Abstract
Background
Obstructive sleep apnea (OSA) is associated with multiple comorbidities, including diabetes. Its development is preceded by alterations in the initial phase of carbohydrate metabolism characterized by insulin resistance. This study aims to evaluate the role of intermittent hypoxia and sleep fragmentation characteristic of OSA on the risk of insulin resistance among apneic patients without diabetes.
Methodology
92 consecutive patients with OSA without evidence of diabetes were recruited. Overnight video polysomnography was performed and, the following morning, fasting blood glucose, insulin and glycosylated hemoglobin were determined. Insulin resistance was measured using the HOMA-IR index.
Results
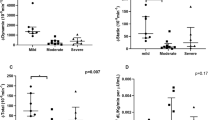
Insulin resistance was present in 52.2% of OSA patients. In these subjects, insulin resistance was independently associated to the apnea index during REM sleep (adjusted odds ratio [aOR] 1.09; 95% CI, 1.03 to 1.16; p = 0.004), desaturation index (aOR 1.08; 95% CI: 1.04 to 1.13; p = 0.027), and sleep time with oxygen saturation below 90% (aOR 1.04; 95% CI 1.00 to 1.08; p = 0.049). Furthermore, the HOMA-IR level was also directly related to the desaturation index (standardized regression coefficient [B] = 0.514, p < 0.001) and to the apnea index during REM sleep (B = 0.344, p = 0.002).
Conclusions
Intermittent hypoxia and disturbances in REM sleep emerge as main contributors to insulin resistance in OSA patients yet to experience diabetes onset.

Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request. We are committed to sharing our research data in accordance with ethical and privacy considerations.
References
Surani S, Brito V, Surani A, Ghamande S (2015) Effect of diabetes mellitus on sleep quality. World J Diabetes 6:868–873
Rasche K, Keller T, Tautz B, Hader C, Hergenc G, Antosiewicz J et al (2010) Obstructive sleep apnea and type 2 diabetes. Eur J Med Res 15:152–156
Martínez Cerón E, Casitas Mateos R, García-Río F (2015) Sleep apnea-hypopnea syndrome and type 2 diabetes. A reciprocal relationship? Arch Bronconeumol 51:128–39
Medeiros CC, Ramos AT, Cardoso MA, França IS, Cardoso Ada S, Gonzaga NC (2011) Insulin resistance and its association with metabolic syndrome components. Arq Bras Cardiol 97:380–389
Ota H, Fujita Y, Yamauchi M, Muro S, Kimura H, Takasawa S (2019) Relationship Between Intermittent Hypoxia and Type 2 Diabetes in Sleep Apnea Syndrome. Int J Mol Sci 20:1–14
Vgontzas AN, Liao D, Pejovic S, Calhoun S, Karataraki M, Bixler EO (2009) Insomnia with objective short sleep duration is associated with type 2 diabetes: A population-based study. Diabetes Care 32:1980–1985
Sulit L, Storfer-Isser A, Kirchner HL, Redline S (2006) Differences in polysomnography predictors for hypertension and impaired glucose tolerance. Sleep 29:777–783
Gangwisch JE, Heymsfield SB, Boden-Albala B, Buijs RM, Kreier F, Pickering TG et al (2007) Sleep duration as a risk factor for diabetes incidence in a large U.S. sample. Sleep 30:1667–73
Xu J, Long YS, Gozal D, Epstein PN (2009) Beta-cell death and proliferation after intermittent hypoxia: role of oxidative stress. Free Radic Biol Med 46:783–790
Li J, Thorne LN, Punjabi NM, Sun CK, Schwartz AR, Smith PL et al (2005) Intermittent hypoxia induces hyperlipidemia in lean mice. Circ Res 97:698–706
Polotsky VY, Li J, Punjabi NM, Rubin AE, Smith PL, Schwartz AR et al (2003) Intermittent hypoxia increases insulin resistance in genetically obese mice. J Physiol 552:253–264
Xu W, Chi L, Row BW, Xu R, Ke Y, Xu B et al (2004) Increased oxidative stress is associated with chronic intermittent hypoxia-mediated brain cortical neuronal cell apoptosis in a mouse model of sleep apnea. Neuroscience 126:313–323
Pialoux V, Hanly PJ, Foster GE, Brugniaux JV, Beaudin AE, Hartmann SE et al (2009) Effects of exposure to intermittent hypoxia on oxidative stress and acute hypoxic ventilatory response in humans. Am J Respir Crit Care Med 180:1002–1009
Stamatakis KA, Punjabi NM (2010) Effects of sleep fragmentation on glucose metabolism in normal subjects. Chest 137:95–101
Apnea N-P (2015) Detection and Mechanism. J Clin Sleep Med 15(11):987–993
Chiner E, Arriero JM, Signes-Costa J, Marco J, Fuentes I (1999) Validation of the Spanish version of the Epworth Sleepiness Scale in patients with a sleep apnea syndrome. Arch Bronconeumol 35(9):422–427
Berry RB, Budhiraja R, Gottlieb DJ et al (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
Bonnet MH, Carey DW, Carskadon MA, Easton PA (1992) EEG arousals: scoring rules and examples: a preliminary report from the Sleep Disorders Atlas Task Force of the American Sleep Disorders Association. Sleep 15:173–84
Lloberes P, Durán-Cantolla J, Martínez-García M, Marín JM, Ferrer A, Corral J et al (2011) Diagnosis and treatment of sleep apnea-hypopnea syndrome Spanish. Society of Pulmonology and Thoracic Surgery. Arch Bronconeumol 47:143–56
Mediano O, González Mangado N, Montserrat JM, Alonso-Álvarez ML, Almendros I, Alonso-Fernández A et al (2022) International Consensus Document on Obstructive Sleep Apnea. Arch Bronconeumol 58:52–68
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
Arjmand B, EbrahimiFana S, Ghasemi E, Kazemi A, Ghodssi-Ghassemabadi R, Dehghanbanadaki H et al (2022) Metabolic signatures of insulin resistance in non-diabetic individuals. BMC Endocr Disord 22:212
Quon MJ (2002) QUICKI is a useful and accurate index of insulin sensitivity. J Clin Endocrinol Metab 87:949–951
Louis M, Punjabi NM (2009) Effects of acute intermittent hypoxia on glucose metabolism in awake healthy volunteers. J Appl Physiol 106:1538–1544
Cantley J, Grey ST, Maxwell PH, Withers DJ (2010) The hypoxia response pathway and β-cell function. Diabetes Obes Metab 12:159–167
Bensellam M, Duvillié B, Rybachuk G, Laybutt DR, Magnan C, Guiot Y et al (2012) Glucose-induced O2 consumption activates hypoxia inducible factors 1 and 2 in rat insulin-secreting pancreatic beta-cells. PLoS ONE 7:e29807
Hecht L, Möhler R, Meyer G (2011) Effects of CPAP-respiration on markers of glucose metabolism in patients with obstructive sleep apnoea syndrome: a systematic review and meta-analysis. Ger Med Sci 9:20–45
Yang D, Liu Z, Yang H (2012) The impact of effective continuous positive airway pressure on homeostasis model assessment insulin resistance in non-diabetic patients with moderate to severe obstructive sleep apnea. Diabetes Metab Res Rev 28:499–504
Yang D, Liu Z, Yang H, Luo Q (2013) Effects of continuous positive airway pressure on glycemic control and insulin resistance in patients with obstructive sleep apnea: a meta-analysis. Sleep Breath 17:33–38
Iftikhar IH, Khan MF, Das A, Magalang UJ (2013) Meta-analysis: continuous positive airway pressure improves insulin resistance in patients with sleep apnea without diabetes. Ann Am Thorac Soc 10:115–120
Somers VK, Dyken ME, Mark AL, Abboud FM (1993) Sympathetic-nerve activity during sleep in normal subjects. N Engl J Med 328:303–307
Findley LJ, Wilhoit SC, Suratt PM (1985) Apnea duration and hypoxemia during REM sleep in patients with obstructive sleep apnea. Chest 87:432–436
Appleton SL, Vakulin A, Martin SA, Lang CJ, Wittert GA, Taylor AW et al (2016) Hypertension Is Associated With Undiagnosed OSA During Rapid Eye Movement Sleep. Chest 150:495–505
Kendzerska T, Gershon AS, Hawker G, Tomlinson G, Leung RS (2014) Obstructive sleep apnea and incident diabetes A historical cohort study. Am J Respir Crit Care Med 190:218–25
Nishimura A, Kasai T, Kikuno S, Nagasawa K, Okubo M, Narui K et al (2019) Apnea Hypopnea Index During Rapid Eye Movement Sleep With Diabetic Retinopathy in Patients With Type 2 Diabetes. J Clin Endocrinol Metab 104:2075–2082
Acknowledgements
The authors would like to extend their heartfelt appreciation to the individuals who made this research possible. We are particularly grateful to the patients who participated in this study for their invaluable contributions. We also wish to acknowledge the dedicated efforts of the staff at the Sleep Unit of La Paz University Hospital for their assistance in data collection. This research was made possible through the generous support of the Fondo de Investigación Sanitaria (FIS) (Health Research Fund) and the European Regional Development Funds (ERDF) under grant numbers PI16/00201, PI19/01612, and PI22/01262, awarded to F. García-Río. Their financial support was instrumental in advancing this study. Additionally, we want to express our gratitude to all individuals who provided guidance, feedback, and assistance throughout the research process. Your contributions have been indispensable and are deeply appreciated.
Funding
This study was supported by grants from Fondo de Investigación Sanitaria (FIS) (health research fund) and European Regional Development Funds PI16/00201, PI19/01612 and PI22/01262 to F. García-Río.
Author information
Authors and Affiliations
Contributions
FG-R had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. AM-M, RC, EM-C, EZ, and FG-R were responsible for developing the research question. AM-M, RC, BS-S, IF-N, JF-L, RG, EM-C, EZ, and FG-R were responsible for the study design and collection of data. AMM-M, EM-C, EZ, and FG-R were responsible for study management and coordination. AM-M and FG-R drafted the paper. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was conducted in compliance with ethical standards and received approval from La Paz University Hospital-IdiPAZ Drug Research Ethics Committee (Protocol ID: PI-1857). Informed consent was obtained from all study participants in accordance with the principles of the Declaration of Helsinki.
Patient consent
Informed written consent was obtained from all participants included in the study, ensuring their voluntary participation, understanding of the study's objectives, and awareness of data collection procedures. The confidentiality of their personal information was strictly maintained.
Conflict of interest
The authors declare no conflicts of interest that could influence the interpretation of the results or the presentation of information in this manuscript. This study was conducted in an unbiased manner, and there are no financial or personal relationships with organizations or individuals that could potentially affect the research.
Permission to reproduce material from other sources
We have obtained necessary permissions to reproduce material from other sources in this article and duly acknowledge the respective sources in the appropriate sections of the manuscript. Any copyrighted material used has been properly cited and credited.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mangas-Moro, A., Casitas, R., Sánchez-Sánchez, B. et al. Characteristics of obstructive sleep apnea related to insulin resistance. Sleep Breath (2024). https://doi.org/10.1007/s11325-024-03040-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11325-024-03040-1