Abstract
Objectives
The aim of this study is to compare imaging techniques to evaluate trabecular bone structure using Fractal Analysis (FA).
Methods
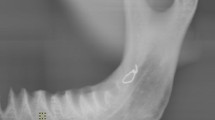
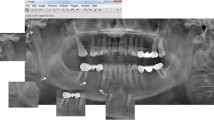
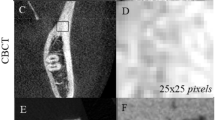
Fifteen sheep hemimandibles were used for this study. Digital images were obtained using periapical radiography, panoramic radiography, and cone-beam computed tomography (CBCT). CBCT imaging was performed in standard (STD) and high-resolution (HR) modes. FA was conducted using ImageJ 1.3 software with the box-counting method on the images. The fractal dimension (FD) values were analyzed by the statistical software Jamovi 1.6.23. Statistical significance was accepted as p < 0.05.
Results
The highest mean FD value was the FD on digital periapical radiographs (PaFD) (1.28 ± 0.04), and the lowest mean FD value was the FD on standard resolution cone-beam computed tomography images (STD-CBCTFD) (1.12 ± 0.10). Although there was no statistically significant difference between the PaFD and the FD on digital panoramic radiographs (PanFD) (p = 0.485), the PaFD was found to be significantly higher than STD-CBCTFD (p < 0.001), and the FD on high-resolution cone-beam computed tomography images (HR-CBCTFD) (p = 0.007). The PanFD was found to be significantly higher than the STD-CBCTFD (p = 0.004).
Conclusion
According to our results, in the evaluation of trabecular bone structure using FA, periapical radiographs and panoramic radiographs have similar image quality for assessment of the FD. On the other hand, CBCT results did not correlate with results from any of the other techniques in this study.



Similar content being viewed by others
Data availability
The datasets used and analyzed in the present study are available from the corresponding author upon reasonable request.
Change history
12 April 2024
A Correction to this paper has been published: https://doi.org/10.1007/s11282-024-00752-8
References
Kato CN, Barra SG, Tavares NP, Amaral TM, Brasileiro CB, Mesquita RA, et al. Use of fractal analysis in dental images: a systematic review. Dentomaxillofac Radiol. 2020;49(2):20180457. https://doi.org/10.1259/dmfr.20180457.
Kisan S, Mishra S, Rout SB. Fractal dimension in medical imaging: a review. IRJET. 2017;4(5):1102–6.
Nandal S, Ghalaut P, Shekhawat H. A radiological evaluation of marginal bone around dental implants: An in-vivo study. Natl J Maxillofac Surg. 2014;5(2):126–37.
Lo Giudice R, Nicita F, Puleio F, Alibrandi A, Cervino G, Lizio AS, et al. Accuracy of periapical radiography and CBCT in endodontic evaluation. Int J Dent. 2018;16:2514243. https://doi.org/10.1155/2018/2514243.
Sebring D, Kvist T, Buhlin K, Jonasson P, EndoReCo LH. Calibration improves observer reliability in detecting periapical pathology on panoramic radiographs. Acta Odontol Scand. 2021;79(7):554–61. https://doi.org/10.1080/00016357.2021.1910728.
Belgin CA, Serindere G. Fractal and radiomorphometric analysis of mandibular bone changes in patients undergoing intravenous corticosteroid therapy. Oral Surg Oral Med Oral Pathol Oral Radiol. 2020;130(1):110–5. https://doi.org/10.1016/j.oooo.2019.12.009.
Demiralp KÖ, Kurşun-Çakmak EŞ, Bayrak S, Akbulut N, Atakan C, Orhan K. Trabecular structure designation using fractal analysis technique on panoramic radiographs of patients with bisphosphonate intake: a preliminary study. Oral Radiol. 2019;35:23–8. https://doi.org/10.1007/s11282-018-0321-4.
Belgin CA, Serindere G. Evaluation of trabecular bone changes in patients with periodontitis using fractal analysis: A periapical radiography study. J Periodontol. 2020;91(7):933–7. https://doi.org/10.1002/jper.19-0452.
Carvalho BF, de Castro JGK, de Melo NS, de Souza Figueiredo PT, Moreira-Mesquita CR, de Paula AP, et al. Fractal dimension analysis on CBCT scans for detecting low bone mineral density in postmenopausal women. Imaging Sci Dent. 2022;52(1):53. https://doi.org/10.5624/isd.20210172.
Bollen A, Taguchi A, Hujoel P, Hollender L. Fractal dimension on dental radiographs. Dentomaxillofac Radiol. 2001;30(5):270–5. https://doi.org/10.1038/sj/dmfr/4600630.
Magat G, Sener SO. Evaluation of trabecular pattern of mandible using fractal dimension, bone area fraction, and gray scale value: comparison of cone-beam computed tomography and panoramic radiography. Oral Radiol. 2019;35(1):35–42. https://doi.org/10.1007/s11282-018-0316-1.
Sharma M, Sharma D, RahiVerma D, Sharma M, Bishnoi RR. Comparing cone-beam computed tomography with panoramic radiography for the evaluation of bone quality. J Pharm Negat Results. 2022;13(10):784–94. https://doi.org/10.47750/pnr.2022.13.S10.085.
VadiatiSaberi B, Khosravifard N, Nooshmand K, DaliliKajan Z, Ghaffari ME. Fractal analysis of the trabecular bone pattern in the presence/absence of metal artifact–producing objects: comparison of cone-beam computed tomography with panoramic and periapical radiography. Dentomaxillofac Radiol. 2021;50(6):20200559. https://doi.org/10.1259/dmfr.20200559.
Szabelska A, Tatara MR, Krupski W. Morphological, densitometric and mechanical properties of mandible in 5-month-old Polish Merino sheep. BMC Vet Res. 2017;13(1):1–7. https://doi.org/10.1186/s12917-016-0921-3.
Esen A, Dolanmaz D, Tüz HH. Biomechanical evaluation of malleable noncompression miniplates in mandibular angle fractures: an experimental study. Br J Oral Maxillofac Surg. 2012;50(5):e65-68. https://doi.org/10.1016/j.bjoms.2011.10.013.
Bayrak S, Cakmak ESK, Kamalak H. Contrast-to-noise ratios of different dental restorative materials An in-vitro cone beam computed tomography study. Eur Oral Res. 2020;54(1):36–41.
Hayek E, Aoun G, Bassit R, Nasseh I. Correlating radiographic fractal analysis at implant recipient sites with primary implant stability: an in vivo preliminary study. Cureus. 2020;12(1):e6539. https://doi.org/10.7759/cureus.6539.
White SC, Rudolph DJ. Alterations of the trabecular pattern of the jaws in patients with osteoporosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(5):628–35. https://doi.org/10.1016/s1079-2104(99)70097-1.
Soylu E, Coşgunarslan A, Çelebi S, Soydan D, Demirbaş AE, Demir O. Fractal analysis as a useful predictor for determining osseointegration of dental implant? A retrospective study. Int J Implant Dent. 2021;7:1–8. https://doi.org/10.1186/s40729-021-00296-0.
Barngkgei I, Halboub E, Almashraqi A. Effect of bisphosphonate treatment on the jawbone: an exploratory study using periapical and panoramic radiographic evaluation. Oral Radiol. 2019;35(2):159–70. https://doi.org/10.1007/s11282-018-0358-4.
Feitosa ÉF, Vasconcellos MM, Magalhães RJP, Domingos-Vieira AC, Visconti MA, Guedes FR, et al. Bisphophonate alterations of the jaw bones in individuals with multiple myeloma. Dentomaxillofac Radiol. 2020;49(2):20190155. https://doi.org/10.1259/dmfr.20190155.
Pham D, Jonasson G, Kiliaridis S. Assessment of trabecular pattern on periapical and panoramic radiographs: a pilot study. Acta Odontol Scand. 2010;68(2):91–7. https://doi.org/10.3109/00016350903468235.
Tugnait A, Clerehugh V, Hirschmann. Radiographic equipment and techniques used in general dental practice A survey of general dental practitioners in England and Wales. J Dent. 2003;31(3):197–203. https://doi.org/10.1016/s0300-5712(03)00013-7.
Baksi BG, Fidler A. Image resolution and exposure time of digital radiographs affects fractal dimension of periapical bone. Clin Oral Investig. 2012;16(5):1507–10. https://doi.org/10.1007/s00784-011-0639-3.
Ho JT, Wu J, Huang HL, Chen MY, Fuh LJ, Hsu JT. Trabecular bone structural parameters evaluated using dental cone-beam computed tomography: cellular synthetic bones. BioMed Eng OnLine. 2013;12(1):1–10. https://doi.org/10.1186/1475-925X-12-115.
Ibrahim N, Parsa A, Hassan B, van der Stelt P, Aartman IH, Wismeijer D. The effect of scan parameters on cone beam CT trabecular bone microstructural measurements of the human mandible. Dentomaxillofac Radiol. 2013;42(10):20130206.
Pauwels R, Faruangsaeng T, Charoenkarn T, Ngonphloy N, Panmekia S. Effect of exposure parameters and voxel size on bone structure analysis in CBCT. Dentomaxillofac Radiol. 2015;44(8):20150078. https://doi.org/10.1259/dmfr.20150078.
Pauwels R, Araki K, Siewerdsen JH, Thongvigitmanee SS. Technical aspects of dental CBCT: state of the art. Dentomaxillofac Radiol. 2015;44(1):20140224. https://doi.org/10.1259/dmfr.20140224.
Jolley L, Majumdar S, Kapila S. Technical factors in fractal analysis of periapical radiographs. Dentomaxillofac Radiol. 2006;35(6):393–7. https://doi.org/10.1259/dmfr/30969642.
Amuk M, Sarıbal GŞ, Ersu N, Yılmaz S. The effects of technical factors on the fractal dimension in different dental radiographic images. Eur Oral Res. 2023;57(2):68–74. https://doi.org/10.26650/eor.2023984422.
Acknowledgements
We would like to thank Lauren Penniman and Alize Dreyer for improving the use of English in the manuscript. We confirm that this work is original, it is not currently under consideration for publication elsewhere.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Ethical approval was exempt for the present study by the Local Animal Ethics Committees at Akdeniz University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: In the sentence beginning ‘The FD (FD), which measures this complexity,..’ in this article, the term ‘FD (FD)’ should have read ‘fractal dimension (FD)’.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yavuz, E., Yardimci, S. Comparison of periapical radiography, panoramic radiography, and CBCT in the evaluation of trabecular bone structure using fractal analysis. Oral Radiol (2024). https://doi.org/10.1007/s11282-024-00743-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11282-024-00743-9