Abstract
Purpose
Malnutrition, inflammation and poor quality of life are prevalent among elderly haemodialysis patients. Megestrol acetate (MA) is a synthetic progestin that is widely used to increase appetite and weight in various clinical settings. MA has been indicated to be effective in improving quality of life in patients with cancers. The aim of the present study was to evaluate the efficacy and safety of MA in treating malnourished elderly haemodialysis patients.
Methods
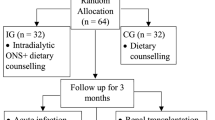
A randomized controlled study involving 46 hypoalbuminemia haemodialysis patients aged 70 years or older was conducted. The patients in MA-treated group (n = 23) took 160 mg of MA daily, while those in control group (n = 23) were enrolled without any intervention. Anthropometric parameters and laboratory results, including height, dry weight, body mass index, and modified subjective global assessment score as well as serum albumin, triglyceride, total cholesterol, hsCRP, IL-1b and IL-6 concentrations were measured in all patients before and after the intervention. Health-related quality of life was also evaluated using the KDQOL-SF 1.3.
Results
In the MA-treated group, a total of 18 patients finished the therapy over a 3-month period. Appetite was reported as improved by 15 patients, and a statistically significant increase was observed in dry weight (53.36 ± 6.15 vs. 54.24 ± 6.32, P < 0.01) and serum albumin concentration (29.05 ± 3.91 vs. 37.67 ± 4.88, P < 0.01) in the MA-treated group compared to those of the control group. The quality of life in both the physical domain (46.73 ± 18.17 vs. 63.37 ± 22.35, P < 0.01) and the mental domain (50.28 ± 20.36 vs. 68.02 ± 25.48, P < 0.01) was also improved in the same group. There was no significant change in the inflammatory marker concentrations after the intervention. No serious or unexpected adverse events were observed except that one patient who withdrew due to excessive fluid gain between haemodialysis sessions.
Conclusion
Our data suggest that MA can be effective in improving nutritional status and quality of life by increasing appetite in elderly haemodialysis patients with acceptable side effects; however, MA might not ameliorate inflammation.

Similar content being viewed by others
References
Kurella M, Covinsky KE, Collins AJ, Chertow GM (2007) Octogenarians and nonagenarians starting dialysis in the United States. Ann Intern Med 146(3):177–183
Stevens LA, Viswanathan G, Weiner DE (2010) Chronic kidney disease and end-stage renal disease in the elderly population: current prevalence, future projections, and clinical significance. Adv Chronic Kidney Dis 17(4):293–301. https://doi.org/10.1053/j.ackd.2010.03.010
Naini AE, Karbalaie A, Abedini M, Askari G, Moeinzadeh F (2016) Comparison of malnutrition in hemodialysis and peritoneal dialysis patients and its relationship with echocardiographic findings. J Res Med Sci 21:78. https://doi.org/10.4103/1735-1995.189695
Burrowes JD, Larive B, Chertow GM, Cockram DB, Dwyer JT, Greene T, Kusek JW, Leung J, Rocco MV (2005) Self-reported appetite, hospitalization and death in haemodialysis patients: findings from the hemodialysis (HEMO) study. Nephrol Dial Transplant 20(12):2765–2774
Brown EA, Johansson L (2011) Epidemiology and management of end-stage renal disease in the elderly. Nat Rev Nephrol 7(10):591–598. https://doi.org/10.1038/nrneph.2011.113
Sohrabi Z, Eftekhari MH, Eskandari MH, Rezaeianzadeh A, Sagheb MM (2015) Malnutrition-inflammation score and quality of life in hemodialysis patients: is there any correlation? Nephro-urol Mon 7(3):e27445. https://doi.org/10.5812/numonthly.7(3)2015.27445
Carrero JJ, Aguilera A, Stenvinkel P, Gil F, Selgas R, Lindholm B (2008) Appetite disorders in uremia. J Ren Nutr 18(1):107–113. https://doi.org/10.1053/j.jrn.2007.10.022
Heng AE, Cano NJM (2010) Nutritional problems in adult patients with stage 5 chronic kidney disease on dialysis (both haemodialysis and peritoneal dialysis). NDT Plus 3(2):109–117
Braga SFM, Sérgio Viana P, Isabel Cristina G, Acúrcio FDA, Andrade EIG, Mariangela Leal C (2011) Factors associated with health-related quality of life in elderly patients on hemodialysis. Revista De Saúde Pública 45(6):1127
Seckinger J, Dschietzig W, Leimenstoll G, Rob PM, Kuhlmann MK, Pommer W, Fraass U, Ritz E, Schwenger V (2016) Morbidity, mortality and quality of life in the ageing haemodialysis population: results from the ELDERLY study. Clin Kidney J 9(6):839–848. https://doi.org/10.1093/ckj/sfw087
Campbell KL, Ash S, Bauer JD (2008) The impact of nutrition intervention on quality of life in pre-dialysis chronic kidney disease patients. Clin Nutr 27(4):537–544. https://doi.org/10.1016/j.clnu.2008.05.002
Ruiz-Garcia V, Lopez-Briz E, Carbonell-Sanchis R, Bort-Marti S, Gonzalvez-Perales JL (2018) Megestrol acetate for cachexia-anorexia syndrome. A systematic review. J Cachexia Sarcopenia Muscle 9(3):444–452. https://doi.org/10.1002/jcsm.12292
Aoyagi T, Terracina KP, Raza A, Matsubara H, Takabe K (2015) Cancer cachexia, mechanism and treatment. World J Gastrointest Oncol 7(4):17–29. https://doi.org/10.4251/wjgo.v7.i4.17
Wazny LD, Nadurak S, Orsulak C, Giles-Smith L, Tangri N (2016) The efficacy and safety of megestrol acetate in protein-energy wasting due to chronic kidney disease: a systematic review. J Ren Nutr 26(3):168–176. https://doi.org/10.1053/j.jrn.2015.11.002
Golebiewska JE, Lichodziejewska-Niemierko M, Aleksandrowicz-Wrona E, Majkowicz M, Lysiak-Szydlowska W, Rutkowski B (2012) Influence of megestrol acetate on nutrition, inflammation and quality of life in dialysis patients. Int Urol Nephrol 44(4):1211–1222. https://doi.org/10.1007/s11255-011-0025-8
Fernandez Lucas M, Teruel JL, Burguera V, Sosa H, Rivera M, Rodriguez Palomares JR, Marcen R, Quereda C (2010) Treatment of uraemic anorexia with megestrol acetate. Nefrologia: publicacion oficial de la Sociedad Espanola Nefrologia 30(6):646–652. https://doi.org/10.3265/Nefrologia.pre2010.Aug.10546
Yeh SS, Marandi M, Thode HC Jr, Levine DM, Parker T, Dixon T, Schuster MW (2010) Report of a pilot, double-blind, placebo-controlled study of megestrol acetate in elderly dialysis patients with cachexia. J Ren Nutr 20(1):52–62. https://doi.org/10.1053/j.jrn.2009.08.005
Lopes AA, Elder SJ, Ginsberg N, Andreucci VE, Cruz JM, Fukuhara S, Mapes DL, Saito A, Pisoni RL, Saran R, Port FK (2007) Lack of appetite in haemodialysis patients–associations with patient characteristics, indicators of nutritional status and outcomes in the international DOPPS. Nephrol Dial Transplant 22(12):3538–3546. https://doi.org/10.1093/ndt/gfm453
Hays RD AN, Alonso J, et al (1997) Kidney disease quality of life short form (KDQOLSF), version 1.3: a manual for use and scoring. http://www.randorg/pubs/papers/2006/P7994pdf. Accessed 21 Oct 2011
Yamashita M, Komatsu R, Maruyama Y, Takaki T, Ichinose H, Sasaki O, Sawase K, Harada T, Funakoshi S (2018) Dietary approach to improving the nutritional status in institutionalized elderly hemodialysis patients with a poor dietary intake: a single-arm pilot study. Nihon Ronen Igakkai zasshi Jpn J Geriatr 55(1):90–97. https://doi.org/10.3143/geriatrics.55.90
Bossola M, Tazza L (2013) Appetite and the risk of death in patients on chronic hemodialysis. J Ren Nutr 23(5):397. https://doi.org/10.1053/j.jrn.2013.03.001
McCarthy HD, Crowder RE, Dryden S, Williams G (1994) Megestrol acetate stimulates food and water intake in the rat: effects on regional hypothalamic neuropeptide Y concentrations. Eur J Pharmacol 265(1–2):99–102
Costa AM, Spence KT, Plata-Salaman CR, ffrench-Mullen JM (1995) Residual Ca2+ channel current modulation by megestrol acetate via a G-protein alpha s-subunit in rat hypothalamic neurones. J Physiol 487(Pt 2):291–303
Schindler AE, Campagnoli C, Druckmann R, Huber J, Pasqualini JR, Schweppe KW, Thijssen JH (2008) Classification and pharmacology of progestins. Maturitas 61(1–2):171–180
Boccanfuso JA, Hutton M, McAllister B (2000) The effects of megestrol acetate on nutritional parameters in a dialysis population. J Ren Nutr 10(1):36–43. https://doi.org/10.1053/jren01000036
Young P, Lombi F, Finn BC, Forrester M, Campolo-Girard V, Pomeranz V, Iriarte R, Bruetman JE, Trimarchi H (2011) “Malnutrition-inflammation complex syndrome” in chronic hemodialysis. Medicina 71(1):66–72
Mikolasevic I, Lukenda V, Racki S, Milic S, Sladoje-Martinovic B, Orlic L (2014) Nonalcoholic fatty liver disease (NAFLD)-a new factor that interplays between inflammation, malnutrition, and atherosclerosis in elderly hemodialysis patients. Clin Interv Aging 9:1295–1303. https://doi.org/10.2147/cia.s65382
Rammohan M, Kalantar-Zadeh K, Liang A, Ghossein C (2005) Megestrol acetate in a moderate dose for the treatment of malnutrition-inflammation complex in maintenance dialysis patients. J Ren Nutr 15(3):345–355
Zhu Q, Scherer PE (2018) Immunologic and endocrine functions of adipose tissue: implications for kidney disease. Nat Rev Nephrol 14(2):105–120. https://doi.org/10.1038/nrneph.2017.157
Turkmen K, Erdur FM, Guney I, Gaipov A, Turgut F, Altintepe L, Saglam M, Tonbul HZ, Abdel-Rahman EM (2012) Sleep quality, depression, and quality of life in elderly hemodialysis patients. Int J Nephrol Renovasc Dis 5:135–142
Beller E, Tattersall M, Lumley T, Levi J, Dalley D, Olver I, Page J, Abdi E, Wynne C, Friedlander M (1997) Improved quality of life with megestrol acetate in patients with endocrine-insensitive advanced cancer: a randomised placebo-controlled trial. Ann Oncol 8(3):277
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zheng, Z., Chen, J., He, D. et al. The effects of megestrol acetate on nutrition, inflammation and quality of life in elderly haemodialysis patients. Int Urol Nephrol 51, 1631–1638 (2019). https://doi.org/10.1007/s11255-019-02245-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-019-02245-8