Abstract
Purpose
Acromegaly has traditionally been associated with significant mortality and cardiovascular morbidity. The aim of this study was to assess the overall mortality and improvement in mortality and morbidity in acromegaly and correlate these with cumulative growth hormone exposure.
Methods
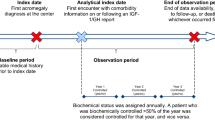
All patients treated for acromegaly at our centre until 2012 were analysed in this retrospective observational study. Baseline demographic details such as age at diagnoses, radiological features and pituitary status were obtained on these 167 patients. Cumulative GH levels (GHy) were calculated as a sum of average of GH readings in consecutive years. Mortality rates and development of new diabetes, hypertension and cardiovascular events (stroke, congestive cardiac failure and ischaemic heart disease) were assessed.
Results
The SMR for overall cohort was 1.6. There has been a significant improvement in SMR over the past two decades (SMR until 1992 2.5; SMR since 1992 1.0). Cumulative GH exposure was significantly high in patients who died (35.2 vs 24.1, p < 0.01) and in those with incident metabolic or vascular events during follow up (51.6 vs 24.4, p = 0.0001). The cardiovascular event rate of the ‘new’ cohort was significantly better than the ‘old’ cohort (8.0 vs. 29.1 %, p < 0.001).
Conclusion
There has been significant improvement in mortality and morbidity associated with acromegaly, in the setting of routine care in a specialized endocrine unit. Early and effective treatment to ‘control’ acromegaly could reduce GH exposure and hence vascular comorbidities.

Similar content being viewed by others
References
Kauppinen-Makelin R, Sane T, Reunanen A, Valimaki MJ, Niskanen L, Markkanen H, Loyttyniemi E, Ebeling T, Jaatinen P, Laine H, Nuutila P, Salmela P, Salmi J, Stenman UH, Viikari J, Voutilainen E (2005) A nationwide survey of mortality in acromegaly. J Clin Endocrinol Metab 90:4081–4086
Colao A, Ferone D, Marzullo P, Lombardi G (2004) Systemic complications of acromegaly: epidemiology, pathogenesis, and management. Endocr Rev 25:102–152
Alexander L, Appleton D, Hall R, Ross WM, Wilkinson R (1980) Epidemiology of acromegaly in the Newcastle region. Clin Endocrinol (Oxf) 12:71–79
Wright AD, Hill DM, Lowy C, Fraser TR (1970) Mortality in acromegaly. Q J Med 39:1–16
Abosch A, Tyrrell JB, Lamborn KR, Hannegan LT, Applebury CB, Wilson CB (1998) Transsphenoidal microsurgery for growth hormone-secreting pituitary adenomas: initial outcome and long-term results. J Clin Endocrinol Metab 83:3411–3418
Arita K, Kurisu K, Tominaga A, Eguchi K, Iida K, Uozumi T, Kazagi F (2003) Mortality in 154 surgically treated patients with acromegaly—a 10-year follow-up survey. Endocr J 50:163–172
Cozzi R, Attanasio R, Montini M, Pagani G, Lasio G, Lodrini S, Barausse M, Albizzi M, Dallabonzana D, Pedroncelli AM (2003) Four-year treatment with octreotide-long-acting repeatable in 110 acromegalic patients: predictive value of short-term results? J Clin Endocrinol Metab 88:3090–3098
Rolston JD, Blevins LS Jr (2012) Gamma knife radiosurgery for acromegaly. Int J Endocrinol 2012:821579. doi:10.1155/2012/821579
Trainer PJ, Drake WM, Katznelson L, Freda PU, Herman-Bonert V, van der Lely AJ, Dimaraki EV, Stewart PM, Friend KE, Vance ML, Besser GM, Scarlett JA, Thorner MO, Parkinson C, Klibanski A, Powell JS, Barkan AL, Sheppard MC, Malsonado M, Rose DR, Clemmons DR, Johannsson G, Bengtsson BA, Stavrou S, Kleinberg DL, Cook DM, Phillips LS, Bidlingmaier M, Strasburger CJ, Hackett S, Zib K, Bennett WF, Davis RJ (2000) Treatment of acromegaly with the growth hormone-receptor antagonist pegvisomant. N Engl J Med 342:1171–1177
Ayuk J, Clayton RN, Holder G, Sheppard MC, Stewart PM, Bates AS (2004) Growth hormone and pituitary radiotherapy, but not serum insulin-like growth factor-I concentrations, predict excess mortality in patients with acromegaly. J Clin Endocrinol Metab 89:1613–1617
Beauregard C, Truong U, Hardy J, Serri O (2003) Long-term outcome and mortality after transsphenoidal adenomectomy for acromegaly. Clin Endocrinol (Oxf) 58:86–91
Holdaway IM, Rajasoorya RC, Gamble GD (2004) Factors influencing mortality in acromegaly. J Clin Endocrinol Metab 89:667–674
Bates AS, Van’t Hoff W, Jones JM, Clayton RN (1993) An audit of outcome of treatment in acromegaly. Q J Med 86:293–299
Dekkers OM, Biermasz NR, Pereira AM, Romijn JA, Vandenbroucke JP (2008) Mortality in acromegaly: a metaanalysis. J Clin Endocrinol Metab 93:61–67
Jenkins D, O’Brien I, Johnson A, Shakespear R, Sheppard MC, Stewart PM (1995) The Birmingham pituitary database: auditing the outcome of the treatment of acromegaly. Clin Endocrinol (Oxf) 43:517–522
Biermasz NR, Dekker FW, Pereira AM, van Thiel SW, Schutte PJ, van Dulken H, Romijn JA, Roelfsema F (2004) Determinants of survival in treated acromegaly in a single center: predictive value of serial insulin-like growth factor I measurements. J Clin Endocrinol Metab 89:2789–2796
Swearingen B, Barker FG, Katznelson L, Biller BM, Grinspoon S, Klibanski A, Moayeri N, Black PM, Zervas NT (1998) Long-term mortality after transsphenoidal surgery and adjunctive therapy for acromegaly. J Clin Endocrinol Metab 83:3419–3426
Ayuk J, Sheppard MC, Clayton RN, Bates AS, Stewart PM (2004) Evidence for the use of igf-I as a predictor of mortality in acromegaly is lacking. J Clin Endocrinol Metab 89:5867–5868
Tomlinson JW, Holden N, Hills RK, Wheatley K, Clayton RN, Bates AS, Sheppard MC, Stewart PM (2001) Association between premature mortality and hypopituitarism. West Midlands Prospective Hypopituitary Study Group. Lancet 357:425–431
Rosen T, Bengtsson BA (1990) Premature mortality due to cardiovascular disease in hypopituitarism. Lancet 336:285–288
Sherlock M, Reulen RC, Aragon-Alonso A, Ayuk J, Clayton RN, Sheppard MC, Hawkins MM, Bates AS, Stewart PM (2014) A paradigm shift in the monitoring of patients with acromegaly: last available growth hormone may overestimate risk. J Clin Endocrinol Metab 99:478–485
Jayasena CN, Comninos AN, Clarke H, Donaldson M, Meeran K, Dhillo WS (2011) The effects of long-term growth hormone and insulin-like growth factor-1 exposure on the development of cardiovascular, cerebrovascular and metabolic co-morbidities in treated patients with acromegaly. Clin Endocrinol (Oxf) 75:220–225
Melmed S, Casanueva FF, Klibanski A, Bronstein MD, Chanson P, Lamberts SW, Strasburger CJ, Wass JA, Giustina A (2013) A consensus on the diagnosis and treatment of acromegaly complications. Pituitary 16:294–302
Sherlock M, Reulen RC, Alonso AA, Ayuk J, Clayton RN, Sheppard MC, Hawkins MM, Bates AS, Stewart PM (2009) ACTH deficiency, higher doses of hydrocortisone replacement, and radiotherapy are independent predictors of mortality in patients with acromegaly. J Clin Endocrinol Metab 94:4216–4223
Bengtsson BA, Eden S, Ernest I, Oden A, Sjogren B (1988) Epidemiology and long-term survival in acromegaly. A study of 166 cases diagnosed between 1955 and 1984. Acta Med Scand 223:327–335
Arosio M, Reimondo G, Malchiodi E, Berchialla P, Borraccino A, De Marinis L, Pivonello R, Grottoli S, Losa M, Cannavo S, Minuto F, Montini M, Bondanelli M, De Menis E, Martini C, Angeletti G, Velardo A, Peri A, Faustini-Fustini M, Tita P, Pigliaru F, Borretta G, Scaroni C, Bazzoni N, Bianchi A, Appetecchia M, Cavagnini F, Lombardi G, Ghigo E, Beck-Peccoz P, Colao A, Terzolo M, Italian Study Group of Acromegaly (2012) Predictors of morbidity and mortality in acromegaly: an Italian survey. Eur J Endocrinol 167:189–198
Orme SM, McNally RJ, Cartwright RA, Belchetz PE (1998) Mortality and cancer incidence in acromegaly: a retrospective cohort study. United Kingdom Acromegaly Study Group. J Clin Endocrinol Metab 83:2730–2734
Nachtigall L, Delgado A, Swearingen B, Lee H, Zerikly R, Klibanski A (2008) Changing patterns in diagnosis and therapy of acromegaly over two decades. J Clin Endocrinol Metab 93:2035–2041
Vallette S, Ezzat S, Chik C, Ur E, Imran SA, Van Uum S, Rivera J, Caspar-Bell G, Serri O (2013) Emerging trends in the diagnosis and treatment of acromegaly in Canada. Clin Endocrinol (Oxf) 79:79–85
Jayasena CN, Izzi-Engbeaya C, Narayanaswamy S, Modi M, Clarke H, Nijher GM, Meeran K, Dhillo WS (2015) Associations of coefficient of variation of serum GH with previous radiotherapy, hypopituitarism and cardiac disease in patients with treated acromegaly. Clin Endocrinol (Oxf) 82:870–875
Dutta P, Hajela A, Pathak A, Bhansali A, Radotra BD, Vashishta RK, Korbonits M, Khandelwal N, Walia R, Sachdeva N, Singh P, Murlidharan R, Devgun JS, Mukherjee KK (2015) Clinical profile and outcome of patients with acromegaly according to the 2014 consensus guidelines: impact of a multi-disciplinary team. Neurol India 63:360–368
Schofl C, Grussendorf M, Honegger J, Tonjes A, Thyroke-Gronostay D, Mayr B, Schopohl J, Participants of German Acromegaly Register (2015) Failure to achieve disease control in acromegaly: cause analysis by a registry-based survey. Eur J Endocrinol. 172:351–356
Schofl C, Franz H, Grussendorf M, Honegger J, Jaursch-Hancke C, Mayr B, Mayr B, Schopohl J, Participants of the German Acromegaly Register (2012) Long-term outcome in patients with acromegaly: analysis of 1344 patients from the German Acromegaly Register. Eur J Endocrinol. 168:39–47
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Nothing to declare.
Rights and permissions
About this article
Cite this article
Varadhan, L., Reulen, R.C., Brown, M. et al. The role of cumulative growth hormone exposure in determining mortality and morbidity in acromegaly: a single centre study. Pituitary 19, 251–261 (2016). https://doi.org/10.1007/s11102-015-0700-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-015-0700-3