Abstract
Objective
This study aimed to analyze the detailed three-dimensional measurements of temporomandibular joint (TMJ) in Chinese adults with normal occlusion and harmonious skeleton.
Methodology
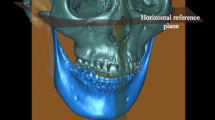
In 51 subjects 102 joints were analyzed using Anatomage Invivo dental 5.4. The measurements include: joints’ parameters, position, angulation, and inclination of the condyle and articular fossa as well as 3D volumetric of the joint-spaces. All measurements were statistically analyzed by paired Student’s t test to find out the differences between the left- and right sides. Pearson correlation coefficient test was done to figure out the relationship of the TMJ parts in the normal situation.
Results
The inter-condyle distances medially, geometrically, and laterally were 90.2 ± 5.2,107 ± 6.1, and 125 ± 5.5 mm, respectively. However, the 102 condyles were angulated on three planes 54.9º ± 11.2, 71.8º ± 7.3, and 12.5º ± 6.3 at vertical-, horizontal-, and midsagittal planes, respectively. The joint spaces measurements were 2.6 ± 0.7 mm, 2.5 ± 0.8 mm, 2.4 ± 0.7 mm, and 3.3 ± 0.7 mm for anterior-, medial-, posterior-, and superior joints, respectively. The total volume of the whole joint-space was 404.3 ± 71mm3. The left condyle position was on the centric position whereas the right condyle was eccentric (slightly anterior).
Conclusion
Chinese subjects are characterized by wide inter-fossa distance and inter-condyle distance; however, no significant correlations with joint spaces in normal occlusion were found. The asymmetries between right- and left mandibular condyle were distinguished in angular and linear-vertical measurements. Finally, this study could be considered as reference data for upcoming research in the Chinese population.





Similar content being viewed by others
Data availability
There is no any restricted available data.
References
Bordoni B, Varacallo M. Anatomy, head and neck, temporomandibular joint. StatPearls Publishing; 2019.
Pileicikiene G, et al. A three-dimensional model of the human masticatory system, including the mandible, the dentition and the temporomandibular joints. Stomatologija. 2007;9(1):27–322.
List T, Axelsson S. Management of TMD: evidence from systematic reviews and meta-analyses. J Oral Rehabil. 2010;37(6):430–51.
Alhammadi MS, Fayed MS, Labib A. Three-dimensional assessment of temporomandibular joints in skeletal class I, class II, and class III malocclusions: cone beam computed tomography analysis. J World Federation Orthodontists. 2016;5(3):80–6.
Gorucu-Coskuner H, Ciger S. Computed tomography assessment of temporomandibular joint position and dimensions in patients with class II division 1 and division 2 malocclusions. J Clin Exp Dent. 2017;9(3):e417.
Ma Q, et al. Temporomandibular condylar morphology in diverse maxillary–mandibular skeletal patterns: a 3-dimensional cone-beam computed tomography study. J Am Dental Assoc. 2018;149(7):589–98.
Vitral RWF, et al. Temporomandibular joint and normal occlusion: Is there anything singular about it? A computed tomographic evaluation. Am J Orthod Dentofac Orthop. 2011;140(1):18–24.
Alhammadi MS, et al. Temporomandibular joint measurements in normal occlusion: a three-dimensional cone beam computed tomography analysis. J World Federation Orthodontists. 2014;3(4):155–62.
Christiansen EL, et al. Computed tomography of condylar and articular disk positions within the temporomandibular joint. Oral Surg Oral Med Oral Pathol. 1987;64(6):757–67.
Koppe T, et al. Factors affecting the variation in the adult temporomandibular joint of archaeological human populations. Ann Anat Anatomischer Anz. 2007;189(4):320–5.
Al-koshab M, Nambiar P, John J. Assessment of condyle and glenoid fossa morphology using CBCT in South-East Asians. PLoS ONE. 2015;10(3):e0121682.
Silva MAG et al. (2008) Cone-beam computed tomography for routine orthodontic treatment planning: a radiation dose evaluation. Am J Orthodontics Dentofac Orthop 133(5): 640. e1–640. e5.
Suomalainen A, et al. Accuracy of linear measurements using dental cone beam and conventional multislice computed tomography. Dentomaxillofacial Radiol. 2008;37(1):10–7.
Zain-Alabdeen E, Alsadhan R. A comparative study of accuracy of detection of surface osseous changes in the temporomandibular joint using multidetector CT and cone beam CT. Dentomaxillofacial Radiol. 2012;41(3):185–91.
Pullinger A. Establishing better biological models to understand occlusion I: TM joint anatomic relationships. J Oral Rehabil. 2013;40(4):296–318.
Smith HF, Terhune CE, Lockwood CA. Genetic, geographic, and environmental correlates of human temporal bone variation. Am J Phys Anthropol. 2007;134(3):312–22.
Hongxing L, et al. Prevalence of temporomandibular disorder pain in Chinese adolescents compared to an age-matched Swedish population. J Oral Rehabil. 2016;43(4):241–8.
Lei J, et al. Sleep disturbance and psychologic distress: prevalence and risk indicators for temporomandibular disorders in a Chinese population. J Oral Facial Pain Headache 2015;29(1):24–31.
Wu N, Hirsch C. Temporomandibular disorders in German and Chinese adolescents. J Orofac Orthop/Fortschr Kieferorthop. 2010;71(3):187–98.
García-Sanz V, et al. Accuracy and reliability of cone-beam computed tomography for linear and volumetric mandibular condyle measurements. A human cadaver study. Sci Rep. 2017;7(1):11993.
Lazić B, et al. Intercondylar distances of the human temporomandibular joints. Coll Antropol. 2006;30(1):37–41.
Rodrigues AF, Fraga MR, Vitral RWF. Computed tomography evaluation of the temporomandibular joint in class II division 1 and class III malocclusion patients: condylar symmetry and condyle-fossa relationship. Am J Orthod Dentofac Orthop. 2009;136(2):199–206.
Rhee S. Differences between Caucasian and Asian attractive faces. Skin Res Technol. 2018;24(1):73–9.
Tecco S, et al. Condylar volume and surface in Caucasian young adult subjects. BMC Med Imaging. 2010;10(1):28.
Čimić S, et al. Measurements of the sagittal condylar inclination: intraindividual variations. CRANIO®. 2014;32(2):104–9.
Galeković NH, et al. Influence of the hinge axis transfer modality on the three-dimensional condylar shift between the centric relation and the maximum intercuspation positions. Acta Stomatol Croat. 2015;49(1):36.
Widman DJ. Functional and morphologic considerations of the articular eminence. Angle Orthod. 1988;58(3):221–36.
Corbett NE, et al. The relation of the condylar path to the articular eminence in mandibular protrusion. Angle Orthod. 1971;41(4):286–92.
Fraga MR, et al. Anteroposterior condylar position: a comparative study between subjects with normal occlusion and patients with class I, class II division 1, and class III malocclusions. Med Sci Monit. 2013;19:903.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Abdulqader, A.A., Ren, L., Alhammadi, M. et al. Three-dimensional analysis of temporomandibular joint in Chinese adults with normal occlusion and harmonious skeleton. Oral Radiol 36, 371–382 (2020). https://doi.org/10.1007/s11282-019-00415-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-019-00415-z