Abstract
Purpose
Atypical meningiomas have histologic and clinical features that fall between those for benign and malignant meningiomas. The incidence of atypical meningiomas has not been well studied with respect to changes in the World Health Organization (WHO) classification scheme over time.
Methods
The National Cancer Institute’s Surveillance, Epidemiology, and End Results (SEER) database was queried to obtain data from 2004 to 2018 for patients with all meningiomas, including atypical. Age-adjusted incidence rates were generated and annual percent change (APC) in the incidence rates was calculated with joinpoint regression. Survival was analyzed using the Kaplan–Meier method and Cox proportional hazards models.
Results
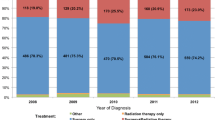
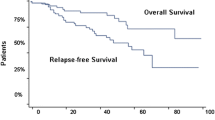
A total of 4476 patients diagnosed with meningioma were identified from the SEER 18 registries. The incidence of atypical meningioma increased at an APC of 5.6% [95% confidence interval [CI], 3.4–7.8]; significantly faster than all meningiomas, which rose at an APC of 2.5% (95%CI 1.8–3.1;p = 0.008). For atypical meningiomas, the 1, 3, 5, and 10-year survival rates were 91.9%, 81.3%, 68.8%, and 34.3%, respectively. Male sex, older age (≥ 60 years), and large tumor size (> 5 cm) were independent risk factors for an unfavorable prognosis.
Conclusions
The incidence of atypical meningioma was observed to be increasing relative to all meningiomas. It is important to diligently monitor atypical meningioma incidence and mortality rates over time to see whether observed uptrends persist. Continued effort toward improving outcomes in patients with atypical meningiomas is warranted, especially in light of an apparent rise in incidence.



Similar content being viewed by others
Abbreviations
- AAPC:
-
Average annual percent change
- APC:
-
Annual percent change
- API:
-
Asian or Pacific Islander
- CI:
-
Confidence interval
- Cm:
-
Centimeters
- HR:
-
Hazard ratio
- ICD-O-3:
-
International classification of diseases for oncology, 3rd edition
- SEER:
-
Surveillance epidemiology, and end results
- US:
-
United States
- WHO:
-
World Health Organization
References
Ostrom QT, Patil N, Cioffi G, Waite K, Kruchko C, Barnholtz-Sloan JS (2020) Corrigendum to: CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2013–2017. Neuro Oncol. https://doi.org/10.1093/neuonc/noaa269
Barthelemy EJ, Sarkiss CA, Lee J, Shrivastava RK (2016) The historical origin of the term “meningioma” and the rise of nationalistic neurosurgery. J Neurosurg 125:1283–1290. https://doi.org/10.3171/2015.10.JNS15877
Zamanipoor Najafabadi AH, van der Meer PB, Boele FW, Taphoorn MJB, Klein M, Peerdeman SM, van Furth WR, Dirven L, Dutch Meningioma C (2020) Long-term disease burden and survivorship issues after surgery and radiotherapy of intracranial meningioma patients. Neurosurgery 88:155–164. https://doi.org/10.1093/neuros/nyaa351
Zamanipoor Najafabadi AH, Peeters MCM, Dirven L, Lobatto DJ, Groen JL, Broekman MLD, Peerdeman SM, Peul WC, Taphoorn MJB, van Furth WR (2017) Impaired health-related quality of life in meningioma patients-a systematic review. Neuro Oncol 19:897–907. https://doi.org/10.1093/neuonc/now250
Kaur G, Sayegh ET, Larson A, Bloch O, Madden M, Sun MZ, Barani IJ, James CD, Parsa AT (2014) Adjuvant radiotherapy for atypical and malignant meningiomas: a systematic review. Neuro Oncol 16:628–636. https://doi.org/10.1093/neuonc/nou025
Backer-Grondahl T, Moen BH, Torp SH (2012) The histopathological spectrum of human meningiomas. Int J Clin Exp Pathol 5:231–242
Kleihues P, Louis DN, Scheithauer BW, Rorke LB, Reifenberger G, Burger PC, Cavenee WK (2002) The WHO classification of tumors of the nervous system. J Neuropathol Exp Neurol 61(3):215–225. https://doi.org/10.1093/jnen/61.3.215
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, Jouvet A, Scheithauer BW, Kleihues P (2007) The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 114:97–109. https://doi.org/10.1007/s00401-007-0243-4
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, Ohgaki H, Wiestler OD, Kleihues P, Ellison DW (2016) The 2016 World Health Organization classification of tumors of the central nervous system: a summary. Acta Neuropathol 131:803–820. https://doi.org/10.1007/s00401-016-1545-1
Pasquier D, Bijmolt S, Veninga T, Rezvoy N, Villa S, Krengli M, Weber DC, Baumert BG, Canyilmaz E, Yalman D, Szutowicz E, Tzuk-Shina T, Mirimanoff RO, Rare Cancer N (2008) Atypical and malignant meningioma: outcome and prognostic factors in 119 irradiated patients. A multicenter, retrospective study of the Rare Cancer Network. Int J Radiat Oncol Biol Phys 71:1388–1393. https://doi.org/10.1016/j.ijrobp.2007.12.020
Claus EB, Bondy ML, Schildkraut JM, Wiemels JL, Wrensch M, Black PM (2005) Epidemiology of intracranial meningioma. Neurosurgery 57(6):1088–1095. https://doi.org/10.1227/01.neu.0000188281.91351.b9
Pearson BE, Markert JM, Fisher WS, Guthrie BL, Fiveash JB, Palmer CA, Riley K (2008) Hitting a moving target: evolution of a treatment paradigm for atypical meningiomas amid changing diagnostic criteria. Neurosurg Focus 24:E3. https://doi.org/10.3171/FOC/2008/24/5/E3
Combs SE, Schulz-Ertner D, Debus J, von Deimling A, Hartmann C (2011) Improved correlation of the neuropathologic classification according to adapted world health organization classification and outcome after radiotherapy in patients with atypical and anaplastic meningiomas. Int J Radiat Oncol Biol Phys 81:1415–1421. https://doi.org/10.1016/j.ijrobp.2010.07.039
Rogers L, Gilbert M, Vogelbaum MA (2010) Intracranial meningiomas of atypical (WHO grade II) histology. J Neurooncol 99:393–405. https://doi.org/10.1007/s11060-010-0343-1
Cain SA, Smoll NR, Van Heerden J, Tsui A, Drummond KJ (2015) Atypical and malignant meningiomas: considerations for treatment and efficacy of radiotherapy. J Clin Neurosci 22:1742–1748. https://doi.org/10.1016/j.jocn.2015.03.054
Klinger DR, Flores BC, Lewis JJ, Hatanpaa K, Choe K, Mickey B, Barnett S (2015) Atypical meningiomas: recurrence, reoperation, and radiotherapy. World Neurosurg 84:839–845. https://doi.org/10.1016/j.wneu.2015.04.033
Adogwa O, Desai SA, Vuong VD, Lilly DT, Ouyang B, Davison M, Khalid S, Bagley CA, Cheng J (2018) Extended length of stay in elderly patients after lumbar decompression and fusion surgery may not be attributable to baseline illness severity or postoperative complications. World Neurosurg 116:e996–e1001. https://doi.org/10.1016/j.wneu.2018.05.148
Simpson D (1957) The recurrence of intracranial meningiomas after surgical treatment. J Neurol Neurosurg Psychiatry 20:22–39. https://doi.org/10.1136/jnnp.20.1.22
Kim HJ, Fay MP, Feuer EJ, Midthune DN (2000) Permutation tests for joinpoint regression with applications to cancer rates. Stat Med 19:335–351. https://doi.org/10.1002/(sici)1097-0258(20000215)19:3%3c335::aid-sim336%3e3.0.co;2-z
Sutradhar BC, Bartlett RF (1993) A small and large sample comparison of Wald’s likelihood ratio and Rao’s tests for testing linear regression with autocorrelated errors. sankhyā Indian J Stat Ser B 55:186–198
Kim HJ, Fay MP, Yu B, Barrett MJ, Feuer EJ (2004) Comparability of segmented line regression models. Biometrics 60:1005–1014. https://doi.org/10.1111/j.0006-341X.2004.00256.x
Kshettry VR, Ostrom QT, Kruchko C, Al-Mefty O, Barnett GH, Barnholtz-Sloan JS (2015) Descriptive epidemiology of World Health Organization grades II and III intracranial meningiomas in the United States. Neuro Oncol 17:1166–1173. https://doi.org/10.1093/neuonc/nov069
Vadivelu S, Sharer L, Schulder M (2010) Regression of multiple intracranial meningiomas after cessation of long-term progesterone agonist therapy. J Neurosurg 112:920–924. https://doi.org/10.3171/2009.8.JNS09201
Yang SY, Park CK, Park SH, Kim DG, Chung YS, Jung HW (2008) Atypical and anaplastic meningiomas: prognostic implications of clinicopathological features. J Neurol Neurosurg Psychiatry 79:574–580. https://doi.org/10.1136/jnnp.2007.121582
Curry WT Jr, Barker FG 2nd (2009) Racial, ethnic and socioeconomic disparities in the treatment of brain tumors. J Neurooncol 93:25–39. https://doi.org/10.1007/s11060-009-9840-5
Mahmood A, Caccamo DV, Tomecek FJ, Malik GM (1993) Atypical and malignant meningiomas: a clinicopathological review. Neurosurgery 33:955–963. https://doi.org/10.1227/00006123-199312000-00001
Younis GA, Sawaya R, DeMonte F, Hess KR, Albrecht S, Bruner JM (1995) Aggressive meningeal tumors: review of a series. J Neurosurg 82:17–27. https://doi.org/10.3171/jns.1995.82.1.0017
Reddy AK, Ryoo JS, Denyer S, McGuire LS, Mehta AI (2019) Determining the role of adjuvant radiotherapy in the management of meningioma: a surveillance, epidemiology, and end results analysis. Neurosurg Focus 46:E3. https://doi.org/10.3171/2019.3.FOCUS1971
Zeng Q, Shi F, Guo Z (2019) Effectiveness of postoperative radiotherapy on atypical meningioma patients: a population-based study. Front Oncol 9:34. https://doi.org/10.3389/fonc.2019.00034
Kaley T, Barani I, Chamberlain M, McDermott M, Panageas K, Raizer J, Rogers L, Schiff D, Vogelbaum M, Weber D, Wen P (2014) Historical benchmarks for medical therapy trials in surgery- and radiation-refractory meningioma: a RANO review. Neuro Oncol 16:829–840. https://doi.org/10.1093/neuonc/not330
Acknowledgements
The authors thank Paul H. Dressel BFA for preparation of the tables and figures and Carrie Owens MSILS and Debra J. Zimmer for editorial assistance.
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
RJP, MJR: contributed to the study conception and design. CCK, MJR, KA: Material preparation, data collection and analysis were performed. CCK, MJR: The first draft of the manuscript was written and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests related to this study.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Ethical approval
The University at Buffalo Institutional Review Board determined that this study was not research involving human subjects and that their review and approval was not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Recker, M.J., Kuo, C.C., Prasad, D. et al. Incidence trends and survival analysis of atypical meningiomas: a population-based study from 2004 to 2018. J Neurooncol 160, 13–22 (2022). https://doi.org/10.1007/s11060-022-04085-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-022-04085-6