Abstract
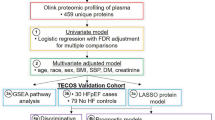
Early prediction of significant morbidity or mortality in patients with acute ST-segment elevation myocardial infarction (STEMI) represents an unmet clinical need. In phenotypically matched population of 139 STEMI patients (72 cases, 67 controls) treated with primary percutaneous coronary intervention, we explored associations between a 24-h relative change from baseline in the concentration of 91 novel biomarkers and the composite outcome of death, heart failure, or shock within 90 days. Additionally, we used random forest models to predict the 90-day outcomes. After adjustment for false discovery rate, the 90-day composite was significantly associated with concentration changes in 14 biomarkers involved in various pathophysiologic processes including: myocardial fibrosis/remodeling (collagen alpha-1, cathepsin Z, metalloproteinase inhibitor 4, protein tyrosine phosphatase subunits), inflammation, angiogenesis and signaling (interleukin 1 and 2 subunits, growth differentiation factor 15, galectin 4, trefoil factor 3), bone/mineral metabolism (osteoprotegerin, matrix extracellular phosphoglycoprotein and tartrate-resistant acid phosphatase), thrombosis (tissue factor pathway inhibitor) and cholesterol metabolism (LDL-receptor). Random forest models suggested an independent association when inflammatory markers are included in models predicting the outcomes within 90 days. Substantial heterogeneity is apparent in the early proteomic responses among patients with acutely reperfused STEMI patients who develop death, heart failure or shock within 90 days. These findings suggest the need to consider synergistic multi-biomarker strategies for risk stratification and to inform future development of novel post-myocardial infarction therapies.

Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Code availability
Assay characteristics including coefficients of variation and calibration are publicly available (www.olink.com/products/cvd-iii-panel). For all statistical analyses except the random forest model, SAS (version 9.4; SAS Institute, Cary, NC) was used; the package randomForest and R statistical software (version 3.5) were used for the random forest analysis.
References
Velagaleti RS, Pencina MJ, Murabito JM et al (2008) Long-term trends in the incidence of heart failure after myocardial infarction. Circulation 118:2057–2062. https://doi.org/10.1161/CIRCULATIONAHA.108.784215
Ezekowitz JA, Kaul P, Bakal JA et al (2009) Declining in-hospital mortality and increasing heart failure incidence in elderly patients with first myocardial infarction. J Am Coll Cardiol 53:13–20. https://doi.org/10.1016/j.jacc.2008.08.067
Granger CB, Goldberg RJ, Dabbous O et al (2003) Predictors of hospital mortality in the global registry of acute coronary events. Arch Intern Med 163:2345–2353. https://doi.org/10.1001/archinte.163.19.2345
Morrow DA, Antman EM, Charlesworth A et al (2000) TIMI risk score for ST-elevation myocardial infarction: a convenient, bedside, clinical score for risk assessment at presentation: an intravenous nPA for treatment of infarcting myocardium early II trial substudy. Circulation 102:2031–2037. https://doi.org/10.1161/01.CIR.102.17.2031
McAllister DA, Halbesma N, Carruthers K et al (2015) GRACE score predicts heart failure admission following acute coronary syndrome. Eur Heart J Acute Cardiovasc Care 4:165–171. https://doi.org/10.1177/2048872614542724
Truong QA, Cannon CP, Zakai NA et al (2009) Thrombolysis in myocardial infarction (TIMI) risk index predicts long-term mortality and heart failure in patients with ST-elevation myocardial infarction in the TIMI 2 clinical trial. Am Heart J 157:673–679. https://doi.org/10.1016/j.ahj.2008.12.010
Vasan RS (2006) Biomarkers of cardiovascular disease: molecular basis and practical considerations. Circulation 113:2335–2362. https://doi.org/10.1161/CIRCULATIONAHA.104.482570
Grabowski M, Filipiak KJ, Malek LA et al (2007) Admission B-type natriuretic peptide assessment improves early risk stratification by Killip classes and TIMI risk score in patients with acute ST elevation myocardial infarction treated with primary angioplasty. Int J Cardiol 115:386–390. https://doi.org/10.1016/j.ijcard.2006.04.038
Klingenberg R, Aghlmandi S, Räber L et al (2018) Improved risk stratification of patients with acute coronary syndromes using a combination of hsTnT, NT-proBNP and hsCRP with the GRACE score. Eur Heart J Acute Cardiovasc Care 7:129–138. https://doi.org/10.1177/2048872616684678
van Diepen S, Newby LK, Lopes RD et al (2013) Prognostic relevance of baseline pro- and anti-inflammatory markers in STEMI: An APEX AMI substudy. Int J Cardiol 168:2127–2133. https://doi.org/10.1016/j.ijcard.2013.01.004
O’Donoghue ML, Morrow DA, Cannon CP et al (2016) Multimarker risk stratification in patients with acute myocardial infarction. J Am Heart Assoc 5:e002586. https://doi.org/10.1161/JAHA.115.002586
Tromp J, Westenbrink BD, Ouwerkerk W et al (2018) Identifying pathophysiological mechanisms in heart failure with reduced versus preserved ejection fraction. J Am Coll Cardiol 72:1081–1090. https://doi.org/10.1016/j.jacc.2018.06.050
Armstrong PW, Adams PX, Al-Khalidi HR et al (2005) Assessment of pexelizumab in acute myocardial infarction (APEX AMI): a multicenter, randomized, double-blind, parallel-group, placebo-controlled study of pexelizumab in patients with acute myocardial infarction undergoing primary percutaneous coronary intervention. Am Heart J 149:402–407. https://doi.org/10.1016/j.ahj.2004.12.015
Armstrong PW, Bett N, Brieger D et al (2007) PexeLizumab for Acute ST-elevation myocardial infarction in patients undergoing primary percutaneous coronary intervention: a randomized controlled trial. JAMA 297:43–51. https://doi.org/10.1001/jama.297.1.43
Shavadia JS, Granger CB, Alemayehu W et al (2020) High-throughput targeted proteomics discovery approach and spontaneous reperfusion in ST-segment elevation myocardial infarction. Am Heart J 220:137–144. https://doi.org/10.1016/j.ahj.2019.09.015
Assarsson E, Lundberg M, Holmquist G et al (2014) Homogenous 96-plex PEA immunoassay exhibiting high sensitivity, specificity, and excellent scalability. PLoS ONE 9:e95192. https://doi.org/10.1371/journal.pone.0095192
Lee EW, Wei LJ, Amato DA, Leurgans S (1992) Cox-type regression analysis for large numbers of small groups of correlated failure time observations. Survival analysis: state of the art. Springer, Dordrecht, pp 237–247
Breiman L (2001) Random forests. Mach Learn 45:5–32. https://doi.org/10.1023/A:1010933404324
Ferreira JP, Verdonschot J, Wang P et al (2021) Proteomic and mechanistic analysis of spironolactone in patients at risk for HF. JACC Heart Fail 9:268–277. https://doi.org/10.1016/j.jchf.2020.11.010
Prabhu SD, Frangogiannis NG (2016) The biological basis for cardiac repair after myocardial infarction. Circ Res 119:91–112. https://doi.org/10.1161/CIRCRESAHA.116.303577
Fraccarollo D, Galuppo P, Bauersachs J, Ertl G (2002) Collagen accumulation after myocardial infarction: Effects of ETA receptor blockade and implications for early remodeling. Cardiovasc Res 54:559–567. https://doi.org/10.1016/S0008-6363(02)00256-0
Yin X, Subramanian S, Hwang SJ et al (2014) Protein biomarkers of new-onset cardiovascular disease: prospective study from the systems approach to biomarker research in cardiovascular disease initiative. Arterioscler Thromb Vasc Biol 34:939–945. https://doi.org/10.1161/ATVBAHA.113.302918
Fraccarollo D, Galuppo P, Schraut S et al (2008) Immediate mineralocorticoid receptor blockade improves myocardial infarct healing by modulation of the inflammatory response. Hypertension 51:905–914. https://doi.org/10.1161/HYPERTENSIONAHA.107.100941
Murakami M, Kusachi S, Nakahama M et al (1998) Expression of the α1 and α2 chains of type IV collagen in the infarct zone of rat myocardial infarction. J Mol Cell Cardiol 30:1191–1202. https://doi.org/10.1006/jmcc.1998.0684
Querejeta R, López B, González A et al (2004) Increased collagen type I synthesis in patients with heart failure of hypertensive origin: relation to myocardial fibrosis. Circulation 110:1263–1268. https://doi.org/10.1161/01.CIR.0000140973.60992.9A
Burke RM, Lighthouse JK, Mickelsen DM, Small EM (2019) Sacubitril/valsartan decreases cardiac fibrosis in left ventricle pressure overload by restoring PKG signaling in cardiac fibroblasts. Circ Hear Fail 12:e005565. https://doi.org/10.1161/CIRCHEARTFAILURE.118.005565
Bartko PE, Dal-Bianco JP, Guerrero JL et al (2017) Effect of losartan on mitral valve changes after myocardial infarction. J Am Coll Cardiol 70:1232–1244. https://doi.org/10.1016/j.jacc.2017.07.734
Vidak E, Javoršek U, Vizovišek M, Turk B (2019) Cysteine cathepsins and their extracellular roles: shaping the microenvironment. Cells 8:264. https://doi.org/10.3390/cells8030264
Nguyen TD, Schwarzer M, Schrepper A et al (2018) Increased protein tyrosine phosphatase 1B (PTP1B) activity and cardiac insulin resistance precede mitochondrial and contractile dysfunction in pressure-overloaded hearts. J Am Heart Assoc 7:e008865. https://doi.org/10.1161/JAHA.118.008865
Bouwens E, Brankovic M, Mouthaan H et al (2019) Temporal patterns of 14 blood biomarker candidates of cardiac remodeling in relation to prognosis of patients with chronic heart failure—the bio-SHiFT study. J Am Heart Assoc 8:e009555. https://doi.org/10.1161/JAHA.118.009555
Liu CL, Guo J, Zhang X et al (2018) Cysteine protease cathepsins in cardiovascular disease: from basic research to clinical trials. Nat Rev Cardiol 15:351–370. https://doi.org/10.1038/s41569-018-0002-3
Buckley LF, Abbate A (2018) Interleukin-1 blockade in cardiovascular diseases: a clinical update. Eur Heart J 39:2063–2069. https://doi.org/10.1093/eurheartj/ehy128
Toldo S, Van Tassell BW, Abbate A (2017) Interleukin-1 blockade in acute myocardial infarction and heart failure: getting closer and closer. JACC 2:431–433. https://doi.org/10.1016/j.jacbts.2017.07.006
Shang L, Feng M, Zhou X, Tang B (2019) Growth differentiation factor 15: a promising prognostic stratification biomarker in patients with acute coronary syndrome. Int J Cardiol 297:16. https://doi.org/10.1016/j.ijcard.2019.08.007
Qamar A, Giugliano RP, Bohula EA et al (2019) Biomarkers and clinical cardiovascular outcomes with ezetimibe in the IMPROVE-IT trial. J Am Coll Cardiol 74:1057–1068. https://doi.org/10.1016/j.jacc.2019.06.038
Bonaca MP, Morrow DA, Braunwald E et al (2011) Growth differentiation factor-15 and risk of recurrent events in patients stabilized after acute coronary syndrome: observations from PROVE IT-TIMI 22. Arterioscler Thromb Vasc Biol 31:203–210. https://doi.org/10.1161/ATVBAHA.110.213512
Stenemo M, Nowak C, Byberg L et al (2018) Circulating proteins as predictors of incident heart failure in the elderly. Eur J Heart Fail 20:55–62. https://doi.org/10.1002/ejhf.980
Gordon KJ, Blobe GC (2008) Role of transforming growth factor-β superfamily signaling pathways in human disease. Biochim Biophys Acta 1782:197–228. https://doi.org/10.1016/j.bbadis.2008.01.006
Meijers WC, Van Der Velde AR, Pascual-Figal DA, De Boer RA (2015) Galectin-3 and post-myocardial infarction cardiac remodeling. Eur J Pharmacol 763:115–121. https://doi.org/10.1016/j.ejphar.2015.06.025
Mosleh W, Chaudhari MR, Sonkawade S et al (2018) The therapeutic potential of blocking galectin-3 expression in acute myocardial infarction and mitigating inflammation of infarct region: a clinical outcome-based translational study. Biomark Insights 13:1177271918771969. https://doi.org/10.1177/1177271918771969
Sharma UC, Mosleh W, Chaudhari MR et al (2017) Myocardial and serum galectin-3 expression dynamics marks post-myocardial infarction cardiac remodelling. Heart Lung Circ 26:736–745. https://doi.org/10.1016/j.hlc.2016.11.007
Erkol A, Oduncu V, Pala S et al (2012) Plasma osteoprotegerin level on admission is associated with no-reflow phenomenon after primary angioplasty and subsequent left ventricular remodeling in patients with acute ST-segment elevation myocardial infarction. Atherosclerosis 221:254–259. https://doi.org/10.1016/j.atherosclerosis.2011.12.031
Pedersen S, Mogelvang R, Bjerre M et al (2012) Osteoprotegerin predicts long-term outcome in patients with st-segment elevation myocardial infarction treated with primary percutaneous coronary intervention. Cardiol 123:31–38. https://doi.org/10.1159/000339880
Andersen GØ, Knudsen EC, Aukrust P et al (2011) Elevated serum osteoprotegerin levels measured early after acute ST-elevation myocardial infarction predict final infarct size. Heart 97:460–465. https://doi.org/10.1136/hrt.2010.206714
Fuernau G, Zaehringer S, Eitel I et al (2013) Osteoprotegerin in ST-elevation myocardial infarction: prognostic impact and association with markers of myocardial damage by magnetic resonance imaging. Int J Cardiol 167:2134–2139. https://doi.org/10.1016/j.ijcard.2012.05.101
Ueland T, Dahl CP, Kjekshus J et al (2011) Osteoprotegerin predicts progression of chronic heart failure: results from CORONA. Circ Heart Fail 4:145–152. https://doi.org/10.1161/CIRCHEARTFAILURE.110.957332
Chirinos JA, Orlenko A, Zhao L et al (2020) Multiple plasma biomarkers for risk stratification in patients with heart failure and preserved ejection fraction. J Am Coll Cardiol 75:1281–1295. https://doi.org/10.1016/j.jacc.2019.12.069
Røysland R, Bonaca MP, Omland T et al (2012) Osteoprotegerin and cardiovascular mortality in patients with non-ST elevation acute coronary syndromes. Heart 98:786–791. https://doi.org/10.1136/heartjnl-2011-301260
Ueland T, Yndestad A, Øie E et al (2005) Dysregulated osteoprotegerin/RANK ligand/RANK axis in clinical and experimental heart failure. Circulation 111:2461–2468. https://doi.org/10.1161/01.CIR.0000165119.62099.14
Bayes-Genis A, Núñez J, Zannad F et al (2017) The PCSK9-LDL receptor axis and outcomes in heart failure: BIOSTAT-CHF subanalysis. J Am Coll Cardiol 70:2128–2136. https://doi.org/10.1016/j.jacc.2017.08.057
Acknowledgements
The authors would like to thank Lisa Soulard of the Canadian VIGOUR Centre for her editorial assistance and preparation of the manuscript submission.
Funding
This work was supported by the Innovation and Investment Award Duke Clinical Research Institute, Canadian VIGOUR Center and Inova Heart Institute.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. deFilippi received grant support from Roche Diagnostics, Siemens Heathineers and has served as a consultant for Roche Diagnostics, Siemens Heathineers, Ortho Clinical, Abbott Diagnostics, Fiji Rebio, Metanomics, Quidel, UpToDate, and WebMD. Dr. Granger received grant support and consulting fees from Boehringer Ingelheim, Bayer, Bristol Myers Squibb, Daiichi Sankyo, Janssen Pharmaceutica, Pfizer, GlaxoSmithKline, and Sanofi, consulting fees and lecture fees from Boston Scientific, grant support from Merck, and consulting fees from AstraZeneca, Armetheon, Eli Lilly, Gilead, Hoffmann-La Roche, Medtronic, Takeda, and the Medicine Company. Dr. Povsic has received grants from Baxter Healthcare, Caladrius Biosciences, Capricor, CSL Behring, and Janssen Pharmaceuticals; and personal fees from Eli Lilly, NovoNordisk, and Pluristem. Dr. Armstrong has served as a consultant for Bayer and Merck, and received research grants from CSL, Boehringer Ingelheim, Bayer, and Merck. All other authors have no disclosures.
Ethical approval
The study was approved by all enrolling hospital research ethics boards and conforms with the Declaration of Helsinki.
Consent to participate
All patients provided informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shavadia, J.S., Alemayehu, W., deFilippi, C. et al. Novel multi-marker proteomics in phenotypically matched patients with ST-segment myocardial infarction: association with clinical outcomes. J Thromb Thrombolysis 53, 841–850 (2022). https://doi.org/10.1007/s11239-021-02582-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-021-02582-5