Abstract
Objectives
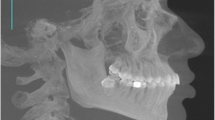
To examine the dimensions (width, length, and height) of the maxillary tuberosity (MT) and their correlations with age and sex, and to identify different anatomical types for adequate positioning of miniscrews in this area.
Methods
The study enrolled 39 patients attending the University of Valencia. The patients comprised 21 males and 18 females with a mean age of 39.7 ± 8.4 years. The dimensions of all 78 MTs were measured on cone beam computed tomography (CBCT) images using Invivo Dental 5 software.
Results
The intraobserver and interobserver errors were good for all measurements. A total of 858 MT measurements were taken. The widths were greater in men than in women, with significant differences. The MT dimensions showed correlations with patient age, whereby older patients presented with greater widths and lengths, but reduced heights. Three different anatomical types were detected according to patient age.
Conclusions
The dimensions (width, length, and height) of the MT vary according to patient age and sex. The MT dimensions conform to particular anatomical types, which should be taken into account when placing miniscrews in this region.




Similar content being viewed by others
References
Chugh KR, Jeong DM, Kim SH, Ko YI, Nelson G. En-masse retraction dependent on a temporary skeletal anchorage device without posterior bonding or banding in an adult with severe bidentoalveolar protrusion: seven years posttreatment. Am J Orthod Dentofac Orthop. 2012;141:484–94.
Bechtold TE, Kim JW, Choi TH, Park YC, Lee KJ. Distalization pattern of the maxillary arch depending on the number of orthodontic miniscrews. Angle Orthod. 2013;83:266–73.
Baik UB, Kook YA, Bayome M, Park JU, Park JH. Vertical eruption patterns of impacted mandibular third molars after the mesialization of second molars using miniscrews. Angle Orthod. 2016;86:565–70.
Lemieux G, Hart A, Cheretakis C, Goodmurphy C, Trexler S, McGary C, et al. Computed tomographic characterization of mini-implant placement pattern and maximum anchorage force in human cadavers. Am J Orthod Dentofac Orthop. 2011;140:356–65.
Marquezan M, Mattos CT, Sant’Anna EF, de Souza MM, Maia LC. Does cortical thickness influence the primary stability of miniscrews?: a systematic review and meta analysis. Angle Orthod. 2014;84:1093–103.
Park J, Cho HJ. Three-dimensional evaluation of interradicular spaces and cortical bone thickness for the placement and initial stability of microimplants in adults. Am J Orthod Dentofac Orthop. 2009;136:314.e1–12 (discussion 314–5).
Venkateswaran S, Rao V, Krishnaswamy NR. En-masse retraction using skeletal anchorage in the tuberosity and retromolar region. J Clin Orthod. 2011;45:268–73.
Sada Garralda VJ. Simultaneous intrusion and distalization using miniscrews in the maxillary tuberosity. J Clin Orthod. 2016;50:605–12.
Kim SH, Yoon HG, Choi YS, Hwang EH, Kook YA, Nelson G. Evaluation of interdental space of the maxillary posterior area for orthodontic mini-implants with cone-bean computed tomography. Am J Orthod Dentofac Orthop. 2009;135:635–41.
Chaimanee P, Suzuki B, Suzuki EY. “Safe zones” for miniscrew implant placement in different dentoskeletal patterns. Angle Orthod. 2011;81:397–403.
Fayed MM, Pazera P, Katsaros C. Optimal sites for orthodontic mini-implant placement assessed by cone beam computed tomography. Angle Orthod. 2012;80:939–51.
Poggio PM, Incorvati C, Velo S, Carano A. “Safe zones”: a guide for miniscrew positioning in the maxillary and mandibular arch. Angle Orthod. 2006;76:191–7.
Apinhasmit W, Chompoopong S, Methathrathip D, Sangvichien S, Karuwanarint S. Clinical anatomy of the posterior maxilla pertaining to Le Fort I osteotomy in Thais. Clin Anat. 2005;18:323–9.
Lopes LF, da Silva VF, Santiago JF Jr, Panzarini SR, Pellizzer EP. Placement of dental implants in the maxillary tuberosity: a systematic review. Int J Oral Maxillofac Surg. 2015;44:229–38.
Li KK, Meara JG, Alexander A Jr. Location of the descending palatine artery in relation to the Le Fort I osteotomy. J Oral Maxillofac Surg. 1996;54:822–5.
Cheung LK, Fung SC, Li T, Samman N. Posterior maxillary anatomy: implications for Le Fort I osteotomy. Int J Oral Maxillofac Surg. 1998;27:346–51.
Graves SL. The pterygoid plate implant: a solution for restoring the posterior maxilla. Int J Periodontics Restor Dent. 1994;14:512–23.
Lee SP, Paik KS, Kim MK. Anatomical study of the pyramidal process of the palatine bone in relation to implant placement in the posterior maxilla. J Oral Rehabil. 2001;28:125–32.
Rodríguez X, Rambla F, De Marcos Lopez L, Méndez V, Vela X, Jiménez Garcia J. Anatomical study of the pterygomaxillary area for implant placement: cone beam computed tomographic scanning in 100 patients. Int J Oral Maxillofac Implants. 2014;29:1049–52.
Khojasteh A, Nazeman P, Tolstunov L. Tuberosity-alveolar block as a donor site for localised augmentation of the maxilla: a retrospective clinical study. Br J Oral Maxillofac Surg. 2016;54:950–5.
Santagata M, Tozzi U, Tartaro G, Santillo V, Giovanni C, Lamart E, et al. Maxillary sinus augmentation with autologous and heterologous bone graft: a clinical and radiographic report of immediate and delayed implant placement. J Maxillofac Oral Surg. 2014;13:401–8.
Farnsworth D, Rossouw PE, Ceen RF, Buschang PH. Cortical bone thickness at common miniscrew implant placement sites. Am J Orthod Dentofac Orthop. 2011;139:495–503.
Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restor Dent. 2003;23:313–23.
Chrcanovic BR, Freire-Maia B. Considerations of maxillary tuberosity fractures during extraction of upper molars: a literature review. Dent Traumatol. 2011;27:393–8.
Vardimon AD, Shoshani K, Shpack N, Reimann S, Bourauel C, Brosh T. Incremental growth of the maxillary tuberosity from 6 to 20 years-a cross-sectional study. Arch Oral Biol. 2010;55:655–62.
Cochran DL. Inflammation and bone loss in periodontal disease. J Periodontol. 2008;79:1569–76.
John V, Alqallaf H, De Bedout T. Periodontal disease and systemic diseases: an update for the clinician. J Indiana Dent Assoc. 2016;95:16–23.
Watanabe H, Deguchi T, Hasegawa M, Ito M, Kim S, Takano-Yamamoto T. Orthodontic miniscrew failure rate and root proximity, insertion angle, bone contact length, and bone density. Orthod Craniofac Res. 2013;16:44–55.
Samrit V, Kharbanda OP, Duggal R, Seith A, Malhotra V. Bone density and miniscrew stability in orthodontic patients. Aust Orthod J. 2012;28:204–12.
Acknowledgements
The authors thank William James Packer, a professional English language editor, for translating the manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study: PL and VS recruited participants, collected data, and compiled medical records; EM made all the main measurements (intraobserver error); DM made the second measurements (interobserver error); and VPG and VGS performed data synthesis, carried out statistical analyses, and prepared the manuscript.
Corresponding author
Ethics declarations
Funding
None.
Conflict of interest
Ester Manzanera, Paula Llorca, David Manzanera, Verónica García-Sanz, Vicente Sada, and Vanessa Paredes-Gallardo declare that they have no conflict of interest.
Human rights statements and informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions. Informed consent was obtained from all patients for being included in the study.
Rights and permissions
About this article
Cite this article
Manzanera, E., Llorca, P., Manzanera, D. et al. Anatomical study of the maxillary tuberosity using cone beam computed tomography. Oral Radiol 34, 56–65 (2018). https://doi.org/10.1007/s11282-017-0284-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-017-0284-x