Abstract
Purpose
The effect of nocturnal wear of denture on sleep quality and integrity is still not well understood. Therefore, this systematic review was conducted to provide evidence on this topic.
Methods
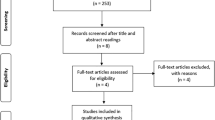
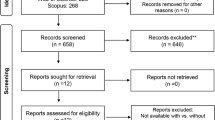
Electronic searches were conducted from 1964 up to September 2015, using MEDLINE, EMBASE, and the Cochrane Central Register of Controlled Trials. Only publications in English or French, in which sleep quality of edentate adult individuals wearing dentures at night was compared to those not wearing were included in the review. Random effects models were used to pool the effect sizes.
Results
A total of 10 studies were included in the systematic review and 5 in the meta-analysis. No statistically significant difference between sleeping with denture and without denture was found for the Apnea-Hypopnea Index (AHI; Standard Mean Difference = −0.60, 95 % CI −1.67–0.47; Z = −1.10; p = 0.27). However, there was considerable heterogeneity in the studies included in the meta-analysis (Tau2 = 1.34; Q-value = 59.32, df = 4 (P < 0.0001); I2 = 93.3 %). When results from randomized controlled trials (RCTs) were pooled in subgroup analyses of AHI, there was a tendency towards favoring sleeping without dentures (P = 0.059) and no evidence of heterogeneity between studies (Tau2 = 0.000; Q-value = 0.06, df = 1 (P = 0.80); I2 = 0.000 %).
Conclusion
The current evidence suggests that there is no difference in the sleep quality and integrity of individuals wearing or not wearing their denture during sleep. However, the results of randomized controlled trials favoring sleeping without dentures and the likely presence of bias in the previous studies indicate the need for further randomized controlled trials for the development of clinical guideline.



Similar content being viewed by others
References
Ohayon MM (2007) Prevalence and comorbidity of sleep disorders in general population. La Revue du praticien 57(14):1521–1528
Vaz Fragoso CA, Gill TM (2007) Sleep complaints in community-living older persons: a multifactorial geriatric syndrome. J Am Geriatr Soc 55(11):1853–1866. doi:10.1111/j.1532-5415.2007.01399.x
Bucca C, Carossa S, Pivetti S, Gai V, Rolla G, Preti G (1999) Edentulism and worsening of obstructive sleep apnoea. Lancet 353(9147):121–122
Cinar AB, Oktay I, Schou L (2013) Relationship between oral health, diabetes management and sleep apnea. Clin Oral Investig 17(3):967–974. doi:10.1007/s00784-012-0760-y
Hansen CA, Axinn S (1984) Incidence of mandibular dysfunction symptoms in individuals who remove their complete dentures during sleep. J Prosthet Dent 51(1):16–18
Bucca C, Cicolin A, Brussino L, Arienti A, Graziano A, Erovigni F, Pera P, Gai V, Mutani R, Preti G, Rolla G, Carossa S (2006) Tooth loss and obstructive sleep apnoea. Respir Res 7:8
Endeshaw YW, Katz S, Ouslander JG, Bliwise DL (2004) Association of denture use with sleep-disordered breathing among older adults. J Public Health Dent 64(3):181–183
Chokroverty S (2010) Overview of sleep & sleep disorders. Indian J Med Res 131:126–140
Neikrug AB, Ancoli-Israel S (2010) Sleep disorders in the older adult—a mini-review. Gerontology 56(2):181–189. doi:10.1159/000236900
Roepke SK, Ancoli-Israel S (2010) Sleep disorders in the elderly. Indian J Med Res 131:302–310
Crowley K (2011) Sleep and sleep disorders in older adults. Neuropsychol Rev 21(1):41–53. doi:10.1007/s11065-010-9154-6
Ivanhoe JR, Cibirka RM, Lefebvre CA, Parr GR (1999) Dental considerations in upper airway sleep disorders: a review of the literature. J Prosthet Dent 82(6):685–698
Ancoli-Israel S, Kripke DF (1991) Prevalent sleep problems in the aged. Biofeedback Self Regul 16(4):349–359
Marcus PA, Joshi A, Jones JA, Morgano SM (1996) Complete edentulism and denture use for elders in New England. J Prosthet Dent 76(3):260–266
Sumi Y, Miura H, Michiwaki Y, Nagaosa S, Nagaya M (2007) Colonization of dental plaque by respiratory pathogens in dependent elderly. Arch Gerontol Geriatr 44(2):119–124. doi:10.1016/j.archger.2006.04.004
Wilson J (1998) The aetiology, diagnosis and management of denture stomatitis. Br Dent J 185(8):380–384. doi:10.1038/sj.bdj.4809821
Compagnoni MA, Souza RF, Marra J, Pero AC, Barbosa DB (2007) Relationship between Candida and nocturnal denture wear: quantitative study. J Oral Rehabil 34(8):600–605. doi:10.1111/j.1365-2842.2007.01754.x
Emami E, de Grandmont P, Rompre PH, Barbeau J, Pan S, Feine JS (2008) Favoring trauma as an etiological factor in denture stomatitis. J Dent Res 87(5):440–444
Divaris K, Ntounis A, Marinis A, Polyzois G, Polychronopoulou A (2012) Loss of natural dentition: multi-level effects among a geriatric population. Gerodontology 29(2):e192–e199. doi:10.1111/j.1741-2358.2010.00440.x
Zomorodian K, Haghighi NN, Rajaee N, Pakshir K, Tarazooie B, Vojdani M, Sedaghat F, Vosoghi M (2011) Assessment of Candida species colonization and denture-related stomatitis in complete denture wearers. Med Mycol 49(2):208–211. doi:10.3109/13693786.2010.507605
Iinuma T, Arai Y, Abe Y, Takayama M, Fukumoto M, Fukui Y, Iwase T, Takebayashi T, Hirose N, Gionhaku N, Komiyama K (2015) Denture wearing during sleep doubles the risk of pneumonia in the very elderly. J Dent Res 94(3 Suppl):28S–36S. doi:10.1177/0022034514552493
Muller F (2015) Oral hygiene reduces the mortality from aspiration pneumonia in frail elders. J Dent Res 94(3 Suppl):14S–16S. doi:10.1177/0022034514552494
Heydecke G, Penrod JR, Takanashi Y, Lund JP, Feine JS, Thomason JM (2005) Cost-effectiveness of mandibular two-implant overdentures and conventional dentures in the edentulous elderly. J Dent Res 84(9):794–799
Gupta P, Thombare R, Pakhan AJ, Singhal S (2011) Cephalometric evaluation of the effect of complete dentures on retropharyngeal space and its effect on spirometric values in altered vertical dimension. ISRN Dent 2011:516969. doi:10.5402/2011/516969
Erovigni F, Graziano A, Ceruti P, Gassino G, De Lillo A, Carossa S (2005) Cephalometric evaluation of the upper airway in patients with complete dentures. Minerva Stomatol 54(5):293–301
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1. doi:10.1186/2046-4053-4-1
OCEBM Levels of Evidence Working Group The Oxford Levels of Evidence 2. http://www.cebm.net/index.aspx?o=5653.
Higgins J, Green S (2011) Cochrane Handbook for systematic reviews of interventions version 5.1.0 [updated March 2011], vol Version 5.1.0. The Cochrane Collaboration.
Emami E, Lavigne G, de Grandmont P, Rompre PH, Feine JS (2012) Perceived sleep quality among edentulous elders. Gerodontology 29(2):e128–e134. doi:10.1111/j.1741-2358.2010.00426.x
Emami E, Salah MH, Rompre P, Huynh N, Beauchamp A, Feine JS (2013) The nocturnal use of complete dentures and sleep stability in edentulous elders. J Dent 41(8):703–709. doi:10.1016/j.jdent.2013.05.017
Almeida FR, Furuyama RJ, Chaccur DC, Lowe AA, Chen H, Bittencourt LR, Frigeiro ML, Tsuda H (2012) Complete denture wear during sleep in elderly sleep apnea patients—a preliminary study. Sleep & breathing = Schlaf & Atmung 16(3):855–863. doi:10.1007/s11325-011-0587-9
Chaccur DCBL, Lucchesi L, Almeida F, Fróes TC, Furuyama RJ, Frigeiro MLMA (2012) Assessment of the impact of vertical dimension alterations on the quality of sleep in elderly patients wearing upper and lower full dentures. Sleep Sci 5:1–6
Arisaka H, Sakuraba S, Tamaki K, Watanabe T, Takeda J, Yoshida K (2009) Effects of wearing complete dentures during sleep on the apnea-hypopnea index. Int J Prosthodont 22(2):173–177
Gassino G, Cicolin A, Erovigni F, Carossa S, Preti G (2005) Obstructive sleep apnea, depression, and oral status in elderly occupants of residential homes. Int J Prosthodont 18(4):316–322
Tsuda H, Almeida FR, Walton JN, Lowe AA (2010) Questionnaire-based study on sleep-disordered breathing among edentulous subjects in a university oral health center. Int J Prosthodont 23(6):503–506
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. doi:10.1136/bmj.327.7414.557
Borenstein MLVH, Higgins JPT, Rothstein HR (2009) Introduction to meta-analysis. doi:10.1002/9780470743386.
Acknowledgments
The authors would like to gratefully acknowledge the help of M. Patrice Dupont, librarian at the Université de Montréal, for the design of the search strategy.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Dr. Emami holds a CIHR Clinician-Scientist award and funds for new investigators from the Fonds de Recherche du Québec-Santé (FRQ-S). Dr. Huynh holds funds for new investigators from the FRQ-S. Dr. Huy Phan The Nguyen received scholarships from the Agence Universitaire de la Francophonie and the Université de Montréal. This systematic review and meta-analysis is based on the randomized controlled trial that is being conducted by this research group and supported from the Canadian Institutes of Health Research (Funding reference number #134,135). The sponsor had no role in the design or conduct of this research.
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Emami, E., Nguyen, H.P.T., Rompré, P. et al. The effect of nocturnal wear of dentures on the sleep quality: a systematic review and meta-analysis. Sleep Breath 21, 9–18 (2017). https://doi.org/10.1007/s11325-016-1369-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-016-1369-1