Abstract
Objects
To evaluate the influence of metabolic syndrome (MetS) induced by high fat diet (HFD) on prostate tissue and local inflammatory factors in rats model, and the protective efficacy of statins against pathological changes of prostate.
Methods
40 Sprague–Dawley rats were divided into 4 subgroups of normal diet (ND), HFD blank, HFD + saline and HFD + simvastatin. After the establishment of models, all subjects were killed to obtain body weight serum lipid, FBG level, FINS and HOMA-IR level. Hyperplasia level of prostate, as well as expression level of interleukin 6 (IL-6), insulin-like growth factor 1 (IGF-1), interleukin 10 (IL-10) and tumor necrosis factor alpha (TNF-α) were also measured.
Results
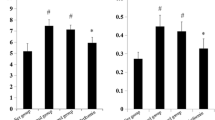
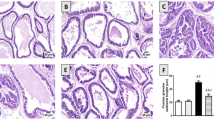
Models have been successfully established. Level of serum lipid, prostatic weight, hyperplasia as well as expressions of IL-6, TNF-α and IGF-1 in the blank and saline subgroups of HFD group were higher than that of ND group (P < 0.05). While simvastatin has significantly resisted the former effects of HFD on serum lipid and prostate (P < 0.05). No significant difference in serum FBG level was found between groups and subunits. FINS levels of ND group was lower than other groups (P < 0.05). In addition, There is no significant difference in FPG and HOMA-IR levels in blank control subunit, saline control subunit, simvastatin subunit (P > 0.05).
Conclusions
MetS induced by HFD is an important factor in the induction of BPH. Simvastatin can alleviate the hyperplasia of prostate through the relief of local inflammation in prostatic tissue.







Similar content being viewed by others
References
Cakir SS, Ozcan L, Polat EC et al (2020) Statins are effective in the treatment of benign prostatic hyperplasia with metabolic syndrome. Aging Male 23(5):538–543
Park YW, Kim SB, Kwon H et al (2013) The relationship between lower urinary tract symptoms/benign prostatic hyperplasia and the number of components of metabolic syndrome. Urology 82(3):674–679
Zhang X, Zeng X, Liu Y et al (2014) Impact of metabolic syndrome on benign prostatic hyperplasia in elderly Chinese men. Urol Int 93(2):214–219
Xia BW, Zhao SC, Chen ZP et al (2020) The underlying mechanism of metabolic syndrome on benign prostatic hyperplasia and prostate volume. Prostate 80(6):481–490
Xu C, Xu Y, Shen Z et al (2018) Effects of metformin on prostatic tissue of rats with metabolic syndrome and benign prostatic hyperplasia. Int Urol Nephrol 50(4):611–617. https://doi.org/10.1007/s11255-018-1826-9
Vykhovanets EV, Resnick MI, Marengo SR (2005) The healthy rat prostate contains high levels of natural killer-like cells and unique subsets of CD4+ helper-inducer T cells: implications for prostatitis. J Urol 173(3):1004–1010
Sirtori CR (2014) The pharmacology of statins. Pharmacol Res 88:3–11. https://doi.org/10.1016/j.phrs.2014.03.002
Romano M, Diomede L, Sironi M et al (2000) Inhibition of monocyte chemotactic protein-1 synthesis by statins. Lab Invest 80(7):1095–1100
Shimizu K, Aikawa M, Takayama K et al (2003) Direct anti-inflammatory mechanisms contribute to attenuation of experimental allograft arteriosclerosis by statins. Circulation 108(17):2113–2120
Zhang X, Zeng X, Dong L et al (2015) The effects of statins on benign prostatic hyperplasia in elderly patients with metabolic syndrome. World J Urol 33(12):2071–2077
Chung GE, Yim JY, Kim D et al (2020) Nonalcoholic fatty liver disease is associated with benign prostate hyperplasia. J Korean Med Sci 35(22):e164
Wang F, Ge A, Dai A et al (2020) Analysis of prostate-specific antigen-related indexes, neutrophil-to-lymphocyte ratio in patients with concurrent benign prostatic hyperplasia and histologic prostatitis. Clin Lab. https://doi.org/10.7754/Clin.Lab.2019.190428
Nickel JC, Roehrborn CG, O’Leary MP et al (2008) The relationship between prostate inflammation and lower urinary tract symptoms: examination of baseline data from the REDUCE trial. Eur Urol 54(6):1379–1384
Robert G, Descazeaud A, Nicolaïew N et al (2009) Inflammation in benign prostatic hyperplasia: a 282 patients’ immunohistochemical analysis. Prostate 69(16):1774–1780. https://doi.org/10.1002/pros.21027
Zlotta AR, Egawa S, Pushkar D et al (2014) Prevalence of inflammation and benign prostatic hyperplasia on autopsy in Asian and Caucasian men. Eur Urol 66(4):619–622
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (2001) Executive Summary of the third report of the National Cholesterol Education Program (NCEP) Expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (Adult Treatment Panel III). JAMA 285(19):2486–2497
Devaraj S, Singh U, Jialal I (2009) Human C-reactive protein and the metabolic syndrome. Curr Opin Lipidol 20(3):182–189
Shankar E, Vykhovanets EV, Vykhovanets OV et al (2012) High-fat diet activates pro-inflammatory response in the prostate through association of Stat-3 and NF-κB. Prostate 72(3):233–243. https://doi.org/10.1002/pros.21425
De Nunzio C, Aronson W, Freedland SJ et al (2012) The correlation between metabolic syndrome and prostatic diseases. Eur Urol 61(3):560–570
Vignozzi L, Gacci M, Maggi M (2016) Lower urinary tract symptoms, benign prostatic hyperplasia and metabolic syndrome. Nat Rev Urol 13(2):108–119
Wang L, Yang JR, Yang LY et al (2008) Chronic inflammation in benign prostatic hyperplasia: implications for therapy. Med Hypotheses 70(5):1021–1023
Gacci M, Vignozzi L, Sebastianelli A et al (2013) Metabolic syndrome and lower urinary tract symptoms: the role of inflammation. Prostate Cancer Prostatic Dis 16(1):101–106
St Sauver JL, Jacobsen SJ, Jacobson DJ et al (2011) Statin use and decreased risk of benign prostatic enlargement and lower urinary tract symptoms. BJU Int 107(3):443–450
Yang X, Zhang Q, Jiang G et al (2019) The effects of statins on benign prostatic hyperplasia and the lower urinary tract symptoms: a meta-analysis. Medicine (Baltimore) 98(18):e15502
McLaren ID, Jerde TJ, Bushman W (2011) Role of interleukins, IGF and stem cells in BPH. Differentiation 82(4–5):237–243
Fibbi B, Penna G, Morelli A et al (2010) Chronic inflammation in the pathogenesis of benign prostatic hyperplasia. Int J Androl 33(3):475–488
Danesh FR, Anel RL, Zeng L et al (2003) Immunomodulatory effects of HMG-CoA reductase inhibitors. Arch Immunol Ther Exp (Warsz) 51:139–148
Kwak BR, Mulhaupt F, Mach F (2003) Atherosclerosis: anti-inflammatory and immunomodulatory activities of statins. Autoimmun Rev 2(6):332–338
Liberale L, Carbone F, Montecucco F et al (2020) Statins reduce vascular inflammation in atherogenesis: A review of underlying molecular mechanisms. Int J Biochem Cell Biol 122:105735
Kaplan-Lefko PJ, Sutherland BW, Evangelou AI et al (2008) Enforced epithelial expression of IGF-1 causes hyperplastic prostate growth while negative selection is requisite for spontaneous metastogenesis. Oncogene 27(20):2868–2876
Lu T, Lin WJ, Izumi K et al (2012) Targeting androgen receptor to suppress macrophage-induced EMT and benign prostatic hyperplasia (BPH) development. Mol Endocrinol 26(10):1707–1715
Cevenini A, Orrù S, Mancini A et al (2018) Molecular signatures of the insulin-like growth factor 1-mediated epithelial-mesenchymal transition in breast, lung and gastric cancers. Int J Mol Sci 19(8):2411
Szkodziński J, Romanowski W, Hudzik B et al (2009) Effect of HMG-CoA (3-hydroxy-3-methylglutaryl-CoA) reductase inhibitors on the concentration of insulin-like growth factor-1 (IGF-1) in hypercholesterolemic patients. Pharmacol Rep 61(4):654–664
Bergen K, Brismar K, Tehrani S (2016) High-dose atorvastatin is associated with lower IGF-1 levels in patients with type 1 diabetes. Growth Horm IGF Res 29:78–82
Liu F, Sun Y, Liu B et al (2018) Insulin-like growth factor-1 induces epithelial-mesenchymal transition in hepatocellular carcinoma by activating survivin. Oncol Rep 40(2):952–958
Yin L, Tang Y, Pan A et al (2019) The application of IL-10 and TNF-α in expressed prostatic secretions and prostatic exosomal protein in urine in the diagnosis of patients with chronic prostatitis. Medicine (Baltimore) 98(33):e16848
Roya N, Fatemeh T, Faramarz MA et al (2020) Frequency of IL-10+CD19+ B cells in patients with prostate cancer compared to patients with benign prostatic hyperplasia. Afr Health Sci 20(3):1264–1272
Zhang P, Zhang X, Huang Y et al (2021) Atorvastatin alleviates microglia-mediated neuroinflammation via modulating the microbial composition and the intestinal barrier function in ischemic stroke mice. Free Radic Biol Med 162:104–117
Acknowledgements
Relevant personnel from the department of pathology, laboratory animals center, and urology of Anhui provincial hospital have provided a great deal of help.
Funding
This study was funded by Natural Science Foundation of Anhui Province (1908085QH315).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical approval
The use of animals in this research was approved by the ethics committee of experimental animal of Anhui medical university.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gong, Y.m., Wang, X., Liu, S. et al. Simvastatin inhibits prostatic hyperplasia in rats with metabolic syndrome. Int Urol Nephrol 54, 2125–2131 (2022). https://doi.org/10.1007/s11255-022-03227-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-022-03227-z