Abstract
Purpose
A comparison of all scoring systems used for screening for obstructive sleep apnea-hypopnea syndrome (OSAHS) is lacking. The aim of this investigation was to evaluate the performance of five scoring systems for screening for OSAHS, as well as to validate the use of the NoSAS and SACS in the Chinese population.
Methods
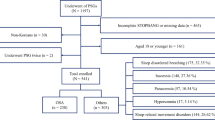
Data were retrospectively collected from hospital-based, manned, overnight sleep monitoring studies for 105 consecutive outpatients using a portable monitor (PM) device.
Results
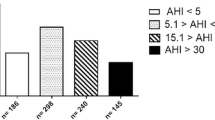
The 105 participants had an average age of 46 years and were mostly men (75%). STOP-Bang, SACS, and NoSAS scoring exhibited moderate predictive values at different AHI cutoffs (AUC 0.761–0.853, 0.722–0.854, and 0.724–0.771 respectively), followed by the STOP and Berlin questionnaire (AUC 0.680–0.781vs 0.624–0.724). Both STOP-Bang and SACS showed excellent sensitivity (89.5–100% vs 93.4–94.6%) and negative predictive value (68–100% vs 77.3–90.9%), while STOP-Bang, STOP, and SACS showed low negative likelihood ratios (− LR) (0–0.2).
Conclusions
Our study indicated that the STOP-Bang questionnaire and the SACS both show better predictive value than other scoring systems among the five screening tools for OSAHS. Both scoring systems are simple and easy to implement for screening for OSAHS in the community and in hospitals.



Similar content being viewed by others
Data Availability
The data supporting the findings of the article is available from the corresponding author by request. Statistical analyses were performed using SPSS v25.0 and GraphPad Prism v8.0.2.
References
Malhotra RK, Kirsch DB, Kristo DA, Olson EJ, Aurora RN, Carden KA, Chervin RD, Martin JL, Ramar K, Rosen CL, Rowley JA, Rosen IM (2018) Polysomnography for obstructive Sleep apnea should include arousal-based scoring: an American Academy of Sleep Medicine position statement. J Clin Sleep Med 14(7):1245–1247. https://doi.org/10.5664/jcsm.7234
Tan A, Hong Y, Tan L, van Dam RM, Cheung YY, Lee CH (2017) Validation of NoSAS score for screening of sleep-disordered breathing in a multiethnic Asian population. Sleep Breath 21(4):1033–1038. https://doi.org/10.1007/s11325-016-1455-4
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365(9464):1046–1053. https://doi.org/10.1016/S0140-6736(05)71141-7
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342(19):1378–1384. https://doi.org/10.1056/NEJM200005113421901
Kendzerska T, Gershon AS, Hawker G, Tomlinson G, Leung RS (2014) Obstructive sleep apnea and incident diabetes. A historical cohort study. Am J Respir Crit Care Med 190(2):218–225. https://doi.org/10.1164/rccm.201312-2209OC
Vaessen TJ, Overeem S, Sitskoorn MM (2015) Cognitive complaints in obstructive sleep apnea. Sleep Med Rev 19:51–58. https://doi.org/10.1016/j.smrv.2014.03.008
Teran-Santos J, Jimenez-Gomez A, Cordero-Guevara J (1999) The association between sleep apnea and the risk of traffic accidents. Cooperative Group Burgos-Santander. N Engl J Med 340(11):847–851. https://doi.org/10.1056/NEJM199903183401104
Watson NF (2016) Health care savings: the economic value of diagnostic and therapeutic care for obstructive sleep apnea. J Clin Sleep Med 12(8):1075–1077. https://doi.org/10.5664/jcsm.6034
Chung F, Yegneswaran B, Liao P, Chung SA, Vairavanathan S, Islam S, Khajehdehi A, Shapiro CM (2008) STOP questionnaire: a tool to screen patients for obstructive sleep apnea. Anesthesiology 108(5):812–821. https://doi.org/10.1097/ALN.0b013e31816d83e4
Dias RA, Hardin KA, Rose H, Agius MA, Apperson ML, Brass SD (2012) Sleepiness, fatigue, and risk of obstructive sleep apnea using the STOP-BANG questionnaire in multiple sclerosis: a pilot study. Sleep Breath 16(4):1255–1265. https://doi.org/10.1007/s11325-011-0642-6
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP (1999) Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 131(7):485–491. https://doi.org/10.7326/0003-4819-131-7-199910050-00002
Gali B, Whalen FX, Schroeder DR, Gay PC, Plevak DJ (2009) Identification of patients at risk for postoperative respiratory complications using a preoperative obstructive sleep apnea screening tool and postanesthesia care assessment. Anesthesiology 110(4):869–877. https://doi.org/10.1097/ALN.0b013e31819b5d70
Marti-Soler H, Hirotsu C, Marques-Vidal P, Vollenweider P, Waeber G, Preisig M, Tafti M, Tufik SB, Bittencourt L, Tufik S, Haba-Rubio J, Heinzer R (2016) The NoSAS score for screening of sleep-disordered breathing: a derivation and validation study. Lancet Respir Med 4(9):742–748. https://doi.org/10.1016/S2213-2600(16)30075-3
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545. https://doi.org/10.1093/sleep/14.6.540
Zhang JN, Peng B, Zhao TT, Xiang M, Fu W, Peng Y (2011) Modification of the Epworth sleepiness scale in Central China. Qual Life Res 20(10):1721–1726. https://doi.org/10.1007/s11136-011-9898-3
Buysse DJ, Reynolds CR, Monk TH, Berman SR, Kupfer DJ (1989) The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28(2):193–213. https://doi.org/10.1016/0165-1781(89)90047-4
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson WS, Tangredi MM (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8(5):597–619. https://doi.org/10.5664/jcsm.2172
Pereira EJ, Driver HS, Stewart SC, Fitzpatrick MF (2013) Comparing a combination of validated questionnaires and level III portable monitor with polysomnography to diagnose and exclude sleep apnea. J Clin Sleep Med 9(12):1259–1266. https://doi.org/10.5664/jcsm.3264
Rowley JA, Aboussouan LS, Badr MS (2000) The use of clinical prediction formulas in the evaluation of obstructive sleep apnea. Sleep 23(7):929–938. https://doi.org/10.1093/sleep/23.7.929
Flemons WW, Whitelaw WA, Brant R, Remmers JE (1994) Likelihood ratios for a sleep apnea clinical prediction rule. Am J Respir Crit Care Med 150(5 Pt 1):1279–1285. https://doi.org/10.1164/ajrccm.150.5.7952553
Chung F, Yegneswaran B, Liao P, Chung SA, Vairavanathan S, Islam S, Khajehdehi A, Shapiro CM (2008) Validation of the Berlin questionnaire and American Society of Anesthesiologists checklist as screening tools for obstructive sleep apnea in surgical patients. Anesthesiology 108(5):822–830. https://doi.org/10.1097/ALN.0b013e31816d91b5
Ahmadi N, Chung SA, Gibbs A, Shapiro CM (2008) The Berlin questionnaire for sleep apnea in a sleep clinic population: relationship to polysomnographic measurement of respiratory disturbance. Sleep Breath 12(1):39–45. https://doi.org/10.1007/s11325-007-0125-y
Blackman A, McGregor C, Dales R, Driver HS, Dumov I, Fleming J, Fraser K, George C, Khullar A, Mink J, Moffat M, Sullivan GE, Fleetham JA, Ayas N, Bradley TD, Fitzpatrick M, Kimoff J, Morrison D, Ryan F, Skomro R, Series F, Tsai W (2010) Canadian Sleep Society/Canadian Thoracic Society position paper on the use of portable monitoring for the diagnosis of obstructive sleep apnea/hypopnea in adults. Can Respir J 17(5):229–232. https://doi.org/10.1155/2010/923718
Vat S, Haba-Rubio J, Tafti M, Tobback N, Andries D, Heinzer R (2015) Scoring criteria for portable monitor recordings: a comparison of four hypopnoea definitions in a population-based cohort. Thorax 70(11):1047–1053. https://doi.org/10.1136/thoraxjnl-2014-205982
Collop NA, Anderson WM, Boehlecke B, Claman D, Goldberg R, Gottlieb DJ, Hudgel D, Sateia M, Schwab R (2007) Clinical guidelines for the use of unattended portable monitors in the diagnosis of obstructive sleep apnea in adult patients. Portable Monitoring Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 3(7):737–747
Collop NA, Tracy SL, Kapur V, Mehra R, Kuhlmann D, Fleishman SA, Ojile JM (2011) Obstructive sleep apnea devices for out-of-center (OOC) testing: technology evaluation. J Clin Sleep Med 7(5):531–548. https://doi.org/10.5664/JCSM.1328
Parra O, Garcia-Esclasans N, Montserrat JM, Garcia EL, Ruiz J, Lopez JA, Guerra JM, Sopena JJ (1997) Should patients with sleep apnoea/hypopnoea syndrome be diagnosed and managed on the basis of home sleep studies? Eur Respir J 10(8):1720–1724. https://doi.org/10.1183/09031936.97.10081720
Driver HS, Pereira EJ, Bjerring K, Toop F, Stewart SC, Munt PW, Fitzpatrick MF (2011) Validation of the MediByte(R) type 3 portable monitor compared with polysomnography for screening of obstructive sleep apnea. Can Respir J 18(3):137–143. https://doi.org/10.1155/2011/760958
Masa JF, Corral J, Pereira R, Duran-Cantolla J, Cabello M, Hernandez-Blasco L, Monasterio C, Alonso A, Chiner E, Zamorano J, Aizpuru F, Montserrat JM (2011) Therapeutic decision-making for sleep apnea and hypopnea syndrome using home respiratory polygraphy: a large multicentric study. Am J Respir Crit Care Med 184(8):964–971. https://doi.org/10.1164/rccm.201103-0428OC
Acknowledgments
We thank the international research fund of Philips-Respironics for supporting us with portable sleep monitoring devices.
Author information
Authors and Affiliations
Contributions
Jinnong Zhang, Wenjing Wang, and Wei Peng conceived and designed the study. Jinnong Zhang supervised the overall study. Shan Yuan collected sleep data. Haiying Zheng and Tianci Yao conducted sleep test and questionnaire survey. Wenjing Wang analyzed the data. Jinnong Zhang and Wenjing Wang wrote the manuscript. Jinnong Zhang, Wenjing Wang, and Jehane Michael Le Grange revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the Medical Ethics Committee of Tongji Medical College, Huazhong University of Science and Technology and performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. Written informed consent was waived by the Medical Ethics Committee.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, W., Yuan, S., Le Grange, J. et al. Evaluating the performance of five scoring systems for prescreening obstructive sleep apnea-hypopnea syndrome. Sleep Breath 25, 1685–1692 (2021). https://doi.org/10.1007/s11325-020-02227-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02227-6