Abstract
Objectives
To compare characteristics of temporomandibular joint (TMJ) and related structures according to Angle class I, II1, II2, and III.
Methods
123 Chinese patients (13–36 years old, 60 males, and 63 females) were classified in four groups according to Angle’s classification: skeletal class I (31 patients), skeletal class II division 1 (30 patients), skeletal class II division 2 (30 patients), and skeletal class III (32 patients). Left and right TMJs of each subject were evaluated independently with cone-beam computed tomography (CBCT). The position of condyle in the joint fossa was analyzed according to Pullinger.
Results
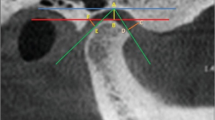
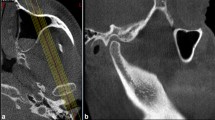
There were significant differences between class III subjects and class I, II1, II2 in the superior joint space (p < 0.05). Compared with class II1, II2, and III subjects, the height and diameter of condyle in class I was significantly larger (p < 0.05). The width of joint fossa was significantly larger in Angle class III than in Angle class I, II1, and II2, while the depth was significantly smaller. The condyle position in class III subjects was more anteriorly displaced compared with that in class I subjects. In class II2 patients, the condyle position was mainly concentric and posterior.
Conclusions
There are significant differences in condylar morphology, joint space, joint fossa morphology, and condylar position between different Angle classifications.

Similar content being viewed by others
References
Piancino MG, Cannavale R, Dalmasso P, Tonni I, Garagiola U, Perillo L, Olivieri AN. Cranial structure and condylar asymmetry of patients with juvenile idiopathic arthritis: a risky growth pattern. Clin Rheumatol. 2018;37:2667–73.
Caruso S, Storti E, Nota A, Ehsani S, Gatto R. Temporomandibular joint anatomy assessed by CBCT images. Biomed Res Int. 2017;2017:2916953.
Stocum DL, Roberts WE. Part I: development and physiology of the temporomandibular joint. Curr Osteoporos Rep. 2018;16:360–8.
Shroff B. Malocclusion as a cause for temporomandibular disorders and orthodontics as a treatment. Oral Maxillofac Surg Clin North Am. 2018;30:299–302.
Saccucci M, D'Attilio M, Rodolfino D, Festa F, Polimeni A, Tecco S. Condylar volume and condylar area in class I, class II and class III young adult subjects. Head Face Med. 2012;8:34.
Kim HO, Lee W, Kook YA, Kim Y. Comparison of the condyle-fossa relationship between skeletal class III malocclusion patients with and without asymmetry: a retrospective three-dimensional cone-beam computed tomograpy study. Korean J Orthod. 2013;43:209–17.
Schlueter B, Kim KB, Oliver D, Sortiropoulos G. Cone beam computed tomography 3D reconstruction of the mandibular condyle. Angle Orthod. 2008;78:880–8.
Ueki K, Marukawa K, Nakagawa K, Yamamoto E. Condylar and temporomandibular joint disc positions after mandibular osteotomy for prognathism. J Oral Maxillofac Surg. 2002;60:1424–32 (discussion 1432–1424).
Coskuner HG, Ciger S. Three-dimensional assessment of the temporomandibular joint and mandibular dimensions after early correction of the maxillary arch form in patients with class II division 1 or division 2 malocclusion. Korean J Orthod. 2015;45:121–9.
Ma Q, Bimal P, Mei L, Olliver S, Farella M, Li H. Temporomandibular condylar morphology in diverse maxillary-mandibular skeletal patterns: a 3-dimensional cone-beam computed tomography study. J Am Dent Assoc. 2018;149:589–98.
Pullinger A, Hollender L. Assessment of mandibular condyle position: a comparison of transcranial radiographs and linear tomograms. Oral Surg Oral Med Oral Pathol. 1985;60:329–34.
Kurusu A, Horiuchi M, Soma K. Relationship between occlusal force and mandibular condyle morphology. Evaluated by limited cone-beam computed tomography. Angle Orthod. 2009;79:1063–9.
Katsavrias EG, Halazonetis DJ. Condyle and fossa shape in class II and class III skeletal patterns: a morphometric tomographic study. Am J Orthod Dentofac Orthop. 2005;128:337–46.
Kuroda S, Tanimoto K, Izawa T, Fujihara S, Koolstra JH, Tanaka E. Biomechanical and biochemical characteristics of the mandibular condylar cartilage. Osteoarthr Cartil. 2009;17:1408–15.
Meikle MC. Remodeling the dentofacial skeleton: the biological basis of orthodontics and dentofacial orthopedics. J Dent Res. 2007;86:12–24.
Ueki K, Nakagawa K, Takatsuka S, Yamamoto E, Laskin DM. Comparison of the stress direction on the TMJ in patients with class I, II, and III skeletal relationships. Orthod Craniofac Res. 2008;11:43–50.
Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning. Part I. Am J Orthod Dentofac Orthop. 1993;103:299–312.
Arnett GW, Bergman RT. Facial keys to orthodontic diagnosis and treatment planning—part II. Am J Orthod Dentofac Orthop. 1993;103:395–411.
Manfredini D, Segu M, Arveda N, Lombardo L, Siciliani G, Alessandro R, Guarda-Nardini L. Temporomandibular joint disorders in patients with different facial morphology. A systematic review of the literature. J Oral Maxillofac Surg. 2016;74:29–46.
Pullinger AG, Solberg WK, Hollender L, Petersson A. Relationship of mandibular condylar position to dental occlusion factors in an asymptomatic population. Am J Orthod Dentofac Orthop. 1987;91:200–6.
Vitral RW, da Silva Campos MJ, Rodrigues AF, Fraga MR. Temporomandibular joint and normal occlusion: is there anything singular about it? A computed tomographic evaluation. Am J Orthod Dentofac Orthop. 2011;140:18–24.
Elfeky HY, Fayed MS, Alhammadi MS, Soliman SAZ, El Boghdadi DM. Three-dimensional skeletal, dentoalveolar and temporomandibular joint changes produced by Twin Block functional appliance. J Orofac Orthop. 2018;79:245–58.
Radescu OD, Colosi HA, Albu S. Effects of rapid palatal expansion (RPE) and twin block mandibular advancement device (MAD) on pharyngeal structures in class II pediatric patients from Cluj-Napoca, Romania. Cranio 2018. https://doi.org/10.1080/08869634.2018.1475940.
Droel R, Isaacson RJ. Some relationships between the glenoid fossa position and various skeletal discrepancies. Am J Orthod. 1972;61:64–78.
Fernandez Sanroman J, Gomez Gonzalez JM, del Hoyo JA. Relationship between condylar position, dentofacial deformity and temporomandibular joint dysfunction: an MRI and CT prospective study. J Craniomaxillofac Surg. 1998;26:35–42.
Baccetti T, Antonini A, Franchi L, Tonti M, Tollaro I. Glenoid fossa position in different facial types: a cephalometric study. Br J Orthod. 1997;24:55–9.
Kikuchi K, Takeuchi S, Tanaka E, Shibaguchi T, Tanne K. Association between condylar position, joint morphology and craniofacial morphology in orthodontic patients without temporomandibular joint disorders. J Oral Rehabil. 2003;30:1070–5.
Vitral RW, Telles Cde S, Fraga MR, de Oliveira RS, Tanaka OM. Computed tomography evaluation of temporomandibular joint alterations in patients with class II division 1 subdivision malocclusions: condyle–fossa relationship. Am J Orthod Dentofac Orthop. 2004;126:48–52.
Paknahad M, Shahidi S, Abbaszade H. Correlation between condylar position and different sagittal skeletal facial types. J Orofac Orthop. 2016;77:350–6.
Acknowledgements
This study was supported by National Natural Science Foundation of China (81771104 and 81400536). Authors are grateful to Seogsong Jeong for his statistical assistance.
Funding
National Natural Science Foundation of China, under Grant/Award numbers: 81771104 and 81400536.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5).
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Song, J., Cheng, M., Qian, Y. et al. Cone-beam CT evaluation of temporomandibular joint in permanent dentition according to Angle's classification. Oral Radiol 36, 261–266 (2020). https://doi.org/10.1007/s11282-019-00403-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-019-00403-3