Abstract
Purpose
To establish a male rat model of neurogenic bladder after bilateral pelvic nerve injury (BPNI) and investigate the factors associated with onset of neurogenic bladder.
Methods
Twenty-four 8-week-old male Sprague–Dawley rats were randomly divided into three groups (n = 8 rats per group). Rats in 4-week and 8-week nerve injury group underwent BPNI, while rats in the sham group underwent a sham operation. Bladder functional analysis were performed and then bladders tissues were harvested for morphological examination and investigating the mRNA expression levels of target genes in all rats.
Results
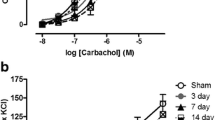
The bladder weight significantly increased in rats following BPNI. Functional analysis revealed non-voiding contractions and decreased detrusor contractility following BPNI, manifested as elevated post-void residual and bladder capacity while reduced maximum voiding pressure and voiding efficiency. The collagen area in bladder tissue and mRNA expression levels of target genes significantly increased at 4 or 8 weeks post-BPNI except Smad3. At 4 weeks post-BPNI, expression levels of vesicular acetylcholine transporter were reduced, then returned to baseline at 8 weeks. Expression levels of tyrosine hydroxylase were reduced at both 4 and 8 weeks post-BPNI.
Conclusions
A neurogenic bladder animal model was successfully established by performing BPNI in male rats, characterized by impaired voiding function, bladder detrusor fibrosis, and reduced neurotransmitter release.




Similar content being viewed by others
References
Ilic D, Evans SM, Allan CA, Jung JH, Murphy D (2018) Laparoscopic and robot-assisted vs. open radical prostatectomy for the treatment of localized prostate cancer. Cochrane Syst Rev 121(6):845–853. https://doi.org/10.1111/bju.14062
Polat F, Willems LH (2019) The oncological and surgical safety of robot-assisted surgery in colorectal cancer: outcomes of a longitudinal prospective cohort study. Surg Endosc 33(11):3644–3655. https://doi.org/10.1007/s00464-018-06653-2
Hollabaugh RS Jr, Steiner MS, Sellers KD, Samm BJ, Dmochowski RR (2000) Neuroanatomy of the pelvis: implications for colonic and rectal resection. Dis Colon Rectum 43(10):1390–1397. https://doi.org/10.1007/bf02236635
Katepratoom C, Manchana T, Amornwichet N (2014) Lower urinary tract dysfunction and quality of life in cervical cancer survivors after concurrent chemoradiation versus radical hysterectomy. Int Urogynecol J 25(1):91–96. https://doi.org/10.1007/s00192-013-2151-6
Yoo KH, Lee SJ (2010) Experimental animal models of neurogenic bladder dysfunction. Int Neurourol J 14(1):1–6. https://doi.org/10.5213/inj.2010.14.1.1
Dewulf K, Weyne E (2019) Functional and molecular characterisation of the bilateral pelvic nerve crush injury rat model for neurogenic detrusor underactivity. BJU Int 123(5a):E86–e96. https://doi.org/10.1111/bju.14649
Deruyver Y, Weyne E, Dewulf K, Rietjens R, Pinto S, Van Ranst N, Franken J, Vanneste M, Albersen M, Gevaert T, Vennekens R, De Ridder D, Voets T, Everaerts W (2018) Intravesical activation of the cation channel TRPV4 improves bladder function in a rat model for detrusor underactivity. Eur Urol 74(3):336–345. https://doi.org/10.1016/j.eururo.2018.05.020
Takaoka EI, Kurobe M, Okada H, Takai S, Suzuki T, Shimizu N, Kwon J, Nishiyama H, Yoshimura N (2018) Effect of TRPV4 activation in a rat model of detrusor underactivity induced by bilateral pelvic nerve crush injury. Neurol Urodyn 37(8):2527–2534. https://doi.org/10.1002/nau.23790
Arellano J, Xelhuantzi N, Mirto N, Hernández ME, Cruz Y (2019) Neural interrelationships of autonomic ganglia from the pelvic region of male rats. Auto Neurosci Basic Clin 217:26–34. https://doi.org/10.1016/j.autneu.2018.12.005
Matsui M, Motomura D, Fujikawa T, Jiang J, Takahashi S, Manabe T, Taketo MM (2002) Mice lacking M2 and M3 muscarinic acetylcholine receptors are devoid of cholinergic smooth muscle contractions but still viable. J Neurosci Off J Soc Neurosci 22(24):10627–10632. https://doi.org/10.1523/jneurosci.22-24-10627.2002
Shefchyk SJ (2002) Spinal cord neural organization controlling the urinary bladder and striated sphincter. Prog Brain Res 137:71–82. https://doi.org/10.1016/s0079-6123(02)37008-0
Chughtai B, Thomas D, Kaplan S (2016) α-blockers, 5-α-reductase inhibitors, acetylcholine, β3 agonists, and phosphodiesterase-5s in medical management of lower urinary tract symptoms/benign prostatic hyperplasia: how much do the different formulations actually matter in the classes? Urol Clin North Am 43(3):351–356. https://doi.org/10.1016/j.ucl.2016.04.013
de Groat WC, Griffiths D, Yoshimura N (2015) Neural control of the lower urinary tract. Compr Physiol 5(1):327–396. https://doi.org/10.1002/cphy.c130056
Andersson KE, Arner A (2004) Urinary bladder contraction and relaxation: physiology and pathophysiology. Physiol Rev 84(3):935–986. https://doi.org/10.1152/physrev.00038.2003
Tan WQ, Fang QQ, Shen XZ et al (2018) Angiotensin-converting enzyme inhibitor works as a scar formation inhibitor by down-regulating Smad and TGF-β-activated kinase 1 (TAK1) pathways in mice. Br J Pharmacol 175(22):4239–4252. https://doi.org/10.1111/bph.14489
Uvin P, Everaerts W, Pinto S, Alpízar YA, Boudes M, Gevaert T, Voets T, Nilius B, Talavera K, De Ridder D (2012) The use of cystometry in small rodents: a study of bladder chemosensation. J Visual Exper JoVE 66:e3869. https://doi.org/10.3791/3869
Sekido N, Kida J, Mashimo H, Wakamatsu D, Okada H, Matsuya H (2016) Promising effects of a novel EP2 and EP3 receptor dual agonist, ONO-8055, on neurogenic underactive bladder in a rat lumbar canal stenosis model. J Urol 196(2):609–616. https://doi.org/10.1016/j.juro.2016.02.064
Nakamura I, Takahashi C, Miyagawa I (1992) The alterations of norepinephrine and acetylcholine concentrations in immature rat urinary bladder caused by streptozotocin-induced diabetes. J Urol 148(2 Pt 1):423–426. https://doi.org/10.1016/s0022-5347(17)36621-1
Manchana T, Prasartsakulchai C, Santingamkun A (2010) Long-term lower urinary tract dysfunction after radical hysterectomy in patients with early postoperative voiding dysfunction. Int Urogynecol J 21(1):95–101. https://doi.org/10.1007/s00192-009-0996-5
Shaker H, Mourad MS, Elbialy MH, Elhilali M (2003) Urinary bladder hyperreflexia: a rat animal model. Neurourol Urodyn 22(7):693–698. https://doi.org/10.1002/nau.10147
Salehi-Pourmehr H, Rahbarghazi R, Mahmoudi J, Roshangar L, Chapple CR, Hajebrahimi S, Abolhasanpour N, Azghani MR (2019) Intra-bladder wall transplantation of bone marrow mesenchymal stem cells improved urinary bladder dysfunction following spinal cord injury. Life Sci 221:20–28. https://doi.org/10.1016/j.lfs.2019.02.011
Lluel P, Palea S, Barras M, Grandadam F, Heudes D, Bruneval P, Corman B, Martin DJ (2000) Functional and morphological modifications of the urinary bladder in aging female rats. Am J Physiol Regul Integr Comp Physiol 278(4):R964–972. https://doi.org/10.1152/ajpregu.2000.278.4.R964
Cameron AP, Clemens JQ, Latini JM, McGuire EJ (2009) Combination drug therapy improves compliance of the neurogenic bladder. J Urol 182(3):1062–1067. https://doi.org/10.1016/j.juro.2009.05.038
Hannan JL, Powers SA, Wang VM, Castiglione F, Hedlund P, Bivalacqua TJ (2017) Impaired contraction and decreased detrusor innervation in a female rat model of pelvic neuropraxia. Int Urogynecol J 28(7):1049–1056. https://doi.org/10.1007/s00192-016-3223-1
Fry CH, Kitney DG, Paniker J, Drake MJ, Kanai A, Andersson KE (2018) Fibrosis and the bladder, implications for function ICI-RS 2017. Neurourol Urodyn 37(S4):S7–s12. https://doi.org/10.1002/nau.23725
Zhao J, Wu M, Chen S, Ji Z, Zheng X (2018) TGF-β1 and connexin-43 expression in neurogenic bladder from rats with sacral spinal cord injury. Neurourol Urodyn 37(8):2502–2509. https://doi.org/10.1002/nau.23767
Akhurst RJ, Hata A (2012) Targeting the TGFβ signalling pathway in disease. Nat Rev Drug Discovery 11(10):790–811. https://doi.org/10.1038/nrd3810
Johnston L, Cunningham RM, Young JS, Fry CH, McMurray G, Eccles R, McCloskey KD (2012) Altered distribution of interstitial cells and innervation in the rat urinary bladder following spinal cord injury. J Cell Mol Med 16(7):1533–1543. https://doi.org/10.1111/j.1582-4934.2011.01410.x
Takahara Y, Maeda M, Nakatani T, Kiyama H (2007) Transient suppression of the vesicular acetylcholine transporter in urinary bladder pathways following spinal cord injury. Brain Res 1137(1):20–28. https://doi.org/10.1016/j.brainres.2006.12.042
Keast JR (2004) Remodelling of connections in pelvic ganglia after hypogastric nerve crush. Neuroscience 126(2):405–414. https://doi.org/10.1016/j.neuroscience.2004.03.059
Raspagliesi F, Bogani G, Spinillo A et al (2017) Introducing nerve-sparing approach during minimally invasive radical hysterectomy for locally-advanced cervical cancer: a multi-institutional experience. Eur J Surg Oncol J Eur Soc Surg Oncol Br Assoc Surg Oncol 43(11):2150–2156. https://doi.org/10.1016/j.ejso.2017.08.015
Crescenze IM, Myers JB, Lenherr SM, Elliott SP, Welk B (2019) Predictors of low urinary quality of life in spinal cord injury patients on clean intermittent catheterization. Neurol Urodyn 38(5):1332–1338. https://doi.org/10.1002/nau.23983
Funding
This work was supported by the Anhui Provincial Natural Science Foundation [grant numbers: 1708085QH179].
Author information
Authors and Affiliations
Contributions
QG, JX, and ZS contributed to the study conception and design. Material preparation, data collection and analysis were performed by QG, MW, YL, and CX. The first draft of the manuscript was written by QG and ZS, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
We declare that we have no conflict of interest.
Ethical approval
Animal experiments were conducted in accordance with institutional guidelines approved by the Animal Care and Use Committee of Anhui Medical University. The work was performed at Provincial Hospital Affiliated to Anhui Medical University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ge, Q., Wang, M., Lin, Y. et al. Establishment of animal model manifested as bladder neurogenic changes generated by bilateral pelvic nerve injury in male rats. Int Urol Nephrol 53, 421–429 (2021). https://doi.org/10.1007/s11255-020-02668-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-020-02668-8