Abstract
Background
Bone mineral density (BMD) has been reported to increase without specific treatment in long-term renal transplant recipients. The aim of this study was to evaluate the effect of ibandronate on BMD and kidney function in long-term renal transplant recipients as compared to a control group. Furthermore, we searched for a gender-specific treatment effect of ibandronate on BMD.
Methods
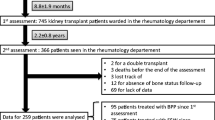
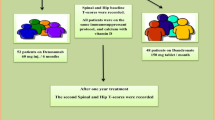
In a retrospective, matched case-control study 60 stable renal transplant recipients were included on long-term follow-up. The patient cohort was divided into two groups. The control group (n = 30) comprised patients with close-to-normal bone mineral density who did not receive ibandronate treatment and the treatment group (n = 30) comprised patients with reduced bone mineral density who received ibandronate treatment. The groups were matched for sex, age at the time of renal transplantation, use of steroids, renal transplant function and time lag between the dual-energy X-ray absorptiometry (DEXA) measurements and renal transplantation. Patients of the treatment group were treated with 12.0 ± 6.7 g ibandronate. Treatment cycles lasted 19.3 ± 11.0 months. The first bone mineral density testing was performed 55.3 ± 60.2 months after renal transplantation followed by a second measurement 26.8 ± 12.1 months later.
Results
Both groups did not differ in absolute (g/cm2) or relative (%) changes in BMD at the lumbar spine (0.033 ± 0.079 vs. 0.055 ± 0.066 g/cm2, p = 0.217 and 3.6 ± 7.8 vs. 6.4 ± 8.1 %, p = 0.124) or femoral neck (0.013 ± 0.106 vs. 0.025 ± 0.077 g/cm2, p = 0.647 and 3.2 ± 13.6 vs. 5.0 ± 13.1 %, p = 0.544) over the study period. There was no correlation of ibandronate dosages with changes in BMD (LS: r = −0.089; p = 0.639 and FN: r =+0.288; p = 0.445). We could neither determine a negative effect of ibandronate on renal transplant function over the study period, estimated via the CKD-EPI formula (−2.9 ± 7.6 vs. −2.7 ± 10.6 mL/min/1.73 m2, p = 0.900) nor a gender-specific action of ibandronate on bone mass changes.
Conclusions
Ibandronate treatment was safe with respect to renal transplant function but did not result in a significant additive improvement in bone mineral density as compared to the untreated control group. A gender-specific action of ibandronate on BMD at the LS or FN could not be determined either.


Similar content being viewed by others
References
Canalis E (2003) Mechanisms of glucocorticoid-induced osteoporosis. Curr Opin Rheumatol 15:454–457
Kalantar-Zadeh K, Molnar MZ, Kovesdy CP, Mucsi I, Bunnapradist S (2012) Management of mineral and bone disorder after kidney transplantation. Curr Opin Nephrol Hypertens 21:389–403
Bia M (2008) Evaluation and management of bone disease and fractures post transplant. Transplant Rev (Orlando) 22:52–61
Weisinger JR, Garlini RG, Rojas E, Bellorin-Font E (2006) Bone disease after renal transplantation. Clin J Am Soc Nephrol 1:1300–1313
Maalouf NM, Shane E (2005) Osteoporosis after solid organ transplantation. J Clin Endocrinol Metab 90:2456–2465
Doumousi E, Leivaditis K, Eleftheriadis T, Liakopoulos V (2015) Osteoporosis after renal transplantation. Int Urol Nephrol 47:503–511
Pichette V, Bonnardeaux A, Prudhomme L, Gagné M, Cardinal J, Ouimet D (1996) Long-term bone loss in kidney transplant recipients: a cross-sectional and longitudinal study. Am J Kidney Dis 28:105–114
Brandenburg VM, Ketteler M, Heussen N, Politt D, Frank RD, Westenfeld R, Ittel TH, Floege J (2006) Lumbar bone mineral density in very long-term renal transplant recipients: impact of circulating sex hormones. Osteoporos Int 16:1611–1620
Brandenburg VM, Ketteler M, Fassbender WJ, Heussen N, Freuding T, Floege J, Ittel TH (2002) Development of lumbar bone mineral density in the late course after kidney transplantation. Am J Kidney Dis 40:1066–1074
Brandenburg VM, Politt D, Ketteler M, Fassbender WJ, Heussen N, Westenfeld R, Freuding T, Floege J, Ittel TH (2004) Early rapid loss followed by long-term consolidation characterizes the development of lumbar bone mineral density after kidney transplantation. Transplantation 77:1566–1571
Grotz WH, Mundinger FA, Rasenack J, Speidel L, Olschewski M, Exner VM, Schollmeyer PJ (1995) Bone loss after kidney transplantation: a longitudinal study in 115 graft recipients. Nephrol Dial Transplant 10:2096–2100
Huang WH, Lee SY, Weng CH, Lai PC (2012) Use of alendronate sodium (Fosamax) to ameliorate osteoporosis in renal transplant patients: a case-control study. PLoS One 7:e48481
Schwarz C, Mitterbauer C, Heinze G, Woloszczuk W, Haas M, Oberbauer R (2004) Nonsustained effect of short-term bisphosphonate therapy ob bone turnover three years after renal transplantation. Kidney Int 65:304–309
Falkiewicz K, Boratyńska M, Zmonarski SC, Milewicz A, Patrzalek D, Biecek P, Klinger M (2009) Evolution of bone disease at 2 years after transplantation: a single-center study. Transplant Proc 41:3063–3066
Jeffrey JR, Leslie WD, Karpinski ME, Nickerson PW, Rush DN (2003) Prevalence and treatment of decreased bone density in renal transplant recipients: a randomized prospective trial of calcitriol versus alendronate. Transplantation 76:1498–1502
Moreno J, Torregrosa JV, Pons F, Campistol JM, Martinez de Osaba MJ, Oppenheimer F (1999) Bone mineral density after renal transplantation: long-term follow-up. Transplant Proc 31:2322–2323
Marcén R, Caballero C, Pascual J, Teruel JL, Tenorio M, Ocaña J, Villafruela JJ, Burgos FJ, Fernández AM, Muriel A, Ortuño J (2006) Lumbar bone mineral density in renal transplant patients on neoral and tacrolimus: a four-year prospective study. Transplantation 81:826–831
Naylor KL, Garg AX, Hodsman AB, Rush DN, Leslie WD (2014) Long-term changes in bone mineral density in kidney transplant recipients. Transplantation 98:1279–1285
Palmer SC, Strippoli GFM, McGregor DO (2005) Interventions for prevention of bone disease in kidney transplant recipients: a systematic review of randomized controlled trials. Am J Kidney Dis 45:638–649
Giannini S, D’Angelo A, Carraro G, Nobile M, Rigotti P, Bonfante L, Marchini F, Zaninotto M, Dalle Carbonare L, Sartori L, Crepaldi G (2001) Alendronate prevents further bone loss in renal transplant recipients. J Bone Miner Res 16:2111–2117
Koc M, Tuglular S, Arikan H, Ozener C, Akoglu E (2002) Alendronate increases bone mineral density in long-term renal transplant recipients. Transplant Proc 34:2111–2113
Cueto-Manzano AM, Konel S, Freemont AJ, Adams JE, Mawer B, Gokal R, Hutchison AJ (2000) Effect of 1,25-dihydroxyvitamin D3 and calcium carbonate on bone loss associated with long-term renal transplantation. Am J Kidney Dis 35:227–236
Torregrosa JV, Moreno A, Guitierrez A, Vidal S, Oppenheimer F (2003) Alendronate for treatment of renal transplant patients with osteoporosis. Transplant Proc 35:1393–1395
Okamoto M, Yamanaka S, Yoshimoto W, Shigematsu T (2014) Alendronate as an effective treatment for bone loss and vascular calcification in kidney transplant recipients. J Transplant 2014:269613. doi:10.1155/2014/269613
Torregrosa JV, Fuster D, Pedroso S, Dieckmann F, Campistol JM, Rubi S, Oppenheimer F (2007) Weekly risedronate in kidney transplant patients with osteoporosis. Transplant Int 8:708–711
Trabulus S, Altiparmak MR, Apaydin S, Serdengecti K, Sariyar M (2008) Treatment of renal transplant recipients with low bone mineral density: a randomized prospective trial of alendronate, alfacalcidol, and alendronate combined with alfacalcidol. Transplant Proc 40:160–166
Grotz WH, Rump LC, Niessen A, Schmidt-Gayk H, Reichelt A, Kirste G, Olschewski M, Schollmeyer PJ (1998) Treatment of osteopenia and osteoporosis after kidney transplantation. Transplantation 66:1004–1008
Eisman JA, Civitelli R, Adami S, Czerwinski E, Recknor C, Prince R, Reginster JY, Zaidi M, Felsenberg D, Hughes C, Mairon N, Masanauskaite D, Reid DM, Delmas PD, Recker RR (2008) Efficacy and tolerability of intravenous ibandronate injections in postmenopausal osteoporosis: 2-year results from the DIVA study. J Rheumatol 35:488–497
Conley E, Muth B, Samaniego M, Lotfi M, Voss B, Armbrust M, Pirsch J, Djamali A (2008) Bisphosphonates and bone fractures in long-term kidney transplant recipients. Transplantation 86:231–237
Horber FF, Casez JP, Steiger U, Czerniak A, Montandon A, Jaeger P (1994) Changes in bone mass early after kidney transplantation. J Bone Miner Res 9:1–9
Almond MK, Kwan JT, Evans K, Cunnungham J (1994) loss of regional bone mineral density in the first 12 months following renal transplantation. Nephron 66:52–57
Tauchmanova L, Carrano R, Sabbatini M, De Rosa M, Orio F, Palomba S, Cascella T, Lombardi G, Federico S, Colao A (2004) Hypothalamic-pituitary-gonadal axis function after successful kidney transplantation in men and women. Hum Reprod 19:867–873
Marcén R, Caballero C, Galeano C, Pascual J, Ocaña J, Tenorio M, Echarri R, Tabernero G, Villafruela JJ, Burgos FJ, Ortuño J (2005) Lumbar bone mineral density after kidney transplantation: a three-year prospective study. Transplant Proc 37:1466–1467
Cruz DN, Brickel HM, Wysolmerski JJ, Gundberg CG, Simpson CA, Kliger AS, Lorber MI, Basadonna GP, Friedman AL, Insogna KL, Bia MJ (2002) Treatment of osteoporosis and osteopenia in long-term renal transplant patients with alendronate. Am J Transplant 2:62–67
Lan G, Peng X, Xie X, Peng F, Wanf Y, Yu S (2008) Alendronate is effective to treat bone loss in renal transplantation recipients. Transplant Proc 40:3496–3498
Cruz DN, Wysolmerski JJ, Brickel HM, Gundberg CG, Simpson CA, Mitnick MA, Kliger AS, Lorber MI, Basadonna GP, Friedman AL, Insogna KL, Bia MJ (2001) Parameters of high bone-turnover predict bone loss in renal transplant patients: a longitudinal study. Transplantation 72:83–88
KDIGO (2009) Clinical practice guideline for the care of kidney transplant recipients. Am J Transplant 9(suppl 3):S93–S96
Author contribution
Frank-Peter Tillmann designed the study, performed the statistical analyses, and drafted the manuscript. Michael Schmitz helped to collect the data and drafted the manuscript. Marcus Jäger and Rüdiger Krauspe conceived the study and helped to draft the manuscript. Lars-Christian Rump conceived the study, participated in its design and coordination and helped to draft the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any conflicts of interest to declare.
Ethical standard
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Tillmann, F.P., Schmitz, M., Jäger, M. et al. Ibandronate in stable renal transplant recipients with low bone mineral density on long-term follow-up. Int Urol Nephrol 48, 279–286 (2016). https://doi.org/10.1007/s11255-015-1133-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-1133-7