Abstract
Background
The success of various therapy methods in the treatment of insomnia and poor quality sleep, both of which play an active role in the chronicization process of migraine, has been the subject of investigation. The aim of this research was to evaluate the success, acceptability, and efficacy of greater occipital nerve block (GON-B) therapy in chronic migraine (CM) patients in improving their sleep quality and developing their beliefs about sleep .
Methods
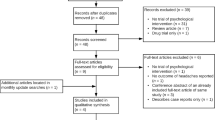
The study included 40 patients with CM from the general population who agreed to receive blockade therapy. Before the injection treatment, 1-week sleep diaries as well as depression and anxiety symptoms were examined. The Pittsburgh Sleep Quality Index (PSQI), Insomnia Severity Index (ISI), Pre-Sleep Arousal Scale (PSAS), Epworth Sleepiness Scale (ESS), and Dysfunctional Beliefs and Attitudes about Sleep (DBAS) scales were measured and evaluated both before and after the completion of 3 months of treatment.
Results
Thirty-seven patients with CM successfully completed our 12-week treatment period. The anxiety and depression scales of the patients decreased after 3 months (p < 0.001). PSQI and its subgroups ratings significantly improved after treatment (p < 0.001). Similarly, ISI, ESS, PSAS, and DBAS test scores also improved after treatment (p < 0.001).
Conclusions
This study provides evidence as to the applicability and acceptability of GON-B in CM treatment in terms of increased sleep quality; improved sleep beliefs, attitudes, and behaviors; and arousals and decreased insomnia findings.
Similar content being viewed by others
Abbreviations
- CM:
-
Chronic migraine
- DBAS:
-
Dysfunctional Beliefs and Attitudes about Sleep
- ESS:
-
Epworth Sleepiness Scale
- GON-B:
-
Greater occipital nerve block
- ISI:
-
Insomnia Severity Index
- PSAS:
-
Pre-sleep arousal scale
- PSQI:
-
Pittsburgh Sleep Quality Index
References
Arnold M (2018) Headache classification committee of the international headache society (IHS) the international classification of headache disorders. Cephalalgia 38(1):1–211
Natoli, J., et al., Global prevalence of chronic migraine: a systematic review. Cephalalgia, 2009: p. no-no.
Borkum JM (2018) Harnessing migraines for neural regeneration. Neural Regen Res 13(4):609–615
Buse DC, Greisman JD, Baigi K, Lipton RB (2019) Migraine progression: a systematic review. Headache 59(3):306–338
Andreou AP, Edvinsson L (2019) Mechanisms of migraine as a chronic evolutive condition. J Headache Pain 20(1):117
Schoonman, G.G., H.W. Schytz, and M. Ashina, Migraine trigger factors. Oxford Textbook of Headache Syndromes, 2020: p. 67.
Boardman HF, Thomas E, Millson DS, Croft PR (2005) Psychological, sleep, lifestyle, and comorbid associations with headache. Headache 45(6):657–669
Irish LA, Kline CE, Gunn HE, Buysse DJ, Hall MH (2015) The role of sleep hygiene in promoting public health: a review of empirical evidence. Sleep Med Rev 22:23–36
Karacan I, Thornby JI, Anch AM, Booth GH, Williams RL, Salis PJ (1976) Dose-related sleep disturbances induced by coffee and caffeine. Clin Pharmacol Ther 20(6):682–689
Ong JJY, De Felice M (2018) Migraine treatment: current acute medications and their potential mechanisms of action. Neurotherapeutics 15(2):274–290
Vagharseyyedin SA, Salmabadi M, BahramiTaghanaki H, Riyasi H (2019) The impact of self-administered acupressure on sleep quality and fatigue among patients with migraine: a randomized controlled trial. Complement Ther Clin Pract 35:374–380
Blumenfeld A, Ashkenazi A, Grosberg B, Napchan U, Narouze S, Nett B, DePalma T, Rosenthal B, Tepper S, Lipton RB (2010) Patterns of use of peripheral nerve blocks and trigger point injections among headache practitioners in the USA: results of the American Headache Society Interventional Procedure Survey (AHS-IPS). Headache 50(6):937–942
Ashkenazi A, Blumenfeld A, Napchan U, Narouze S, Grosberg B, Nett R, DePalma T, Rosenthal B, Tepper S, Lipton RB (2010) Peripheral nerve blocks and trigger point injections in headache management–a systematic review and suggestions for future research. Headache 50(6):943–952
Ashkenazi A, Young WB (2005) The effects of greater occipital nerve block and trigger point injection on brush allodynia and pain in migraine. Headache 45(4):350–354
Blumenfeld A, Ashkenazi A, Napchan U, Bender SD, Klein BC, Berliner R, Ailani J, Schim J, Friedman DI, Charleston L IV, Young WB, Robertson CE, Dodick DW, Silberstein SD, Robbins MS (2013) Expert consensus recommendations for the performance of peripheral nerve blocks for headaches–a narrative review. Headache 53(3):437–446
Inan N, Inan LE, Coskun O, Tunc T, Ilhan M (2016) Effectiveness of greater occipital nerve blocks in migraine prophylaxis. Noro Psikiyatr Ars 53(1):45–48
Ünal-Artık HA, İnan LE, Ataç-Uçar C, Yoldaş TK (2017) Do bilateral and unilateral greater occipital nerve block effectiveness differ in chronic migraine patients? Neurol Sci 38(6):949–954
Buysse DJ, Reynolds CF III, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28(2):193–213
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Morin CM, Stone J, Trinkle D, Mercer J, Remsberg S (1993) Dysfunctional beliefs and attitudes about sleep among older adults with and without insomnia complaints. Psychol Aging 8(3):463–467
Edinger JD, Wohlgemuth WK, Radtke RA, Marsh GR, Quillian RE (2001) Does cognitive-behavioral insomnia therapy alter dysfunctional beliefs about sleep? Sleep 24(5):591–599
Bastien CH, Vallieres A, Morin CM (2001) Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med 2(4):297–307
Nicassio PM, Mendlowitz DR, Fussell JJ, Petras L (1985) The phenomenology of the pre-sleep state: the development of the pre-sleep arousal scale. Behav Res Ther 23(3):263–271
Beck AT, Steer RA, Carbin MG (1988) Psychometric properties of the Beck Depression Inventory: twenty-five years of evaluation. Clin Psychol Rev 8(1):77–100
Beck AT, Epstein N, Brown G, Steer RA (1988) An inventory for measuring clinical anxiety: psychometric properties. J Consult Clin Psychol 56(6):893–897
Inan LE, Inan N, Unal-Artık HA, Atac C, Babaoglu G (2019) Greater occipital nerve block in migraine prophylaxis: narrative review. Cephalalgia 39(7):908–920
Inan L et al (2015) Greater occipital nerve blockade for the treatment of chronic migraine: a randomized, multicenter, double-blind, and placebo-controlled study. Acta Neurol Scand 132(4):270–277
Young WB (2010) Blocking the greater occipital nerve: utility in headache management. Curr Pain Headache Rep 14(5):404–408
Bigal ME, Lipton RB (2008) Clinical course in migraine: conceptualizing migraine transformation. Neurology 71(11):848–855
Cooke L, Eliasziw M, Becker WJ (2007) Cutaneous allodynia in transformed migraine patients. Headache 47(4):531–539
Mathew NT, Reuveni U, Perez F (1987) Transformed or evolutive migraine. Headache 27(2):102–106
Andreou AP, Edvinsson L (2019) Mechanisms of migraine as a chronic evolutive condition. J Headache Pain 20(1):1–17
Alstadhaug K (2009) Migraine and the hypothalamus. Cephalalgia 29(8):809–817
Shauly O, Gould DJ, Sahai-Srivastava S, Patel KM (2019) Greater occipital nerve block for the treatment of chronic migraine headaches: a systematic review and meta-analysis. Plast Reconstr Surg 144(4):943–952
Cooper, W.M. and A.K. Masih, Cervicogenic headache, in Headache and Migraine Biology and Management. 2015, Elsevier. p. 203-212.
Yilmaz V, Aras B, Erturk FA, Cakcı FA, Umay E (2019) Migraine in patients with fibromyalgia and outcomes of greater occipital nerve blockage. Clin Neurol Neurosurg 181:54–57
Flamer D, Alakkad H, Soneji N, Tumber P, Peng P, Kara J, Hoydonckx Y, Bhatia A (2019) Comparison of two ultrasound-guided techniques for greater occipital nerve injections in chronic migraine: a double-blind, randomized, controlled trial. Reg Anesth Pain Med 44(5):595–603
Ulusoy EK, Bolatturk OF (2020) The effect of greater occipital nerve blockade on the quality of life, disability and comorbid depression, anxiety, and sleep disturbance in patients with chronic migraine. Neurol Sci 41:1829–1835
Morin CM, Vallières A, Ivers H (2007) Dysfunctional beliefs and attitudes about sleep (DBAS): validation of a brief version (DBAS-16). Sleep 30(11):1547–1554
Kloss JD, Nash CO, Walsh CM, Culnan E, Horsey S, Sexton-Radek K (2016) A “Sleep 101” program for college students improves sleep hygiene knowledge and reduces maladaptive beliefs about sleep. Behav Med 42(1):48–56
Crawford MR, Luik AI, Espie CA, Taylor HL, Burgess HJ, Jones AL, Rush University Sleep Research Team, Ong JC (2020) Digital cognitive behavioral therapy for insomnia in women with chronic migraines. Headache 60:902–915
Cox RC, Olatunji BO (2016) A systematic review of sleep disturbance in anxiety and related disorders. J Anxiety Disord 37:104–129
Song Z et al (2009) Pain relief by spinal cord stimulation involves serotonergic mechanisms: an experimental study in a rat model of mononeuropathy. Pain 147(1-3):241–248
Vgontzas A, Pavlovic JM (2018) Sleep disorders and migraine: review of literature and potential pathophysiology mechanisms. Headache 58(7):1030–1039
Author information
Authors and Affiliations
Contributions
Hikmet Saçmacı: Concept, blockade therapy, wrote the initial manuscript, acquisition of data, and review of manuscript. Tülin Aktürk: blockade therapy, patient monitoring, and review of manuscript. Nermin Tanık: blockade therapy and review of manuscript. Levent Ertuğrul İnan: Concept, initiation, and critical revision of manuscript.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study protocol was approved by the Local Ethics Committee
Informed consent
Informed consent was obtained from all individual participants included in the study
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Saçmacı, H., Aktürk, T., Tanık, N. et al. Clinical success of greater occipital nerve blockade in improving sleep quality of chronic migraineurs: a prospective observational study. Sleep Breath 25, 1003–1010 (2021). https://doi.org/10.1007/s11325-021-02309-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-021-02309-z