Abstract
This paper studies factors explaining the gender mental health gap using Australian data. We show that men have significantly higher mean outcomes and the left tail of the combined distribution is disproportionately female. Using regression-based decompositions, we examine the degree that both socioeconomic inequalities and life experience account for this phenomenon. We find that disparities in income play a substantial role, and subject to an assumption of exogeneity, would be enough to account for the gender gap amongst individuals with very poor psychological wellbeing. We also examine the mental health effects of various negative life experience, such as the death of a family member or being a victim of violence. At the individual level, these variables have large effect sizes but are not strongly correlated with gender to explain our mental health disparities.
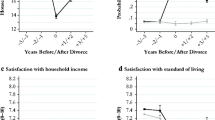
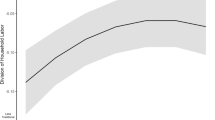
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Understanding the drivers of inequality in mental health is important, because the social and economic cost for individuals at the low end of the poor mental health spectrum can be catastrophic. People who live with acute and chronic mental illness often have significantly higher risk of suicide (Gili et al., 2019; Hoertel et al., 2015) and reduced capacity to engage in productive activities, such as education, work and social interactions (Cornaglia et al., 2015; Chopra, 2009; Christensen et al., 2021; Lu et al., 2009). Additionally, people with mental illness require more healthcare services while healthcare interventions, including medications, social supports and psychological therapies, have been shown to have lower effectiveness for people in lower socioeconomic groups (Beauchamp et al., 2014; Lorant et al., 2003; Rojas-Garcia et al., 2015).
The existing literature on mental health disparities often focuses on the mean differences between genders, overlooking the nuances across the entire distribution of mental health outcomes. While some studies have explored specific factors contributing to the gender mental health gap, such as the role of social norms (Caroli & Weber-Baghdiguian, 2016), dimensions of the self (Rosenfield et al., 2000) or the exposure to work and family stressors (Marchand et al., 2016), relatively less is known about the factors that explain the gender mental health gap beyond the mean. To our knowledge, only Churchill et al. (2020) have examined gender mental health differences at different quantiles, and these authors focused on locus of control as the primary explanatory factor. Most research tends to examine either socioeconomic factors or life experiences in isolation, without considering their interplay and differential impacts on mental health outcomes for men and women (see, e.g., Hashmi et al., 2020; Watson and Osberg, 2017). There remains a notable gap in understanding how economic and life experiences collectively shape this disparity across the entire distribution.
This study bridges the gap by adopting a holistic approach that considers both economic and life experience factors simultaneously and evaluates their distinct contributions to the gender mental health gap across the full distribution of outcomes, with a special focus on the low end. By doing so, we move beyond the traditional focus on mean differences and provide valuable insights for policymakers aiming to develop targeted interventions to reduce mental health disparities and promote mental wellbeing for all individuals, regardless of gender.
We address the research gap by employing econometric models and performing statistical decompositions to contrast two potential explanations for the gender differences in mental health. The first is a socioeconomic account that attributes the metal health gap to differentials in socioeconomic outcomes, while the second is a social, or life-experience explanation that attributes inequalities to differences in exposure to various social experiences. Health inequalities and disparities in economic and social outcomes are mutually linked, via positive and self-reinforcing associations between these various facets of wellbeing (see, e.g., Grossman, 2017; Huguet et al., 2008; Kim and Koh, 2021; Kawachi and Kennedy, 1999; Kulhánová et al., 2014; Li and Powdthavee, 2015). The relationships between health and socioeconomic inequalities are of significant interest to policymakers, as interventions that equalise socioeconomic variables could generate positive spillovers affecting the distribution of public health outcomes (Clark et al., 2008; Clark & D’Ambrosio, 2015; Osmani & Sen, 2003). By examining the full distribution of mental health outcomes, we extend beyond traditional analyses of the mean, providing a more nuanced understanding of the gender gap in mental health.
On average, men and women have different economic and social experiences (Berry & Welsh, 2010; Suter & Miller, 1973). For example, men typically have higher labour market participation rates, longer and less interrupted careers, and greater incomes. Conversely, women often face disadvantages in the paid labor market due to childrearing and other familial responsibilities. Given that these economic factors influence individuals’ psychological wellbeing (Clark et al., 2021; Zimmerman & Katon, 2005), they likely contribute to the gender mental health gap.
Differences in psychological makeup, social networks, and support systems between men and women could also play a role in how they handle adverse life events. Theories, such as those proposed by Bem (1981), suggest that masculinity and femininity are not fixed traits but rather roles that individuals adopt within societal norms. For instance, women are often expected to fulfill caregiving roles, which can increase their exposure to stress and potentially limit their access to personal support networks. The idea that taking a job allows women to mitigate the uncertainties of home life underscores the unique pressures they face (Hochschild, 2018). Moreover, early-life attachment styles, where women tend to be more emotionally responsive and dependent, contrast with men’s tendency towards independence and self-reliance, influencing stress responses throughout life (Bowlby, 1969). Additionally, women are more inclined to seek and receive social support, and there are notable differences in how men and women find satisfaction-women through intimate conversations, while men through companionship and task completion (Cohen & Wills, 1985). These dynamics suggest that men and women may process and react to stress differently.
Furthermore, the nature of life events experienced by men and women varies. For example, women were found to be more likely to experience financial distress than men (Zhou et al., 2023). Boys from disadvantaged families were more likely to have disciplinary issues and lower academic performance than girls from similar backgrounds (Autor et al., 2019). If these experiences occur more frequently for women than men (or vice versa), or have differing effects upon mental wellbeing that are correlated with gender, they may potentially drive health outcome differences.
Our study utilizes recent, high-quality Australian microdata to analyze the gender mental health gap. We reproduce the established result that women have poorer mental health than men on average (Australian Bureau of Statistics, 2021; Berry & Welsh, 2010), and show that they are strongly over-represented amongst individuals with very poor outcomes (i.e., there is a larger percentage of women at the lower end of the mental health distribution). Using regression-based decompositions based upon the Recentered Influence Function (RIF), we then show that socioeconomic variables such as income and employment do indeed play important roles in understanding aggregate outcome gaps. Subject to an assumption of exogeneity, our economic variables are sufficient to explain the entire gender gap amongst individuals with very poor mental health, which was defined as individuals at the bottom 10th quantile of the mental health score distribution. However, not all socioeconomic variables reinforce gender mental health inequalities. For examples, differentials in educational outcomes that favour women partially close the gender mental health gap.
We then turn our attention to the roles played by differing life experiences, such as being divorced, experiencing a death of spouse or child, or having an injured family member, in shaping mental health outcomes. Interestingly, while our life experience variables are extremely potent in predicting psychological health at the individual level, they contribute little to explain male–female differences in mental health. For example, negative life events such as experiencing physical violence have dire consequences for mental health for both men and women, especially for those who already located in the lower quantiles of the mental health distribution. However, the data indicate that these experiences are relatively rare, and not correlated strongly with gender; thus such experience does not explain why men in our panel appear to have better psychological wellbeing.
In addition to negative life experiences being rare events that drive our unexpected results, several potential factors may contribute to these findings. Other underlying risk factors, unrelated to the life experiences we examined, may be influential. For example, biological differences might affect mental health outcomes (HILDA does not collect variables such as blood group, heart rate, or blood pressure for us to control for in our study). Furthermore, differences in reporting or responding to mental illness between genders could contribute to the observed results. For instance, women are more likely to blame themselves when they are victims of violence, potentially exacerbating their mental health issues. Men and women may also perceive and report their mental health symptoms differently, affecting the apparent prevalence and severity of mental health issues in our study. Therefore, while adverse life experiences are crucial for understanding individual mental health trajectories, they do not sufficiently account for the gender gap in mental health within our Australian context.
Our research makes two contributions to the body of literature on health inequality. First, our econometric method goes beyond an analysis of the conditional mean by providing a full-distribution decomposition of psychological wellbeing. This approach allows us to disentangle the relative importance of various factors in driving the observed disparities. Second, to our knowledge, this study is the first that contrasts the impacts of economic and life experiences on gender mental health gap. By considering both sets of factors, policymakers can develop more effective interventions to address mental health disparities, focusing on modifiable factors that contribute to gender differences in mental wellbeing.
The paper is structured as follows. Section 2 describes the dataset and variables of interest. Section 3 describes our unconditional quantile regression models, which are still relatively new in the analysis of inequality, presents our model estimates and uses these models to decompose health inequalities into contributions from covariates. Section 4 suggests policies that might be effective in alleviating very poor mental health, and for closing the gender mental health gap.
2 Data
2.1 The HILDA Dataset
We use data from Release 20 of the Household, Income and Labour Dynamics in Australia (HILDA) survey, which is an ongoing longitudinal study that began in 2001 with an approximately nationally representative sample of Australian households (Watson & Wooden, 2021). HILDA is comparable to the USA’s Panel Study of Income Dynamics (PSID), the British Household Panel Survey (BHPS) or the German Socio-Economic Panel (SOEP), so our results are generalisable. The first wave (2001) comprised 13,969 participants from 7682 households. In 2011, 2153 households (5462 individuals) were added to the panel.
HILDA collects information about the composition of households, income, employment, family relationships, and personal (individual) wellbeing. Individual person questionnaires are administered to every member of the household aged 15 years or older (with parental consent sought before interviewing persons aged under 18 years and living with their parents). All respondents completing an individual questionnaire are also asked to complete a separate self-completion questionnaire (SCQ) about general health and wellbeing, lifestyle and living situation, personal and household finances, job and the workplace, and parenting. We use data from both the household and individual surveys in our analyses.
Our study begins with a comprehensive dataset comprising 410,658 observations. We screen this sample to exclude individuals who did not complete interviews, focusing on the integrity and reliability of our data. This process results in a reduction to 305,143 observations.
Further refining our sample, we exclude participants with negative Mental Health Inventory-5 (MHI-5) scores, which indicated either No SCQ, Multiple Response SCQ, or Refused/Not Stated. This exclusion criterion aim to maintain the quality and relevance of our data, leading to the removal of an additional 31,921 observations. Consequently, our sample size is reduced to 273,222 observations.
Subsequently, we apply restrictions to ensure the meaningfulness of our analyses by focusing on relevant variables such as marital status and life events. This step further narrow our sample to 269,694 observations. Among these refined observations, we identify 887 cases where the after-tax equivalized income was zero. Given the nature of our analysis, which required logarithmic transformation of income, these cases are excluded. This step left us with 268,807 observations, evenly distribute between males (125,870) and females (142,937).
The implementation of multiple imputations address the remaining missing values, enhancing the robustness of our analyses. We document the results of these imputations in the Appendix A, demonstrating that the outcomes derived from the imputed data closely align with those presented in our main text.
2.2 Key Variables
Our analyses employ four variable types and we preview each below. These are the dependent variable (mental health aggregates), a range of economic indicators, a series of life experience markers, and a standard set of demographic controls.
2.2.1 MHI-5 Mental Health Aggregates
We measure individual-level mental health using the MHI-5 subscale of the SF-36 health aggregate. The SF-36 is a commonly used multi-dimensional instrument to measure health outcomes at population level, supported by substantial international research evidence of its responsiveness, validity and reliability in a range of studies (see, e.g., Brazier et al., 1992; Butterworth and Crosier, 2004; Jenkinson et al., 1994; Wu et al., 2023). Specifically, the reliability coefficient for the composite mental health measures was shown to exceed the recommended level of 0.85, with Cronbach’s \(\alpha = 0.95\) (Brazier et al., 1992). This high coefficient indicates the consistency and dependability of the composite scores derived from the mental health assessments, ensuring that our findings on gender differences in mental health are based on robust and reliable measures.
The MHI-5 score was derived following the procedure described in Ware et al. (1994). This is a 0–100 scale designed to be approximately cardinal in interpretation, where greater values are indicative of better outcomes. The five questions used to construct MHI-5 score are (1) been a nervous person, (2) felt so down in the dumps nothing could cheer you up, (3) felt calm and peaceful, (4) felt down, and (4) been a happy person. Each participant was asked to rate how often they had the aforementioned feeling in the past four weeks: (1) All of the time, (2) Most of the time, (3) A good bit of the time, (4) Some of the time, (5) A little of the time, (6) None of the time. The (reversed) answers were then added, subtracting 5, dividing by 25, and multiplying the sum by 100 with 0 implies a serious mental health problem and 100 means very good mental health (Roy & Schurer, 2013). Although MHI-5 includes only a subset of SF-36, its validity and reliability in detecting mental health issues in general population have been validated (see, e.g., Hoeymans et al., 2004; Rumpf et al., 2001; Thorsen et al., 2013).
2.2.2 Economic Variables
We measure the statistical relationships between economic disparities and mental health states using a range of economic indicators, focusing on income, labour force participation and education.Footnote 1
Household income is an indicator of individuals’ access to economic resources. This variable is the sum of all inflows such as labour earnings and government transfers, minus taxes. We then adjust for economies of scale within the household using the “OECD-modified scale”, following the formulaFootnote 2
We opt not to use individual income because household income serves as a better indicator of economic welfare at the individual level. This decision is grounded in the recognition that within households, income is often shared among members, particularly in the case of married couples with children. Consequently, household income emerges as a more relevant and comprehensive measure in capturing the economic wellbeing of individuals (Buhmann et al., 1988).Footnote 3 While we regard household income as the best single measure of individual economic welfare, this variable assumes perfect sharing of income within households, which may result in an overestimate of the welfare of women because in many households, women do not work or earn less than men.
Labour market participation and education levels are included as sequences of dummy variables. Labour force status has three categories: employed, unemployed and not in the labour force, with the last group treated as the reference group. The “not in the labour force” group includes those who perform unpaid work in the home as a primary carer, either for children or for older adults in their family. The highest education level achieved has four categories: certificates and diplomas, undergraduate, postgraduate, and grade 12 or below, with the last group treated as the reference group.
Lastly, we supplement measures of economic wellbeing with quintiles of the socioeconomic indexes for areas SEIFA (Summerfield et al., 2020). The index has been used widely to capture the additional unobserved variation in the distribution of income and wealth that might associate with residential location.
2.2.3 Life Experience
The role of social factors in an individual’s mental health is potentially crucial. Typically, significant life events affect men and women differently, with varying frequencies. For instance, domestic violence is more likely to affect women. Additionally, men and women have different emotional reactions to life experiences, as they prioritize different factors. When men and women encounter distinct rates of life events or experience diverse impacts on their mental well-being, it can contribute to the gender mental health disparity.
A series of life experience markers are used to capture an individuals’ social experiences. These are dummy variables, with a value of 1 indicating that an individual had experienced the given event in the past year. We consider a broad range of these experiences, including death of spouse or child, death of close relative or family member, serious injury or illness to family member, natural disaster that damaged or destroyed home, fire or made redundant, victim of physical violence, close family member detained in jail, and being detained in jail.
2.2.4 Control Variables
We include standard demographic variables, such as marital status, household size, and individual age to control for omitted variable biases. Marital status has three categories: legally married or de facto, divorced/separated, and single; “marital status = single” is then used as the reference group. Marital status is likely to be an important determinant of mental health as it is indicative of an individual’s family support network. Similarly, household size reflects both the presence of a support structure and potential care responsibilities. Age and its square are used to control for trajectories in wellbeing over the lifecycle.
2.3 Descriptive Statistics
Figures 1 and 2 describe the distribution of mental health score MHI-5 by gender. In the 20-year HILDA panel, men have a significantly higher mean MHI-5 score than women in every period of the data (2001–2020, shown in the left panel of Fig. 1). The vertical gaps between the two lines (i.e. differences in means of MHI-5 scores for men and women over time) are relatively constant from one year to the next, indicating that the higher MHI-5 mean score for males is a highly persistent feature in the sample, Additionally, there is a higher variance for women, resulting in a much greater proportion of very low scores.Footnote 4 The percentage of women who have MHI-5 scores of less than or equal to 50 is consistently higher than that of men in each of those years, as shown in the right panel of Fig. 1. Together, these facts imply that the left tail of the MHI-5 distribution for women is always thicker than that for men, as shown in Fig. 2.
Kernel Density of MHI-5 scores, HILDA, 2001–20. Notes The figure depicts kernel densities of MHI-5 scores for men (solid line) and women (dashed line). The densities are estimated with fixed-bandwidth and boundary corrections at 0 and 100. The left figure is the kernel density estimated for men and women in 2020, which is the latest year in our data. The right figure is the kernel density estimate for the pooled sample
Table 1 below provides summary statistics for our variables of interest. We give mean values for men and women in the left and middle columns, with the difference in average outcomes on the right. Variables are grouped by outcome, demographics, economic and life experiences. It is important to note that there are significant differences in mean values for men and women for most variables.
With regards to economic variables, on average, men had significantly higher income than women, with almost 5% more after-tax equivalised annual income. Women were more likely to report being “not in the labour force” compared to men, with around 38% of women reporting not working compared to 26% of men. On the other hand, men were more likely to report being employed with almost 70% working compared to about 59% of women working. Women were also more likely to have an undergraduate degree, and made up a larger proportion of the lower education group (i.e. Grade 12 or below) than men, while men were more likely to obtain certificates, diplomas and postgraduate degrees, as shown in Table 1.
The proportion of male that experience any major negative life events were reportedly different from that of female, with the exception of experiencing a natural disaster that damaged or destroyed their home. While men were more likely to be sacked, made redundant or jailed, women reported more of other negative life events. For example, the percentage of men reported being fired or made redundant was 1.5% higher compared to that of women. However, this could be because women were also more likely to report being “not in the labour force”. Among other negative life events that women were more likely to experience than men, we note that being of physical violence, death of a spouse or child, and close family member being jailed are rarer events (less than 2% of the sample) compared to having a serious injury or illness to family member or experiencing death of close relative or family member (between 10 and 20% of the sample).
3 Models and Results
3.1 Models
Our regression-based decompositions of mental health inequality use unconditional quantile regression (UQR). This is a relatively new technique developed by Firpo et al. (2009) for unconditional quantiles modelling. As shown in the non-parametric estimates of the densities for mental health scores stratified by gender in Fig. 2, an analysis of the conditional mean will mask disproportional impacts of the economic and social factors on both the absolute levels of mental health (of men and women) and its relative differences (between genders). Thus, an analysis of unconditional quantiles is useful for understanding how the relationship differs according to the location in the distribution.
The UQR was done by first transforming the outcome variable (MHI-5) using a recentered influence function (RIF) and then regressing the transformed MHI-5 against explanatory factors. The UQR allows us to evaluate the impact of changes in the distribution of various factors on quantiles of the unconditional distribution of mental health scores. UQR, therefore, looks at the entire distribution of the outcome variable, and thus is relevant for studying inequality, which is intrinsically linked to distributions rather than means (Kneib et al., 2021).
The analysis contains two parts. In the first part, we first apply the UQR method to estimate the correlates of the mental health state (MHI-5 score), for men and women separately. The regressions for men and women are:
and
where \(y_{Mit}\) and \(y_{Wit}\) are the i’s observation of mental health in year t for men and women, respectively; \(\alpha _M\) and \(\alpha _W\) are constant terms; \(\gamma _t\) is the year fixed effects; \(\textbf{x}_{Mit}\) and \(\textbf{x}_{Wit}\) are vectors of demographic, economic and life event variables for men and women i in year t; \(\varvec{\beta }_{M,\tau } \) and \(\varvec{\beta }_{W,\tau }\) are vectors of coefficients of the corresponding covariates at the \(\tau \) quantile for men and women; \(\epsilon _{Mit,\tau }\) and \(\epsilon _{Wit,\tau }\) are error terms.Footnote 5
In the second part of the paper, we use the RIF regression results to decompose the predicted outcome gap to examine how each factor contributes to the differences in mental health between men and women. Amongst various ways to perform decomposition in economics (e.g., Fortin et al., 2011), we focus on the aggregate effect of each explanatory variable. We compute the gap at the \(\tau \)th quantile following the formula:
where \({\hat{\Delta }}_{j,\tau }\) is the gap at quantile \(\tau \)th associated with variable j; \(\bar{x}_{jM}\) and \(\bar{x}_{jW}\) are the means of variable j for the men and women group; \({\hat{\beta }}_{jM, \tau }\) and \({\hat{\beta }}_{jW, \tau }\) are the estimates of variable j from regression (1) and (2) respectively. This decomposition allows us to econometrically study factors that account for the differentials in mental health scores between men and women.
3.2 Results
3.2.1 Correlates of Mental Health Inequality
We estimate our models over five main quantiles (10th, 25th, 50th, 75th and 90th) for men and women. The results are shown in Tables 2 and 3, respectively.Footnote 6 Most variables are statistically significant and have the expected signs, with the economic variables having positive association with mental health score while life event shocks have negative impacts on mental health score, and the effect magnitudes being disproportionately larger at the lower quantiles.
Economic variables like after-tax equivalised income, being employed or having a higher level of education were correlated positively with MHI-5 scores. Although the positive correlation between mental health and economics variables has been shown in the literature (see, e.g., Araya et al., 2003; Kiely et al., 2015; Ross and Mirowsky, 1995), the larger size effects at lower quantiles reflect increasing returns to scale in mental health: that is, individuals who scored lower in the MHI-5 might experience much higher returns from any improvement in other aspects of life than individuals who already were in the relatively good mental health states. Income is more strongly correlated with MHI-5 scores for men at the 10th and 25th quantiles than women, but the impact’s magnitude reduces in higher quantiles. At the 50th, 75th and 90th quantiles, increasing income appeared to benefit the mental health of women more than men. For example, a 1% increase in income would increase the average 10th quantile of MHI-5 for men and women by 0.03 and 0.02, but would increase the average 90th quantile of mental health for men and women by 0.0093 and 0.011, respectively.
Being employed predicts improvements in the mental health state for both men and women, and the impacts are amplified at lower quantiles. Interestingly, unemployment appeared to be uncorrelated with the MHI-5 score for men while it was statistically correlated with lower state of mental health in women for those in 25th and 50th quintiles (with the correlation stronger in the former). This may be due to a tendency that women were more worried about their ability to secure a job compared to their counterparts, while it has been shown that greater job insecurity is associated with reduced self-reported health (Lepinteur, 2021).
Another important observation is that higher level of education was not always associated with higher MHI-5 scores. Having a higher level of education is associated with higher scores for those at lower quantiles but with lower scores at higher quantiles. An explanation for this could be that higher education is not necessarily translated into higher paid jobs, which might partly contribute to reduced mental health. For example, in order to work in certain professional fields, higher education is required but relative pay, compared to other occupations, might not be better.
All life events had negative impacts on mental health score for both men and women, which is also consistent with existing literature (see, e.g., Brose et al., 2021; Di Giuseppe et al., 2020; Gonzalez et al., 2011; Watson and Osberg, 2017).Footnote 7 However, our full-distribution regressions showed that the impact magnitudes were always larger for the lower quantiles. Among the eight major life shocks, the top three that significantly reduced the mental health state of men in the 10th quantile include: being a victim of physical violence, being detained in jail, and experiencing the death of a spouse or child.
While it is common knowledge that women who experienced physical assaults often suffered from poor mental health, the findings highlight that being a victim of physical violence was also traumatic for men, for both physical and mental health. However, being a victim of physical violence reduced women’s mental health score more than men’s; this held true at all five quantiles across the distribution. For example, if the proportion of victims of physical violence in the population was to increase by 10 percentage points, the average 10th quantile of MHI-5 for women would drop by 5.29 points, while that of men would drop by 3.32 points.
Experiencing the death of a spouse or child and being sacked or made redundant have stronger negative consequences for the mental health of women than men, ranking as the second and the third major correlates of poor mental health in women. The negative impact of these negative events might have implications for intergenerational mobility, as mothers’ mental health is found as a channel that translates financial problems on the noncognitive outcomes of their children (Clark et al., 2020).
In summary, economic outcomes like household income or education were observed to be less important contributors to low MHI-5 score at the individual level than negative life events such as being a victim of violence, especially for those at the bottom of the MHI-5 distribution. We speculate that individuals at the lower end of the mental health distribution experience more severe consequences from adverse events, as indicated by larger coefficients, because they have fewer resources or coping mechanisms available to them. With larger effect sizes and higher prevalence of exposure to negative life events among women, this conclusion aligns with our hypothesis that negative life events are strongly correlated with worse mental health in women who already are in the low mental health score range.
3.2.2 Decomposition of Gender Mental Health Gap
We now employ the regression estimates to gain insight into the factors that contribute to the disparities in mental health between genders. Based on the RIF regression results presented in Section 3.2.1, we decompose the predicted outcome gap using Eq. (3). The results presented in Table 4 show a strong link between economic disparities and gender mental health gap, especially at the lower end of the mental health score distribution.
Among economic factors, income and labour market participation contribute to increasing the gender mental health gap. Specifically, disparity in income is sufficient to explain the aggregate gender mental health differences at the 10th and 25th quantiles. Indeed, even closing 58% of the income gap would fully close the mental health differential between men and women at the 10th quantile. Our results extend the literature on social determinants of mental health, which shows that poverty or income deprivation is negative and significantly related with mental health (Cuesta & Budría, 2015; Isaacs et al., 2018). Thus, not only low income is strongly associated with poor mental health, income differences between men and women is also the single most important predictor of the gender mental health gap for those with poor psychological wellbeing.
On the contrary, education narrows the gender mental health differences with “certificates and diploma” and “undergraduate” having the strongest impact at the low end of the mental health score distribution. As one moves toward the high end of mental health score distribution and the high end of the education system (i.e. postgraduate study), education tends to further the mental health gap between men and women. The fact that economic factors play important roles in gender mental health gap has positive implication for policy because socioeconomic variables are partially modifiable. Efforts to reduce the variation in economic inequalities may therefore plausibly feed through to close outcome gaps in health.
All the negative life events were associated with increasing gender-based mental health gap with the exception of being detained in jail. This result held across quantiles, even though their contribution to the gap decreased as one moved to higher quantiles. Among negative life events, serious injury or illness to a family member contributed most to the mental health gap between men and women. One possible explanation is that women often took a carer role after such events, regardless of whether or not the family member was their own or their spouse’s family. If the women facing such situations also carry on normal professional work and housework, then the additional caring responsibility might be perceived as an unfair division of labour, leading to lower life satisfaction and mental health (Flèche et al., 2020). Note that serious injury or illness of a family member did not have the largest absolute impact on MHI-5 scores, but physical assault experience, imprisonment and family’s death. The contribution of all these negative life events to the gender mental health gap was relatively small compared to the contribution of economic factors such as income. Although the impacts of some life shocks were extremely severe at the individual level, these types of events are infrequent for both men and women, contributing marginally to the gender-based mental health gap.
We note that apart from income, differences in the age distribution played an important role in the gender mental health gap, possibly because men and women have different paths through life and their trajectories through life are different. The contemporary literature on mental health inequality includes similar findings (e.g., Hashmi et al., 2020; Veisani and Delpisheh, 2015) and attributes this fact to the ageing or retirement effect. Although male and female health needs at older ages are different (Gómez-Costilla et al., 2021), it is hypothesised that as people get older, they become more psychologically stable, thus men’s and women’s mental health states tend to converge. The constant in Table 4 accounts for common underlying risk factors that are unrelated to other variables examined in our studies, such as biological differences, or differences in reporting or responding to mental illness. Overall, the gender mental health gap decreases as one moves from the lower quantiles to the higher quantiles of the distribution, as shown in the last row of Table 4.Footnote 8
4 Discussion and Conclusion
This paper has studied the structure of the mental health gap between men and women in Australia. Men are shown to have a highly robust advantage in MHI-5 Mental Health scores; one that is particularly large in the left tail of the health-outcome distribution. We considered two potential sources of this disparity—(1) the persistent economic disadvantage experienced by women in terms of income, and (2) the differences that men and women have in terms of their life experiences.
Using regression-based decompositions based upon the Recentered Influence Function, we showed that income is a highly significant determinant of mental health for individuals in the lower quantiles of the unconditional MHI-5 distribution. This feature, combined with lower mean incomes for women and higher rates of poverty and disadvantage, suggests that the over-representation of women amongst individuals with very poor mental health is strongly linked with economic disparities. Although regression models such as these may be influenced by reverse causal effects or omitted variable bias, our results are robust, consistent with expectations, and line up with existing findings in related literature. Policies that compress the income distribution and mitigate poverty are therefore likely to narrow the gender gap in individuals with very poor mental health. Other socioeconomic variables such as education have relatively small effect sizes, and in some instances generate female advantages in psychological health.
We also considered the possibility that social experiences (captured with life event variables) may contribute to this outcome gap. Men and women on average lead different types of lives, and care different amounts about relationships, risk, caring, family, and many other such factors. Since these variables are also likely to be important determinants of mental wellbeing, they offer an alternative to the economic explanation for the mental health gaps. Our models show that factors like divorce, job loss, incarceration, experiencing violence, and the death of friends or family members are indeed highly influential over individuals’ mental states. However, these social factors are relatively rare and do not differ substantially between men and women, and are therefore not a meaningful source of gender disparity. Policies that offer social support for individuals suffering from adverse life events are likely to reduce health inequalities, as these variables have unusually large effect sizes for individuals with already poor mental health. However, they will not meaningfully lower gender gaps.
Data Availability
The unit record data from the HILDA Survey were obtained from the Australian Data Archive, which is hosted by The Australian National University. The HILDA Survey was initiated and is funded by the Australian Government Department of Social Services (DSS) and is managed by the Melbourne Institute of Applied Economic and Social Research (Melbourne Institute). The findings and views based on the data, however, are those of the author and should not be attributed to the Australian Government, DSS, the Melbourne Institute, the Australian Data Archive or The Australian National University and none of those entities bear any responsibility for the analysis or interpretation of the unit record data from the HILDA Survey provided by the author.
Notes
All monetary values used in this study are adjusted for inflation. We calculate the Consumer Price Index (CPI) for each state each year as the average of four quarters—all commodity groups, following the data from the Australian Bureau of Statistics with index reference period: 2011–12 = 100.0.
We present results using individual income as a robustness check in Appendix C.
Some studies show that women report being happier than men and have higher average “life-satisfaction” scores on average (Graham and Chattopadhyay, 2013; Joshanloo and Jovanović 2020). However, it could be because women have different reference points when answering the same life satisfaction question (Montgomery, 2016) or men less likely to report their problems for fear of stigma or to do with dominant notions of masculinity (Affleck et al., 2018). Stevenson and Wolfers (2009) found that women experienced an absolute and relative decline in happiness across multiple datasets spanning a number of Western industrialised countries.
Although HILDA collects panel data, we do not use standard panel data techniques like random effects or fixed effects because we are interested in inequality; using fixed effects will wipe out the dispersion that we care about, and there is no random effects version of our approach. Instead, we run the pooled model with year fixed-effects. The estimates for selected years are presented in Appendixes D and E.
We acknowledge that it is important to account for past mental health conditions because there is likely correlation between \(\epsilon _{it}\) and \(\epsilon _{i, t-1}\) that is not necessarily controlled for in the model (i.e., an individual responses can be similar over the years). However, we do not include a lag dependent variable, because if we did, what explains inequality in \(y_t\) will be in \(y_{t-1}\), and what explains inequality in \(y_{t-1}\) will be in \(y_{t-2}\). This recursion will not help us to get to the root source of inequality and create endogeneity issue in short panel. We are unaware of any dynamic technique for Quantile Regression. As a result, instead of accounting for the correlations as coefficients in the model, we resolve this issue using clustered robust standard error at the individual level.
The full results are provided in Appendix B.
Hashmi et al. (2020) did not study the mental health of men and women separately, but they found that exposure to negative life events was most harmful for the mental health of people in the most disadvantaged socioeconomic groups.
We expand our analysis by examining the impact of gender on outcomes and introducing further metrics to assess inequality, such as the interquantile share ratio, the Gini coefficient, and the log variance. The findings derived from these expanded analyses corroborate the conclusions reached in the main text, as detailed in Appendix F.
References
Affleck, W., Carmichael, V., & Whitley, R. (2018). Men’s mental health: Social determinants and implications for services. The Canadian Journal of Psychiatry, 63(9), 581–589.
Araya, R., Lewis, G., Rojas, G., & Fritsch, R. (2003). Education and income: Which is more important for mental health? Journal of Epidemiology & Community Health, 57(7), 501–505.
Australian Bureau of Statistics. (2021). First insights from the national study of mental health and wellbeing, 2020–21. https://www.abs.gov.au/articles/first-insights-national-study-mental-health-and-wellbeing-2020-21
Autor, D., Figlio, D., Karbownik, K., Roth, J., & Wasserman, M. (2019). Family disadvantage and the gender gap in behavioral and educational outcomes. American Economic Journal: Applied Economics, 11(3), 338–381.
Beauchamp, A., Backholer, K., Magliano, D., & Peeters, A. (2014). The effect of obesity prevention interventions according to socioeconomic position: A systematic review. Obesity Reviews, 15(7), 541–554.
Bem, S. L. (1981). Gender schema theory: A cognitive account of sex typing. Psychological review, 88(4), 354.
Berry, H. L., & Welsh, J. A. (2010). Social capital and health in Australia: An overview from the household, income and labour dynamics in Australia survey. Social Science & Medicine, 70(4), 588–596.
Bowlby, J. (1969). Attachment and loss (79th ed.). Random House.
Brazier, J. E., Harper, R., Jones, N., O’cathain, A., Thomas, K., Usherwood, T., & Westlake, L. (1992). Validating the SF-36 health survey questionnaire: New outcome measure for primary care. British Medical Journal, 305(6846), 160–164.
Brose, A., Blanke, E. S., Schmiedek, F., Kramer, A. C., Schmidt, A., & Neubauer, A. B. (2021). Change in mental health symptoms during the covid-19 pandemic: The role of appraisals and daily life experiences. Journal of Personality, 89(3), 468–482.
Buhmann, B., Rainwater, L., Schmaus, G., & Smeeding, T. M. (1988). Equivalence scales, well-being, inequality, and poverty: Sensitivity estimates across ten countries using the luxembourg income study (lis) database. Review of Income and Wealth, 34(2), 115–142.
Butterworth, P., & Crosier, T. (2004). The validity of the SF-36 in an Australian national household survey: Demonstrating the applicability of the household income and labour dynamics in Australia (HILDA) survey to examination of health inequalities. BMC Public Health, 4(1), 1–11.
Caroli, E., & Weber-Baghdiguian, L. (2016). Self-reported health and gender: The role of social norms. Social Science & Medicine, 153, 220–229.
Chopra, P. (2009). Mental health and the workplace: Issues for developing countries. International Journal of Mental Health Systems, 3(1), 1–9.
Christensen, T. N., Wallstrøm, I. G., Bojesen, A. B., Nordentoft, M., & Eplov, L. F. (2021). Predictors of work and education among people with severe mental illness who participated in the danish individual placement and support study: Findings from a randomized clinical trial. Social Psychiatry and Psychiatric Epidemiology, 56(9), 1669–1677.
Churchill, S. A., Munyanyi, M. E., Prakash, K., & Smyth, R. (2020). Locus of control and the gender gap in mental health. Journal of Economic Behavior & Organization, 178, 740–758.
Clark, A. E., & D’Ambrosio, C. (2015). Attitudes to income inequality. In Handbook of Income Distribution (vol. 2, pp. 1147–1208). Elsevier.
Clark, A. E., D’Ambrosio, C., & Barazzetta, M. (2020). Childhood circumstances and young adulthood outcomes: The role of mothers’ financial problems. Health Economics, 30(2), 342–357.
Clark, A. E., D’Ambrosio, C., & Zhu, R. (2021). Living in the shadow of the past: Financial profiles and well-being. The Scandinavian Journal of Economics, 123(3), 910–939.
Clark, A. E., Frijters, P., & Shields, M. A. (2008). Relative income, happiness, and utility: An explanation for the easterlin paradox and other puzzles. Journal of Economic Literature, 46(1), 95–144.
Cohen, S., & Wills, T. A. (1985). Stress, social support, and the buffering hypothesis. Psychological Bulletin, 98(2), 310.
Cornaglia, F., Crivellaro, E., & McNally, S. (2015). Mental health and education decisions. Labour Economics, 33, 1–12.
Cuesta, M. B., & Budría, S. (2015). Income deprivation and mental well-being: The role of non-cognitive skills. Economics & Human Biology, 17, 16–28.
Di Giuseppe, G., Thacker, N., Schechter, T., & Pole, J. D. (2020). Anxiety, depression, and mental health-related quality of life in survivors of pediatric allogeneic hematopoietic stem cell transplantation: A systematic review. Bone Marrow Transplantation, 55(7), 1240–1254.
Firpo, S., Fortin, N. M., & Lemieux, T. (2009). Unconditional quantile regressions. Econometrica, 77(3), 953–973.
Flèche, S., Lepinteur, A., & Powdthavee, N. (2020). Gender norms, fairness and relative working hours within households. Labour Economics, 65, 101866.
Fortin, N., Lemieux, T., & Firpo, S. (2011). Decomposition methods in economics. In Handbook of Labor Economics (vol. 4, pp. 1–102). Elsevier
Gili, M., Castellví, P., Vives, M., de la Torre-Luque, A., Almenara, J., Blasco, M. J., Cebrià, A. I., Gabilondo, A., Pérez-Ara, M. A., Miranda-Mendizabal, A., et al. (2019). Mental disorders as risk factors for suicidal behavior in young people: A meta-analysis and systematic review of longitudinal studies. Journal of Affective Disorders, 245, 152–162.
Gómez-Costilla, P., García-Prieto, C., & Somarriba-Arechavala, N. (2021). Aging and gender health gap: A multilevel analysis for 17 European countries. Social Indicators Research, 160, 1–19.
Gonzalez, J. S., Fisher, L., & Polonsky, W. H. (2011). Depression in diabetes: Have we been missing something important? Diabetes Care, 34(1), 236–239.
Graham, C., & Chattopadhyay, S. (2013). Gender and well-being around the world. International Journal of Happiness and Development, 1(2), 212–232.
Grossman, M. (2017). Determinants of health: An economic perspective. Columbia University Press.
Hashmi, R., Alam, K., & Gow, J. (2020). Socioeconomic inequalities in mental health in Australia: Explaining life shock exposure. Health Policy, 124(1), 97–105.
Hochschild, A. R. (2018). The time bind: When work becomes home and home becomes work. In Social stratification (pp. 803–807). Routledge.
Hoertel, N., Franco, S., Wall, M. M., Oquendo, M., Kerridge, B., Limosin, F., & Blanco, C. (2015). Mental disorders and risk of suicide attempt: A national prospective study. Molecular Psychiatry, 20(6), 718–726.
Hoeymans, N., Garssen, A. A., Westert, G. P., & Verhaak, P. F. (2004). Measuring mental health of the Dutch population: A comparison of the GHQ-12 and the MHI-5. Health and Quality of Life Outcomes (p. 6).
Huguet, N., Kaplan, M. S., & Feeny, D. (2008). Socioeconomic status and health-related quality of life among elderly people: Results from the joint Canada/United States survey of health. Social Science & Medicine, 66(4), 803–810.
Isaacs, A. N., Enticott, J., Meadows, G., & Inder, B. (2018). Lower income levels in Australia are strongly associated with elevated psychological distress: Implications for healthcare and other policy areas. Frontiers in Psychiatry, 9, 536.
Jenkinson, C., Wright, L., & Coulter, A. (1994). Criterion validity and reliability of the SF-36 in a population sample. Quality of Life Research, 3(1), 7–12.
Joshanloo, M., & Jovanović, V. (2020). The relationship between gender and life satisfaction: Analysis across demographic groups and global regions. Archives of Women’s Mental Health, 23(3), 331–338.
Kawachi, I., & Kennedy, B. P. (1999). Income inequality and health: pathways and mechanisms. Health Services Research, 34(1 Pt 2), 215–227. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1088996/.
Kiely, K. M., Leach, L. S., Olesen, S. C., & Butterworth, P. (2015). How financial hardship is associated with the onset of mental health problems over time. Social Psychiatry and Psychiatric Epidemiology, 50(6), 909–918.
Kim, S., & Koh, K. (2021). The effects of income on health: Evidence from lottery wins in Singapore. Journal of Health Economics, 76, 102414.
Kneib, T., Silbersdorff, A., & Säfken, B. (2021). Rage against the mean—a review of distributional regression approaches. Econometrics and Statistics.
Kulhánová, I., Hoffmann, R., Judge, K., Looman, C. W. N., Eikemo, T. A., Bopp, M., Deboosere, P., Leinsalu, M., Martikainen, P., Rychtaříková, J., Wojtyniak, B., Menvielle, G., & Mackenbach, J. P. (2014). Assessing the potential impact of increased participation in higher education on mortality: Evidence from 21 European populations. Social Science & Medicine, 117, 142–149.
Lepinteur, A. (2021). The asymmetric experience of gains and losses in job security on health. Health Economics, 30(9), 2217–2229.
Li, J., & Powdthavee, N. (2015). Does more education lead to better health habits? Evidence from the school reforms in Australia. Social Science & Medicine, 127, 83–91.
Lorant, V., Deliège, D., Eaton, W., Robert, A., Philippot, P., & Ansseau, M. (2003). Socioeconomic inequalities in depression: A meta-analysis. American Journal of Epidemiology, 157(2), 98–112.
Lu, C., Frank, R. G., Liu, Y., Shen, J., et al. (2009). The impact of mental health on labour market outcomes in China. Journal of Mental Health Policy and Economics, 12(3), 157.
Marchand, A., Bilodeau, J., Demers, A., Beauregard, N., Durand, P., & Haines, V. Y., III. (2016). Gendered depression: Vulnerability or exposure to work and family stressors? Social science & medicine, 166, 160–168.
Montgomery, M. (2016). Are women really happier than men around the world? https://blogs.worldbank.org/impactevaluations/are-women-really-happier-men-around-world-guest-post-mallory-montgomery
Osmani, S., & Sen, A. (2003). The hidden penalties of gender inequality: Fetal origins of ill-health. Economics & Human Biology, 1(1), 105–121.
Rojas-Garcia, A., Ruiz-Perez, I., Rodriguez-Barranco, M., Bradley, D. C. G., Pastor-Moreno, G., & Ricci-Cabello, I. (2015). Healthcare interventions for depression in low socioeconomic status populations: A systematic review and meta-analysis. Clinical Psychology Review, 38, 65–78.
Rosenfield, S., Vertefuille, J., & McAlpine, D. D. (2000). Gender stratification and mental health: An exploration of dimensions of the self. Social Psychology Quarterly, 63, 208–223.
Ross, C. E., & Mirowsky, J. (1995). Does employment affect health? Journal of Health and Social Behavior, 36, 230–243.
Roy, J., & Schurer, S. (2013). Getting stuck in the blues: Persistence of mental health problems in Australia. Health Economics, 22(9), 1139–1157.
Rumpf, H.-J., Meyer, C., Hapke, U., & John, U. (2001). Screening for mental health: Validity of the MHI-5 using DSM-IV Axis I psychiatric disorders as gold standard. Psychiatry Research, 105(3), 243–253.
Stevenson, B., & Wolfers, J. (2009). The paradox of declining female happiness. American Economic Journal: Economic Policy, 1(2), 190–225.
Summerfield, M., Bevitt, A., Fok, Y. K., Hahn, M., La, N., Macalalad, N., O’Shea, M., Watson, N., Wilkins, R., & Wooden, M. (2020). HILDA User Manual Release 20.
Suter, L. E., & Miller, H. P. (1973). Income differences between men and career women. American Journal of Sociology, 78(4), 962–974.
Thorsen, S. V., Rugulies, R., Hjarsbech, P. U., & Bjorner, J. B. (2013). The predictive value of mental health for long-term sickness absence: The major depression inventory (MDI) and the mental health inventory (MHI-5) compared. BMC Medical Research Methodology, 13(1), 115.
Veisani, Y., & Delpisheh, A. (2015). Decomposing of socioeconomic inequality in mental health: A cross-sectional study into female-headed households. Journal of Research in Health Sciences, 15(4), 218–222.
Ware, J. E., Kosinski, M., & Keller, S. D. (1994). SF-36 Physical and Mental Health Summary Scales: A User’s Manual.
Watson, B., & Osberg, L. (2017). Healing and/or breaking? The mental health implications of repeated economic insecurity. Social Science & Medicine, 188, 119–127.
Watson, N., & Wooden, M. (2021). The household, income and labour dynamics in Australia (HILDA) survey. Jahrbücher für Nationalökonomie und Statistik, 241(1), 131–141.
Wu, Q., Chen, Y., Zhou, Y., Huang, Y., Liu, R., et al. (2023). Reliability, validity, and sensitivity of short-form 36 health survey (sf-36) in patients with sick sinus syndrome. Medicine, 102(24), e33979.
Zhou, Y., Lu, W., Liu, C., & Gan, H. (2023). The gender gap in financial distress. Applied Economics, 66, 1–16.
Zimmerman, F. J., & Katon, W. (2005). Socioeconomic status, depression disparities, and financial strain: What lies behind the income-depression relationship? Health Economics, 14(12), 1197–1215.
Acknowledgements
We would like to thank Prasada Rao, Son Nghiem, Trong Anh Trinh, Tracy Comans, Tim Ludlow, Jason Pole, Aude Bernard and two anonymous referees for their thoughtful comments. All errors remaining are our own.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no Conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
A Results Using Multiple Imputation
B Full RIF Regression Results
C Results Using Individual Income
D Results Using Wave 9
E Results Using Wave 20
F Treatment Effects of Gender
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nguyen, T.T., Nguyen, K.H. & Rohde, N. Economic Disparities, Life Events, and the Gender Mental Health Gap. Soc Indic Res 174, 1053–1100 (2024). https://doi.org/10.1007/s11205-024-03424-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11205-024-03424-6