pollutant data (Liu et al. 2021), but the prediction model had a less ideal performance for some pollutants such as SO2 (R square was 0.58). In addition, most previous studies on air pollution and AMI deaths estimated air pollution exposure based on a limited number of ground air quality monitoring stations (Chen et al. 2021; Yu et al. 2018; Zhu et al. 2017), failing to consider the air pollution level within the residential areas of decedents.
The recent advances in using satellite remote sensing and spatiotemporal models to derive air pollution data with high spatial resolution present opportunities to reduce exposure measurement bias in assessing the health impacts of air pollution. In this study, we utilized high-resolution air pollution data and conducted a multi-region time-stratified case-crossover analysis to investigate if short-term residential exposure to air pollutants (PM1, PM2.5, NO2, O3, and SO2) was associated with risk of AMI deaths at home in China. Furthermore, we attempted to examine if sex, age, educational attainment, and season modified the association between air pollutants and AMI deaths.
Methods
Study area and data collection
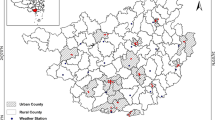
This study was conducted in Jiangsu Province, China. Jiangsu is an eastern coastal province of China and had 77 million inhabitants in its 13 cities in 2016. Previous studies have reported an association between exposure to air pollutants and the risk of cardiovascular mortality in some cities of Jiangsu Province (Chen et al. 2021; Yu et al. 2018; Zhu et al. 2017; Song et al. 2022), although they largely used city-level air pollution exposure as an approximation of individual-level air pollution exposure. We chose Jiangsu Province as the research site also because of our established collaborations with the local government agency (i.e., Jiangsu Provincial Center for Disease Control and Prevention).
Data on deaths from AMI (International Classification of Diseases, tenth version: I21) in these 13 cities from January 1, 2016 to 31 December 2019 were obtained from Jiangsu Provincial Centre for Disease Control and Prevention. For each decedent, we extracted information on their residential address, place of death, date of death, age, sex, and educational attainment. Those deaths which occurred at home were identified from the “place of death” variable and were included in this study. Age at death was categorized into four groups, including < 65, 65–74, 75–84, and ≥ 85 years. Educational attainment was dichotomized as “< 10 years” or “≥ 10 years.” We only included AMI deaths that occurred in the study region and within the study period, and we excluded those whose individual information (e.g., age, sex) was incomplete or not available.
For exposure data, we obtained satellite-derived air pollution data including daily concentrations of PM1, PM2.5, NO2, SO2, and O3. Briefly, daily air pollutant concentrations were predicted across China using a series of models with a machine learning technique called “space–time extremely randomized trees.” These models used air pollution data from ground-monitoring network, satellite remote sensing products (National Aeronautics and Space Administration’s (NASA) Terra and Aqua MODIS aerosol products), and other variables (e.g., weather conditions and land cover) as data input, and predicted daily concentrations of air pollutants at a high spatial resolution. The spatial resolutions of data on PM1 and PM2.5 and data on NO2, SO2, and O3 were 1 km and 10 km, respectively. Results from the 10-fold cross-validations suggested a high prediction accuracy for each pollutant (R square was 0.77 for PM1, 0.90 for PM2.5, 0.84 for NO2, 0.84 for SO2, and 0.87 for O3). The details of the air pollution data have been previously described (Wei et al. 2019, 2020, 2021, 2022). To adjust for temperature in the model assessing the association between air pollution and AMI deaths, we also collected hourly air temperature data from an enhanced global dataset for “the land component of the fifth generation of European reanalysis” (ERA5-land), and this air temperature data had a spatial resolution of 9 km (CDS 2021; Hersbach et al. 2020). Daily mean temperature values were calculated by averaging hourly air temperatures within 24 h. To measure residential exposure to air pollution and temperature, each decedent’s residential address was geocoded and then matched to daily spatially gridded values.
Study design
We used a time-stratified case-crossover study design to quantify the association between short-term exposure to air pollutants and risk of AMI deaths. Specifically, for each decedent, the date of death was the “case” day and “control” days were the same days in the weeks before and after the death within the same month and calendar year. For instance, if one AMI case died on Sunday, December 21, 2018 (i.e., “case” day), “control” days would have been all other Sundays within this month, including December 7, 14, and 28, 2018. This study design was chosen because it has two merits. Firstly, it can examine the association of AMI death risk with air pollution exposure at individual level. Secondly, it can automatically adjust for long-term trend and seasonality of health outcome as well as time-invariant individual variables such as age, sex, and cigarette smoking (Bhaskaran et al. 2011).
Statistical analyses
A conditional logistic regression model was utilized to fit the association between air pollution exposure and AMI death risk. To account for the temporal auto-correlation of daily air pollutant concentrations and capture the potential nonlinear association between air pollution exposure and AMI death risk (Yan et al. 2019), we used the logistic regression model combined with a distributed lag nonlinear model (DLNM). For each air pollutant, we used a cross-basis function in DLNM to simultaneously capture exposure-response and lag-response associations. A natural cubic spline function with three degrees of freedom and a maximum lag of 7 days were used for each pollutant. We also included daily mean temperature as a covariate in the models, and a natural cubic spline function with three degrees of freedom and a maximum lag of 14 days were used for temperature. The used model was as follows:
where stratumi refers to the fixed time strata i (i.e., the matched case and control periods in the same calendar month in the same year); \({\beta}_{0,{\textrm{stratum}}_{\textrm{i}}}\)indicates the intercept of stratum i; β1 ∗ air pollutant refers to the estimated coefficient β1 for each air pollutant; β ∗ covariate is the coefficient β for mean temperature.
Although the regression model with a linear or piecewise linear function may perform better statistically, we used a nonlinear function in model construction because it is closer to the complex nature of exposure-response association (Yan et al. 2019). This modeling strategy was chosen in alignment with previous studies (Liu et al. 2021; Bhaskaran et al. 2011), and based on the Bayesian information criterion. Stratified analyses were conducted to examine whether age, sex, educational attainment, and season (cold season: October to March; warm season: April to September) modified the association between air pollution exposure and AMI death risk. Result comparisons between dichotomized subgroups were examined through a two-sample z-test and trend test for ordinal categorical subgroups was performed by meta-regression technique.
All data analyses were performed using packages “survival” and “dlnm” in R software version 4.1.0. A two-sided P-value < 0.05 was considered statistically significant. We estimated odds ratio (OR) and its 95% confidence interval (CI) at a single lag day and accumulated over few days associated with an interquartile range (IQR) increase in air pollutant concentration (Guo et al. 2013). Besides, we estimated the potential minimum risk threshold and risk turning point of air pollutant from the above-fitted nonlinear exposure-response associations. Minimum risk threshold refers to a specific concentration value above which death risk increases continuously and risk turning point refers to a specific concentration above which death risk increment pattern starts to change (Chen et al., 2017a, b; Li et al. 2021). To quantify the association of AMI death risk with exposure to air pollutant concentrations below the air quality standards recommended by China and the World Health Organization (WHO), we compared the minimum risk threshold with the thresholds recommended in the China and WHO air quality standards.
Sensitivity analysis
Two sensitivity analyses were conducted. First, in recognition of the fact that people who died from AMI may not always stay indoors prior to death, we estimated the air pollution exposure within different spatial buffer areas (i.e., the radii of 10 km and 20 km within their residential address) and examined the association of AMI death risk with air pollution exposure within these buffer areas. Second, aside from one-pollutant models used for the main analysis, we also used two-pollutant models.
Results
Characteristics of the study population and exposures
There were 102,183 AMI deaths at home during the study period (Supplementary Fig. S1), and 49.3% of them were males (Supplementary Table S1). The mean death age was 78.8 years and 85.8% of the deaths occurred in elderly people (≥ 65 years). Most of these decedents had ≥ 10 years of education (97.0%) and more than half of the deaths occurred in the cold season (57.3%).
The mean values of PM1, PM2.5, NO2, SO2, and O3 on case days were 33.6 μg/m3, 55.3 μg/m3, 35.2 μg/m3, 16.6 μg/m3, and 102.6 μg/m3, respectively (Table 1). The correlation coefficients between two pollutants included in two-pollutant models were all less than 0.6 and less than 0.5 in most cases. The mean values of all air pollutants (except for NO2) on case days were higher than that on control days (P < 0.05). Meanwhile, during the days when AMI deaths happened, there were 20.4%, 0.9%, 0%, and 10.6% of days exceeding the Chinese air quality standards for PM2.5, NO2, SO2, and O3, respectively. During the days when AMI deaths happened, there were 99.5%, 71.0%, 2.7%, and 43.9% of days exceeding the WHO air standards for PM2.5, NO2, SO2, and O3, respectively.
Association between short-term exposure to air pollutants and risk of AMI deaths
Figure 1 shows the exposure-response association between exposure to five air pollutants and odds of AMI deaths at home. For PM1, PM2.5, and NO2, odds of AMI deaths increased sharply when people were exposed to these air pollutants under certain level (i.e., a turning point). The identified turning points for PM1, PM2.5, and NO2 were 28 μg/m3 (lag0–1), 50 μg/m3 (lag0–1), and 30 μg/m3 (lag0–2), respectively. For O3, odds of AMI deaths started to increase when O3 concentration exceeded 59 μg/m3 (lag0–5). There was a monotonical increase in odds of AMI deaths after exposure to SO2 (lag0–2). Noticeably, for all air pollutants included in the China or WHO air quality standards, exposure to concentrations lower than the WHO or China air quality standards was still associated with higher odds of AMI deaths.
Exposure-response association between exposure to air pollutants and odds of AMI deaths at home. Solid red line is the estimated point effect of air pollutant and shaded green area is the 95% confidence interval; exposure-response association curves were plotted with lag0–1 for PM1, lag0–1 for PM2.5, lag0–2 for NO2, lag0–5 for SO2, and lag0–5 for O3
The specific effect estimates for the association between air pollutants and odds of AMI deaths are shown in Table 2. For each air pollutant, the greatest value of effect estimates across different lags is presented. The odds of AMI deaths increased by 20% (95%CI: 8 to 33%), 22% (95%CI: 12 to 33%), 13% (95%CI: 3 to 25%), 14% (95%CI: 2 to 27%), and 7% (95%CI: 3 to 12%) for an IQR increase in PM1, PM2.5, NO2, SO2, and O3, respectively.
The timing when odds of AMI deaths increased significantly after exposure to air pollutants is presented in Fig. 2. When exposed to PM1 or PM2.5, odds of AMI deaths increased significantly on the same day of exposure or one day after exposure. Specifically, PM1- and PM2.5-related OR estimates ranged from 1.12 at lag0 to 0.94 at lag6 and from 1.14 at lag0 to 0.98 at lag6, respectively. When exposed to NO2, SO2, or O3, odds of AMI deaths increased a few days after exposure, with OR estimates ranging from 1.04 at lag1 to 1.01 at lag6, from 1.06 at lag6 to 1.00 at lag3, and from 1.02 at lag 6 to 1.01 at lag0, respectively.
Modification effect of age, sex, educational attainment, and season
Effect estimates for the association between exposure to air pollutants and odds of AMI deaths in different subgroups are shown in Table 3. A greater magnitude of association between exposure to NO2 or O3 and increased odds of AMI deaths was observed in females and in the warm season. The greatest association between PM1 exposure and increased odds of AMI deaths was found in individuals aged ≤ 64 years (OR: 1.31, 95%CI: 1.15 to 1.50), and the magnitude of this association decreased with the increase of age (P-value = 0.03).
Sensitivity analysis results
For all air pollutants except for SO2, the exposure-response associations were robust after considering various buffer areas in measuring residential exposure to air pollution (Fig. 3). Results from the two-pollutant models were consistent with the results from the single-pollutant models (Supplementary Table S2).
Discussion
This study found that residential exposure to routinely monitored and unmonitored air pollutants (PM1, PM2.5, NO2, SO2, or O3), even lower than the newest WHO air quality standards, was associated with increased odds of AMI deaths at home. The associations of O3 and NO2 with odds of AMI deaths at home were stronger in females and in the warm season. The association between PM1 and odds of AMI deaths at home appeared to be stronger in young adults than that in the elderly.
Previous studies have provided epidemiological evidence on the association between air pollution exposure and AMI death risk (Liu et al. 2021; Liang et al. 2018; Ren et al. 2010). Air pollution could be from both local sources and neighboring regions. Therefore, linking residential air pollution exposure and AMI deaths at home is essential. The present study is novel because we examined the association between residential air pollution exposure and AMI deaths at home. In many countries (e.g., USA, UK), a large proportion of deaths from cardiovascular diseases (e.g., acute heart attacks) happen at home (Cross and Warraich 2019; Wu et al. 2021). Our results suggested that residential exposure to air pollution may be a trigger of AMI deaths at home. Although Liu et al. have quantified the association between exposure to air pollutants and AMI deaths (Liu et al. 2021), they included all AMI deaths rather than those deaths occurred at home. Therefore, it is challenging to directly compare our results with theirs. Nevertheless, air pollutants such as PM10, PM2.5, NO2, SO2, and O3 have been shown to be risk factors for AMI mortality, suggesting that residential exposure to these pollutants could increase the risk of AMI deaths in China.
The main strength of this study was that we leveraged high-resolution air pollution data and individual-level health data to examine the association between short-term residential exposure to air pollution and risk of AMI deaths at home. Notably, our study demonstrated that exposure to air pollution lower than the air quality standards recommended by WHO was still associated with a higher risk of AMI deaths. Recently, WHO has released more stringent air quality standards (WHO 2021). The existing studies have consistently reported adverse cardiovascular impacts of low-level air pollution exposure (Liu et al. 2021; Cheng et al. 2021; deSouza et al. 2021). The findings from our study and previous studies suggested that exposure to low-level air pollution is still detrimental to cardiovascular health.
Three main biological mechanisms have been proposed to explain the association between short-term exposure to air pollutants and an increased risk of AMI attacks, including systematic oxidative stress, inflammation, and autonomic imbalance (Claeys et al. 2016). Fine and ultrafine particulate matters (e.g., PM2.5) have large surface area and can carry a large number of toxicants (e.g., transition metals) deep into respiratory tract, causing increases in biomarkers (e.g., oxidized low density lipoprotein and interleukin-6) of oxidative stress and inflammatory responses (Claeys et al. 2016; Araujo et al. 2008; Kelly 2003; Lin et al. 2019). Gaseous pollutants such as O3 and SO2 can modify automatic nervous system balance via the activation of pulmonary neural reflexes, whereby leading to vasoconstriction, vascular congestion, and changes in blood pressure and heart rate (Claeys et al. 2016; Perez et al. 2014). These biological responses promote or accelerate atherothrombosis and could trigger AMI attacks.
We found a stronger association between O3 exposure and risk of AMI deaths at home in the warm season than that in the cold season, which was consistent with the finding reported in a previous meta-analysis (Bergmann et al. 2020). This finding could be explained by two reasons. First, ambient O3 level is generally higher during warm months (particularly during summer). Second, people tend to open windows or go outdoors more during warm months (Bergmann et al. 2020). We also observed stronger associations of O3 and NO2 with risk of AMI deaths at home in females, echoing the finding of a previous meta-analysis (Zhao et al. 2017). Clinicians should remind their patients with high risk of AMI attacks (e.g., those with pre-existing cardiovascular diseases, particularly females) to pay attention to air quality forecasting and avoid outdoor activities during days with heavy air pollution.
In the present study, we found an association between short-term exposure to PM1 and an increased risk of AMI deaths. PM1 has a small particulate size and can deposit deep into lungs, eliciting oxidative stress and inflammation response that can cause damages to heart (Niu et al. 2021). Besides, PM1 is able to carry large concentrations of toxic components that can directly pass into circulatory system (Niu et al. 2021; Delfino et al. 2005; Polichetti et al. 2009). The association between PM1 and adverse health events (e.g., cardiovascular deaths) has been increasingly reported in China and elsewhere (Chen et al., 2017a, b; Mei et al. 2022; Perez et al. 2009). Available evidence suggested that PM1 was responsible for a large proportion of PM2.5-related disease burden (Chen et al. 2017a, b; Hu et al. 2018).
We observed a nonlinear exposure-response association between short-term exposure to air pollutants and risk of AMI deaths. Risk of AMI deaths increased faster at lower concentrations of air pollutants and appeared to flatten out at higher concentrations. This finding may be partially explained by the implementation of clean air policy, society-wide health education, and behavior adaptation (Yan et al. 2019). Similar phenomenon has also been reported in other regions of China (Liu et al. 2021; Yan et al. 2019). Adopting a nonlinear assumption of exposure-response association may help identify crucial risk turning point, which is useful for prevention of cardiovascular events (Liu et al. 2021; Yan et al. 2019).
Several limitations of this study should be acknowledged. First, this study was conducted only in one province of China, and cautions are needed when generalizing our findings to other settings. Future studies are warranted to clarify the role of background air pollution level, pollutant composition, and source in assessing the association between air pollution exposure and risk of AMI deaths. Second, we adopted a case-crossover study design that is ideal for controlling for short-term time-invariant cardiovascular risk factors. However, some short-term time-varying factors such as indoor air quality and noise pollution were not taken into account in this study. Third, although we used satellite remote sensing data to estimate residential exposure to air pollution, we could not rule out the possibility that exposure measurement bias may still exist. Fourth, due to the issue of data availability, we were only able to obtain data on AMI patients who died at home but could not obtain death data on AMI patients who died on the way to hospitals and those who died in nursing facilities. We cannot rule out the possibility that the effect of air pollution on AMI mortality may vary by the death place of AMI patients. Fifth, since this was the first study to explore the effect of air pollutants on AMI deaths at home stratified by sex, we were less able to directly compare our findings with previous studies and explore the underlying reasons behind the difference in the association between air pollution exposure and AMI deaths across two sexes. Sixth, only PM1, PM2.5, NO2, SO2, and O3 were examined in our study, and other air pollutants such as CO (carbon monoxide) that may have an impact on AMI mortality were not included in our study because of the unavailability of high-resolution CO data. Despite the limitations, our findings have potential implications for protecting public health. First, AMI is a major public health issue in China and the associated disease burden shows an upward trend in recent years (Chang et al. 2017; Liu et al. 2017; Li et al. 2022). In China, most AMI deaths take place at home. Second, this study suggests that PM1 is an important but currently less reported risk factor of AMI death. Future research is urgently needed to assess the adverse health effect of PM1 or finer particulate matter. Third, results of subgroup analyses by season, educational level, age, and sex are useful for targeting vulnerable populations.
Conclusion
In conclusion, this large-scale case-crossover study in China provides evidence that residential exposure to routinely monitored and unmonitored air pollutants, even at concentrations lower than the newest WHO air quality standards, is still associated with a higher risk of AMI deaths at home. Females are more vulnerable to NO2 and O3 than males, and young adults are more vulnerable to PM1 than elderly. Since air pollution is an important contributor to global cardiovascular disease burden, our findings highlight that continued efforts to lower air pollution or avoid air pollution exposure are necessary in residential settings. Future studies are warranted to understand the biological mechanisms behind the triggering of AMI deaths by air pollution exposure, to develop intervention strategies to reduce AMI deaths triggered by air pollution exposure, and to evaluate the cost-effectiveness, accessibility, and sustainability of these intervention strategies.
Data availability
All data generated or analyzed during this study are included in this published article.
References
Araujo JA, Barajas B, Kleinman M et al (2008) Ambient particulate pollutants in the ultrafine range promote early atherosclerosis and systemic oxidative stress. Circ Res 102(5):589–596
Bergmann S, Li B, Pilot E, Chen R, Wang B, Yang J (2020) Effect modification of the short-term effects of air pollution on morbidity by season: a systematic review and meta-analysis. Sci Total Environ 716:136985
Bhaskaran K, Hajat S, Armstrong B et al (2011) The effects of hourly differences in air pollution on the risk of myocardial infarction: case crossover analysis of the MINAP database. BMJ 343:d5531
Chang J, Liu X, Sun Y (2017) Mortality due to acute myocardial infarction in China from 1987 to 2014: secular trends and age-period-cohort effects. Int J Cardiol. 227:229–238
Chen G, Li S, Zhang Y et al (2017) Effects of ambient PM1 air pollution on daily emergency hospital visits in China: an epidemiological study. Lancet Planet Health 1(6):e221–e229
Chen Q, Wang Q, Xu B, Xu Y, Ding Z, Sun H (2021) Air pollution and cardiovascular mortality in Nanjing, China: evidence highlighting the roles of cumulative exposure and mortality displacement. Chemosphere. 265:129035
Chen R, Yin P, Meng X et al (2017) Fine particulate air pollution and daily mortality. A nationwide analysis in 272 Chinese cities. Am J Respir Crit Care Med 196(1):73–81
Cheng J, Ho HC, Webster C et al (2021) Lower-than-standard particulate matter air pollution reduced life expectancy in Hong Kong: a time-series analysis of 8.5 million years of life lost. Chemosphere 272:129926
Claeys MJ, Rajagopalan S, Nawrot TS, Brook RD (2016) Climate and environmental triggers of acute myocardial infarction. Eur Heart J 38(13):955–960
Copernicus Climate Change Service Climate Data Store (CDS). (2021) ERA5: fifth generation of ECMWF atmospheric reanalyses of the global climate. https://cds.climate.copernicus.eu/cdsapp#!/home (accessed on July 27, 2021).
Cross SH, Warraich HJ (2019) Changes in the place of death in the United States. N Engl J Med 381(24):2369–2370
Delfino RJ, Sioutas C, Malik S (2005) Potential role of ultrafine particles in associations between airborne particle mass and cardiovascular health. Environ Health Perspect 113(8):934–946
deSouza P, Braun D, Parks RM, Schwartz J, Dominici F, Kioumourtzoglou M-A (2021) Nationwide study of short-term exposure to fine particulate matter and cardiovascular hospitalizations among Medicaid enrollees. Epidemiology 32(1):6–13
GBD 2019 Risk Factors Collaborators. (2020) Global burden of 87 risk factors in 204 countries and territories, 1990-2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 396(10258):1223-1249
Guo Y, Li S, Tian Z, Pan X, Zhang J, Williams G (2013) The burden of air pollution on years of life lost in Beijing, China, 2004-08: retrospective regression analysis of daily deaths. BMJ 347:f7139
Hersbach H, Bell B, Berrisford P et al (2020) The ERA5 global reanalysis. Q J R Meteorol Soc 146(730):1999–2049
Hu K, Guo Y, Hu D et al (2018) Mortality burden attributable to PM1 in Zhejiang province. China. Environ Int 121:515–522
Jia EZ, Xu ZX, Cai HZ et al (2012) Time distribution of the onset of chest pain in subjects with acute ST-elevation myocardial infarction: an eight-year, single-center study in China. PLoS ONE 7(3):e32478
Kelly FJ (2003) Oxidative stress: its role in air pollution and adverse health effects. Occup Environ Med 60(8):612–616
Li M, Dong H, Wang B et al (2021) Association between ambient ozone pollution and mortality from a spectrum of causes in Guangzhou, China. Sci Total Environ 754:142110
Li S, Gao X, Yang J, Xu H, Wang Y, Zhao Y, Yin L, Wu C, Wang Y, Zheng Y, Li B, Zhang X, Ye Y, Fu R, Dong Q, Sun H, Yan X, Wu Y, Zhang J et al (2022) Number of standard modifiable risk factors and mortality in patients with first-presentation ST-segment elevation myocardial infarction: insights from China Acute Myocardial Infarction registry. BMC Med. 20(1):217
Liang H, Qiu H, Tian L (2018) Short-term effects of fine particulate matter on acute myocardial infraction mortality and years of life lost: a time series study in Hong Kong. Sci Total Environ 615:558–563
Lin Z, Chen R, Jiang Y et al (2019) Cardiovascular benefits of fish-oil supplementation against fine particulate air pollution in China. J Am Coll Cardiol 73(16):2076–2085
Liu H, Tian Y, Xiang X, Sun K, Juan J, Song J, Cao Y, Xu B, Hu Y (2017) Air pollution and hospitalization for acute myocardial infarction in China. Am J Cardiol. 120(5):753–758
Liu Y, Pan J, Fan C et al (2021) Short-term exposure to ambient air pollution and mortality from myocardial infarction. J Am Coll Cardiol 77(3):271–281
Mei L, Yan S, Li Y et al (2022) Association between short-term PM1 exposure and cardiorespiratory diseases: evidence from a systematic review and meta-analysis. Atmos Pollut Res 13(1):101254
Mohammad MA, Karlsson S, Haddad J et al (2018) Christmas, national holidays, sport events, and time factors as triggers of acute myocardial infarction: SWEDEHEART observational study 1998-2013. BMJ 363:k4811
Niu X, Wang Y, Ho SSH et al (2021) Characterization of organic aerosols in PM1 and their cytotoxicity in an urban roadside area in Hong Kong. Chemosphere 263:128239
Perez CM, Hazari MS, Farraj AK (2014) Role of autonomic reflex arcs in cardiovascular responses to air pollution exposure. Cardiovasc Toxicol 15:69–78
Perez L, Medina-Ramón M, Künzli N et al (2009) Size fractionate particulate matter, vehicle traffic, and case-specific daily mortality in Barcelona, Spain. Environ Sci Technol 43(13):4707–4714
Polichetti G, Cocco S, Spinali A, Trimarco V, Nunziata A (2009) Effects of particulate matter (PM10, PM2.5 and PM1) on the cardiovascular system. Toxicology 261(1):1–8
Rajagopalan S, Al-Kindi SG, Brook RD (2018) Air pollution and cardiovascular disease: JACC state-of-the-art review. J Am Coll Cardiol 72(17):2054–2070
Ren C, Melly S, Schwartz J (2010) Modifiers of short-term effects of ozone on mortality in eastern Massachusetts - a casecrossover analysis at individual level. Environ Health 9(1):3
Sert Kuniyoshi FH, Garcia-Touchard A, Gami AS et al (2008) Day–night variation of acute myocardial infarction in obstructive sleep apnea. J Am Coll Cardiol 52(5):343–346
Song J, Ding Z, Zheng H, Xu Z, Cheng J, Pan R, Yi W, Wei J, Su H (2022) Short-term PM1 and PM2.5 exposure and asthma mortality in Jiangsu Province, China: What's the role of neighborhood characteristics? Ecotoxicol Environ Saf. 241:113765
Wei J, Li Z, Cribb M et al (2020) Improved 1km resolution PM2.5 estimates across China using enhanced space–time extremely randomized trees. Atmos Chem Phys 20(6):3273–3289
Wei J, Li Z, Guo J et al (2019) Satellite-derived 1-km-resolution PM1 concentrations from 2014 to 2018 across China. Environ Sci Technol 53(22):13265–13274
Wei J, Li Z, Li K et al (2022) Full-coverage mapping and spatiotemporal variations of ground-level ozone (O3) pollution from 2013 to 2020 across China. Remote Sens Environ 270:112775
Wei J, Li Z, Lyapustin A et al (2021) Reconstructing 1-km-resolution high-quality PM2.5 data records from 2000 to 2018 in China: spatiotemporal variations and policy implications. Remote Sens Environ 252:112136
World Health Organization (WHO) (2021) WHO global air quality guidelines: particulate matter (PM2.5 and PM10), ozone, nitrogen dioxide, sulfur dioxide and carbon monoxide. In. Geneva
Wu J, Mamas MA, Mohamed MO et al (2021) Place and causes of acute cardiovascular mortality during the COVID-19 pandemic. Heart 107(2):113–119
Xu R, Wei J, Liu T, Li Y, Yang C, Shi C, Chen G, Zhou Y, Sun H, Liu Y (2022) Association of short-term exposure to ambient PM1 with total and cause-specific cardiovascular disease mortality. Environ Int. 169:107519
Yan M, Wilson A, Bell ML et al (2019) The shape of the concentration-response association between fine particulate matter pollution and human mortality in Beijing, China, and its implications for health impact assessment. Environ Health Perspect 127(6):067007
Yen CC, Chen PL (2022) Regional air pollution severity affects the incidence of acute myocardial infarction triggered by short-term pollutant exposure: a time-stratified case-crossover analysis. Environ Sci Pollut Res Int. 29(6):8473–8478
Yu Y, Yao S, Dong H, Ji M, Chen Z, Li G, Yao X, Wang SL, Zhang Z (2018) Short-term effects of ambient air pollutants and myocardial infarction in Changzhou, China. Environ Sci Pollut Res Int. 25(22):22285–22293
Zhao L, Liang H-R, Chen F-Y, Chen Z, Guan W-J, Li J-H (2017) Association between air pollution and cardiovascular mortality in China: a systematic review and meta-analysis. Oncotarget 8(39):66438–66448
Zhu J, Zhang X, Zhang X, Dong M, Wu J, Dong Y, Chen R, Ding X, Huang C, Zhang Q, Zhou W (2017) The burden of ambient air pollution on years of life lost in Wuxi, China, 2012-2015: a time-series study using a distributed lag non-linear model. Environ Pollut. 224:689–697
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions This work was supported by National Natural Science Foundation of China (42105165) and High-level Scientific Research Foundation of Anhui Medical University (0305044201), and Discipline Construction of Anhui Medical University (0301001836).
Author information
Authors and Affiliations
Contributions
Jian Cheng: conceptualization, funding acquisition, formal analysis, visualization, and writing—original draft. Hao Zheng: formal analysis and visualization. Jing Wei: formal analysis and visualization. Cunrui Huang: writing—review and editing. Hung Chak Ho: writing—review and editing. Shengzhi Sun: writing—review and editing. Dung Phung: writing—review and editing. Ho Kim: writing—review and editing. Xiling Wang: writing—review and editing. Zhongliang Bai: writing—review and editing. Mohammad Zahid Hossain: writing—review and editing. Shilu Tong: writing—review and editing. Hong Su: writing—review and editing. Zhiwei Xu: conceptualization, network building, and writing—review and editing.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was approved by the Institutional Ethics Board at the School of Public Health, Anhui Medical University (ethics approval number: 20210330). The approval included an informed consent waiver.
Consent for publication
Not applicable (this manuscript does not include any individual person’s information).
Conflict of interest
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 59 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cheng, J., Zheng, H., Wei, J. et al. Short-term residential exposure to air pollution and risk of acute myocardial infarction deaths at home in China. Environ Sci Pollut Res 30, 76881–76890 (2023). https://doi.org/10.1007/s11356-023-27813-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-023-27813-5