Abstract
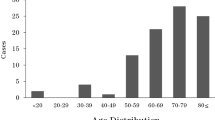
In a multicenter, prospective study of filamentous fungal keratitis in Greece, predisposing factors, etiology, treatment practices, and outcome, were determined. Corneal scrapings were collected from patients with clinical suspicion of fungal keratitis, and demographic and clinical data were recorded. Fungal identification was based on morphology, molecular methods, and matrix assisted laser desorption ionization time-of-flight mass-spectrometry. A total of 35 cases were identified in a 16-year study period. Female to male ratio was 1:1.7 and median age 48 years. Corneal injury by plant material, and soft contact lens use were the main risk factors (42.8% and 31.4%, respectively). Trauma was the leading risk factor for men (68.1%), contact lens use (61.5%) for women. Fusarium species were isolated more frequently (n = 21, 61.8%). F. solani was mostly associated with trauma, F. verticillioides and F. proliferatum with soft contact lens use. Other fungi were: Purpureocillium lilacinum (14.7%), Alternaria (11.8%), Aspergillus (8.8%), and Phoma foliaceiphila, Beauveria bassiana and Curvularia spicifera, one case each. Amphotericin B and voriconazole MIC50s against Fusarium were 2 mg/L and 4 mg/L respectively. Antifungal therapy consisted mainly of voriconazole locally or both locally and systemically, alone or in combination with liposomal AmB. Cure/improvement rate with antifungal therapy alone was 52%, keratoplasty was required in 40% of cases, and enucleation in 8%. In conclusion, filamentous fungal keratitis in Greece is rare, but with considerable morbidity. A large proportion of cases resulted in keratoplasty despite appropriate antifungal treatment.
Similar content being viewed by others
References
Kibret T, Bitew A. Fungal keratitis in patients with corneal ulcer attending Minilik II Memorial Hospital, Addis Ababa. Ethiop BMC Ophthalmol. 2016. https://doi.org/10.1186/s12886-016-0330-1.
Knutsson KA, Iovieno A, Matuska S, Fontana L, Rama P. Topical corticosteroids and fungal keratitis: a review of the literature and case series. J Clin Med. 2021. https://doi.org/10.3390/jcm10061178.
Alfonso EC, Forster RK, Garg P. Fungal infections. In: Foster CS, Azar DT, Dohlman CH, editors. Smolin and Thoft’s the cornea scientific foundations & clinical practice, vol. 4. Baltimore: Lippincott Williams & Wilkins; 2005. p. 405–16.
Hoffman JJ, Burton MJ, Leck A. Mycotic keratitis—a global threat from the filamentous fungi. J Fungi (Basel). 2021. https://doi.org/10.3390/jof7040273.
Manikandan P, Abdel-Hadi A, Randhir Babu Singh Y, Revathi R, Anita R, Banawas S, et al. Fungal keratitis epidemiology, rapid detection, and antifungal susceptibilities of fusarium and aspergillus isolates from corneal scrapings. Biomed Res Int. 2019. https://doi.org/10.1155/2019/6395840.
Thomas PA, Leck AK, Myatt M. Characteristic clinical features as an aid to the diagnosis of suppurative keratitis caused by filamentous fungi. Br J Ophthalmol. 2005. https://doi.org/10.1136/bjo.2005.076315.
Brown L, Leck AK, Gichangi M, Burton MJ, Denning DW. The global incidence and diagnosis of fungal keratitis. Lancet Infect Dis. 2021. https://doi.org/10.1016/S1473-3099(20)30448-5.
Tortorano AM, Prigitano A, Esposto MC, Arsic Arsenijevic V, Kolarovic J, Ivanovic D, et al. ECMM working group. European Confederation of medical mycology (ECMM) epidemiological survey on invasive infections due to fusarium species in Europe. Eur J Clin Microbiol Infect Dis. 2014. https://doi.org/10.1007/s10096-014-2111-1.
Al-Hatmi AMS, Ahmed SA, van Diepeningen AD, Drogari-Apiranthitou M, Verweij PE, Meis JF, de Hoog GS. Fusarium metavorans sp. nov.: the frequent opportunist “FSSC6.” Med Mycol. 2018. https://doi.org/10.1093/mmy/myx107.
Cassagne C, Normand AC, L’Ollivier C, Ranque S, Piarroux R. Performance of MALDI-TOF MS platforms for fungal identification. Mycoses. 2016. https://doi.org/10.1111/myc.12506.
Peng Y, Zhang Q, Xu C, Shi W. MALDI-TOF MS for the rapid identification and drug susceptibility testing of filamentous fungi. Exp Ther Med. 2019. https://doi.org/10.3892/etm.2019.8118.
Gómez-Velásquez JC, Loaiza-Díaz N, Norela Hernández G, Lima N, Mesa-Arango AC. Development and validation of an in-house library for filamentous fungi identification by MALDI-TOF MS in a clinical laboratory in Medellin (Colombia). Microorganisms. 2020. https://doi.org/10.3390/microorganisms8091362.
Eucast Definitive Document E.Def 9.1: method for the determination of broth dilution minimum inhibitory concentrations of antifungal agents for conidia forming moulds. 2008. https://www.eucast.org/astoffungi/previous_versions_of_documents/. Accessed 25 Feb 2022.
Vagiakou E, Orfanidou M, Miltsakakis D, Zourla K, Petrou E, Goula A. Fungal keratitis caused by Alternaria spp following injury. Acta Microbiol Hell. 2008;53:44–8.
Peponis V, Rosenberg P, Chalkiadakis SE, Insler M, Amariotakis A. Fungal scleral keratitis and endophthalmitis following pterygium excision. Eur J Ophthalmol. 2009. https://doi.org/10.1177/112067210901900326.
Konidaris V, Mersinoglou A, Vyzantiadis TA, Papadopoulou D, Boboridis KG, Ekonomidis P. Corneal transplant infection due to alternaria alternata: a case report. Case Rep Ophthalmol Med. 2013. https://doi.org/10.1155/2013/589620.
Adamopoulou A, Sakellaris D, Koronis S, Balidis M, Zachariadis Z, Tranos P, Kozeis N, Gatzioufas Z, Anogeianakis G, Mikropoulos DG, Konstas AG. Rare persistent corneal infection by phoma sp.—a case report. Ophthalmol Ther. 2019. https://doi.org/10.1007/s40123-019-0163-0.
Mikropoulos DG, Kymionis GD, Voulgari N, Kaisari E, Nikolakopoulos KA, Katsanos A, Konstas AG. Intraoperative photoactivated chromophore for infectious keratitis-corneal cross-linking (PACK-CXL) during penetrating keratoplasty for the management of fungal keratitis in an immunocompromised patient. Ophthalmol Ther. 2019. https://doi.org/10.1007/s40123-019-0196-4.
Atzamoglou S, Siopi M, Meletiadis J, Markopoulos I, Kontomichos L, Batsos G, Paroikakis E, Peponis V. A corneal perforation related to Beauveria bassiana and post-penetrating keratoplasty management discussion. Cureus. 2021. https://doi.org/10.7759/cureus.15724.
Petrou E, Orfanidou M, Georgios S. Dimtsas GS, Moutzouri-Sidiri M, Voulgaridi I, Vyzantiadis TA, Vagiakou E, Droutsas K. A case of keratomycosis caused by Curvularia spicifera (previously Bipolaris spicifera) and review of the literature. Acta Microbiol Hell. 2022; 67(1): 59
Kymionis GD, Kouroupaki AI, Liakopoulos DA, Arandjelovic IR, Tsoulnaras KI. Multiorganism, drug-resistant keratitis treated by corneal crosslinking. Eur J Ophthalmol. 2016. https://doi.org/10.5301/ejo.5000755.
Clinical breakpoints for fungi (Candida and Aspergillus species). In: The European committee on antimicrobial susceptibility testing—EUCAST. 2019. https://www.eucast.org/astoffungi/clinicalbreakpointsforantifungals/. Accessed 25 Feb 2022.
Acharya Y, Acharya B, Karki P. Fungal keratitis: study of increasing trend and common determinants. Nepal J Epidemiol. 2017. https://doi.org/10.3126/nje.v7i2.17975.
Chitamparam S, Lim TH, Tai E, Ibrahim M. Mycotic keratitis in a tertiary hospital in Northeastern Malaysia. Turk J Ophthalmol. 2020. https://doi.org/10.4274/tjo.galenos.2020.57609.
Ong HS, Fung SSM, Macleod D, Dart JKG, Tuft SJ, Burton MJ. Altered patterns of fungal keratitis at a London ophthalmic referral hospital an eight-year retrospective observational study. Am J Ophthalmol. 2016;168:227–36. https://doi.org/10.1016/j.ajo.2016.05.021.
Rosa RH Jr, Miller D, Alfonso EC. The changing spectrum of fungal keratitis in South Florida. Ophthalmology. 1994. https://doi.org/10.1016/s0161-6420(94)31225-5.
Mosquera Gordillo MA, Barón Cano N, Garralda Luquin A, López Gutiérrez C, Mengual Verdú E, Trujillo Cabrera G, et al. Keratitis secondary to Fusarium spp. in Spain 2012–2014. Arch Soc Esp Oftalmol (Engl Ed). 2018. https://doi.org/10.1016/j.oftal.2017.08.005.
Olivier R, Knoeri J, Leveziel L, Negrier P, Georgeon C, Kobal A, et al. Update on fungal keratitis in France: a case-control study. Acta Ophthalmol. 2021. https://doi.org/10.1111/aos.14910.
Roth M, Holtmann C, Daas L, Kakkassery V, Kurzai O, Geerling G, et al. Results from the German fungal keratitis registry: significant differences between cases with and without a history of contact lens use. Cornea. 2021. https://doi.org/10.1097/ICO.0000000000002705.
Oliveira Dos Santos C, Kolwijck E, van Rooij J, Stoutenbeek R, Visser N, Cheng YY, et al. Epidemiology and clinical management of fusarium keratitis in the Netherlands 2005–2016. Front Cell Infect Microbiol. 2020. https://doi.org/10.3389/fcimb.2020.00133.
Nowik KE, Wylęgała A, Nowik K, Wylęgała E. A single-centre retrospective observational study of fungal keratitis in Poland with a review of findings in Europe. Ann Agric Environ Med. 2020. https://doi.org/10.26444/aaem/109414.
Tuft SJ, Tullo AB. Fungal keratitis in the United Kingdom 2003–2005. Eye (Lond). 2009. https://doi.org/10.1038/eye.2008.298.
Farrell S, McElnea E, Moran S, Knowles S, Murphy CC. Fungal keratitis in the Republic of Ireland. Eye (Lond). 2017. https://doi.org/10.1038/eye.2017.82.
Nielsen SE, Nielsen E, Julian HO, Lindegaard J, Højgaard K, Ivarsen A, Hjortdal J, Heegaard S. Incidence and clinical characteristics of fungal keratitis in a Danish population from 2000 to 2013. Acta Ophthalmol. 2015. https://doi.org/10.1111/aos.12440.
Bograd A, Seiler T, Droz S, Zimmerli S, Früh B, Tappeiner C. Bacterial and fungal keratitis: a retrospective analysis at a university hospital in Switzerland. Klin Monbl Augenheilkd. 2019. https://doi.org/10.1055/a-0774-7756.
Van Diepeningen AD, Feng P, Ahmed S, Sudhadham M, Bunyaratavej S, de Hoog GS. Spectrum of Fusarium infections in tropical dermatology evidenced by multilocus sequencing typing diagnostics. Mycoses. 2015. https://doi.org/10.1111/myc.12273.
Sara S, Sharpe K, Morris S. Multidrug-resistant Fusarium keratitis: diagnosis and treatment considerations. BMJ Case Rep. 2016. https://doi.org/10.1136/bcr-2016-215401.
Sav H, Rafati H, Öz Y, Dalyan-Cilo B, Ener B, Mohammadi F, Ilkit M, van Diepeningen AD, Seyedmousavi S. Biofilm formation and resistance to fungicides in clinically relevant members of the fungal genus Fusarium. J Fungi (Basel). 2018. https://doi.org/10.3390/jof4010016.
Chen CA, Hsu SL, Hsiao CH, Ma DH, Sun CC, Yu HJ, Fang PC, Kuo MT. Comparison of fungal and bacterial keratitis between tropical and subtropical Taiwan: a prospective cohort study. Ann Clin Microbiol Antimicrob. 2020. https://doi.org/10.1186/s12941-020-00353-3.
Khor WB, Aung T, Saw SM, Wong TY, Tambyah PA, Tan AL, et al. An outbreak of Fusarium keratitis associated with contact lens wear in Singapore. JAMA. 2006. https://doi.org/10.1001/jama.295.24.2867.
Chang DC, Grant GB, O’Donnell K, Wannemuehler KA, Noble-Wang J, Rao CY, Fusarium Keratitis Investigation Team, et al. Multistate outbreak of fusarium keratitis associated with use of a contact lens solution. JAMA. 2006. https://doi.org/10.1001/jama.296.8.953.
Epstein AB. In the aftermath of the Fusarium keratitis outbreak: what have we learned? Clin Ophthalmol. 2007;1(4):355–66.
Bullock JD, Warwar RE, Elder BL, Khamis HJ. Microbiological investigations of ReNu plastic bottles and the 2004 to 2006 ReNu with moistureloc-related worldwide Fusarium keratitis event. Eye Contact Lens. 2016. https://doi.org/10.1097/ICL.0000000000000175.
Mela EK, Anastassiou ED, Gartaganis SP, Christofidou M. Fungal isolation from disinfectant solutions of contact lens storage cases among asymptomatic users. Eye Contact Lens. 2015. https://doi.org/10.1097/ICL.0000000000000069.
Krysik K, Wroblewska-Czajka E, Lyssek-Boron A, Wylegala EA, Dobrowolski D. Total penetrating keratoplasty: indications, therapeutic approach, and long-term follow-up. J Ophthalmol. 2018. https://doi.org/10.1155/2018/9580292.
Al-Hatmi AMS, Meis JF, de Hoog GS. Fusarium: molecular diversity and intrinsic drug resistance. PLoS Pathog. 2016. https://doi.org/10.1371/journal.ppat.1005464.
Luangsa-Ard J, Houbraken J, van Doorn T, Hong SB, Borman AM, Hywel-Jones NL, Samson RA. Purpureocillium, a new genus for the medically important Paecilomyces lilacinus. FEMS Microbiol Lett. 2011. https://doi.org/10.1111/j.1574-6968.2011.02322.x.
Almeida Oliveira M, Carmo A, Rosa A, Murta J. Posaconazole in the treatment of refractory Purpureocillium lilacinum (former Paecilomyces lilacinus) keratitis: the salvation when nothing works. BMJ Case Rep. 2019. https://doi.org/10.1136/bcr-2018-228645.
Turner LD, Conrad D. Retrospective case-series of Paecilomyces lilacinus ocular mycoses in Queensland Australia. BMC Res Notes. 2015. https://doi.org/10.1186/s13104-015-1591-0.
Sponsel W, Chen N, Dang D, Paris G, Graybill J, Najvar LK, et al. Topical voriconazole as a novel treatment for fungal keratitis. Antimicrob Agents Chemother. 2006. https://doi.org/10.1128/AAC.50.1.262-268.2006.
Todokoro D, Yamada N, Fukuchi M, Kishi S. Topical voriconazole therapy of Purpureocillium lilacinum keratitis that occurred in disposable soft contact lens wearers. Int Ophthalmol. 2014. https://doi.org/10.1007/s10792-014-9965-1.
Al-Hatmi AMS, Castro MA, de Hoog GS, Badali H, Alvarado VF, Verweij PE, Meis JF, Zago VV. Epidemiology of Aspergillus species causing keratitis in Mexico. Mycoses. 2019. https://doi.org/10.1111/myc.12855.
Khor WB, Prajna VN, Garg P, Mehta JS, Xie L, Liu Z, ACSIKS Group, et al. The Asia cornea society infectious keratitis study: a prospective multicenter study of infectious keratitis in Asia. Am J Ophthalmol. 2018. https://doi.org/10.1016/j.ajo.2018.07.040.
Manikandan P, Varga J, Kocsubé S, Anita R, Revathi R, Németh TM, Narendran V, Vágvölgyi C, Panneer Selvam K, Shobana CS, Babu Singh YR, Kredics L. Epidemiology of Aspergillus keratitis at a tertiary care eye hospital in South India and antifungal susceptibilities of the causative agents. Mycoses. 2013. https://doi.org/10.1111/j.1439-0507.2012.02194.x.
Rudramurthy SM, Paul RA, Chakrabarti A, Mouton JW, Meis JF. Invasive aspergillosis by Aspergillus flavus: epidemiology, diagnosis, antifungal resistance, and management. J Fungi (Basel). 2019. https://doi.org/10.3390/jof5030055.
Zaini F, Lotfali E, Fattahi A, Siddig E, Farahyar S, Kouhsari E, Saffari M. Voriconazole resistance genes in Aspergillus flavus clinical isolates. J Mycol Med. 2020. https://doi.org/10.1016/j.mycmed.2020.100953.
Hsiao CH, Yeh LK, Chen HC, Lin HC, Chen PY, Ma DH, Tan HY. Clinical characteristics of alternaria keratitis. J Ophthalmol. 2014. https://doi.org/10.1155/2014/536985.
Monno R, Alessio G, Guerriero S, Caggiano G, Capolongo C, De Vito D, Sanguinetti M. Alternaria is an infrequent cause of keratitis: a case report and review of the literature. Eye Contact Lens. 2015. https://doi.org/10.1097/ICL.0000000000000012.
Yildiz EH, Ailani H, Hammersmith KM, Eagle RC Jr, Rapuano CJ, Cohen EJ. Alternaria and Paecilomyces keratitis associated with soft contact lens wear. Cornea. 2010. https://doi.org/10.1097/ICO.0b013e3181ba0cde.
Ursea R, Tavares LA, Feng MT, McColgin AZ, Snyder RW, Wolk DM. Non-traumatic Alternaria keratomycosis in a rigid gas-permeable contact lens patient. Br J Ophthalmol. 2010. https://doi.org/10.1136/bjo.2009.164632.
da Cunha KC, Sutton DA, Fothergill AW, Cano J, Gené J, Madrid H, De Hoog S, Crous PW, Guarro J. Diversity of Bipolaris species in clinical samples in the United States and their antifungal susceptibility profiles. J Clin Microbiol. 2012. https://doi.org/10.1128/JCM.01965-12.
Manamgoda DS, Rossman AY, Castlebury LA, Crous PW, Madrid H, Chukeatirote E, et al. The genus Bipolaris. Stud Mycol. 2014. https://doi.org/10.1016/j.simyco.2014.10.002.
Thiel MA, Zinkernagel AS, Burhenne J, Kaufmann C, Haefeli WE. Voriconazole concentration in human aqueous humor and plasma during topical or combined topical and systemic administration for fungal keratitis. Antimicrob Agents Chemother. 2007. https://doi.org/10.1128/AAC.00762-06.
Chidambaram JD, Venkatesh Prajna N, Srikanthi P, Lanjewar S, Shah M, Elakkiya S, Lalitha P, Burton MJ. Epidemiology, risk factors, and clinical outcomes in severe microbial keratitis in South India. Ophthalmic Epidemiol. 2018. https://doi.org/10.1080/09286586.2018.1454964.
Gopinathan U, Garg P, Fernandes M, Sharma S, Athmanathan S, Rao GN. The epidemiological features and laboratory results of fungal keratitis. Cornea. 2002. https://doi.org/10.1097/00003226-200208000-00004.
Acknowledgements
We are grateful to Prof. Anna Maria Tortorano, University of Milan, Dr. Anne van Diepeningen and Bert Gerrits van den Ende, Westerdijk Fungal Biodiversity Institute, Utrect, the Netherlands, for their valuable contribution to the molecular identification of our strains. We would also like to thank Mrs Theodora Koliou (Department of Microbiology, Medical School, National and Kapodistrian University of Athens) for her excellent technical assistance with MALDI TOF.
Funding
The study was partially financed by a grant from Gilead Sciences Hellas Μ.EPE (ASKLEPIOS Programme, 2013).
Author information
Authors and Affiliations
Contributions
AM collected data, performed diagnostic tests, and wrote the first draft. MD-A and GP conceived, designed, and supervised the study. MS provided data and performed diagnostic tests. MD-A analyzed data and edited the manuscript. JM, MS, MC, IC, AA, EP, GV and GP, reviewed and commented on previous versions of the manuscript. All authors provided data and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical Approval
The study has been approved by the Ethics Committee and Scientific Council of Attikon University Hospital (14/4/2014).
Additional information
Handling Editor: Philip Aloysius Thomas.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Author query raised during the typesetting stage was inadvertently included at the end of abstract section. It has been removed.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mpakosi, A., Siopi, M., Vrioni, G. et al. Filamentous Fungal Keratitis in Greece: A 16-Year Nationwide Multicenter Survey. Mycopathologia 187, 439–453 (2022). https://doi.org/10.1007/s11046-022-00666-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-022-00666-1