Abstract
Purpose
This report presents the first investigation of the radiomics value in predicting the meningioma volumetric response to gamma knife radiosurgery (GKRS).
Methods
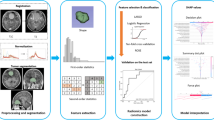
The retrospective study included 93 meningioma patients imaged by three Tesla MRI. Tumor morphology was quantified by calculating 337 shape, first- and second-order radiomic features from MRI obtained before GKRS. Analysis was performed on original 3D MR images and after their laplacian of gaussian (LoG), logarithm and exponential filtering. The prediction performance was evaluated by Pearson correlation, linear regression and ROC analysis, with meningioma volume change per month as the outcome.
Results
Sixty calculated features significantly correlated with the outcome. The feature selection based on LASSO and multivariate regression started from all available 337 radiomic and 12 non-radiomic features. It selected LoG-sigma-1-0-mm-3D_firstorder_InterquartileRange and logarithm_ngtdm_Busyness as the predictively most robust and non-redundant features. The radiomic score based on these two features produced an AUC = 0.81. Adding the non-radiomic karnofsky performance status (KPS) to the score has increased the AUC to 0.88. Low values of the radiomic score defined a homogeneous subgroup of 50 patients with consistent absence (0%) of tumor progression.
Conclusion
This is the first report of a strong association between MRI radiomic features and volumetric meningioma response to radiosurgery. The clinical importance of the early and reliable prediction of meningioma responsiveness to radiosurgery is based on its potential to aid individualized therapy decision making.


Similar content being viewed by others
Data availability
The datasets generated during and analyzed during the current study are available from the corresponding author on reasonable request.
References
Rogers L, Barani I, Chamberlain M, Kaley TJ, McDermott M, Raizer J, Schiff D, Weber DC, Wen PY, Vogelbaum MA (2015) Meningiomas: knowledge base, treatment outcomes, and uncertainties: a RANO review. J Neurosurg 122:4–23. https://doi.org/10.3171/2014.7.JNS131644
Cohen-Inbar O, Lee CC, Sheehan JP (2016) The contemporary role of stereotactic radiosurgery in the treatment of meningiomas. Neurosurg Clin N Am 27:215–228. https://doi.org/10.1016/j.nec.2015.11.006
Ius T, Tel A, Minniti G, Somma T, Solari D, Longhi M, De Bonis P, Scerrati A, Caccese M, Barresi V, Fiorentino A, Gorgoglione L, Lombardi G, Robiony M (2021) Advances in multidisciplinary management of skull base meningiomas. Cancers. https://doi.org/10.3390/cancers13112664
Sheehan J, Pikis S, Islim AI, Chen CJ, Bunevicius A, Peker S, Samanci Y, Nabeel AM, Reda WA, Tawadros SR, El-Shehaby AMN, Abdelkarim K, Emad RM, Delabar V, Mathieu D, Lee CC, Yang HC, Liscak R, Hanuska J, Alvarez RM, Patel D, Kondziolka D, Moreno NM, Tripathi M, Speckter H, Albert C, Bowden GN, Benveniste RJ, Lunsford LD, Jenkinson MD (2022) An international multicenter matched cohort analysis of incidental meningioma progression during active surveillance or after stereotactic radiosurgery: the IMPASSE study. Neuro-Oncology 24:116–124. https://doi.org/10.1093/neuonc/noab132
Fatima N, Meola A, Pollom E, Chaudhary N, Soltys S, Chang SD (2019) Stereotactic radiosurgery in large intracranial meningiomas: a systematic review. World Neurosurg 129:269–275. https://doi.org/10.1016/j.wneu.2019.06.064
Helis CA, Hughes RT, Cramer CK, Tatter SB, Laxton AW, Bourland JD, Munley MT, Chan MD (2020) Stereotactic radiosurgery for atypical and anaplastic meningiomas. World Neurosurg 144:e53–e61. https://doi.org/10.1016/j.wneu.2020.07.211
DiBiase SJ, Kwok Y, Yovino S, Arena C, Naqvi S, Temple R, Regine WF, Amin P, Guo C, Chin LS (2004) Factors predicting local tumor control after Gamma Knife stereotactic radiosurgery for benign intracranial meningiomas. Int J Radiat Oncol Biol Phys 60:1515–1519. https://doi.org/10.1016/j.ijrobp.2004.05.073
Starke RM, Nguyen JH, Rainey J, Williams BJ, Sherman JH, Savage J, Yen CP, Sheehan JP (2011) Gamma Knife surgery of meningiomas located in the posterior fossa: factors predictive of outcome and remission. J Neurosurg 114:1399–1409. https://doi.org/10.3171/2010.11.JNS101193
Santacroce A, Walier M, Regis J, Liscak R, Motti E, Lindquist C, Kemeny A, Kitz K, Lippitz B, Martinez Alvarez R, Pedersen PH, Yomo S, Lupidi F, Dominikus K, Blackburn P, Mindermann T, Bundschuh O, van Eck AT, Fimmers R, Horstmann GA (2012) Long-term tumor control of benign intracranial meningiomas after radiosurgery in a series of 4565 patients. Neurosurgery 70(1):32–39. https://doi.org/10.1227/NEU.0b013e31822d408a
Sheehan JP, Starke RM, Kano H, Kaufmann AM, Mathieu D, Zeiler FA, West M, Chao ST, Varma G, Chiang VL, Yu JB, McBride HL, Nakaji P, Youssef E, Honea N, Rush S, Kondziolka D, Lee JY, Bailey RL, Kunwar S, Petti P, Lunsford LD (2014) Gamma Knife radiosurgery for sellar and parasellar meningiomas: a multicenter study. J Neurosurg 120:1268–1277. https://doi.org/10.3171/2014.2.JNS13139
Mansouri A, Larjani S, Klironomos G, Laperriere N, Cusimano M, Gentili F, Schwartz M, Zadeh G (2015) Predictors of response to Gamma Knife radiosurgery for intracranial meningiomas. J Neurosurg 123:1294–1300. https://doi.org/10.3171/2014.12.JNS141687
Cesme DH, Alkan A, Sari L, Yabul F, Temur HO, Aykan ME, Seyithanoglu MH, Hatiboglu MA (2021) Importance of pre-treatment fractional anisotropy value in predicting volumetric response in patients with meningioma treated with Gamma Knife radiosurgery. Curr Med Imaging 17:871–877. https://doi.org/10.2174/2213335608999210128182047
O’Connor KP, Algan O, Vesely SK, Palejwala AH, Briggs RG, Conner AK, Cornwell BO, Andrews B, Sughrue ME, Glenn CA (2019) Factors associated with treatment failure and radiosurgery-related edema in WHO grade 1 and 2 meningioma patients receiving Gamma Knife radiosurgery. World Neurosurg 130:e558–e565. https://doi.org/10.1016/j.wneu.2019.06.152
Tropine A, Dellani PD, Glaser M, Bohl J, Ploner T, Vucurevic G, Perneczky A, Stoeter P (2007) Differentiation of fibroblastic meningiomas from other benign subtypes using diffusion tensor imaging. J Magn Reson Imaging 25:703–708. https://doi.org/10.1002/jmri.20887
Speckter H, Bido J, Hernandez G, Mejia DR, Suazo L, Valenzuela S, Perez-Then E, Stoeter P (2016) Prognostic value of diffusion tensor imaging parameters for Gamma Knife radiosurgery in meningiomas. J Neurosurg 125:83–88. https://doi.org/10.3171/2016.7.GKS161455
Berberat J, Roelcke U, Remonda L, Schwyzer L (2021) Long-term apparent diffusion coefficient value changes in patients undergoing radiosurgical treatment of meningiomas. Acta Neurochir 163:89–95. https://doi.org/10.1007/s00701-020-04567-4
Speckter H, Bido J, Hernandez G, Rivera D, Suazo L, Valenzuela S, Miches I, Oviedo J, Gonzalez C, Stoeter P (2018) Pretreatment texture analysis of routine MR images and shape analysis of the diffusion tensor for prediction of volumetric response after radiosurgery for meningioma. J Neurosurg 129:31–37. https://doi.org/10.3171/2018.7.GKS181327
Chang Y, Lafata K, Sun W, Wang C, Chang Z, Kirkpatrick JP, Yin FF (2019) An investigation of machine learning methods in delta-radiomics feature analysis. PLoS ONE 14:e0226348. https://doi.org/10.1371/journal.pone.0226348
Hu J, Zhao Y, Li M, Liu J, Wang F, Weng Q, Wang X, Cao D (2020) Machine learning-based radiomics analysis in predicting the meningioma grade using multiparametric MRI. Eur J Radiol 131:109251. https://doi.org/10.1016/j.ejrad.2020.109251
Park YW, Oh J, You SC, Han K, Ahn SS, Choi YS, Chang JH, Kim SH, Lee SK (2019) Radiomics and machine learning may accurately predict the grade and histological subtype in meningiomas using conventional and diffusion tensor imaging. Eur Radiol 29:4068–4076. https://doi.org/10.1007/s00330-018-5830-3
Kandemirli SG, Chopra S, Priya S, Ward C, Locke T, Soni N, Srivastava S, Jones K, Bathla G (2020) Presurgical detection of brain invasion status in meningiomas based on first-order histogram based texture analysis of contrast enhanced imaging. Clin Neurol Neurosurg 198:106205. https://doi.org/10.1016/j.clineuro.2020.106205
Hamerla G, Meyer HJ, Schob S, Ginat DT, Altman A, Lim T, Gihr GA, Horvath-Rizea D, Hoffmann KT, Surov A (2019) Comparison of machine learning classifiers for differentiation of grade 1 from higher gradings in meningioma: a multicenter radiomics study. Magn Reson Imaging 63:244–249. https://doi.org/10.1016/j.mri.2019.08.011
Morin O, Chen WC, Nassiri F, Susko M, Magill ST, Vasudevan HN, Wu A, Vallieres M, Gennatas ED, Valdes G, Pekmezci M, Alcaide-Leon P, Choudhury A, Interian Y, Mortezavi S, Turgutlu K, Bush NAO, Solberg TD, Braunstein SE, Sneed PK, Perry A, Zadeh G, McDermott MW, Villanueva-Meyer JE, Raleigh DR (2019) Integrated models incorporating radiologic and radiomic features predict meningioma grade, local failure, and overall survival. Neurooncol Adv. https://doi.org/10.1093/noajnl/vdz011
Kalasauskas D, Kronfeld A, Renovanz M, Kurz E, Leukel P, Krenzlin H, Brockmann MA, Sommer CJ, Ringel F, Keric N (2020) Identification of high-risk atypical meningiomas according to semantic and radiomic features. Cancers. https://doi.org/10.3390/cancers12102942
Patibandla MR, Lee CC, Tata A, Addagada GC, Sheehan JP (2018) Stereotactic radiosurgery for WHO grade I posterior fossa meningiomas: long-term outcomes with volumetric evaluation. J Neurosurg 129:1249–1259. https://doi.org/10.3171/2017.6.JNS17993
McMahon SJ (2018) The linear quadratic model: usage, interpretation and challenges. Phys Med Biol 64:01TR01. https://doi.org/10.1088/1361-6560/aaf26a
Speckter H, Santana J, Miches I, Hernandez G, Bido J, Rivera D, Suazo L, Valenzuela S, Garcia J, Stoeter P (2019) Assessment of the alpha/beta ratio of the optic pathway to adjust hypofractionated stereotactic radiosurgery regimens for perioptic lesions. J Radiat Oncol 8:279–289. https://doi.org/10.1007/s13566-019-00398-8
Vernimmen FJ, Slabbert JP (2010) Assessment of the alpha/beta ratios for arteriovenous malformations, meningiomas, acoustic neuromas, and the optic chiasma. Int J Radiat Biol 86:486–498. https://doi.org/10.3109/09553001003667982
Fedorov A, Beichel R, Kalpathy-Cramer J, Finet J, Fillion-Robin JC, Pujol S, Bauer C, Jennings D, Fennessy F, Sonka M, Buatti J, Aylward S, Miller JV, Pieper S, Kikinis R (2012) 3D Slicer as an image computing platform for the quantitative imaging network. Magn Reson Imaging 30:1323–1341. https://doi.org/10.1016/j.mri.2012.05.001
van Griethuysen JJM, Fedorov A, Parmar C, Hosny A, Aucoin N, Narayan V, Beets-Tan RGH, Fillion-Robin JC, Pieper S, Aerts H (2017) Computational radiomics system to decode the radiographic phenotype. Cancer Res 77:e104–e107. https://doi.org/10.1158/0008-5472.CAN-17-0339
Huang RY, Bi WL, Weller M, Kaley T, Blakeley J, Dunn I, Galanis E, Preusser M, McDermott M, Rogers L, Raizer J, Schiff D, Soffietti R, Tonn JC, Vogelbaum M, Weber D, Reardon DA, Wen PY (2019) Proposed response assessment and endpoints for meningioma clinical trials: report from the response assessment in neuro-oncology working group. Neuro-Oncology 21:26–36. https://doi.org/10.1093/neuonc/noy137
Kolakshyapati M, Ikawa F, Abiko M, Mitsuhara T, Kinoshita Y, Takeda M, Kurisu K (2018) Multivariate risk factor analysis and literature review of postoperative deterioration in karnofsky performance scale score in elderly patients with skull base meningioma. Neurosurg Focus 44:E14. https://doi.org/10.3171/2018.1.FOCUS17730
Paddick I (2000) A simple scoring ratio to index the conformity of radiosurgical treatment plans: technical note. J Neurosurg 93(Suppl 3):219–222. https://doi.org/10.3171/jns.2000.93.supplement
O’Connor JPB (2017) Cancer heterogeneity and imaging. Semin Cell Dev Biol 64:48–57. https://doi.org/10.1016/j.semcdb.2016.10.001
Yang HC, Wu CC, Lee CC, Huang HE, Lee WK, Chung WY, Wu HM, Guo WY, Wu YT, Lu CF (2021) Prediction of pseudoprogression and long-term outcome of vestibular schwannoma after Gamma Knife radiosurgery based on preradiosurgical MR radiomics. Radiother Oncol 155:123–130. https://doi.org/10.1016/j.radonc.2020.10.041
Wald LL (2019) Ultimate MRI. J Magn Reson 306:139–144. https://doi.org/10.1016/j.jmr.2019.07.016
You J, Yin J (2021) Performances of whole tumor texture analysis based on MRI: predicting preoperative T stage of rectal carcinomas. Front Oncol 11:678441. https://doi.org/10.3389/fonc.2021.678441
Xiao DD, Yan PF, Wang YX, Osman MS, Zhao HY (2018) Glioblastoma and primary central nervous system lymphoma: preoperative differentiation by using MRI-based 3D texture analysis. Clin Neurol Neurosurg 173:84–90. https://doi.org/10.1016/j.clineuro.2018.08.004
Chen S, Harmon S, Perk T, Li X, Chen M, Li Y, Jeraj R (2019) Using neighborhood gray tone difference matrix texture features on dual time point PET/CT images to differentiate malignant from benign FDG-avid solitary pulmonary nodules. Cancer Imaging 19:56. https://doi.org/10.1186/s40644-019-0243-3
Perez-Morales J, Tunali I, Stringfield O, Eschrich SA, Balagurunathan Y, Gillies RJ, Schabath MB (2020) Peritumoral and intratumoral radiomic features predict survival outcomes among patients diagnosed in lung cancer screening. Sci Rep 10:10528. https://doi.org/10.1038/s41598-020-67378-8
Baidya Kayal E, Kandasamy D, Khare K, Bakhshi S, Sharma R, Mehndiratta A (2021) Texture analysis for chemotherapy response evaluation in osteosarcoma using MR imaging. NMR Biomed 34:e4426. https://doi.org/10.1002/nbm.4426
Lee CC, Trifiletti DM, Sahgal A, DeSalles A, Fariselli L, Hayashi M, Levivier M, Ma L, Alvarez RM, Paddick I, Regis J, Ryu S, Slotman B, Sheehan J (2018) Stereotactic radiosurgery for benign (World Health Organization Grade I) cavernous sinus meningiomas-international stereotactic radiosurgery society (ISRS) practice guideline: a systematic review. Neurosurgery 83:1128–1142. https://doi.org/10.1093/neuros/nyy009
Funding
This work was supported by the University Instituto Tecnologico de Santo Domingo (INTEC), Dominican Republic, Grant Number CBA-221024-2020-P-1.
Author information
Authors and Affiliations
Contributions
Conception and design: HS and MR. Data collection: HS, JJ, WH, AM, JB, GH, DR, LS, SV, PS. Data analysis and interpretation: All authors. Manuscript writing: HS, MR, PS. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Kire Trivodaliev is employed by QMENTA Inc., Boston, MA, USA. All other authors have nothing to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Speckter, H., Radulovic, M., Trivodaliev, K. et al. MRI radiomics in the prediction of the volumetric response in meningiomas after gamma knife radiosurgery. J Neurooncol 159, 281–291 (2022). https://doi.org/10.1007/s11060-022-04063-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-022-04063-y