Abstract
Purpose
To study prognostic values of distal ureter involvement (DUI) and survival outcomes in bladder cancer at T1 and T2 stages.
Methods
The national Surveillance, Epidemiology, and End Results database (2004–2015) was applied to obtain bladder cancer patients. We used the Kaplan–Meier method with the log-rank test, subgroup analyses, the multivariable Cox proportional hazard model and propensity score matching (PSM).
Results
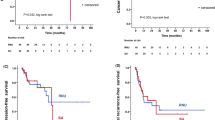
A total of 490 patients with DUI and 28,498 patients with non-DUI (non-involvement) were enrolled in our study. After 1:1 PSM, 490 matched pairs were picked out. The multivariable Cox regression before and after PSM revealed that the DUI group had a high risk of overall mortality (HR = 1.374, P < 0.001 before PSM; HR = 1.513, P < 0.001 after PSM) and cancer-specific mortality (HR = 1.632, P < 0.001 before PSM; HR = 1.699, P < 0.001 after PSM). The results of survival analyses showed that patients in the DUI group had lower survival probability in OS (P = 0.0011) and CSS (P < 0.0001) analyses. Nevertheless, in the subgroup analysis, significant differences were only observed in the T1 stage in terms of CSS and T2a stage in terms of OS and CSS (all P < 0.05).
Conclusion
The prognosis of DUI was poorer than that of non-DUI. DUI was an independent risk factor for OM and CSM in bladder cancer at T1 and T2 stages especially for those at T1 and T2a stages.






Similar content being viewed by others
Data availability statement
The data in this article came from the SEER database. The data can be found here: https://seer.cancer.gov/data/.
References
Antoni S, Ferlay J, Soerjomataram I, Znaor A, Jemal A, Bray F (2017) Bladder cancer incidence and mortality: a global overview and recent trends. Eur Urol 71(1):96–108. https://doi.org/10.1016/j.eururo.2016.06.010
Babjuk M, Burger M, Compérat EM, Gontero P, Mostafid AH, Palou J et al (2019) European Association of Urology guidelines on non-muscle-invasive bladder Cancer (TaT1 and carcinoma in situ)—2019 update. Eur Urol 76(5):639–657. https://doi.org/10.1016/j.eururo.2019.08.016
Kulkarni GS, Black PC, Sridhar SS, Kapoor A, Zlotta AR, Shayegan B et al (2019) Canadian Urological Association guideline: muscle-invasive bladder cancer. Can Urol Assoc J 13(8):230–238. https://doi.org/10.5489/cuaj.5902
Boustead GB, Fowler S, Swamy R, Kocklebergh R, Hounsome L (2014) Stage, grade and pathological characteristics of bladder cancer in the UK: British Association of Urological Surgeons (BAUS) urological tumour registry. BJU Int 113(6):924–930. https://doi.org/10.1111/bju.12468
Lorenzo Soriano L, Ordaz Jurado G, Pontones Moreno JL, Villarroya Castillo S, Hernández Girón S, Sáez Moreno I et al (2019) Tumor budding: prognostic value in muscle-invasive bladder cancer. Urology 130:93–98. https://doi.org/10.1016/j.urology.2019.04.006
Zhan X, Guo J, Chen L, Deng W, Liu X, Zhu K et al (2021) Prognostic significance of bladder neck involvement in non-muscle-invasive bladder cancer: a SEER database analysis with 19,919 patients. Cancer Med. https://doi.org/10.1002/cam4.4219
Mei Y, Zheng J, Xiang P, Liu C, Fan Y (2020) Prognostic value of the miR-200 family in bladder cancer: a systematic review and meta-analysis. Medicine (Baltimore) 99(47):e22891. https://doi.org/10.1097/md.0000000000022891
Sanderson KM, Rouprêt M (2007) Upper urinary tract tumour after radical cystectomy for transitional cell carcinoma of the bladder: an update on the risk factors, surveillance regimens and treatments. BJU Int 100(1):11–16. https://doi.org/10.1111/j.1464-410X.2007.06841.x
Chou EC, Lin AT, Chen KK, Chang LS (2006) Superficial transitional cell carcinoma of the ureteral orifice: higher risk of developing subsequent upper urinary tract tumors. Int J Urol 13(6):682–685. https://doi.org/10.1111/j.1442-2042.2006.01385.x
Wright JL, Hotaling J, Porter MP (2009) Predictors of upper tract urothelial cell carcinoma after primary bladder cancer: a population based analysis. J Urol 181(3):1035–1039. https://doi.org/10.1016/j.juro.2008.10.168 (discussion 1039)
Volkmer BG, Schnoeller T, Kuefer R, Gust K, Finter F, Hautmann RE (2009) Upper urinary tract recurrence after radical cystectomy for bladder cancer—who is at risk? J Urol 182(6):2632–2637. https://doi.org/10.1016/j.juro.2009.08.046
Rodriguez Faba O, Gaya JM, Breda A, Juarez Del Dago P, Pisano F, Salas D et al (2016) Resection of the intramural portion of the distal ureter during transurethral resection of bladder tumors: predictive factors for secondary stenosis and development of upper urinary tract recurrence. J Urol 196(1):52–56. https://doi.org/10.1016/j.juro.2016.01.038
Moschini M, Gallina A, Freschi M, Luzzago S, Fossati N, Gandaglia G et al (2016) Effect on postoperative survival of the status of distal ureteral margin: the necessity to achieve negative margins at the time of radical cystectomy. Urol Oncol 34(2):59.e15–22. https://doi.org/10.1016/j.urolonc.2015.09.001
Hou G, Zheng W, Zhang W, Zheng Y, Zhang L, Gao M et al (2020) Survival nomogram for patients with upper tract recurrence after resection for localized bladder urothelial carcinoma. Future Oncol 16(34):2835–2844. https://doi.org/10.2217/fon-2020-0560
Tellini R, Mari A, Muto G, Cacciamani GE, Ferro M, Stangl-Kremser J et al (2021) Impact of smoking habit on perioperative morbidity in patients treated with radical cystectomy for urothelial bladder cancer: a systematic review and meta-analysis. Eur Urol Oncol 4(4):580–593. https://doi.org/10.1016/j.euo.2020.10.006
Cacciamani GE, Ghodoussipour S, Mari A, Gill KS, Desai M, Artibani W et al (2020) Association between smoking exposure, neoadjuvant chemotherapy response and survival outcomes following radical cystectomy: systematic review and meta-analysis. J Urol 204(4):649–660. https://doi.org/10.1097/ju.0000000000000813
Watanabe K, Shirotake S, Umezawa Y, Takahashi T, Yamanaka T et al (2019) A case in which bladder cancer invaded the ureteral orifice and was resected via photodynamic diagnosis-assisted transurethral resection involving orally administered 5-aminolevulinic acid. IJU Case Rep 2(6):313–316. https://doi.org/10.1002/iju5.12109
Gakis G, Black PC, Bochner BH, Boorjian SA, Stenzl A, Thalmann GN et al (2017) Systematic review on the fate of the remnant urothelium after radical cystectomy. Eur Urol 71(4):545–557. https://doi.org/10.1016/j.eururo.2016.09.035
Funding
This work was supported by the National Natural Science Foundation of P.R. China (Grant Nos. 82060467 and 81760457) and the Natural Science Foundation of Jiangxi (Grant No. S2017ZRZDB0212).
Author information
Authors and Affiliations
Contributions
SX sorted the literature and wrote the manuscript. XPZ contributed significantly to data collection and data analysis. GW, TC, JW, LX, MJ, WD, KZ, ZZ, XC, QZ, WH, CZ, and XCZ helped in the revision of the manuscript. All authors contributed to the article and approved the submitted version.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationship that could be construed as a potential conflict of interest.
Ethical approval statement
The data from SEER are publicly available and de-identified.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xiao, S., Zhan, X., Chen, T. et al. Prognostic values of distal ureter involvement and survival outcomes in bladder cancer at T1 and T2 stages: a propensity score matching study. Int Urol Nephrol 54, 3123–3137 (2022). https://doi.org/10.1007/s11255-022-03260-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-022-03260-y