Abstract
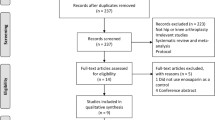
In the last decade, major advances in venous thromboembolism (VTE) prophylaxis in orthopaedic surgery have included the development of new anticoagulants that are poised to replace low molecular weight heparins (LMWHs) and improvements in operative and perioperative care that have likely led to a decline in the rates of symptomatic VTE and mortality independent of anticoagulant use. A systematic review of the literature was performed to identify phase III randomized controlled trials of VTE prevention that compared new anticoagulants (fondaparinux, rivaroxaban, dabigatran, apixaban) with LMWH (enoxaparin) in major elective orthopaedic surgery. Our aims were to obtain best estimates of the rates of patient important events (symptomatic VTE, mortality, and bleeding) in contemporary trials of VTE prevention, and to consider the implications of these contemporary rates for clinical practice and future research. Fourteen studies, which enrolled 40,285 patients, were included in the analyses. The combined median rates (ranges) for all five anticoagulants for symptomatic VTE and mortality to the end of follow-up were 0.99 % (0.15–2.58 %) and 0.26 % (0–0.92 %) respectively, whereas the median rate (range) of clinically important bleeding was 3.44 % (2.25–7.74 %). In contemporary trials of anticoagulants, the rates of symptomatic VTE and mortality are low, but the rates of clinically important post-operative bleeding remain relatively high. Based on these results, we propose that approaches that minimize bleeding without substantially reducing efficacy merit investigation, particularly if improvement in surgical and perioperative care have also resulted in falling baseline patient important VTE rates independent of anticoagulant use.




Similar content being viewed by others
References
MacLean S, Mulla S, Akl EA, Jankowski M, Vandvik PO, Ebrahim S, McLeod S, Bhatnagar N, Guyatt GH (2012) Patient values and preferences in decision making for antithrombotic therapy: a systematic review: antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 141(2 Suppl):e1S–e23S. doi:10.1378/chest.11-2290
Collins R, Scrimgeour A, Yusuf S, Peto R (1988) Reduction in fatal pulmonary embolism and venous thrombosis by perioperative administration of subcutaneous heparin. Overview of results of randomized trials in general, orthopedic, and urologic surgery. N Engl J Med 318(18):1162–1173. doi:10.1056/nejm198805053181805
Falck-Ytter Y, Francis CW, Johanson NA, Curley C, Dahl OE, Schulman S, Ortel TL, Pauker SG, Colwell JCW (2012) Prevention of VTE in orthopedic surgery patients: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians evidence-based clinical practice guidelines. CHEST J 141 (2_suppl):e278S–e325S. doi:10.1378/chest.11-2404
Guyatt GH, Eikelboom JW, Gould MK, Garcia DA, Crowther M, Murad MH, Kahn SR, Falck-Ytter Y, Francis CW, Lansberg MG, Akl EA, Hirsh J (2012) Approach to outcome measurement in the prevention of thrombosis in surgical and medical patients: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians evidence-based clinical practice guidelines. CHEST J 141 (2_suppl):e185S–e194S. doi:10.1378/chest.11-2289
Guideline on clinical investigation of medicinal products for the prevention of venous thromboembolism (VTE) in patients undergoing high VTE-risk surgery. (2013) European Medicines Agency. http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2013/05/WC500143764.pdf. Accessed 7 Oct 2014
Lassen MR, Raskob GE, Gallus A, Pineo G, Chen D, Portman RJ (2009) Apixaban or enoxaparin for thromboprophylaxis after knee replacement. N Engl J Med 361(6):594–604. doi:10.1056/NEJMoa0810773
Lassen MR, Raskob GE, Gallus A, Pineo G, Chen D, Hornick P (2010) Apixaban versus enoxaparin for thromboprophylaxis after knee replacement (ADVANCE-2): a randomised double-blind trial. Lancet 375(9717):807–815. doi:10.1016/s0140-6736(09)62125-5
Lassen MR, Gallus A, Raskob GE, Pineo G, Chen D, Ramirez LM (2010) Apixaban versus enoxaparin for thromboprophylaxis after hip replacement. N Engl J Med 363(26):2487–2498. doi:10.1056/NEJMoa1006885
Lassen MR, Bauer KA, Eriksson BI, Turpie AG (2002) Postoperative fondaparinux versus preoperative enoxaparin for prevention of venous thromboembolism in elective hip-replacement surgery: a randomised double-blind comparison. Lancet 359(9319):1715–1720. doi:10.1016/s0140-6736(02)08652-x
Bauer KA, Eriksson BI, Lassen MR, Turpie AG (2001) Fondaparinux compared with enoxaparin for the prevention of venous thromboembolism after elective major knee surgery. N Engl J Med 345(18):1305–1310. doi:10.1056/NEJMoa011099
Turpie AG, Bauer KA, Eriksson BI, Lassen MR (2002) Postoperative fondaparinux versus postoperative enoxaparin for prevention of venous thromboembolism after elective hip-replacement surgery: a randomised double-blind trial. Lancet 359(9319):1721–1726. doi:10.1016/s0140-6736(02)08648-8
Eriksson BI, Borris LC, Friedman RJ, Haas S, Huisman MV, Kakkar AK, Bandel TJ, Beckmann H, Muehlhofer E, Misselwitz F, Geerts W (2008) Rivaroxaban versus enoxaparin for thromboprophylaxis after hip arthroplasty. N Engl J Med 358(26):2765–2775. doi:10.1056/NEJMoa0800374
Kakkar AK, Brenner B, Dahl OE, Eriksson BI, Mouret P, Muntz J, Soglian AG, Pap AF, Misselwitz F, Haas S (2008) Extended duration rivaroxaban versus short-term enoxaparin for the prevention of venous thromboembolism after total hip arthroplasty: a double-blind, randomised controlled trial. Lancet 372(9632):31–39. doi:10.1016/s0140-6736(08)60880-6
Lassen MR, Ageno W, Borris LC, Lieberman JR, Rosencher N, Bandel TJ, Misselwitz F, Turpie AG (2008) Rivaroxaban versus enoxaparin for thromboprophylaxis after total knee arthroplasty. N Engl J Med 358(26):2776–2786. doi:10.1056/NEJMoa076016
Turpie AG, Lassen MR, Davidson BL, Bauer KA, Gent M, Kwong LM, Cushner FD, Lotke PA, Berkowitz SD, Bandel TJ, Benson A, Misselwitz F, Fisher WD (2009) Rivaroxaban versus enoxaparin for thromboprophylaxis after total knee arthroplasty (RECORD4): a randomised trial. Lancet 373(9676):1673–1680. doi:10.1016/s0140-6736(09)60734-0
Ginsberg JS, Davidson BL, Comp PC, Francis CW, Friedman RJ, Huo MH, Lieberman JR, Muntz JE, Raskob GE, Clements ML, Hantel S, Schnee JM, Caprini JA (2009) Oral thrombin inhibitor dabigatran etexilate versus North American enoxaparin regimen for prevention of venous thromboembolism after knee arthroplasty surgery. J Arthroplasty 24(1):1–9. doi:10.1016/j.arth.2008.01.132
Eriksson BI, Dahl OE, Rosencher N, Kurth AA, van Dijk CN, Frostick SP, Kalebo P, Christiansen AV, Hantel S, Hettiarachchi R, Schnee J, Buller HR (2007) Oral dabigatran etexilate vs. subcutaneous enoxaparin for the prevention of venous thromboembolism after total knee replacement: the RE-MODEL randomized trial. J Thromb Haemost 5(11):2178–2185. doi:10.1111/j.1538-7836.2007.02748.x
Eriksson BI, Dahl OE, Rosencher N, Kurth AA, van Dijk CN, Frostick SP, Prins MH, Hettiarachchi R, Hantel S, Schnee J, Buller HR (2007) Dabigatran etexilate versus enoxaparin for prevention of venous thromboembolism after total hip replacement: a randomised, double-blind, non-inferiority trial. Lancet 370(9591):949–956. doi:10.1016/s0140-6736(07)61445-7
Eriksson BI, Dahl OE, Huo MH, Kurth AA, Hantel S, Hermansson K, Schnee JM, Friedman RJ (2011) Oral dabigatran versus enoxaparin for thromboprophylaxis after primary total hip arthroplasty (RE-NOVATE II*). A randomised, double-blind, non-inferiority trial. Thromb Haemost 105(4):721–729. doi:10.1160/th10-10-0679
Berger J, Eikelboom JW, Quinlan DJ, Guyatt G, Büller HR, Sobieraj-Teague M, Harrington RA, Hirsh J (2013) Venous thromboembolism prophylaxis: do trial results enable clinicians and patients to evaluate whether the benefits justify the risk? Proceedings of an Ad Hoc Working Group Meeting. J Thromb Haemost 11 (4):778–782. doi:10.1111/jth.4900
Quinlan DJ, Eikelboom JW, Dahl OE, Eriksson BI, Sidhu PS, Hirsh J (2007) Association between asymptomatic deep vein thrombosis detected by venography and symptomatic venous thromboembolism in patients undergoing elective hip or knee surgery. J Thromb Haemost 5(7):1438–1443. doi:10.1111/j.1538-7836.2007.02571.x
Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJ, Gavaghan DJ, McQuay HJ (1996) Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 17(1):1–12
Eriksson BI, Bauer KA, Lassen MR, Turpie AG (2001) Fondaparinux compared with enoxaparin for the prevention of venous thromboembolism after hip-fracture surgery. N Engl J Med 345(18):1298–1304. doi:10.1056/NEJMoa011100
Adam SS, McDuffie JR, Lachiewicz PF, Ortel TL, Williams JJW (2013) Comparative effectiveness of new oral anticoagulants and standard thromboprophylaxis in patients having total hip or knee replacement: a systematic review. Ann Intern Med 159(4):275–284. doi:10.7326/0003-4819-159-4-201308200-00008
Turpie AG, Bauer KA, Eriksson BI, Lassen MR (2002) Fondaparinux versus enoxaparin for the prevention of venous thromboembolism in major orthopedic surgery: a meta-analysis of four randomized double-blind studies. Arch Intern Med 162(16):1833–1840
Anderson F, Hirsh J, White K, Fitzgerald R (2003) Temporal trends in prevention of venous thromboembolism following primary total hip or knee arthroplasty 1996–2001: findings from the Hip and Knee Registry. Chest 124(Suppl 6):349–356
Bjornara B, Gudmundsen T, Dahl O (2006) Frequency and timing of clinical venous thromboembolism after major joint surgery. J Bone Joint Surg Br 88:386–391
Lapidus L, Ponzer S, Pettersson H, de Bri E (2013) Symptomatic venous thromboembolism and mortality in orthopaedic surgery—an observational study of 45,968 consecutive procedures. BMC Musculoskelet Disord 14(1):177
Leclerc J, Gent M, Hirsh J, Geerts W, Ginsberg J (1998) The incidence of symptomatic venous thromboembolism during and after prophylaxis with enoxaparin: a multi-institutional cohort study of patients who underwent hip or knee arthroplasty. Canadian collaborative group. Arch Intern Med 158:873–878
Samama C, Ravaud P, Parent F, Barre J, Mertl P, Mismetti P (2007) Epidemiology of venous thromboembolism after lower limb arthroplasty: the FOTO study. J Thromb Haemost 5:2360–2367
White R, Romano P, Zhou H, Rodrigo J, Bargar W (1998) Incidence and time course of thromboembolic outcomes following total hip or knee arthroplasty. Arch Intern Med 158:1525–1531
White R, Zhou H, Romano P (2003) Incidence of symptomatic venous thromboembolism after different elective or urgent surgical procedures. Thromb Haemost 90:446–455
Turpie AGG, Haas S, Kreutz R, Mantovani LG, Pattanayak CW, Holberg G, Jamal W, Schmidt A, van Eickels M, Lassen MR (2014) A non-interventional comparison of rivaroxaban with standard of care for thromboprophylaxis after major orthopaedic surgery in 17,701 patients with propensity score adjustment. Thromb Haemost 111(1):94–102. doi:10.1160/TH13-08-0666
Murray DW, Britton AR, Bulstrode CJK (1996) Thromboprophylaxis and death after total hip replacement. J Bone Joint Surg, Br 78-B(6):863–870
Hunt LP, Ben-Shlomo Y, Clark EM, Dieppe P, Judge A, MacGregor AJ, Tobias JH, Vernon K, Blom AW (2013) 90-day mortality after 409096 total hip replacements for osteoarthritis, from the National Joint Registry for England and Wales: a retrospective analysis. Lancet 382(9898):1097–1104
Kwong LM, Kistler KD, Mills R, Wildgoose P, Klaskala W (2012) Thromboprophylaxis, bleeding and post-operative prosthetic joint infection in total hip and knee arthroplasty: a comprehensive literature review. Expert Opin Pharmacother 13(3):333–344. doi:10.1517/14656566.2012.652087
Muntz J, Scott DA, Lloyd A, Egger M (2004) Major bleeding rates after prophylaxis against venous thromboembolism: systematic review, meta-analysis, and cost implications. Int J Technol Assess Health Care 20(4):405–414
Vera-Llonch M, Hagiwara M, Oster G (2006) Clinical and economic consequences of bleeding following major orthopedic surgery. Thromb Res 117(5):569–577. doi:10.1016/j.thromres.2005.04.018
Parvizi J, Ghanem E, Joshi A, Sharkey PF, Hozack WJ, Rothman RH (2007) Does “excessive” anticoagulation predispose to periprosthetic infection? J Arthroplast 22(6 Suppl 2):24–28. doi:10.1016/j.arth.2007.03.007
Sanchez-Ballester J, Smith M, Hassan K, Kershaw S, Elsworth CS, Jacobs L (2005) Wound infection in the management of hip fractures: a comparison between low-molecular weight heparin and mechanical prophylaxis. Acta Orthop Belg 71(1):55–59
Kulshrestha V, Kumar S (2013) DVT prophylaxis after TKA: routine anticoagulation Vs risk screening approach—A randomized study. J Arthroplast. doi:10.1016/j.arth.2013.05.025
Pulmonary Embolism Prevention (PEP) Trial Collaborative Group (2000) Prevention of pulmonary embolism and deep vein thrombosis with low dose aspirin: Pulmonary Embolism Prevention (PEP) trial. Lancet 355(9212):1295–1302
Raskob GE, Hirsh J (2003) Controversies in timing of the first dose of anticoagulant prophylaxis against venous thromboembolism after major orthopedic surgery. Chest 124(6 Suppl):379S–385S
Neumann I, Rada G, Claro JC, Carrasco-Labra A, Thorlund K, Akl EA, Bates SM, Guyatt GH (2012) Oral direct Factor Xa inhibitors versus low-molecular-weight heparin to prevent venous thromboembolism in patients undergoing total hip or knee replacement: a systematic review and meta-analysis. Ann Intern Med 156(10):710–719. doi:10.7326/0003-4819-156-10-201205150-00421
Anderson DR, Dunbar MJ, Bohm ER, Belzile E, Kahn SR, Zukor D, Fisher W, Gofton W, Gross P, Pelet S, Crowther M, MacDonald S, Kim P, Pleasance S, Davis N, Andreou P, Wells P, Kovacs M, Rodger MA, Ramsay T, Carrier M, Vendittoli PA (2013) Aspirin versus low-molecular-weight heparin for extended venous thromboembolism prophylaxis after total hip arthroplasty: a randomized trial. Ann Intern Med 158(11):800–806
Acknowledgment
NCC received an educational grant from the Haematology Society of Australia and New Zealand.
Conflicts of interest
All authors have completed the ICMJE uniform disclosure form at www.icmje.org/coi_disclosure.pdf. JWE has received consulting fees and/or honoraria from Astra-Zeneca, Bayer, Boehringer-Ingelheim, Bristol-Myer-Squibb, Daiichi-Sankyo, Eli-Lilly, Glaxo-Smith-Kline, Pfizer, Janssen, Sanofi-Aventis, and has received grants and/or in-kind support from Astra-Zeneca, Bayer, Boehringer-Ingelheim, Bristol-Myer-Squibb, Glaxo-Smith-Kline, Pfizer, Janssen, Sanofi-Aventis. All other authors declare no competing financial interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chan, N.C., Siegal, D., Lauw, M.N. et al. A systematic review of contemporary trials of anticoagulants in orthopaedic thromboprophylaxis: suggestions for a radical reappraisal. J Thromb Thrombolysis 40, 231–239 (2015). https://doi.org/10.1007/s11239-014-1153-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-014-1153-7