Abstract
Cadmium, lead, and mercury are nephrotoxic metals that are commonly found as hazardous pollutants in many areas of the USA. We examined the relationship between exposure to cadmium, lead, and mercury with the occurrence of urgency urinary incontinence (UUI) and stress urinary incontinence (SUI) in women. This study was conducted using data on women > 20 years of age, collected between 2005 and 2016, who reported experiencing urinary incontinence in the National Health and Nutrition Examination Survey (NHANES). Restricted cubic spline analysis was used to characterize a dose–response relationship between continuous exposure to different nephrotoxic metals and the occurrence of UUI and SUI. A total of 4406 women were included in this study, with 2624 (59.6%) suffering from SUI and 3177 (72.1%) suffering from UUI in the weighted population. The results of our multivariate analysis indicated that age, race, marital status, body mass index (BMI), and exposure to nephrotoxic metals were risk factors for developing UI. The odds ratio (OR; 95% confidence interval) for developing UI was positively correlated with the exposure to cadmium and lead in women. The OR of SUI occurrence increased with increasing levels of cadmium in blood, with a peak at 4 µg/L. The OR of UUI occurrence increased with increasing levels of blood and urinary lead, with peaks at 7 µg/dL and 5 µg/L, respectively. The presence of mercury was not significantly correlated with the occurrence of SUI or UUI. Exposure to high levels of cadmium and lead, which are nephrotoxic metals, is associated with the occurrence of UI in women.






Similar content being viewed by others
Data availability statement
The data that support the findings of this study are available from the corresponding author, Bo Peng, upon reasonable request.
Change history
23 March 2023
A Correction to this paper has been published: https://doi.org/10.1007/s11356-023-26634-w
References
Afsar B, Elsurer Afsar R, Kanbay A, Covic A, Ortiz A, Kanbay M (2019) Air pollution and kidney disease: review of current evidence. Clin Kidney J 12(1):19–32. https://doi.org/10.1093/ckj/sfy111
Almousa S, Bandin van Loon A (2018) The prevalence of urinary incontinence in nulliparous adolescent and middle-aged women and the associated risk factors: a systematic review. Maturitas 107:78–83. https://doi.org/10.1016/j.maturitas.2017.10.003
Bridges CC, Zalups RK (2017) The aging kidney and the nephrotoxic effects of mercury. J Toxicol Environ Health B Crit Rev 20(2):55–80. https://doi.org/10.1080/10937404.2016.1243501
Brown JS, Vittinghoff E, Wyman JF, Stone KL, Nevitt MC, Ensrud KE, Grady D (2000) Urinary incontinence: does it increase risk for falls and fractures? Study of Osteoporotic Fractures Research Group. J Am Geriatr Soc 48(7):721–725. https://doi.org/10.1111/j.1532-5415.2000.tb04744.x
CDC (2006) Centers for disease control and prevention: NHANES Survey Methods and Analytic Guidelines. (Accessed March 2022). CDC https://wwwn.cdc.gov/nchs/nhanes/analyticguidelines.aspx
Chowdhury R, Ramond A, O’Keeffe LM, Shahzad S, Kunutsor SK, Muka T, Gregson J, Willeit P, Warnakula S, Khan H, Chowdhury S, Gobin R, Franco OH, Di Angelantonio E (2018) Environmental toxic metal contaminants and risk of cardiovascular disease: systematic review and meta-analysis. BMJ 362:k3310. https://doi.org/10.1136/bmj.k3310
Chughtai B, Thomas D, Russell D, Bowles K, Prigerson H (2019) Prevalence of and risk factors for urinary incontinence in home hospice patients. Eur Urol 75(2):268–271. https://doi.org/10.1016/j.eururo.2018.10.027
Dolan LC, Flannery BM, Hoffman-Pennesi D, Gavelek A, Jones OE, Kanwal R, Wolpert B, Gensheimer K, Dennis S, Fitzpatrick S (2020) A review of the evidence to support interim reference level for dietary lead exposure in adults. Regul Toxicol Pharmacol 111:104579. https://doi.org/10.1016/j.yrtph.2020.104579
Duan W, Xu C, Liu Q, Xu J, Weng Z, Zhang X, Basnet TB, Dahal M, Gu A (2020) Levels of a mixture of heavy metals in blood and urine and all-cause, cardiovascular disease and cancer mortality: a population-based cohort study. Environ Pollut (Barking, Essex: 1987) 263(Pt A):114630. https://doi.org/10.1016/j.envpol.2020.114630
Edwards JR, Prozialeck WC (2009) Cadmium, diabetes and chronic kidney disease. Toxicol Appl Pharmacol 238(3):289–293. https://doi.org/10.1016/j.taap.2009.03.007
Fowler BA, DuVal G (1991) Effects of lead on the kidney: roles of high-affinity lead-binding proteins. Environ Health Perspect 91:77–80. https://doi.org/10.1289/ehp.919177
John G (2020) Urinary incontinence and cardiovascular disease: a narrative review. Int Urogynecol J 31(5):857–863. https://doi.org/10.1007/s00192-019-04058-w
Johri N, Jacquillet G, Unwin R (2010) Heavy metal poisoning: the effects of cadmium on the kidney. Biometals 23(5):783–792. https://doi.org/10.1007/s10534-010-9328-y
Kerper LE, Hinkle PM (1997) Cellular uptake of lead is activated by depletion of intracellular calcium stores. J Biol Chem 272(13):8346–8352. https://doi.org/10.1074/jbc.272.13.8346
Lukacz ES, Santiago-Lastra Y, Albo ME, Brubaker L (2017) Urinary Incontinence in women: a review. JAMA 318(16):1592–1604. https://doi.org/10.1001/jama.2017.12137
Minassian VA, Yan X, Lichtenfeld MJ, Sun H, Stewart WF (2012) The iceberg of health care utilization in women with urinary incontinence. Int Urogynecol J 23(8):1087–1093. https://doi.org/10.1007/s00192-012-1743-x
Muth CC (2017) Urinary incontinence in women. JAMA 318(16):1622. https://doi.org/10.1001/jama.2017.15571
Nygaard IE, Shaw JM (2016) Physical activity and the pelvic floor. Am J Obstet Gynecol 214(2):164–171. https://doi.org/10.1016/j.ajog.2015.08.067
Odabaei G, Chatterjee D, Jazirehi AR, Goodglick L, Yeung K, Bonavida B (2004) Raf-1 kinase inhibitor protein: structure, function, regulation of cell signaling, and pivotal role in apoptosis. Adv Cancer Res 91:169–200. https://doi.org/10.1016/s0065-230x(04)91005-6
Orr SE, Bridges CC (2017) Chronic kidney disease and exposure to nephrotoxic metals. Int J Mol Sci 18(5). https://doi.org/10.3390/ijms18051039
Orsini N, Greenland S (2011) A procedure to tabulate and plot results after flexible modeling of a quantitative covariate. Stand Genomic Sci 11(1):1–29. https://doi.org/10.1177/1536867X1101100101
Peng S, Hajela RK, Atchison WD (2002) Characteristics of block by Pb2+ of function of human neuronal L-, N-, and R-type Ca2+ channels transiently expressed in human embryonic kidney 293 cells. Mol Pharmacol 62(6):1418–1430. https://doi.org/10.1124/mol.62.6.1418
Rana MN, Tangpong J, Rahman MM (2018) Toxicodynamics of lead, cadmium, mercury and arsenic- induced kidney toxicity and treatment strategy: a mini review. Toxicol Rep 5:704–713. https://doi.org/10.1016/j.toxrep.2018.05.012
Satarug S, Gobe GC, Vesey DA, Phelps KR (2020) Cadmium and lead exposure, nephrotoxicity, and mortality. Toxics 8(4). https://doi.org/10.3390/toxics8040086
Simons TJ (1993) Lead transport and binding by human erythrocytes in vitro. Pflugers Arch 423(3–4):307–313. https://doi.org/10.1007/bf00374410
Singh RD, Tiwari R, Khan H, Kumar A, Srivastava V (2015) Arsenic exposure causes epigenetic dysregulation of IL-8 expression leading to proneoplastic changes in kidney cells. Toxicol Lett 237(1):1–10. https://doi.org/10.1016/j.toxlet.2015.05.014
Sun Y, Zhou Q, Zheng J (2019) Nephrotoxic metals of cadmium, lead, mercury and arsenic and the odds of kidney stones in adults: an exposure-response analysis of NHANES 2007–2016. Environ Int 132:105115. https://doi.org/10.1016/j.envint.2019.105115
Thévenod F (2003) Nephrotoxicity and the proximal tubule. Nephron Physiol 93(4):87-p93. https://doi.org/10.1159/000070241
Urinary Incontinence in Women (2020) Ann Intern Med 172(3):ITC17–ITC32. https://doi.org/10.7326/aitc202002040%m32016335
Vaughan CP, Markland AD (2020) Urinary incontinence in women. Ann Intern Med 172(3):ITC17–ITC32. https://doi.org/10.7326/AITC202002040
Weinberg AE, Leppert JT, Elliott CS (2015) Biochemical measures of diabetes are not independent predictors of urinary incontinence in women. J Urol 194(6):1668–1674. https://doi.org/10.1016/j.juro.2015.06.074
Wood LN, Anger JT (2014) Urinary Incontinence in Women. Bmj 349:g4531. https://doi.org/10.1136/bmj.g4531
Wu JM, Vaughan CP, Goode PS, Redden DT, Burgio KL, Richter HE, Markland AD (2014) Prevalence and trends of symptomatic pelvic floor disorders in U.S. women. Obstet Gynecol 123(1):141–148. https://doi.org/10.1097/aog.0000000000000057
Yang B, Xie Y, Guo M, Rosner MH, Yang H, Ronco C (2018a) Nephrotoxicity and Chinese herbal medicine. Clin J Am Soc Nephrol 13(10):1605–1611. https://doi.org/10.2215/cjn.11571017
Yang E, Lisha NE, Walter L, Obedin-Maliver J, Huang AJ (2018b) Urinary incontinence in a national cohort of older women: implications for caregiving and care dependence. J Womens Health (larchmt) 27(9):1097–1103. https://doi.org/10.1089/jwh.2017.6891
Yao X, Steven Xu X, Yang Y, Zhu Z, Zhu Z, Tao F, Yuan M (2021) Stratification of population in NHANES 2009–2014 based on exposure pattern of lead, cadmium, mercury, and arsenic and their association with cardiovascular, renal and respiratory outcomes. Environ Int 149:106410. https://doi.org/10.1016/j.envint.2021.106410
Zalups RK, Ahmad S (2004) Homocysteine and the renal epithelial transport and toxicity of inorganic mercury: role of basolateral transporter organic anion transporter 1. J Am Soc Nephrol 15(8):2023–2031. https://doi.org/10.1097/01.asn.0000135115.63412.a9
Zheng LY, Sanders AP, Saland JM, Wright RO, Arora M (2017) Environmental exposures and pediatric kidney function and disease: a systematic review. Environ Res 158:625–648. https://doi.org/10.1016/j.envres.2017.06.029
Zipf G, Chiappa M, Porter KS, Ostchega Y, Lewis BG, Dostal J (2013) National health and nutrition examination survey: plan and operations, 1999–2010. Vital Health Stat 1(56):1–37
Acknowledgements
We thanked Bullet Edits for editing this manuscript.
Funding
We are very grateful to all the participants in this research project. This work was supported by the National Key R&D Program of China (Grant No. 2021YFC2009304); the National Natural Science Foundation of China (Grant No. 81870517 and 32070646); Shanghai Association for Science and Technology Commission (Grant No. 19140905700 and 19140905402).
Author information
Authors and Affiliations
Contributions
Conception and design: JN, ZL, WM, and BP. Administrative support: YL, HZ, JX, and GW. Provision of study materials or patients: YW, JX, YZ. Collection and assembly of data: WM, KW, and BP. Data analysis and interpretation: JN, ZL, and KW.
Manuscript writing: All authors. Final approval of manuscript: all authors.
Corresponding author
Ethics declarations
Ethics approval
The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). This study used previously collected deidentified data, which was deemed exempt from review by the Ethics Committee of the Tenth People’s Hospital of Shanghai.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.

11356_2022_20598_MOESM1_ESM.jpg
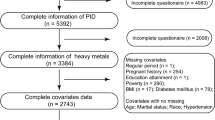
Supplementary file1 (JPG 208 KB) Figure S1: Flow chart depicting the criteria used in this study to include or exclude data collected in the NHANES 2005–2016.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ni, J., Li, Z., Lu, Y. et al. Relationship between exposure to cadmium, lead, and mercury and the occurrence of urinary incontinence in women. Environ Sci Pollut Res 29, 68410–68421 (2022). https://doi.org/10.1007/s11356-022-20598-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-022-20598-z