Abstract
Background
The efficacy of various common treatment options for dry eye disease (DED) has been investigated against placebo. However, the potential beneficial effect of placebo in the management of DED is still unclear.
Aim
This meta-analysis investigated the impact of placebo administration in DED in Ocular Surface Disease Index (OSDI), Schirmer I test (SIT), tear breakup time (TBUT), corneal staining, and complications.
Method
This meta-analysis and systematic review was conducted according to the 2020 PRISMA guidelines. In March 2022, Pubmed, Web of Science, Google Scholar, and Embase were accessed. All the randomised clinical trials which investigated any active treatment against a placebo control group were considered. The following data were extracted at baseline and at last follow-up: Ocular Surface Disease Index (OSDI), tear breakup time test (TBUT), Schirmer I test (SIT), corneal staining.
Results
Data from 56 studies (12,205 patients) were retrieved. Placebo administration is not effective in improving TBUT (P = 0.3), OSDI (P = 0.2), SIT (P = 0.1) and corneal staining (P = 0.1) from baseline to last follow-up. Active treatment led to a higher TBUT and SIT compared to placebo administration (P < 0.0001). The active treatment resulted in a lower OSDI compared to placebo administration (P = 0.0005). Five studies reported data on the corneal staining. No difference was found between placebo administration and active treatment (P = 0.8).
Conclusion
Placebo administration does not impact symptoms of DED and can be successfully employed to evaluate the efficacy of active treatments.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Impact statements
-
Placebo administration is not effective in improving symptoms of dry eye disease
-
Placebo administration can be considered as a safe passive comparator to evaluate efficacy and safety of active treatments in dry eye disease
Introduction
Dry eye disease (DED) is a common condition of the ocular surface [1], with a prevalence of up to 50% of the global population [2]. Etiological factors include ocular surface inflammation and damage, neurosensory abnormalities, and tear film instability, which is caused by insufficient tear production or quality of the tear film [3]. The main subtypes of DED are aqueous deficient and evaporative DED, with frequent co-existence of both subtypes [2]. DED results in visual disturbance, burning, pain, and photophobia [4, 5]. Conventional therapies for DED include artificial tears, punctal occlusion, topical corticosteroids or secretagogues, and oral essential fatty acid supplementation [6,7,8,9]. Artificial tears are a mainstay therapy as they provide an affordable and immediate relief [10]. However, as inflammation is a key component in the pathogenesis of DED, artificial tears might be inadequate in improving the ocular surface damage in patients with more severe DED. Recently, the importance of drugs with anti-inflammatory or secretagogue properties has been highlighted in such cases [11].
In randomized controlled trials (RCTs), the efficacy of an active treatment is commonly evaluated by the difference in outcome between the intervention and placebo group [12]. The placebo effect describes a phenomenon of improvement of symptoms in patients receiving an inert substance [13]. Placebo administration can actually be more beneficial than no-treatment in many clinical settings [14]. Therefore, the clinical impact of a placebo might be neglected [15], resulting in an “efficacy paradox” [16]. This term describes the discrepancy between the treatment efficacy suggested by RCTs and the treatment efficacy observed in the clinical practice [16]. The rate of placebo effect in RCTs investigating various conditions is estimated at 30–40% [17,18,19]. The placebo effect lowers the statistical power of RCTs, challenging the interpretation of the treatment effects [20]. Placebo effects have been attributed to complex processes, such as behavioural conditioning, patients’ expectations, regression to the mean, and the Hawthorne effect [21,22,23,24]. Regression to the mean describes that extreme outliers tend to a more average value [24]. In clinical practice, patients with a symptomatic condition often tend to improve spontaneously, even without treatment [24]. The Hawthorne effect relates to a change in behaviour of individuals in response to the perception of being observed [25]. Therefore, it affects the generalisability of RCTs to clinical practice [25]. Placebo administration is a major methodological challenge in RCTs investigating DED [27]. The special feature of DED trials is that placebo administration might involve adding a liquid to the ocular surface with possible inherent therapeutic effects in DED [27]. Recently, the processes involved in inducing a placebo effect have been investigated, but the exact mechanisms underlying the placebo effects are not fully understood yet [26]. In some RCTs, patients received a placebo prior to the randomisation procedure to reduce the placebo effects during the treatment period [9, 28, 29]. However, placebo effects were evidenced also in these studies [27]. The efficacy of various common treatment options for DED has been investigated in the clinical setting using placebo as a comparator [7, 9, 29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85].
Aim
This meta-analysis investigated the impact of placebo administration in DED in Ocular Surface Disease Index (OSDI), Schirmer I test (SIT), tear breakup time (TBUT), corneal staining, and complications.
Method
Eligibility criteria
All the randomised clinical trials which investigated any active treatment with a placebo control group were accessed. According to the authors language capabilities, articles in English, German, Italian, French and Spanish were eligible. Only level I of evidence studies, according to Oxford Centre of Evidence-Based Medicine [86], were considered. Only studies published in peer reviewed journals were considered. Reviews, opinions, letters, editorials were not considered. Animal and in vitro studies were not eligible.
Search strategy
This meta-analysis and systematic review was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses: the 2020 PRISMA statement [87]. The PICOT algorithm was preliminary pointed out:
-
P (Population): DED;
-
I (Intervention): Placebo;
-
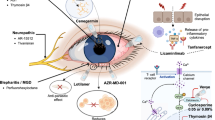
C (Comparison): Different active treatment (including artificial tears, omega-3 and omega-6 fatty acids, intense pulsed light, acupuncture, cyclosporine, loteprednol, betamethasone, rebamipide, diquafosol tetrasodium, uridine, lifitegrast, botulinumtoxin-A, CF101 (adenosine receptor agonist), SkQ1 (Visomitin), SAR 1118 (integrin antagonist), isunakinra (topical interleukin-1 receptor inhibitor), bevacizumab, canakinumab, secukinumab, Royal Jelly, vitamin A, D-3-Hydroxybutyrate, tretinoin, olopatadine hydrochloride, OTX-101, thymosin b4)
-
O (Outcomes): Ocular Surface Disease Index; Tear breakup time test; Schirmer I test, Corneal Staining.
In March 2022, the following databases were accessed: PubMed, Web of Science, Google Scholar, Embase. Only randomized controlled trials were taken into consideration. No time constraint was set for the search. The following keywords were used for the search bar with the Boolean operators AND/OR: xerophthalmus, dry eye disease, xeropthalmia, placebo, management, therapy, Ocular Surface Disease Index; Tear breakup time test; TBUT; Schirmer I test, SIT; Corneal Staining (Supplementary material 1).
Selection and data collection
Two authors (F.M. and J.P.) independently performed the database search. All the resulting titles were screened and, if suitable, the abstract was accessed. The full-texts of the abstracts which matched the topic of interest were accessed. If the full-text of the article was not retrievable or accessible, the study was excluded. The bibliography of the full-text articles was also screened by hand. Any disagreements were discussed and settled by consensus.
Data items
Two authors (F.M. and J.P.) independently performed data extraction. Study generalities (author, year, journal, number of patients, mean age, women) were extracted. The following data were extracted at baseline and at last follow-up: OSDI [88], TBUT [89], SIT [90], corneal staining.
Assessment of the risk of bias and quality of recommendations
The between studies risk of bias assessment was evaluated using the risk of bias tool of the Review Manager software (The Nordic Cochrane Collaboration, Copenhagen). The following biases were evaluated by an author independently (J.P.): selection, performance, detection, attrition, reporting, other sources of bias. To investigate the overall risk of publication bias, the funnel plot of the most reported outcome was performed. To grade the quality (or certainty) of evidence and strength of recommendations, the Grading of Recommendations Assessment, Development and Evaluation (GRADE) was performed [91].
Synthesis methods
The statistical analysis was performed by one authors (F.M.). To assess the improvement from baseline to the last follow-up, the IBM SPSS software version 25 was used. Mean difference (MD) and unpaired t-test were evaluated. For the comparisons, a meta-analysis was conducted using the Review Manager software (The Nordic Cochrane Collaboration, Copenhagen) version 5.3. Data were analyzed using the inverse variance and MD effect measure. The comparisons were performed with a fixed model effect as set up. Heterogeneity was assessed through the \(\chi \)2 and the Higgins-I2 test. If \(\chi \)2 < 0.05 and I2 test > 60%, a random model effect was adopted. The confidence intervals (CI) were set at 95% in all analyses. Values of P < 0.05 were considered statistically significant. Forest plots were performed for each comparison.
Results
Study selection
After screening the resulting titles, 998 articles were accessed. Of them, 479 were duplicates. A further 459 articles were excluded because of lack of randomization (n = 106), not comparing directly placebo with an active treatment (n = 211), not focusing on the topic (N = 44), language incompatibility (N = 7), including patients with Sjögren’s syndrome (N = 36), including postmenopausal patients (N = 16) or improper study design (N = 40). A further four studies were excluded as they lacked quantitative data. Finally, 56 articles were included in the meta-analysis. As a placebo, the studies included in this meta-analysis used saline [30, 33, 34, 37, 45, 47, 48, 53, 57, 71, 72, 74, 77] or balanced salt solution [35], vehicle drops [29, 43, 50, 52, 56, 61, 66,67,68, 80], artificial tears [81], sham pulsed light treatment [55, 78], sham acupuncture [92], an ophthalmic solution containing base only [36], oral vitamin E [39], olive oil [7, 42, 44, 51, 70, 75, 83], sunflower oil [59, 85], safflower oil [84], wheat germ oil [65], corn oil [54], palm and coconut oil [62, 63], medium-chain fatty acids [60], or tablets without the active ingredient with the same appearance as the active treatment [40, 46, 49, 58, 69, 79], placebo beverage with a similar texture, flavour, and taste as the active agent [31],1000 IU of vitamin A in a study using 100,000 IU of vitamin A as active treatment [76], or the placebo was not exactly specified [9, 41, 73, 82]. Therefore, the choice of placebo was heterogenous. The search strategy used for literature search in PubMed is reported in Supplementary material 1. The literature search results are shown in Fig. 1.
Study risk of bias assessment
Given the randomised nature of the studies selected, the risk of selection bias was low. Most authors performed blinding of participants, personnel, and assessor, leading to an overall low risk of performance and detection biases. Equally, the risk of detection and attrition biases were low. Finally, the risk of other bias was low to moderate. Concluding, the risk of bias graph evidenced a good quality of the methodological assessment (Fig. 2).
Risk of publication bias
To assess the overall risk of publication bias, the funnel plot of the most commonly reported outcome was performed and evaluated (SIT). The plot evidenced good symmetry, and the effects were located withing the pyramidal shapes of acceptability (Fig. 3). This indicates a low risk of publication bias.
Study characteristics and results of individual studies
Data from 4934 patients were retrieved. 73% (3602 of 4934 patients) were women. The mean follow-up was 12.2 ± 16.0 weeks. The mean age was 50.3 ± 14.5 years. Baseline comparability between the placebo and active treatment was found in terms of TBUT (P = 0.8), OSDI (P = 0.7), SIT (P = 0.7), corneal staining (P = 0.7). Generalities of the included studies are reported in Table 1, and the analysis of the baseline comparability is shown in Supplementary material 2.
Efficacy of placebo administration
Placebo administration is not effective in improving TBUT (P = 0.3), OSDI (P = 0.2), SIT (P = 0.1), and corneal staining (P = 0.1) from baseline to last follow-up (Supplementary material 3).
Efficacy of placebo administration compared to the active treatment
Active treatment evidenced a higher TBUT (MD 0.82; 95% CI 0.55 to 1.09; P < 0.0001), SIT (MD 0.61; 95% CI 0.41 to 0.82; P < 0.0001), and OSDI (MD − 2.79; 95% CI − 4.26 to − 1.21; P = 0.0005) compared to placebo administration. No difference was found between placebo administration and active treatment in corneal staining (P = 0.8). These results are shown in greater detail in Fig. 4
Quality of the recommendations
The level of evidence quality according to the GRADE system was high for TBUT, SIT, and OSDI, whereas a low level of evidence in quality for the corneal staining was evidenced (Fig. 5).
Discussion
Statement of key findings
The present study demonstrated that placebo administration did not improve symptoms of DED at the last follow-up. Placebo administration can therefore be considered as passive comparator to evaluate the efficacy and safety of active treatments in DED.
Strengths and weaknesses
The literature search was performed in Pubmed, Web of Science, Google Scholar and Embase, as previously recommended to guarantee efficient coverage [115]. Within the selection and data collection, no severe disagreements between the two responsible authors occurred. Therefore, no impact on internal validity must be expected. The present meta-analysis and systematic review was detailed and precise, but has several limitations. Firstly, the active treatment and the placebos protocols showed a high variability. Hypothetically, different effects might be attributable to different placebos. Selek et al. and Goldstein et al. attributed the symptomatic improvement witnessed in the placebo group to a lubricating effect of the vehicle itself on the ocular surface [73]. Shin et al. evaluated the efficacy of acupuncture for DED, and employed a sham acupuncture control group which they referred to as the placebo group [92]. Yet, placebo acupuncture is technically impossible. Accordingly, “sham” describes any control treatment of acupuncture aiming to make the patients believe that they received the real treatment [116, 117]. A superior efficacy of sham acupuncture compared to pharmacological placebo has been suggested [118]. Conversely, patients demonstrating a therapeutic effect to placebo were excluded after a 2-week-run-in period. Thereby, the risk of a strong placebo effect should be mitigated [61]. Moreover, the heterogeneous length of follow-up might also limit the reliability of our results. Given the lack of quantitative data available for inclusion, no further subgroups were possible to investigate. Hence, conclusions from the present study must be interpreted with caution.
Interpretation
Previously, Imanaka et al. investigated predictive factors of the placebo effect in trials for DED, collecting data from 205 patients enrolled in 3 placebo-controlled RCTs. High baseline scores and age affected the placebo responses of the corneal staining score [27]. Ageing is an essential risk factor for DED [27]. The high proportion of females (73%) in the present study agrees with previous publications and has been attributed to the effects of sex steroids including oestrogens, glucocorticoids, and epigenetics [93]. While the exact association of sex steroids and DED is still unclear, relatively low levels of serum androgen in females are associated to lower anti-inflammatory effects on the ocular surface, promoting DED [94]. Hypothetically, the placebo might have a beneficial effect in patients with high baseline scores by acting as artificial tears [27]. Also, the greater placebo effect in patients with high baseline scores can be attributed to the regression to the mean phenomenon [24]. In other conditions, such as low back pain, a previous meta-analysis showed rapid symptom improvement in the first 6 weeks and less marked improvement thereafter both in the treatment and placebo groups [95]. Therefore, regression to the mean might commonly be falsely interpreted as efficacy, but occurs simply by chance and with time [96]. Placebo effects have been reported in patients with depression, cardiovascular diseases, asthma, and different pain syndromes [97,98,99,100,101]. Notably, a systematic review collecting data from 72 RCTs with 9827 patients with fibromyalgia and 70 RCTs with 10,297 patients with diabetic neuropathy showed a superior effect of placebo administration compared to non-treatment. The placebo group showed a significant reduction of pain and fatigue [102]. It has been presumed that the examination by a doctor and the actual physical motions of taking medications can have therapeutic effects [96]. Placebo effects have been attributed to the release of substances such as endogenous opioids [103], endocannabinoids [104], dopamine [105], oxytocin [106], and vasopressin [107]. These substances show specific effects to the target system [101]. In addition, neuroimaging studies have shown changes similar to those caused by opioids in brain activation patterns induced by placebo [108]. In DED, patients show positive perceptions regarding the effectiveness of their treatments [109]. The improvement anticipated by the patient might be attributable to the measured improvement [110]. Notably, some of the studies included in this meta-analysis showed some beneficial effect of placebo on SIT [81, 83], TBUT [31, 75], corneal staining [53, 66, 75] or OSDI [7, 75, 79]. The small, nonstatistical reduction of corneal staining induced by placebo may well be regression to the mean [53]. Chang et al. investigated the efficacy of oral uridine compared to placebo on DED. They reported a reduction of corneal staining and improvement of SIT in the uridine compared to the placebo group with statistically significant differences between the groups. Moreover, treatment with uridine significantly reduced the OSDI score. However, the placebo group also showed some reduction of the OSDI score. The authors assume that these nonsignificant differences between the groups are attributable to the placebo effect [79]. In 2018, the Dry Eye Assessment and Management (DREAM) trial concluded that omega-3 fatty acid supplements do not provide better outcomes than placebo in the management of DED [75, 111]. As to adverse events, placebo proved safe in the studies considered for our meta-analysis. However, Kinoshita et al. reported that eye irritation occurred more frequently in the placebo than in the treatment (rebamipide) group. However, the authors did not specify what the placebo consisted of [9]. In the DREAM trial, the percentage of patients with at least one serious adverse event was 8.1% in the placebo group receiving olive oil. The percentage of patients with at least one nonserious adverse event was similar in the active treatment group and the placebo group (61.9% and 60.8%, respectively) [75]. In the DREAM extension study, one patient in the placebo group was hospitalized for dyspnoea as a serious adverse event [83]. A randomized study published in 2017 reported that patients were more likely to report adverse events when they were aware that they received statin therapy than when they were blinded [112]. Therefore, negative expectations of the patients regarding the treatment with either active or inert substance might cause a negative placebo effect, called the nocebo effect [112]. Nocebo effects have been described in many clinical contexts. Up to 19% of adult and 26% of elderly patients receiving placebos report side effects [113]. They have been partly attributed to the verbal suggesting in the context of informed-consent process [101]: in the clinical setting, expectancies might be affected by the preceding description of the treatment [101]. On a neurobiological level, the nocebo effect has been shown to be mediated by cholecystokinin [114] and to be associated with hyperactivity of the hypothalamic–pituitary–adrenal axis [101]. This increased activity is antagonized by benzodiazepine, which suggests the role of anxiety of patients in nocebo effects [101].
Further research
Altogether, distinguishing whether an observed effect is secondary to placebo, regression to the mean, or simply part of the course of the disease, can be challenging [96]. The exact intensity of the placebo effects in clinical trials on DED remains difficult to determine. In patients with DED, placebo did not show beneficial therapeutic effects, but was safe. However, no subgroup analysis could be performed given the lack of quantitative data available for inclusion. Therefore, further research is warranted to focus on evaluating different types of placebo administration in DED.
Conclusion
Placebo administration does not impact symptoms of DED and can be successfully administered to evaluate the efficacy of active treatments. These conclusions must be interpreted within the limitations of the present study.
References
Alshamrani AA, Almousa AS, Almulhim AA, et al. Prevalence and risk factors of dry eye symptoms in a Saudi Arabian population. Middle East Afr J Ophthalmol. 2017;24(2):67–73.
Craig JP, Nelson JD, Azar DT, et al. TFOS DEWS II report executive summary. Ocul Surf. 2017;15(4):802–12.
Craig JP, Nichols KK, Akpek EK, et al. TFOS DEWS II definition and classification report. Ocul Surf. 2017;15(3):276–83.
Ohashi Y, Ishida R, Kojima T, et al. Abnormal protein profiles in tears with dry eye syndrome. Am J Ophthalmol. 2003;136(2):291–9.
Javadi MA, Feizi S. Dry eye syndrome. J Ophthalmic Vis Res. 2011;6(3):192–8.
Ervin AM, Law A, Pucker AD. Punctal occlusion for dry eye syndrome: summary of a Cochrane systematic review. Br J Ophthalmol. 2019;103(3):301–6.
Deinema LA, Vingrys AJ, Wong CY, et al. A randomized, double-masked, placebo-controlled clinical trial of two forms of omega-3 supplements for treating dry eye disease. Ophthalmology. 2017;124(1):43–52.
Mencucci R, Boccalini C, Caputo R, et al. Effect of a hyaluronic acid and carboxymethylcellulose ophthalmic solution on ocular comfort and tear-film instability after cataract surgery. J Cataract Refract Surg. 2015;41(8):1699–704.
Kinoshita S, Awamura S, Oshiden K, et al. Rebamipide (OPC-12759) in the treatment of dry eye: a randomized, double-masked, multicenter, placebo-controlled phase II study. Ophthalmology. 2012;119(12):2471–8.
Ang BCH, Sng JJ, Wang PXH, et al. Sodium hyaluronate in the treatment of dry eye syndrome: a systematic review and meta-analysis. Sci Rep. 2017;7(1):9013.
International Dry Eye WorkShop (2007) Management and therapy of dry eye disease: report of the Management and Therapy Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007;5(2):163–78.
Hafliðadóttir SH, Juhl CB, Nielsen SM, et al. Placebo response and effect in randomized clinical trials: meta-research with focus on contextual effects. Trials. 2021;22(1):493.
Roji R, Stone P, Ricciardi F, et al. Placebo response in trials of drug treatments for cancer-related fatigue: a systematic review, meta-analysis and meta-regression. BMJ Support Palliat Care. 2020;10(4):385–94.
Furukawa TA. Review: placebo is better than no treatment for subjective continuous outcomes and for treatment of pain. ACP J Club. 2002;136(1):20.
Zhang W, Doherty M. Efficacy paradox and proportional contextual effect (PCE). Clin Immunol. 2018;186:82–6.
Walach H. The efficacy paradox in randomized controlled trials of CAM and elsewhere: beware of the placebo trap. J Altern Complement Med. 2001;7(3):213–8.
Cho HJ, Hotopf M, Wessely S. The placebo response in the treatment of chronic fatigue syndrome: a systematic review and meta-analysis. Psychosom Med. 2005;67(2):301–13.
Furukawa TA, Cipriani A, Atkinson LZ, et al. Placebo response rates in antidepressant trials: a systematic review of published and unpublished double-blind randomised controlled studies. Lancet Psychiatry. 2016;3(11):1059–66.
Papakostas GI, Fava M. Does the probability of receiving placebo influence clinical trial outcome? A meta-regression of double-blind, randomized clinical trials in MDD. Eur Neuropsychopharmacol. 2009;19(1):34–40.
Howick J, Friedemann C, Tsakok M, et al. Are treatments more effective than placebos? A systematic review and meta-analysis. PLoS ONE. 2013;8(5):e62599.
Benedetti F. Mechanisms of placebo and placebo-related effects across diseases and treatments. Annu Rev Pharmacol Toxicol. 2008;48:33–60.
Price DD, Finniss DG, Benedetti F. A comprehensive review of the placebo effect: recent advances and current thought. Annu Rev Psychol. 2008;59:565–90.
Colloca L, Miller FG. Harnessing the placebo effect: the need for translational research. Philos Trans R Soc Lond B Biol Sci. 2011;366(1572):1922–30.
McDonald CJ, Mazzuca SA, McCabe GP Jr. How much of the placebo “effect” is really statistical regression? Stat Med. 1983;2(4):417–27.
McCarney R, Warner J, Iliffe S, et al. The Hawthorne effect: a randomised, controlled trial. BMC Med Res Methodol. 2007;7:30.
Horin AP, Lee KM, Colloca L. Placebo effects in therapeutic outcomes. Curr Clin Pharmacol. 2014;9(2):116–22.
Imanaka T, Sato I, Tanaka S, et al. Predictive factors for the placebo effect in clinical trials for dry eye: a pooled analysis of three clinical trials. Br J Ophthalmol. 2017;101(11):1471–4.
International Dry Eye WorkShop (2007) Design and conduct of clinical trials: report of the Clinical Trials Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf. 2007;5(2):153–62.
Sheppard JD, Torkildsen GL, Lonsdale JD, et al. Lifitegrast ophthalmic solution 5.0% for treatment of dry eye disease: results of the OPUS-1 phase 3 study. Ophthalmology. 2014;121(2):475–83.
Kasetsuwan N, Chantaralawan K, Reinprayoon U, et al. Efficacy of topical bevacizumab 0.05% eye drops in dry eye disease: a double-masked, randomized trial. PLoS ONE. 2020;15(6):e0234186.
Kawashima M, Tsuno S, Matsumoto M, et al. Hydrogen-producing milk to prevent reduction in tear stability in persons using visual display terminals. Ocul Surf. 2019;17(4):714–21.
Malhotra R, Devries DK, Luchs J, et al. Effect of OTX-101, a novel nanomicellar formulation of cyclosporine A, on corneal staining in patients with keratoconjunctivitis sicca: a pooled analysis of phase 2b/3 and phase 3 studies. Cornea. 2019;38(10):1259–65.
Choi MG, Yeo JH, Kang JW, et al. Effects of botulinum toxin type A on the treatment of dry eye disease and tear cytokines. Graefes Arch Clin Exp Ophthalmol. 2019;257(2):331–8.
Szegedi S, Scheschy U, Schmidl D, et al. Effect of single instillation of two hyaluronic acid-based topical lubricants on tear film thickness in patients with dry eye syndrome. J Ocul Pharmacol Ther. 2018;34(9):605–11.
He Y, Li J, Zhu J, et al. The improvement of dry eye after cataract surgery by intraoperative using ophthalmic viscosurgical devices on the surface of cornea: The results of a consort-compliant randomized controlled trial. Medicine (Baltimore). 2017;96(50):e8940.
Toshida H, Funaki T, Ono K, et al. Efficacy and safety of retinol palmitate ophthalmic solution in the treatment of dry eye: a Japanese Phase II clinical trial. Drug Des Devel Ther. 2017;11:1871–9.
Schmidl D, Werkmeister R, Kaya S, et al. A controlled, randomized double-blind study to evaluate the safety and efficacy of chitosan-N-acetylcysteine for the treatment of dry eye syndrome. J Ocul Pharmacol Ther. 2017;33(5):375–82.
Kheirkhah A, Di Zazzo A, Satitpitakul V, et al. A pilot randomized trial on safety and efficacy of a novel topical combined inhibitor of Janus kinase 1/3 and spleen tyrosine kinase for GVHD-associated ocular surface disease. Cornea. 2017;36(7):799–804.
Goyal P, Jain AK, Malhotra C. Oral omega-3 fatty acid supplementation for laser in situ keratomileusis-associated dry eye. Cornea. 2017;36(2):169–75.
Inoue S, Kawashima M, Hisamura R, et al. Clinical evaluation of a royal jelly supplementation for the restoration of dry eye: a prospective randomized double blind placebo controlled study and an experimental mouse model. PLoS ONE. 2017;12(1):e0169069.
Holland EJ, Luchs J, Karpecki PM, et al. Lifitegrast for the treatment of dry eye disease: results of a phase III, randomized, double-masked, placebo-controlled trial (OPUS-3). Ophthalmology. 2017;124(1):53–60.
Chinnery HR, Naranjo Golborne C, Downie LE. Omega-3 supplementation is neuroprotective to corneal nerves in dry eye disease: a pilot study. Ophthalmic Physiol Opt. 2017;37(4):473–81.
Goldstein MH, Martel JR, Sall K, et al. Multicenter Study Of A Novel Topical Interleukin-1 receptor inhibitor, isunakinra, in subjects with moderate to severe dry eye disease. Eye Contact Lens. 2017;43(5):287–96.
Bhargava R, Kumar P, Arora Y. Short-term omega 3 fatty acids treatment for dry eye in young and middle-aged visual display terminal users. Eye Contact Lens. 2016;42(4):231–6.
López-de la Rosa A, Pinto-Fraga J, Blázquez Arauzo F, et al. Safety and efficacy of an artificial tear containing 0.3% hyaluronic acid in the management of moderate-to-severe dry eye disease. Eye Contact Lens. 2017;43(6):383–8.
Petrov A, Perekhvatova N, Skulachev M, et al. SkQ1 ophthalmic solution for dry eye treatment: results of a phase 2 safety and efficacy clinical study in the environment and during challenge in the controlled adverse environment model. Adv Ther. 2016;33(1):96–115.
Kawakita T, Uchino M, Fukagawa K, et al. Randomized, multicenter, double-blind study of the safety and efficacy of 1%D-3-hydroxybutyrate eye drops for dry eye disease. Sci Rep. 2016;6:20855.
Baek J, Doh SH, Chung SK. The effect of topical diquafosol tetrasodium 3% on dry eye after cataract surgery. Curr Eye Res. 2016;41(10):1281–5.
Wang L, Chen X, Hao J, et al. Proper balance of omega-3 and omega-6 fatty acid supplements with topical cyclosporine attenuated contact lens-related dry eye syndrome. Inflammopharmacology. 2016;24(6):389–96.
Donnenfeld ED, Karpecki PM, Majmudar PA, et al. Safety of lifitegrast ophthalmic solution 5.0% in patients with dry eye disease: a 1-year, multicenter, randomized, placebo-controlled study. Cornea. 2016;35(6):741–8.
Bhargava R, Chandra M, Bansal U, et al. A randomized controlled trial of omega 3 fatty acids in rosacea patients with dry eye symptoms. Curr Eye Res. 2016;41(10):1274–80.
Brzheskiy VV, Efimova EL, Vorontsova TN, et al. Results of a multicenter, randomized, double-masked, placebo-controlled clinical study of the efficacy and safety of visomitin eye drops in patients with dry eye syndrome. Adv Ther. 2015;32(12):1263–79.
Grosskreutz CL, Hockey HU, Serra D, et al. Dry eye signs and symptoms persist during systemic neutralization of IL-1β by canakinumab or IL-17A by secukinumab. Cornea. 2015;34(12):1551–6.
Bhargava R, Kumar P. Oral omega-3 fatty acid treatment for dry eye in contact lens wearers. Cornea. 2015;34(4):413–20.
Craig JP, Chen YH, Turnbull PR. Prospective trial of intense pulsed light for the treatment of meibomian gland dysfunction. Invest Ophthalmol Vis Sci. 2015;56(3):1965–70.
Sosne G, Dunn SP, Kim C. Thymosin β4 significantly improves signs and symptoms of severe dry eye in a phase 2 randomized trial. Cornea. 2015;34(5):491–6.
Kaya S, Schmidl D, Schmetterer L, et al. Effect of hyaluronic acid on tear film thickness as assessed with ultra-high resolution optical coherence tomography. Acta Ophthalmol. 2015;93(5):439–43.
Kawakita T, Kawabata F, Tsuji T, et al. Effects of dietary supplementation with fish oil on dry eye syndrome subjects: randomized controlled trial. Biomed Res. 2013;34(5):215–20.
Sheppard JD Jr, Singh R, McClellan AJ, et al. Long-term supplementation with n-6 and n-3 PUFAs improves moderate-to-severe keratoconjunctivitis sicca: a randomized double-blind clinical trial. Cornea. 2013;32(10):1297–304.
Kangari H, Eftekhari MH, Sardari S, et al. Short-term consumption of oral omega-3 and dry eye syndrome. Ophthalmology. 2013;120(11):2191–6.
Semba CP, Torkildsen GL, Lonsdale JD, et al. A phase 2 randomized, double-masked, placebo-controlled study of a novel integrin antagonist (SAR 1118) for the treatment of dry eye. Am J Ophthalmol. 2012;153(6):1050–60.
Larmo PS, Järvinen RL, Setälä NL, et al. Oral sea buckthorn oil attenuates tear film osmolarity and symptoms in individuals with dry eye. J Nutr. 2010;140(8):1462–8.
Järvinen RL, Larmo PS, Setälä NL, et al. Effects of oral sea buckthorn oil on tear film Fatty acids in individuals with dry eye. Cornea. 2011;30(9):1013–9.
Lee JH, Han K, Kim TH, et al. Acupuncture for dry eye syndrome after refractive surgery: A randomized controlled pilot trial. Integr Med Res. 2021;10(1):100456.
Wojtowicz JC, Butovich I, Uchiyama E, et al. Pilot, prospective, randomized, double-masked, placebo-controlled clinical trial of an omega-3 supplement for dry eye. Cornea. 2011;30(3):308–14.
Villani E, Laganovska G, Viola F, et al. A multicenter, double-blind, parallel group, placebo-controlled clinical study to examine the safety and efficacy of T-Clair SPHP700-3 in the management of mild to moderate dry eye in adults. Cornea. 2011;30(3):265–8.
Vogel R, Crockett RS, Oden N, et al. Demonstration of efficacy in the treatment of dry eye disease with 0.18% sodium hyaluronate ophthalmic solution (Vismed, Rejena). Am J Ophthalmol. 2010;149(4):594–601.
Avni I, Garzozi HJ, Barequet IS, et al. Treatment of dry eye syndrome with orally administered CF101: data from a phase 2 clinical trial. Ophthalmology. 2010;117(7):1287–93.
Drouault-Holowacz S, Bieuvelet S, Burckel A, et al. Antioxidants intake and dry eye syndrome: a crossover, placebo-controlled, randomized trial. Eur J Ophthalmol. 2009;19(3):337–42.
Kokke KH, Morris JA, Lawrenson JG. Oral omega-6 essential fatty acid treatment in contact lens associated dry eye. Cont Lens Anterior Eye. 2008;31(3):141–6 (quiz 70).
Mah FS, O’Brien T, Kim T, et al. Evaluation of the effects of olopatadine ophthalmic solution, 0.2% on the ocular surface of patients with allergic conjunctivitis and dry eye. Curr Med Res Opin. 2008;24(2):441–7.
Johnson ME, Murphy PJ, Boulton M. Effectiveness of sodium hyaluronate eyedrops in the treatment of dry eye. Graefes Arch Clin Exp Ophthalmol. 2006;244(1):109–12.
Selek H, Unlü N, Orhan M, et al. Evaluation of retinoic acid ophthalmic emulsion in dry eye. Eur J Ophthalmol. 2000;10(2):121–7.
Aragona P, Papa V, Micali A, et al. Long term treatment with sodium hyaluronate-containing artificial tears reduces ocular surface damage in patients with dry eye. Br J Ophthalmol. 2002;86(2):181–4.
Asbell PA, Maguire MG, Pistilli M, et al. n-3 fatty acid supplementation for the treatment of dry eye disease. N Engl J Med. 2018;378(18):1681–90.
Katz J, West KP Jr, Khatry SK, et al. Impact of vitamin A supplementation on prevalence and incidence of xerophthalmia in Nepal. Invest Ophthalmol Vis Sci. 1995;36(13):2577–83.
Shokoohi-Rad S, Javaheri SZH, Malekabad FZ, et al. Effects of preoperative doses of betamethasone acetate 0.1% on dry eye control after cataract surgery. Indian J Ophthalmol. 2020;68(3):450–4.
Xue AL, Wang MTM, Ormonde SE, et al. Randomised double-masked placebo-controlled trial of the cumulative treatment efficacy profile of intense pulsed light therapy for meibomian gland dysfunction. Ocul Surf. 2020;18(2):286–97.
Chang KC, Oh JY, In YS, et al. Preliminary effects of oral uridine on the ocular surface in dry eye patients. J Korean Med Sci. 2009;24(4):701–7.
Pflugfelder SC, Maskin SL, Anderson B, et al. A randomized, double-masked, placebo-controlled, multicenter comparison of loteprednol etabonate ophthalmic suspension, 0.5%, and placebo for treatment of keratoconjunctivitis sicca in patients with delayed tear clearance. Am J Ophthalmol. 2004;138(3):444–57.
Willen CM, McGwin G, Liu B, et al. Efficacy of cyclosporine 0.05% ophthalmic emulsion in contact lens wearers with dry eyes. Eye Contact Lens. 2008;34(1):43–5.
Semba RD, Muhilal M, West Jr KP, et al. Hyporetinolemia and acute phase proteins in children with and without xerophthalmia. Am J Clin Nutr. 2000;72(1):146–53.
Hussain M, Shtein RM, Pistilli M, et al. The Dry Eye Assessment and Management (DREAM) extension study—a randomized clinical trial of withdrawal of supplementation with omega-3 fatty acid in patients with dry eye disease. Ocul Surf. 2020;18(1):47–55.
Epitropoulos AT, Donnenfeld ED, Shah ZA, et al. Effect of oral re-esterified omega-3 nutritional supplementation on dry eyes. Cornea. 2016;35(9):1185–91.
Oleñik A, Jiménez-Alfaro I, Alejandre-Alba N, et al. A randomized, double-masked study to evaluate the effect of omega-3 fatty acids supplementation in meibomian gland dysfunction. Clin Interv Aging. 2013;8:1133–8. https://www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence. Accessed on March 2022.
Howick J CI, Glasziou P, Greenhalgh T, et al. The 2011 Oxford CEBM levels of evidence. Oxford Centre for Evidence-Based Medicine; 2011. https://urldefense.com/v3/__, https://www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence. Accessed on March 2022.
Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
Walt JRM, Stern K. Evaluating the functional impact of dry eye: the ocular surface disease Index. Drug Inf J. 1997;31:1436.
Cho P, Leung L, Lam A, et al. Tear break-up time: clinical procedures and their effects. Ophthalmic Physiol Opt. 1998;18(4):319–24.
Cho P, Yap M. Schirmer test. I. A review. Optom Vis Sci. 1993;70(2):152–6.
Atkins D, Best D, Briss PA, et al. Grading quality of evidence and strength of recommendations. BMJ. 2004;328(7454):1490.
Shin MS, Kim JI, Lee MS, et al. Acupuncture for treating dry eye: a randomized placebo-controlled trial. Acta Ophthalmol. 2010;88(8):e328–33.
Sullivan DA, Rocha EM, Aragona P, et al. TFOS DEWS II sex, gender, and hormones report. Ocul Surf. 2017;15(3):284–333.
Truong S, Cole N, Stapleton F, et al. Sex hormones and the dry eye. Clin Exp Optom. 2014;97(4):324–36.
Artus M, van der Windt D, Jordan KP, et al. The clinical course of low back pain: a meta-analysis comparing outcomes in randomised clinical trials (RCTs) and observational studies. BMC Musculoskelet Disord. 2014;15:68.
Seitzman GD, Lietman TM. Dry eye research-still regressing? Ophthalmology. 2019;126(2):192–4.
Colloca L. The Placebo effect in pain therapies. Annu Rev Pharmacol Toxicol. 2019;59:191–211.
Leuchter AF, Hunter AM, Tartter M, et al. Role of pill-taking, expectation and therapeutic alliance in the placebo response in clinical trials for major depression. Br J Psychiatry. 2014;205(6):443–9.
Kemeny ME, Rosenwasser LJ, Panettieri RA, et al. Placebo response in asthma: a robust and objective phenomenon. J Allergy Clin Immunol. 2007;119(6):1375–81.
Avins AL, Pressman A, Ackerson L, et al. Placebo adherence and its association with morbidity and mortality in the studies of left ventricular dysfunction. J Gen Intern Med. 2010;25(12):1275–81.
Colloca L, Barsky AJ. Placebo and nocebo effects. N Engl J Med. 2020;382(6):554–61.
Chen X, Zou K, Abdullah N, et al. The placebo effect and its determinants in fibromyalgia: meta-analysis of randomised controlled trials. Clin Rheumatol. 2017;36(7):1623–30.
Eippert F, Bingel U, Schoell ED, et al. Activation of the opioidergic descending pain control system underlies placebo analgesia. Neuron. 2009;63(4):533–43.
Benedetti F, Amanzio M, Rosato R, et al. Nonopioid placebo analgesia is mediated by CB1 cannabinoid receptors. Nat Med. 2011;17(10):1228–30.
Benedetti F, Colloca L, Torre E, et al. Placebo-responsive Parkinson patients show decreased activity in single neurons of subthalamic nucleus. Nat Neurosci. 2004;7(6):587–8.
Kessner S, Sprenger C, Wrobel N, et al. Effect of oxytocin on placebo analgesia: a randomized study. JAMA. 2013;310(16):1733–5.
Colloca L, Pine DS, Ernst M, et al. Vasopressin boosts placebo analgesic effects in women: a randomized trial. Biol Psychiatry. 2016;79(10):794–802.
Petrovic P, Kalso E, Petersson KM, et al. Placebo and opioid analgesia—imaging a shared neuronal network. Science. 2002;295(5560):1737–40.
Kheirkhah A, Crnej A, Ren A, et al. Patients’ perceived treatment effectiveness in dry eye disease. Cornea. 2017;36(8):893–7.
Pollo A, Amanzio M, Arslanian A, et al. Response expectancies in placebo analgesia and their clinical relevance. Pain. 2001;93(1):77–84.
Asbell PA, Maguire MG, Peskin E, et al. Dry Eye Assessment and Management (DREAM©) Study: study design and baseline characteristics. Contemp Clin Trials. 2018;71:70–9.
Gupta A, Thompson D, Whitehouse A, et al. Adverse events associated with unblinded, but not with blinded, statin therapy in the Anglo-Scandinavian Cardiac Outcomes Trial-Lipid-Lowering Arm (ASCOT-LLA): a randomised double-blind placebo-controlled trial and its non-randomised non-blind extension phase. Lancet. 2017;389(10088):2473–81.
Rosenzweig P, Brohier S, Zipfel A. The placebo effect in healthy volunteers: influence of experimental conditions on the adverse events profile during phase I studies. Clin Pharmacol Ther. 1993;54(5):578–83.
Benedetti F, Amanzio M, Vighetti S, et al. The biochemical and neuroendocrine bases of the hyperalgesic nocebo effect. J Neurosci. 2006;26(46):12014–22.
Bramer WM, Rethlefsen ML, Kleijnen J, et al. Optimal database combinations for literature searches in systematic reviews: a prospective exploratory study. Syst Rev. 2017;6(1):245.
Lee MS, Shin BC, Choi TY, et al. Acupuncture for treating dry eye: a systematic review. Acta Ophthalmol. 2011;89(2):101–6.
Park J, White A, Stevinson C, et al. Validating a new non-penetrating sham acupuncture device: two randomised controlled trials. Acupunct Med. 2002;20(4):168–74.
Linde K, Niemann K, Meissner K. Are sham acupuncture interventions more effective than (other) placebos? A re-analysis of data from the Cochrane review on placebo effects. Forsch Komplementmed. 2010;17(5):259–64.
Funding
Open Access funding enabled and organized by Projekt DEAL. No specific funding was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Prinz, J., Maffulli, N., Fuest, M. et al. Placebo administration for dry eye disease: a level I evidence based systematic review and meta-analysis. Int J Clin Pharm 44, 1087–1101 (2022). https://doi.org/10.1007/s11096-022-01439-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-022-01439-y