Abstract
Purpose
The relationship between chronic heart failure and sleep-disordered breathing (SDB) has been frequently described. However, little is known about the association of mitral regurgitation (MR) and SDB or the impact of transcatheter mitral valve repair (TMVR) on SDB. Our aims were first to determine the prevalence of SDB in patients with MR, and second to determine the effect of TMVR on SDB.
Methods
Patients with MR being evaluated for TMVR at the University Hospital Bonn underwent polygraphy (PG) to determine the prevalence of SDB. After TMVR, a subset of patients was followed up with transthoracic echocardiography (TTE) and PG to evaluate the effect of TMVR on SDB.
Results
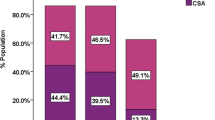
In 53 patients, mean age was 76.0 ± 8.5 years and 62% were male. Patients predominantly had more than moderate mitral regurgitation (94%). SDB was highly prevalent (68%) with predominantly central sleep apnoea (CSA, 67%). After TMVR in 15 patients, the apnoea/hypopnoea index (AHI) and central apnoea index (AI) were significantly reduced among patients with SDB (AHI − 8.0/h, p = 0.021; central AI − 6.9/h, p = 0.046). The left atrial volume index (LAVI) at baseline was significantly higher in patients with CSA than in patients with obstructive sleep apnoea (OSA) and was significantly reduced after TMVR (63.5 ml/m2 ± 27.2 vs. 38.3 ml/m2 ± 13.0; − 18.4 ml/m2, p = 0.027).
Conclusion
SDB, especially CSA, is highly prevalent in patients with mitral regurgitation. In the follow-up cohort TMVR led to a significant reduction of the AHI, predominantly of central events. The findings of the study suggest that TMVR may be a suitable therapy not only for MR but also for the accompanying CSA. LAVI may be a useful indicator for CSA in patients with MR.




Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- AHI:
-
Apnoea/hypopnoea index
- AI:
-
Apnoea index
- AS:
-
Aortic valve stenosis
- CPAP:
-
Continuous positive airway pressure
- CSA:
-
Central sleep apnoea
- ESS:
-
Epworth Sleepiness Scale
- HF:
-
Heart failure
- LAVI:
-
Left atrial volume index
- LVEF:
-
Left ventricular ejection fraction
- MR:
-
Mitral regurgitation
- OSA:
-
Obstructive sleep apnoea
- PG:
-
Cardiorespiratory polygraphy
- SDB:
-
Sleep-disordered breathing
- TMVR:
-
Transcatheter mitral valve repair
- TTE:
-
Transthoracic echocardiography
References
Yoshihisa A, Takeishi Y (2019) Sleep disordered breathing and cardiovascular diseases. J Atheroscler Thromb 26(4):315–327
Parati G, Lombardi C, Castagna F, Mattaliano P, Filardi PP, Agostoni P et al (2016) Heart failure and sleep disorders. Nat Rev Cardiol 13(7):389–403
Khayat R, Pederzoli A, Abraham WT (2009) Central sleep apnea in heart failure 6(2):72–78
Bradley TD, Floras JS (2003) Sleep apnea and heart failure: part II: central sleep apnea. Circulation 107(13):1822–1826
Vazir A, Hastings PC, Dayer M, McIntyre HF, Henein MY, Poole-Wilson PA et al (2007) A high prevalence of sleep disordered breathing in men with mild symptomatic chronic heart failure due to left ventricular systolic dysfunction. Eur J Heart Fail 9(3):243–250
Oldenburg O, Lamp B, Faber L, Teschler H, Horstkotte D, Töpfer V (2007) Sleep-disordered breathing in patients with symptomatic heart failure: a contemporary study of prevalence in and characteristics of 700 patients. Eur J Heart Fail 9(3):251–257
Hanly PJ, Zuberi-Khokhar NS (1996) Increased mortality associated with Cheyne-Stokes respiration in patients with congestive heart failure. Am J Respir Crit Care Med 153(1):272–276
Sinha A-M, Skobel EC, Breithardt O-A, Norra C, Markus KU, Breuer C et al (2004) Cardiac resynchronization therapy improves central sleep apnea and Cheyne-Stokes respiration in patients with chronic heart failure. J Am Coll Cardiol 44(1):68–71
Tamura A, Kawano Y, Kadota J (2009) Carvedilol reduces the severity of central sleep apnea in chronic heart failure. Circ J Off J Jpn Circ Soc 73(2):295–298
Linhart M, Sinning J-M, Ghanem A, Kozhuppakalam FJ, Fistéra R, Hammerstingl C et al (2015) Prevalence and impact of sleep disordered breathing in patients with severe aortic stenosis. PLoS ONE 10(7):e0133176
Linhart M, Pabst S, Fistéra R, Ghanem A, Hammerstingl C, Kozhuppakalam F et al (2013) Transcatheter valve implantation improves central sleep apnoea in severe aortic stenosis. EuroIntervention 9(8):923–928
Prendergast B, Vahanian A (2022) The 2021 ESC/EACTS guidelines for the management of valvular heart disease: a new template for Heart Teams and their patients. Cardiovasc Res 118(1):e11–e13
Feldman T, Wasserman HS, Herrmann HC, Gray W, Block PC, Whitlow P et al (2005) Percutaneous mitral valve repair using the edge-to-edge technique. J Am Coll Cardiol 46(11):2134–2140
Giallauria F, Di Lorenzo A, Parlato A, Testa C, Bobbio E, Vigorito C et al (2020) Individual patient data meta-analysis of the effects of the CARILLON® mitral contour system. ESC Heart Fail 7(6):3383–3391
Khan MS, Siddiqi TJ, Butler J, Friede T, Levy WC, Witte KK et al (2021) Functional outcomes with Carillon device over 1 year in patients with functional mitral regurgitation of Grades 2+ to 4+: results from the REDUCE-FMR trial. ESC Heart Fail 8(2):872–878
Nickenig G, Hammerstingl C, Schueler R, Topilsky Y, Grayburn PA, Vahanian A et al (2016) Transcatheter mitral annuloplasty in chronic functional mitral regurgitation. JACC Cardiovasc Interv 9(19):2039–2047
Maisano F, Taramasso M, Nickenig G, Hammerstingl C, Vahanian A, Messika-Zeitoun D et al (2016) Cardioband, a transcatheter surgical-like direct mitral valve annuloplasty system: early results of the feasibility trial. Eur Heart J 37(10):817–825
Goliasch G, Bartko PE, Pavo N, Neuhold S, Wurm R, Mascherbauer J et al (2018) Refining the prognostic impact of functional mitral regurgitation in chronic heart failure. Eur Heart J 39(1):39–46
Nickenig G, Estevez-Loureiro R, Franzen O, Tamburino C, Vanderheyden M, Lüscher TF et al (2014) Percutaneous mitral valve edge-to-edge repair: in-hospital results and 1-year follow-up of 628 patients of the 2011–2012 Pilot European Sentinel Registry. J Am Coll Cardiol 64(9):875–884
Kapur VK, Auckley DH, Chowdhuri S, Kuhlmann DC, Mehra R, Ramar K et al (2017) Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine Clinical Practice Guideline. J Clin Sleep Med 13(03):479–504
Riemann D, Baum E, Cohrs S, Crönlein T, Hajak G, Hertenstein E et al (2017) S3-Leitlinie Nicht erholsamer Schlaf/Schlafstörungen: Kapitel „Insomnie bei Erwachsenen“ (AWMF-Registernummer 063–003), Update 2016. Somnologie 21(1):2–44
Bloch KE, Schoch OD, Zhang JN, Russi EW (1999) German version of the Epworth Sleepiness Scale. Respir Int Rev Thorac Dis 66(5):440–447
Lancellotti P, Tribouilloy C, Hagendorff A, Popescu BA, Edvardsen T, Pierard LA et al (2013) Recommendations for the echocardiographic assessment of native valvular regurgitation: an executive summary from the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 14(7):611–644
Mehra R, Redline S (2014) Arrhythmia risk associated with sleep disordered breathing in chronic heart failure. Curr Heart Fail Rep 11(1):88–97
Linz D, Baumert M, Desteghe L, Kadhim K, Vernooy K, Kalman JM et al (2019) Nightly sleep apnea severity in patients with atrial fibrillation: potential applications of long-term sleep apnea monitoring. Int J Cardiol Heart Vasc 24:100424
Ding N, Ni B-Q, Zhang X-L, Huang H-P, Su M, Zhang S-J et al (2013) Prevalence and risk factors of sleep disordered breathing in patients with rheumatic valvular heart disease. J Clin Sleep Med JCSM Off Publ Am Acad Sleep Med 9(8):781–787
Spiesshoefer J, Spieker M, Klose S, Keymel S, Boentert M, Krüger S et al (2019) Reduction of sleep-disordered breathing following effective percutaneous mitral valve repair with the MitraClip system. Sleep Breath Schlaf Atm 23(3):815–824
Gerçek M, Oldenburg O, Gerçek M, Fox H, Rudolph V, Puehler T et al (2021) Prevalence of sleep disordered breathing in patients with primary mitral regurgitation undergoing mitral valve surgery. J Clin Med 10(9):2039
Daher A, Müller T, Marx N, Schröder J, Almalla M, Keszei AP et al (2021) Effects of transcatheter mitral valve repair using MitraClip® device on sleep disordered breathing in patients with mitral valve regurgitation. J Clin Med 10(15):3332
Cowie MR, Woehrle H, Wegscheider K, Angermann C, d’Ortho M-P, Erdmann E et al (2015) Adaptive servo-ventilation for central sleep apnea in systolic heart failure. N Engl J Med 373(12):1095–1105
Abe H, Takahashi M, Yaegashi H, Eda S, Kitahara H, Tsunemoto H et al (2009) Valve repair improves central sleep apnea in heart failure patients with valvular heart diseases. Circ J Off J Jpn Circ Soc 73(11):2148–2153
Calvin AD, Somers VK, Johnson BD, Scott CG, Olson LJ (2014) Left atrial size, chemosensitivity, and central sleep apnea in heart failure. Chest 146(1):96–103
Acknowledgements
We thank Mrs. Karin Springmann for her support in the sleep study laboratory of the University Hospital of Bonn, Germany.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The research was conducted according to the principles of the Declaration of Helsinki. Written informed consent was obtained from all subjects. The study was approved by the local ethics committee (Ethics committee of the Medical Faculty, Rheinische Friedrich-Wilhelms-Universität Bonn).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Biener, L., Vogelhuber, J., Alboany, H. et al. Prevalence of sleep-disordered breathing in patients with mitral regurgitation and the effect of mitral valve repair. Sleep Breath 27, 599–610 (2023). https://doi.org/10.1007/s11325-022-02667-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-022-02667-2