Abstract
Purpose
Obstructive sleep apnea (OSA) has been implicated in complications of cardiovascular disease, including arrhythmias and sudden cardiac death (SCD). Prolonged QT interval is associated with arrhythmias and SCD in patients with cardiovascular disease and apparently healthy humans. Apneic episodes during sleep in OSA patients are associated with QT prolongation due to increased vagal activity, but it is not understood whether chronic QT prolongation persists during normoxic daytime wakefulness.
Methods
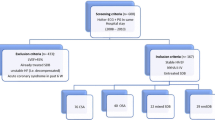
To determine whether daytime QT intervals in OSA patients are prolonged compared to control subjects, we recruited 97 (76 male, 21 female) newly diagnosed patients with OSA [apnea-hypopnea index (AHI) ≥5 events/h] and 168 (100 male, 68 female) healthy volunteers (AHI <5 events/h) and measured daytime resting QT and RR intervals from the electrocardiograms to determine QT prolongation corrected for heart rate (QTc).
Results
All subjects with OSA were older and heavier, with increased heart rate, significantly increased AHI and arousal index, and reduced oxygen saturation (SpO2) during sleep, and spent less time in sleep with >90 % SpO2 compared to respective controls. QTc in patients with OSA (410 ± 3.3 for male and 433 ± 5.6 for female) was significantly increased compared to respective control groups (399 ± 2.9 for male and 417 ± 2.9 for female), after adjustment for age and body mass index.
Conclusions
Our data show that OSA in either men or women is associated with a significant increase in resting daytime QTc. The propensity for ventricular arrhythmias in patients with OSA may be a result of abnormalities in resting cardiac repolarization.

Similar content being viewed by others
References
Somers VK, White DP, Amin R, Abraham WT, Costa F, Culebras A, Daniels S, Floras JS, Hunt CE, Olson LJ, Pickering TG, Russell R, Woo M, Young T (2008) Sleep apnea and cardiovascular disease: an American Heart Association/american College Of Cardiology Foundation Scientific Statement from the American Heart Association Council for High Blood Pressure Research Professional Education Committee, Council on Clinical Cardiology, Stroke Council, and Council On Cardiovascular Nursing. In collaboration with the National Heart, Lung, and Blood Institute National Center on Sleep Disorders Research (National Institutes of Health). Circulation 118(10):1080–1111
Guilleminault C, Connolly SJ, Winkle RA (1983) Cardiac arrhythmia and conduction disturbances during sleep in 400 patients with sleep apnea syndrome. Am J Cardiol 52(5):490–494
Pearce S, Saunders P (2003) Obstructive sleep apnoea can directly cause death. Thorax 58(4):369
Algra A, Tijssen JG, Roelandt JR, Pool J, Lubsen J (1991) QTc prolongation measured by standard 12-lead electrocardiography is an independent risk factor for sudden death due to cardiac arrest. Circulation 83(6):1888–1894
Schouten EG, Dekker JM, Meppelink P, Kok FJ, Vandenbroucke JP, Pool J (1991) QT interval prolongation predicts cardiovascular mortality in an apparently healthy population. Circulation 84(4):1516–1523
de Bruyne MC, Kors JA, Hoes AW, Klootwijk P, Dekker JM, Hofman A, van Bemmel JH, Grobbee DE (1999) Both decreased and increased heart rate variability on the standard 10-second electrocardiogram predict cardiac mortality in the elderly: the Rotterdam Study. Am J Epidemiol 150(12):1282–1288
de Bruyne MC, Hoes AW, Kors JA, Hofman A, van Bemmel JH, Grobbee DE (1999) Prolonged QT interval predicts cardiac and all-cause mortality in the elderly. The Rotterdam Study. Eur Heart J 20(4):278–284
Rautaharju PM, Nelson JC, Kronmal RA, Zhang ZM, Robbins J, Gottdiener JS, Furberg CD, Manolio T, Fried L (2001) Usefulness of T-axis deviation as an independent risk indicator for incident cardiac events in older men and women free from coronary heart disease (the Cardiovascular Health Study). Am J Cardiol 88(2):118–123
Davey P (2000) QT interval and mortality from coronary artery disease. Prog Cardiovasc Dis 42(5):359–384
Munger RG, Prineas RJ, Crow RS, Changbumrung S, Keane V, Wangsuphachart V, Jones MP (1991) Prolonged QT interval and risk of sudden death in South-East Asian men. Lancet 338(8762):280–281
Schwartz PJ, Wolf S (1978) QT interval prolongation as predictor of sudden death in patients with myocardial infarction. Circulation 57(6):1074–1077
Wheelan K, Mukharji J, Rude RE, Poole WK, Gustafson N, Thomas LJ Jr, Strauss HW, Jaffe AS, Muller JE, Roberts R et al (1986) Sudden death and its relation to QT-interval prolongation after acute myocardial infarction: two-year follow-up. Am J Cardiol 57(10):745–750
Krasemann T, Strompen C, Blumenberg J, Gehrmann J, Burkhardtsmaier G, Vogt J (2009) Changes of the corrected QT interval in healthy boys and girls over day and night. Eur Heart J 30(2):202–208
Kautzner J, Yi G, Camm AJ, Malik M (1994) Short- and long-term reproducibility of QT, QTc, and QT dispersion measurement in healthy subjects. Pacing Clin Electrophysiol 17(5 Pt 1):928–937
Veglio M, Maule S, Matteoda C, Quadri R, Valentini M, Pecchio O, Piancino G, Chiandussi L (1996) Use of corrected QT interval in autonomic function testing: assessment of reproducibility. Clin Auton Res 6(6):309–312
Browne KF, Prystowsky E, Heger JJ, Chilson DA, Zipes DP (1983) Prolongation of the Q-T interval in man during sleep. Am J Cardiol 52(1):55–59
Shamsuzzaman AS, Gersh BJ, Somers VK (2003) Obstructive sleep apnea: implications for cardiac and vascular disease. JAMA 290(14):1906–1914
Gillis AM, Stoohs R, Guilleminault C (1991) Changes in the QT interval during obstructive sleep apnea. Sleep 14(4):346–350
Horii M, Takasaki I, Ohtsuka K, Tsukiyama H, Takahashi A, Hatori Y, Hakuta T (1987) Changes of heart rate and QT interval at high altitude in alpinists: analysis by Holter ambulatory electrocardiogram. Clin Cardiol 10(4):238–242
Fuenmayor AJ, Stock FU, Fuenmayor AC, Fuenmayor PA (2002) QT interval and final portion of T wave: measurements and dispersion in infants born at high altitude. Int J Cardiol 82(2):123–126
Roche F, Reynaud C, Pichot V, Duverney D, Costes F, Garet M, Gaspoz JM, Barthelemy JC (2003) Effect of acute hypoxia on QT rate dependence and corrected QT interval in healthy subjects. Am J Cardiol 91(7):916–919
Lehmann MH, Timothy KW, Frankovich D, Fromm BS, Keating M, Locati EH, Taggart RT, Towbin JA, Moss AJ, Schwartz PJ, Vincent GM (1997) Age-gender influence on the rate-corrected QT interval and the QT-heart rate relation in families with genotypically characterized long QT syndrome. J Am Coll Cardiol 29(1):93–99
Young T, Peppard PE, Gottlieb DJ (2002) Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med 165(9):1217–1239
Bazett H (1918) An analysis of the time-relations of electrocardiograms. Heart 7:353–370
Smith TA, Mason JM, Bell JS, Francisco JT (1979) Sleep apnea and Q-T interval prolongation—a particularly lethal combination. Am Heart J 97(4):505–508
Mehra R, Benjamin EJ, Shahar E, Gottlieb DJ, Nawabit R, Kirchner HL, Sahadevan J, Redline S (2006) Association of nocturnal arrhythmias with sleep-disordered breathing: the Sleep Heart Health Study. Am J Respir Crit Care Med 173(8):910–916
Javaheri S (2000) Effects of continuous positive airway pressure on sleep apnea and ventricular irritability in patients with heart failure. Circulation 101(4):392–397
Ryan CM, Usui K, Floras JS, Bradley TD (2005) Effect of continuous positive airway pressure on ventricular ectopy in heart failure patients with obstructive sleep apnoea. Thorax 60(9):781–785
Dietrich H, Borchard U, Hafner D, Hirth C (1985) Antiarrhythmic and electrophysiological actions of flecainide, bepridil and amiodarone on isolated heart preparations during controlled hypoxia. Arch Int Pharmacodyn Ther 274(2):267–282
Murakawa Y, Inoue H, Nozaki A, Sugimoto T (1992) Role of sympathovagal interaction in diurnal variation of QT interval. Am J Cardiol 69(4):339–343
Magnano AR, Holleran S, Ramakrishnan R, Reiffel JA, Bloomfield DM (2002) Autonomic nervous system influences on QT interval in normal subjects. J Am Coll Cardiol 39(11):1820–1826
Ahnve S, Vallin H (1982) Influence of heart rate and inhibition of autonomic tone on the QT interval. Circulation 65(3):435–439
Narkiewicz K, Somers VK (2003) Sympathetic nerve activity in obstructive sleep apnoea. Acta Physiol Scand 177(3):385–390
Narkiewicz K, Montano N, Cogliati C, van de Borne PJ, Dyken ME, Somers VK (1998) Altered cardiovascular variability in obstructive sleep apnea. Circulation 98(11):1071–1077
Cicek D, Lakadamyali H, Gokay S, Sapmaz I, Muderrisoglu H (2012) Effect of obstructive sleep apnea on heart rate, heart rate recovery and QTc and P-wave dispersion in newly diagnosed untreated patients. Am J Med Sci 344(3):180–185. doi:10.1097/MAJ.0b013e318239a67f
Barta K, Szabo Z, Kun C, Munkacsy C, Bene O, Magyar MT, Csiba L, Lorincz I (2010) The effect of sleep apnea on QT interval, QT dispersion, and arrhythmias. Clin Cardiol 33(6):E35–E39. doi:10.1002/clc.20619
Rossi VA, Stoewhas AC, Camen G, Steffel J, Bloch KE, Stradling JR, Kohler M (2012) The effects of continuous positive airway pressure therapy withdrawal on cardiac repolarization: data from a randomized controlled trial. Eur Heart J 33(17):2206–2212. doi:10.1093/eurheartj/ehs073
Baumert M, Smith J, Catcheside P, McEvoy RD, Abbott D, Sanders P, Nalivaiko E (2008) Variability of QT interval duration in obstructive sleep apnea: an indicator of disease severity. Sleep 31(7):959–966
Tirlapur VG, Mir MA (1982) Nocturnal hypoxemia and associated electrocardiographic changes in patients with chronic obstructive airways disease. N Engl J Med 306(3):125–130
De Olazabal JR, Miller MJ, Cook WR, Mithoefer JC (1982) Disordered breathing and hypoxia during sleep in coronary artery disease. Chest 82(5):548–552
Kassotis J, Costeas C, Bedi AK, Tolat A, Reiffel J (2000) Effects of aging and gender on QT dispersion in an overtly healthy population. Pacing Clin Electrophysiol 23(7):1121–1126
el-Gamal A, Gallagher D, Nawras A, Gandhi P, Gomez J, Allison DB, Steinberg JS, Shumacher D, Blank R, Heymsfield SB (1995) Effects of obesity on QT, RR, and QTc intervals. Am J Cardiol 75(14):956–959
Vervaet P, Amery W (1993) QTc-measurements: a case–control study on serum electrolytes. Acta Cardiol 48(6):565–578
Johansson BW, Jorming B (1972) Hereditary prolongation of QT interval. Br Heart J 34(7):744–751
Fu EY, Clemo HF, Ellenbogen KA (1998) Acquired QT prolongation: mechanisms and implications. Cardiol Rev 6(6):319–324
Henderson W, Chu J, Hoffman R (2001) QTc prolongation and drugs. Clin Pharmacol Ther 70(6):567–568
Makkar RR, Fromm BS, Steinman RT, Meissner MD, Lehmann MH (1993) Female gender as a risk factor for torsades de pointes associated with cardiovascular drugs. JAMA 270(21):2590–2597
Lu HR, Remeysen P, Somers K, Saels A, De Clerck F (2001) Female gender is a risk factor for drug-induced long QT and cardiac arrhythmias in an in vivo rabbit model. J Cardiovasc Electrophysiol 12(5):538–545
Kimbrough J, Moss AJ, Zareba W, Robinson JL, Hall WJ, Benhorin J, Locati EH, Medina A, Napolitano C, Priori S, Schwartz PJ, Timothy K, Towbin JA, Vincent GM, Zhang L (2001) Clinical implications for affected parents and siblings of probands with long-QT syndrome. Circulation 104(5):557–562
Khositseth A, Nantarakchaikul P, Kuptanon T, Preutthipan A (2011) QT dispersion in childhood obstructive sleep apnoea syndrome. Cardiol Young 21(2):130–135. doi:10.1017/S1047951110001514
Acknowledgments
The authors are grateful to J. Denise Wetzel, CCHMC Medical Writer, for critical review of the manuscript.
Funding
These studies were supported by a Perkins Memorial Award, an American Heart Association Scientist Development Grant (0730129N, AS) and AHA Fellowship Grant (09-20069G, FSK), and the National Institutes of Health (NIH) grants HL-70302, HL-65176, TW05463, TW05469, and 1 UL1 RR024150. This publication was made possible by CTSA Grant Number UL1 TR000135 from the National Center for Advancing Translational Sciences (NCATS), a component of the NIH. Its contents are solely the responsibility of the authors and do not necessarily represent the official view of NIH.
Conflict of interest
Dr. Somers has served as a consultant for Respicardia, NeuPro, and ResMed and is an investigator on studies funded with grants from the Philips Respironics Foundation. Dr. Pressman has received funding from the Philips Respironics Foundation. The other authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shamsuzzaman, A., Amin, R.S., van der Walt, C. et al. Daytime cardiac repolarization in patients with obstructive sleep apnea. Sleep Breath 19, 1135–1140 (2015). https://doi.org/10.1007/s11325-015-1119-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1119-9