Abstract
Purpose
Preference-based measures can provide measurements of health-related quality of life and be utilized for cost-effectiveness analyses of interventions in individuals with chronic obstructive pulmonary disease (COPD). The purpose of this study is to evaluate whether generic preference-based measures are reliable, valid, and responsive in COPD.
Methods
A systematic review was performed using the Consensus-based Standards for the selection of health Measurement Instruments (COSMIN) guidelines. Three databases were searched: MEDLINE, EMBASE, and CINAHL. Studies were included if the sample represented individuals with COPD and the aim was to evaluate one or more psychometric properties or the interpretability of generic preference-based measures.
Results
Six hundred and sixty-seven abstracts were screened, 65 full-text articles were reviewed and 24 articles met the inclusion criteria. Measures which emerged from the search were the EQ-5D, the SF-6D, the Quality of Well-being scale, the 15D, and the Health Utilities Index 3. Evidence for the test–retest reliability of these measures was limited. Construct validity of the measures was well supported with correlations with generic health profiles being 0.37–0.68, and correlations with COPD-specific health profiles being 0.53–0.75. Evidence for known-groups validity of these measures was poor and data on responsiveness were mixed.
Conclusion
Generic preference-based measures’ sensitivity to change and ability to discriminate between different disease severities in COPD was poorly supported. Future research may consider examining the development of COPD-specific preference-based measures that may allow for a more accurate detection of change and discrimination among disease severities to facilitate cost-effectiveness evaluations.

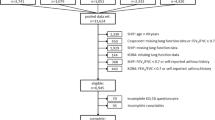
Adapted from the PRISMA statement [54]. COPD chronic obstructive pulmonary disease, GPBM Generic preference-based measure, N/A not applicable
Similar content being viewed by others
Data availability
The data that support the findings of this study are available in the supplementary material of this article.
Abbreviations
- AUC:
-
Area under the curve
- COPD:
-
Chronic obstructive pulmonary disease
- COSMIN:
-
Consensus-based standards for the selection of health measurement instruments
- ES:
-
Effect size
- FEV1 :
-
Forced expiratory volume in one second
- GPBM:
-
Generic preference-based measure
- GRADE:
-
Grading of recommendations assessment, development, and evaluation
- HUI2 & HUI3:
-
Health utilities index mark 2 & 3
- HRQoL:
-
Health-related quality of life
- MID:
-
Minimal important difference
- QWB:
-
Quality of well-being
- SRM:
-
Standardized response mean
References
Global strategy for prevention, diagnosis and management of COPD. (2019).
Miravitlles, M., & Ribera, A. (2017). Understanding the impact of symptoms on the burden of COPD. Respiratory Research, 18(1), 67. https://doi.org/10.1186/s12931-017-0548-3.
Perng, D. W., Tao, C. W., Su, K. C., Tsai, C. C., Liu, L. Y., & Lee, Y. C. (2009). Anti-inflammatory effects of salmeterol/fluticasone, tiotropium/fluticasone or tiotropium in COPD. European Respiratory Journal. https://doi.org/10.1183/0903193600115308.
Boueri, F. M. V., Bucher-Bartelson, B. L., Glenn, K. A., & Make, B. J. M. (2001). Quality of life measured with a generic instrument (Short Form-36) improves following pulmonary rehabilitation in patients with COPD. Chest. https://doi.org/10.1378/chest.119.1.77.
Neumann, P. J., Goldie, S. J., & Weinstein, M. C. (2000). Preference-based measures in economic evaluation in health care. Annual Review of Public Health. https://doi.org/10.1146/annurev.publhealth.21.1.587.
Brazier, J., Ara, R., Rowen, D., & Chevrou-Severac, H. (2017). A review of generic preference-based measures for use in cost-effectiveness models. PharmacoEconomics. https://doi.org/10.1007/s40273-017-0545-x.
Whitehead, S. J., & Ali, S. (2010). Health outcomes in economic evaluation: The QALY and utilities. British Medical Bulletin. https://doi.org/10.1093/bmb/ldq033.
Gutacker, N., Bojke, C., Daidone, S., Devlin, N., & Street, A. (2013). Hospital variation in patient-reported outcomes at the level of EQ-5D dimensions: Evidence from England. Medical Decision Making. https://doi.org/10.1177/0272989X13482523.
Zhou, Z., Fang, Y., Zhou, Z., Li, D., Wang, D., Li, Y., et al. (2017). Assessing income-related health inequality and horizontal inequity in China. Social Indicators Research. https://doi.org/10.1007/s11205-015-1221-1.
Bolarinwa, O. (2015). Principles and methods of validity and reliability testing of questionnaires used in social and health science researches. Nigerian Postgraduate Medical Journal. https://doi.org/10.4103/1117-1936.173959.
De Vet, H. C. W., Terwee, C. B., Mokkink, L. B., & Knol, D. L. (2011). Measurement in medicine: A practical guide. Cambridge: Cambridge University Press.
Terwee, C. B., Jansma, E. P., Riphagen, I. I., & De Vet, H. C. W. (2009). Development of a methodological PubMed search filter for finding studies on measurement properties of measurement instruments. Quality of Life Research. https://doi.org/10.1007/s11136-009-9528-5.
Vilagut, G. (2014). Test-retest reliability BT. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research (pp. 6622–6625). Netherlands Dordrecht: Springer.
Mokkink, L. B., Terwee, C. B., Patrick, D. L., Alonso, J., Stratford, P. W., Knol, D. L., et al. (2010). The COSMIN study reached international consensus on taxonomy, terminology, and definitions of measurement properties for health-related patient-reported outcomes. Journal of Clinical Epidemiology. https://doi.org/10.1016/j.jclinepi.2010.02.006.
Chin, C.-L., & Yao, G. (2014). Convergent validity BT. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research (pp. 1275–1276). Netherlands Dordrecht: Springer.
Davidson, M. (2014). Known-groups validity BT. In A. C. Michalos (Ed.), Encyclopedia of quality of life and well-being research (pp. 3481–3482). Netherlands Dordrecht: Springer.
Mokkink, L. B., de Vet, H. C. W., Prinsen, C. A. C., Patrick, D. L., Alonso, J., Bouter, L. M., et al. (2018). COSMIN risk of bias checklist for systematic reviews of patient-reported outcome measures. Quality of Life Research. https://doi.org/10.1007/s11136-017-1765-4.
Mokkink, L. B., Prinsen, C. A. C., Patrick, D. L., Alonso, J., Bouter, L. M., De Vet, H. C. W., & Terwee, C. B. (2018). COSMIN methodology for systematic reviews of Patient—Reported Outcome Measures ( PROMs ). User Manual, (February), 1–78.
Cohen, J. (1988). Statistical power analysis for the behavioural science (2nd ed.). Hillsdale, NJ: Lawrence Erlbaum Associates.
Deeks, J. J. (2011). Chapter 9: Analysing data and undertaking meta-analyses. Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011).
Schünemann, H., Brożek, J., Guyatt, G., & Oxman, A. (2013). GRADE handbook for grading quality of evidence and strength of recommendations. The GRADE Working Group.
Thuppal, S., Markwell, S., Crabtree, T., & Hazelrigg, S. (2019). Comparison between the EQ-5D-3L and the SF-6D quality of life (QOL) questionnaires in patients with chronic obstructive pulmonary disease (COPD) undergoing lung volume reduction surgery (LVRS). Quality of Life Research, 28(7), 1885–1892. https://doi.org/10.1007/s11136-019-02123-x.
Nolan, C. M., Longworth, L., Lord, J., Canavan, J. L., Jones, S. E., Kon, S. S. C., et al. (2016). The EQ-5D-5L health status questionnaire in COPD: Validity, responsiveness and minimum important difference. Thorax, 71(6), 493–500. https://doi.org/10.1136/thoraxjnl-2015-207782.
Wacker, M. E., Jörres, R. A., Karch, A., Wilke, S., Heinrich, J., Karrasch, S., et al. (2016). Assessing health-related quality of life in COPD: Comparing generic and disease-specific instruments with focus on comorbidities. BMC Pulmonary Medicine, 16(1), 1–11. https://doi.org/10.1186/s12890-016-0238-9.
Chen, J., Wong, C. K., McGhee, S. M., Pang, P. K., & Yu, W. C. (2014). A comparison between the EQ-5D and the SF-6D in patients with chronic obstructive pulmonary disease (COPD). PLoS ONE. https://doi.org/10.1371/journal.pone.0112389.
Ferreira, L. N., Ferreira, P. L., & Pereira, L. N. (2014). Comparing the performance of the SF-6D and the EQ-5D in different patient groups. Acta Médica Portuguesa, 27(2), 236.
Kim, S. H., Oh, Y. M., & Jo, M. W. (2014). Health-related quality of life in chronic obstructive pulmonary disease patients in Korea. Health and Quality of Life Outcomes, 12(1), 1–7. https://doi.org/10.1186/1477-7525-12-57.
Lin, F. J., Pickard, A. S., Krishnan, J. A., Joo, M. J., Au, D. H., & Carson, S. S. (2014). Measuring health-related quality of life in chronic obstructive pulmonary disease: Properties of the EQ-5D-5L and PROMIS-43 short form. BMC Medical Research Methodology, 14, 78. https://doi.org/10.1186/1471-2288-14-78.
Manca, S., Rodriguez, E., Huerta, A., Torres, M., Lazaro, L., Curi, S., et al. (2014). Usefulness of the CAT, LCOPD, EQ-5D and COPDSS scales in understanding the impact of lung disease in patients with Alpha-1 antitrypsin deficiency. COPD Journal of Chronic Obstructive Pulmonary Disease, 11(5), 480–488. https://doi.org/10.3109/15412555.2014.898030.
Peters, M., Crocker, H., Dummett, S., Jenkinson, C., Doll, H., & Fitzpatrick, R. (2014). Change in health status in long-term conditions over a one year period: A cohort survey using patient-reported outcome measures. Health and Quality of Life Outcomes, 12(1), 1–10.
Goossens, L. M. A., Nivens, M. C., Sachs, P., Monz, B. U., & Rutten-Van Mölken, M. P. M. H. (2011). Is the EQ-5D responsive to recovery from a moderate COPD exacerbation? Respiratory Medicine, 105(8), 1195–1202. https://doi.org/10.1016/j.rmed.2011.02.018.
Pickard, A. S., Yang, Y., & Lee, T. A. (2011). Comparison of health-related quality of life measures in chronic obstructive pulmonary disease. Health and Quality of Life Outcomes. https://doi.org/10.1186/1477-7525-9-26.
Menn, P., Weber, N., & Holle, R. (2010). Health-related quality of life in patients with severe COPD hospitalized for exacerbations—comparing EQ-5D, SF-12 and SGRQ. Health and Quality of Life Outcomes, 8, 1–9. https://doi.org/10.1186/1477-7525-8-39.
Polley, L., Yaman, N., Heaney, L., Cardwell, C., Murtagh, E., Ramsey, J., et al. (2008). Impact of cough across different chronic respiratory diseases: Comparison of two cough-specific health-related quality of life questionnaires. Chest, 134(2), 295–302. https://doi.org/10.1378/chest.07-0141.
Ringbaek, T., Brøndum, E., Martinez, G., & Lange, P. (2008). EuroQoL in assessment of the effect of pulmonary rehabilitation COPD patients. Respiratory Medicine, 102(11), 1563–1567. https://doi.org/10.1016/j.rmed.2008.06.016.
Rutten-Van Mölken, M. P. M. H., Oostenbrink, J. B., Tashkin, D. P., Burkhart, D., & Monz, B. U. (2006). Does quality of life of COPD patients as measured by the generic EuroQol five-dimension questionnaire differentiate between COPD severity stages? Chest, 130(4), 1117–1128. https://doi.org/10.1378/chest.130.4.1117.
Stavem, K. (1999). Reliability, validity and responsiveness of two multiattribute utility measures in patients with chronic obstructive pulmonary disease. Quality of Life Research, 8(1–2), 45–54. https://doi.org/10.1023/A:1026475531996.
Harper, R., Brazier, J. E., Waterhouse, J. C., Walters, S. J., Jones, N. M. B., & Howard, P. (1997). Comparison of outcome measures for patients with chronic obstructive pulmonary disease (COPD) in an outpatient setting. Thorax, 52(10), 879–887. https://doi.org/10.1136/thx.52.10.879.
Walters, S. J., & Brazier, J. E. (2003). What is the relationship between the minimally important difference and health state utility values? The case of the SF-6D. Health and Quality of Life Outcomes, 1(4), 1–8.
Kaplan, R. M. (2005). The minimally clinically important difference in generic utility-based measures. COPD Journal of Chronic Obstructive Pulmonary Disease, 2(1), 91–97. https://doi.org/10.1081/COPD-200052090.
Anderson, J. P., Kaplan, R. M., Berry, C. C., Bush, J. W., & Rumbaut, R. G. (1989). Interday reliability of function assessment for a health status measure: The quality of well-being scale. Medical Care, 27(11), 1076–1084.
Kaplan, R. M., Atkins, C. J., & Timms, R. (1984). Validity of a quality of well-being scale as an outcome measure in chronic obstructive pulmonary disease. Journal of Chronic Diseases, 37(2), 85–95.
Koskela, J., Kupiainen, H., Kilpeläinen, M., Lindqvist, A., Sintonen, H., Pitkäniemi, J., et al. (2014). Longitudinal HRQoL shows divergent trends and identifies constant decliners in asthma and COPD. Respiratory Medicine, 108(3), 463–471. https://doi.org/10.1016/j.rmed.2013.12.001.
Mazur, W., Kupiainen, H., Pitkäniemi, J., Kilpeläinen, M., Sintonen, H., & Lindqvist, A. (2011). Comparison between the disease-specific airways questionnaire 20 and the generic 15D instruments in COPD. Health and Quality of Life Outcomes, 9, 4. https://doi.org/10.1186/1477-7525-9-4.
Puhan, M. A., Guyatt, G. H., Goldstein, R., Mador, J., McKim, D., Stahl, E., et al. (2007). Relative responsiveness of the chronic respiratory questionnaire, St. Georges respiratory questionnaire and four other health-related quality of life instruments for patients with chronic lung disease. Respiratory Medicine, 101(2), 308–316. https://doi.org/10.1016/j.rmed.2006.04.023.
Brazier, J., Ratcliffe, J., Salomon, J. A., & Tsuchiya, A. (2007). Measuring and valuing health benefits for economic evaluation. Oxford: OUP.
Chauvin, A., Rupley, L., Meyers, K., Johnson, K., & Eason, J. (2008). Outcomes in cardiopulmonary physical therapy: Chronic respiratory disease questionnaire (CRQ). Cardiopulmonary Physical Therapy Journal, 19(2), 61–67.
Petrillo, J., Van Nooten, F., Jones, P., & Rutten-Van Mölken, M. (2011). Utility estimation in chronic obstructive pulmonary disease: A preference for change? PharmacoEconomics. https://doi.org/10.2165/11589280-000000000-00000.
Simon Pickard, A., Wilke, C., Jung, E., Patel, S., Stavem, K., & Lee, T. A. (2008). Use of a preference-based measure of health (EQ-5D) in COPD and asthma. Respiratory Medicine. https://doi.org/10.1016/j.rmed.2007.11.016.
Finch, A. P., Brazier, J. E., & Mukuria, C. (2018). What is the evidence for the performance of generic preference-based measures? A systematic overview of reviews. European Journal of Health Economics. https://doi.org/10.1007/s10198-017-0902-x.
Qian, X., Tan, R. L. Y., Chuang, L. H., & Luo, N. (2020). Measurement properties of commonly used generic preference-based measures in East and South-East Asia: A systematic review. PharmacoEconomics. https://doi.org/10.1007/s40273-019-00854-w.
Fayers, P. M., Hays, R., & Hays, R. D. (2005). Assessing quality of life in clinical trials: Methods and practice. Oxford: Oxford University Press.
Brazier, J. E., Rowen, D., Mavranezouli, I., Tsuchiya, A., Young, T., Yang, Y., et al. (2012). Developing and testing methods for deriving preference based measures of health from condition-specific measures (and other patient-based measures of outcome). Health Technology Assessment. https://doi.org/10.3310/hta16320.
Moher, D., Liberati, A., Tetzlaff, J., Altman, D. G., Altman, D., Antes, G., et al. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Medicine. https://doi.org/10.1371/journal.pmed.1000097.
Acknowledgements
All authors (AM, MKB, JW, NP, AK) contributed to the study’s conception and/or design. Screening of articles and quality assessments were performed by AM and NP. The first draft of the manuscript was written by AM. Preliminary edits were made by AK and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript, and AM is the guarantor of the paper.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mehdipour, A., Beauchamp, M.K., Wald, J. et al. Measurement properties of preference-based measures for economic evaluation in COPD: a systematic review. Qual Life Res 29, 2875–2885 (2020). https://doi.org/10.1007/s11136-020-02569-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-020-02569-4