Abstract
Purpose
Women with early-stage cervical cancer may experience changes in their quality of life (QoL) due to treatment or to the effects of the cancer. In this study, we examined differences in QoL by treatment modality between women who underwent surgery only and those treated with concurrent chemoradiation (CCRT).
Methods
The sample of 290 women had been diagnosed with stage I–II cervical cancer. Data were collected on these women’s demographic and disease characteristics, general QoL, and cancer-specific QoL using an author-designed demographic-disease survey, the European Organization for Research and Treatment of Cancer QoL questionnaire, and the Taiwanese-version Cervical Cancer Module 24 questionnaire, respectively. Data were analyzed by descriptive statistics and analysis of covariance.
Results
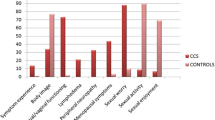
Women with cervical cancer who underwent surgery only had significantly worse constipation and body image than those treated with CCRT. Women who underwent CCRT had worse physical and role functioning than those who underwent surgery only. Women who had CCRT also reported worse symptoms, such as fatigue, appetite loss, diarrhea, financial difficulties, sexual enjoyment, and sexual/vaginal functioning, than those who had only surgery.
Conclusions
Our results add knowledge about QoL in women with early-stage cervical cancer who receive different treatment modalities. When suggesting treatment modalities for women with cervical cancer, health professionals should also consider changes in women’s QoL after cancer treatment. To improve women’s QoL after treatment, professionals should also offer timely and individualized interventions based on women’s cervical cancer treatment.
Similar content being viewed by others
References
Ministry of Health and Welfare, Executive Yuan, Taiwan. (2016). 2015 statistics of causes of death. http://www.mohw.gov.tw/en/Ministry/Statistic_P.aspx?f_list_no=474&fod_list_no=6242&doc_no=56508. Accessed 02 December 2016.
Health Promotion Administration, Ministry of Health and Welfare, Taiwan. (2016a). Cancer registry annual report, 2013. http://www.hpa.gov.tw/Bhpnet/Web/Stat/StatisticsShow.aspx?No=201604210001. Accessed 02 December 2016.
Health Promotion Administration, Ministry of Health and Welfare, Taiwan. (2016b). The age-standardized death rates of cervical cancer per 100,000 population, 1979–2014. https://cris.hpa.gov.tw/pagepub/Home.aspx?itemNo=cr.q.10. Accessed 02 December 2016.
Health Promotion Administration, Ministry of Health and Welfare, Taiwan. (2016c). The relative survival rates of cervical cancer, 1987–2013. https://cris.hpa.gov.tw/pagepub/Home.aspx?itemNo=cr.a.10. Accessed 04 December 2016.
Katanyoo, K., Sanguanrungsirikul, S., & Manusirivithaya, S. (2012). Comparison of treatment outcomes between squamous cell carcinoma and adenocarcinoma in locally advanced cervical cancer. Gynecologic Oncology, 125, 292–296.
Undurraga, M., Loubeyre, P., Dubuisson, J.-B., Schneider, D., & Petignat, P. (2010). Early-stage cervical cancer: Is surgery better than radiotherapy? Expert Review of Anticancer Therapy, 10(3), 451–460.
Chen, R. J., Lin, Y. H., Chen, C. A., Huang, S. C., Chow, S. N., & Hsieh, C. Y. (1999). Influence of histologic type and age on survival rates for invasive cervical carcinoma in Taiwan. Gynecological Oncology, 73, 184–190.
Lee, J.-Y., Youm, J., Kim, J.-W., Kim, K., Kim, H.-J., Cho, J.-Y., et al. (2016). An alternative triage strategy based on preoperative MRI for avoiding trimodality therapy in stage IB cervical cancer. Cancer Research and Treatment, 48(1), 259–265.
Lang, H. C., Chang, K., & Ying, Y. H. (2012). Quality of life, treatments, and patients’ willingness to pay for a complete remission of cervical cancer in Taiwan. Health Economics, 21, 1217–1233.
Einstein, M. H., Rash, J. K., Cappell, R. J., Swietlik, J. M., Hollenberg, J. P., & Connor, J. P. (2012). Quality of life in cervical cancer survivors: Patient and provider perspectives on common complications of cervical cancer and treatment. Gynecologic Oncology, 125, 163–167.
Weaver, K. E., Forsythe, L. P., Reeve, B. B., Alfano, C. M., Rodriguez, J. L., Sabatino, S. A., et al. (2012). Mental and physical health-related quality of life among U.S. Cancer Survivors: Population estimates from the 2010 National Health Interview Survey. Cancer Epidemiology, Biomarkers and Prevention, 21, 2108–2117.
Klee, M., Thranov, I., & Machin, D. (2000). The patients’ perspective on physical symptoms after radiotherapy for cervical cancer. Gynecologic Oncology, 76, 14–23.
Yavas, G., Gogan, N. U., Yavas, C., Benzer, N., Yuce, D., & Celik, C. (2012). Prospective assessment of quality of life and psychological distress in patients with gynecologic malignancy. International Journal of Gynecological Cancer, 22, 1096–1101.
Greimel, E. R., Winter, R., Kapp, K. S., & Haas, J. (2009). Quality of life and sexual functioning after cervical cancer treatment: A long-term follow-up study. Psycho-oncology, 18, 476–482.
Hsu, W. C., Chung, N. N., Chen, Y. C., Ting, L. L., Wang, P. M., Hsieh, P. C., et al. (2009). Comparison of surgery or radiotherapy on complications and quality of life in patients with stage IB and IIA uterine cervical cancer. Gynecologic Oncology, 115, 41–45.
Bjelic-Radisic, V., Jensen, P. T., Vlasic, K. K., Waldenstrom, A. C., Springer, S., Chie, W., et al. (2012). Quality of life characteristics in patients with cervical cancer. European Journal of Cancer, 48, 3009–3018.
Frumovitz, M., Sun, C. C., Schover, L. R., Munsell, M. F., Jhingran, A., Wharton, J. T., et al. (2005). Quality of life and sexual functioning in cervical cancer survivors. Journal of Clinical Oncology, 23(30), 7428–7436.
Vistad, I., Fossa, S. D., & Dahl, A. A. (2006). A critical review of patient-rated quality of life studies of long-term survivors of cervical cancer. Gynecologic Oncology, 102, 563–572.
Westin, S. N., Sun, C. C., Tung, C. S., Lacour, R. A., Meyer, L. A., Urbauer, D. L., et al. (2016). Survivors of gynecologic malignancies: Impact of treatment on health and well-being. Journal of Cancer Survivorship, 10, 261–270.
Chie, W. C., Yang, C. H., Hsu, C., & Yang, P. C. (2004). Quality of life of lung cancer: Validation of the Taiwanese Chinese version of the EORTC QLQ-C30 and QLQ-LC13. Quality of Life Research, 13(1), 257–262.
Aaronson, N. K., Kaasa, S., Ahmedzai, S., Bergman, B., Bullinger, M., Cull, A., et al. (1993). The European Organization for Research and Treatment of Cancer QLQ-C30: A quality-of-life instrument for use in international clinical trials in oncology. Journal of the National Cancer Institute, 85(5), 365–376.
Greimel, E. R., Vlasic, K. K., Waldenstrom, A. C., Duric, V. M., Jensen, P. T., Singer, S., et al. (2006). The European Organization for Research and Treatment of Cancer (EORTC) Quality-of-Life Questionnaire Cervical Cancer Module. Cancer, 107(8), 1812–1822.
Korfage, I. J., Essink-Bot, M.-L., Mols, F., Poll-Franse, L. V. D., Kruitwagen, R., & Ballegooijen, M. V. (2009). Health-related quality of life in cervical cancer survivors: A population-based survey. International Journal of Radiation Oncology Biology Physics, 73(5), 1501–1509.
Singh, G. K., Miller, B. A., Hankey, B. F., & Edwards, B. K. (2004). Persistent area socioeconomic disparities in U.S. incidence of cervical cancer, mortality, stage, and survival, 1975–2000. Cancer, 101, 1051–1057.
Ramesh, H. S. J., Boase, T., & Audisio, R. A. (2006). Risk assessment for cancer surgery in elderly patients. Clinical Interventions in Aging, 1(3), 221–227.
Nogueira-Rodrigues, A., de Melo, A. C., Garces, A. H. I., Paulino, E., Alves, F. V. G., Vilaça Mdo, N., et al. (2016). Patterns of care and outcome of elderly women diagnosed with cervical cancer in the developing world. International Journal of Gynecological Cancer, 26(7), 1246–1251.
Nosaka, K., Shibata, K., Utsumi, F., Yoshida, K., Niimi, K., Sekiya, R., et al. (2016). Feasibility and benefit of concurrent chemoradiotherapy for elderly patients with uterine cervical cancer. Tumori. doi:10.5301/tj.5000530.
Yoshida, K., Sasaki, R., Nishimura, H., Miyawaki, D., Kawabe, T., Okamoto, Y., et al. (2011). Radiotherapy for Japanese elderly patients with cervical cancer: Preliminary survival outcomes and evaluation of treatment-related toxicity. Archives of Gynecology and Obstetrics, 284, 1007–1014.
Koh, W.-J., Geer, B. E., Abu-Rustum, N. R., Campos, S. M., Cho, K. R., Chon, H. S., et al. (2016). NCCN clinical practice guidelines in oncology: Cervical cancer. Resource document. National Comprehensive Cancer Network. https://www.nccn.org/professionals/physician_gls/f_guidelines.asp#site. Accessed 22 December 2016.
Kim, M.-K., Sim, J. A., Yun, Y. H., Bae, D.-S., Nam, J. H., Park, C. T., et al. (2016). Health-related quality of life and sociodemographic characteristics as prognostic indicators of long-term survival in disease-free cervical cancer survivors. International Journal of Gynecological Cancer, 26(4), 743–749.
Hazewinkel, M. H., Sprangers, M. A., Velden, J. V. D., Burger, M. P. M., & Roovers, J.-P. W. R. (2012). Severe pelvic floor symptoms after cervical cancer treatment are predominantly associated with mental and physical well-being and body image: A cross-sectional study. International Journal of Gynecological Cancer, 22(1), 154–160.
Kirwan, J. M., Symonds, P., Green, J. A., Tierney, J., Collingwood, M., & Williams, C. J. (2003). A systematic review of acute and late toxicity of concomitant chemoradiation for cervical cancer. Radiotherapy and Oncology, 68, 217–226.
Davidson, S. (2011). Treatment for advanced cervical cancer: Impact on quality of life. Critical Reviews in Oncology/Hematology, 79, 24–30.
Pfaendler, K. S., Wenzel, L., Mechanic, M. B., & Penner, K. R. (2015). Cervical cancer survivorship: Long-term quality of life and social support. Clinical Therapeutics, 37(1), 39–48.
Sekse, R. J. T., Hufthammer, K. O., & Vika, M. E. (2014). Fatigue and quality of life in women treated for various types of gynaecological cancers: A cross-sectional study. Journal of Clinical Nursing, 24, 546–555.
Vistad, I., Fossa, S. D., Kristensen, G. B., & Dahl, A. A. (2007). Chronic fatigue and its correlates in long-term survivors of cervical cancer treated with radiotherapy. BJOG: An International Journal of Obstetrics and Gynaecology, 114(9), 1150–1158.
Kirchheiner, K., Potter, R., Tanderup, K., Lindegaard, J. C., Haie-Meder, C., Petric, P., et al. (2016). Health-related quality of life in locally advanced cervical cancer patients after definitive chemoradiation therapy including image guided adaptive brachytherapy: An analysis from the EMBRACE study. International Journal of Radiation Oncology Biology Physics, 94(5), 1088–1098.
Bye, A., Trope, C., Loge, J. H., Hjermstad, M., & Kaasa, S. (2000). Health-related quality of life and occurrence of intestinal side effects after pelvic radiotherapy: Evaluation of long-term effects of diagnosis and treatment. Acta Oncologica, 39(2), 173–180.
Carlsson, M., Strang, P., & Bjurstrom, C. (2000). Treatment modality affects long-term quality of life in gynaecological cancer. Anticancer Research, 20, 563–568.
Jones, J. M., Olson, K., Catton, P., Catton, C. N., Fleshner, N. E., Krzyzanowska, M. K., et al. (2016). Cancer-related fatigue and associated disability in post-treatment cancer survivors. Journal of Cancer Survivorship, 10, 51–61.
Pearson, E. J. M., Morris, M. E., Di Stefano, M., & McKinstry, C. E. (2016). Interventions for cancer-related fatigue: A scoping review. European Journal of Cancer Care. doi:10.1111/ecc.12516.
Meneses-Echávez, J. F., González-Jiménez, E., & Ramírez-Vélez, R. (2015). Effects of supervised multimodal exercise interventions on cancer-related fatigue: Systematic review and meta-analysis of randomized controlled trials. BioMed Research International, 2015, 1–13.
Timmerman, L. G., Weering, M. G. H. D.-V., Tonis, T. M., Hermens, H. J., & Vollenbroek-Hutten, M. M. R. (2015). Relationship between patterns of daily physical activity and fatigue in cancer survivors. European Journal of Oncology Nursing, 19, 162–168.
Obama, K., Maru, M., Maeda, R., & Kubota, T. (2015). Cancer-related fatigue and physical activity among premenopausal cervical and endometrial cancer survivors in Japan. Journal of Medical and Dental Sciences, 62, 57–68.
Du Toit, G. C., & Kidd, M. (2015). Prospective quality of life study of South African women undergoing treatment for advanced-stage cervical cancer. Clinical Therapeutics, 37(10), 2324–2331.
Barnes, W., Waggoner, S., Delgado, G., Maher, K., Potkul, R., Barter, J., et al. (1991). Manometric characterization of rectal dysfunction following radical hysterectomy. Gynecologic Oncology, 42, 116–119.
Kim, H. S., Kim, K., Ryoo, S.-B., Seo, J. H., Kim, S. Y., Park, J. W., et al. (2015). Conventional versus nerve-sparing radical surgery for cervical cancer: A meta-analysis. Journal of Gynecologic Oncology, 26, 100–110.
Park, S. Y., Bae, D.-S., Nam, J. H., Park, C.-T., Cho, C.-H., Lee, J. M., et al. (2007). Quality of life and sexual problems in disease-free survivors of cervical cancer compared with the general population. Cancer, 110, 2716–2725.
Eifel, P. J. (2006). Concurrent chemotherapy and radiation therapy as the standard of care for cervical cancer. Nature Clinical Practice Oncology, 3(5), 248–255.
Burns, M., Costello, J., Ryan-Woolley, B., & Davidson, S. (2007). Assessing the impact of late treatment effects in cervical cancer: An exploratory study of women’s sexuality. European Journal of Cancer Care, 16, 364–372.
Buković, D., Silovski, H., Silovski, T., Hojsak, I., Šakić, K., & Hrgović, Z. (2008). Sexual functioning and body image of patients treated for ovarian cancer. Sexuality and Disability, 26, 63–73.
Juraskova, I., Butow, P., Robertson, R., Sharpe, L., McLeod, C., & Hacker, N. (2003). Post-treatment sexual adjustment following cervical and endometrial cancer: A qualitative insight. Psycho-Oncology, 12(3), 267–279.
Ye, S., Yang, J., Cao, D., Lang, J., & Shen, K. (2014). A systematic review of quality of life and sexual function of patients with cervical cancer after treatment. International Journal of Gynecological Cancer, 24, 1146–1157.
Jensen, P. T., Groenvold, M., Klee, M. C., Thranov, I., Petersen, M. A., & Machin, D. (2004). Early-stage cervical carcinoma, radical hysterectomy, and sexual function. Cancer, 100, 97–106.
Jensen, P. T., Groenvold, M., Klee, M. C., Thranov, I., Petersen, M. A., & Machin, D. (2003). Longitudinal study of sexual function and vaginal changes after radiotherapy for cervical cancer. International Journal of Radiation Oncology Biology Physics, 56, 937–949.
Pieterse, Q. D., Kenter, G. G., Maas, C. P., de Kroon, C. D., Creutzberg, C. L., Trimbos, J. B. M. Z., et al. (2013). Self-reported sexual, bowel and bladder function in cervical cancer patients following different treatment modalities: Longitudinal prospective cohort study. International Journal of Gynecological Cancer, 23(9), 1717–1725.
Ganz, P. A., Desmond, K. A., Belin, T. R., Meyerowitz, B. E., & Rowland, J. H. (1999). Predictors of sexual health in women after a breast cancer diagnosis. Journal of Clinical Oncology, 17(8), 2371–2380.
Bezjak, A., Tu, D., Bacon, M., Osoba, D., Zee, B., Stuart, G., et al. (2004). Quality of life in ovarian cancer patients: Comparison of paclitaxel plus cisplatin, with cyclophosphamide plus cisplatin in a randomized study. Journal of Clinical Oncology, 22(22), 4595–4603.
Herzog, T. J., & Wright, J. D. (2007). The impact of cervical cancer on quality of life: The components and means for management. Gynecologic Oncology, 107, 572–577.
Bukovic, D., Strinic, T., Habek, M., Hojsak, I., Silovski, H., Krhen, I., et al. (2003). Sexual life after cervical carcinoma. Collegium Antropologicum, 27, 173–180.
Acknowledgements
This study was support by the Ministry of Science and Technology (NMRPD1C0092) and LinKou Chang Gung Memorial Hospital (BMRPD37A). All authors sincerely thank all participants for generously sharing their experiences in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, CC., Chang, TC., Tsai, YF. et al. Quality of life among survivors of early-stage cervical cancer in Taiwan: an exploration of treatment modality differences. Qual Life Res 26, 2773–2782 (2017). https://doi.org/10.1007/s11136-017-1619-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-017-1619-0