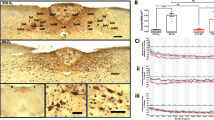
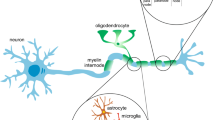
The aim of the present work was to identify structural, spatial, and quantitative changes in elements of the paranigral nucleus (PNN) of the midbrain and anterior cingulate field (ACF) of the telencephalon in different conditions of circulatory hypoxia. The anterior medial part of the PNN and layers V–VI of the ACF were studied in healthy rats seven days (n = 4) after occlusion of both common carotid arteries and in intact (control 1, n = 4) and sham-operated (control 2, n = 4) rats. Histological sections stained with cresyl violet by the Nissl method and processed for detection of glial fibrillary acidic protein and Iba1 protein were used to identify the ratio of essentially unchanged, hypochromic, pyknomorphic, and ghost neurons, along with the numbers of astrocytes, oligodendrocytes, microgliocytes, and endotheliocytes. The areas of neurons and gliocyte bodies were measured, along with the distances from these cells to capillary walls, and gliocyte:neuron indexes were calculated. The results showed that after exposure to different conditions of circulatory hypoxia, the cellular elements of the brain showed a spectrum of characteristic pathological changes. Neurons showed signs of nuclear pyknosis, lysis, and conversion to “ghost” cells. Cells in the nuclear zone of hypoxia tended to undergo death or pyknosis. Neurons located outside the hypoxic area and exposed only to the humoral actions of the responses of the glutamate-calcium cascade often showed acute swelling. The reactions of microgliocytes, with minor increases in numbers and structural signs of activation, represented early diffuse signs of focal hypoxia in the forebrain. Endotheliocyte proliferation seen at seven days of ischemia was not associated with the chain of cascade reactions, but occurred only in the focus of hypoxia. The concentrations of viable neurons and astrocytes close to blood capillaries and the increase in the number of satellite types of glial cells represent an adaptive mechanism and a constitute a condition for cell survival in the conditions of various types of cerebral ischemia.
Similar content being viewed by others
References
D. V. Bogomolov, Forensic Medical Diagnosis of Narcotic Intoxication on the Basis of Morphological Data: Auth. Abstr. Dissert. Doct. Med. Sci., Moscow (2001).
Yu. G. Vasil’ev and D. S. Berestov, Homeostasis and Brain Plasticity [in Russian], State Agricultural Academy, Izhevsk (2011).
E. I. Gusev and V. I. Skvortsova, Cerebral Ischemia [in Russian], Meditsina, Moscow (2001).
A. V. Droblenkov, “Morphological signs of poisoning with ethanol, alcohol abstinence, and chronic alcohol intoxication in the mesocorticolimbic dopaminergic system,” Sud.-Med. Ekspert., 54, No. 5, 11–17 (2011).
A. V. Droblenkov and N. R. Karelina, “Structural characteristics of neurons and macrogliocytes in interacting compartments of the mesoaccumbocingulate dopaminergic system in rats,” Morfologiya, 136, No. 5, 11–17 (2009).
A. V. Droblenkov, N. R. Karelina, and P. D. Shabanov, “Changes in neurons and gliocytes in the mesoaccumbocingulate system in perinatal exposure to morphine in rats,” Morfologiya, 136, No. 6, 35–37 (2009).
Yu. M. Zhabotinskii, Normal and Pathological Neuron Morphology [in Russian], Nauka, Moscow (1965).
B. S. Litvintsev, M. M. Odinak, O. N. Gaikova, et al., “Clinical and morphological characteristics of the neurological signs of drug addiction,” Profilakt. Klin. Med., 39, No. 2, 99–104 (2011).
V. P. Poshivalov, An Ethological Atlas for Pharmacological Studies in Rodents [in Russian], depos. VINITI, No. 3164–3178 (1978).
P. D. Shabanov, I. V. Zarubina, and V. S. Soultanov, “The mechanism of action of polyprenols in cerebral ischemia,” Med. Akad. Zh., 11, No. 2, 24–31 (2011).
C. Charriaut-Marlangue, I. Margaill, and A. J. Represa, “Apoptosis and necrosis after reversible focal ischemia: an in situ DNA fragmentation analysis,” J. Cereb. Blood Flow Metab., 16, 186–194 (1996).
M. D. Ginsberg and R. Busto, “Rodent models of cerebral ischemia,” Stroke, 20, 1627–1642 (1989).
H. Kajihara, R. Tsutsumi, A. Kinoshita, et al., “Activated astrocytes with glycogen accumulation in ischemic penumbra during the early stage of brain infarction: immunohistochemical and electron microscopic studies,” Brain Res., 909, No. 3, 92–101 (2001).
V. V. Marysheva, V. V. Mikheev, and P. D. Shabanov, “Effect of amtizol on resistance of SHR mice to acute hypoxia with hypercapnia under conditions as isolated functioning of one cerebral hemisphere,” Bull. Exp. Biol. Med., 154, No. 4, 453–456 (2013).
G. S. Okoye, E. M. Powel, and H. M. Gellar, “Migration of A7 immortalized astrocyte cells grafted into the adult rat striatum,” J. Comp. Phys., 262, 524–534 (1995).
G. Racchetti, R. D’Alessandro, and J. Meldolesi, “Astrocyte stellation, a process dependent on Rac1 is sustained by the regulated exocytosis of enlargeosomes,” Glia, 60, No. 3, 465–475 (2012).
O. U. Scremin, “Cerebral blood vessels,” in: The Rat Nervous System, Elsevier Academic Press, Amsterdam (2004), 3rd ed., pp. 1176–1780.
R. R. Voskuhl, R. S. Peterson, B. Song, et al., “Reactive astrocytes form scar-like perivascular barriers to leukocytes during adaptive immune inflammation of the CNS,” J. Neurosci., 29, 11511–11522 (2009).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Morfologiya, Vol. 143, No. 3, pp. 14–21, May–June, 2013.
Rights and permissions
About this article
Cite this article
Droblenkov, A.V., Naumov, N.V., Monid, M.V. et al. Reactive Changes in the Cellular Elements of the Rat Brain in Different Conditions of Circulatory Hypoxia. Neurosci Behav Physi 44, 606–613 (2014). https://doi.org/10.1007/s11055-014-9958-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-014-9958-6